Culturally Inclusive Nutrition Counseling: Applying Plate-Based Nutrition Principles Across Food Traditions
The Dietary Guidelines for Americans, 2025-2030 emphasize balanced dietary patterns and food quality but focus primarily on population-level recommendations rather than practical strategies for adapting guidance across culturally diverse eating patterns.
This guide addresses that gap by translating plate-based nutrition principles into culturally inclusive counseling strategies, while emphasizing flexibility across cultural traditions. This page complements dietitian care and is designed to equip primary care and family physicians, internists, nurse practitioners, and physician assistants with practical, time-efficient tools to support culturally inclusive nutrition discussions in clinical practice.1,2
Why Cultural Eating Patterns Matter in Clinical Nutrition
Food choices are closely linked to identity, family structure, food access, and health behaviors. A substantial body of evidence demonstrates that dietary counseling is more effective when it reflects patients’ cultural norms and lived experiences.3-5
Clinical relevance includes:
-
Improved dietary adherence and patient engagement
-
Stronger trust and communication in clinical encounters
-
More favorable cardiometabolic outcomes when recommendations align with customary diets
Key Counseling Point: Culturally tailored interventions have shown benefits for glycemic control, blood pressure, and lipid parameters in multiple studies, particularly among populations at higher cardiometabolic risk.4,5
Applying Plate-Based Nutrition Principles Across Cultures
Plate-based nutrition frameworks emphasize balance across food groups rather than prescriptive food lists or rigid meal plans. This approach allows primary care clinicians to provide evidence-based dietary guidance while adapting recommendations to patients’ customary eating patterns and cultural contexts.
In practice, applying these principles requires recognizing how core nutrition components (vegetables, fruits, protein, grains, and dairy or alternatives) appear within different food traditions. The table below translates plate-based nutrition principles into clinically relevant examples, highlighting familiar foods from diverse cuisines that meet common nutritional goals and can be used to support culturally inclusive counseling conversations.
Table 1. Plate-Based Nutrition Across Diverse Food Traditions
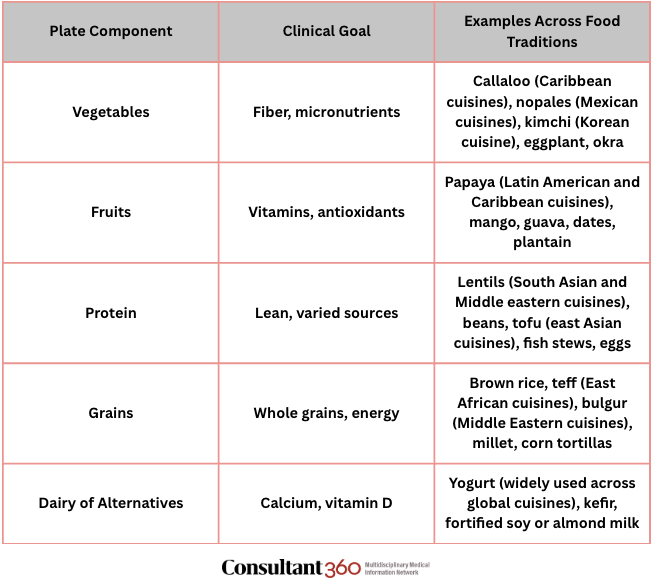
Note: Food examples reflect items commonly used across a range of global cuisines and are not intended to represent a single, fixed cultural tradition.
Clinical example: A traditional fish-based dish may support heart-healthy eating patterns when grilled or baked, but contributes substantially more saturated fat and calories when deep-fried, regardless of the cuisine in which it is prepared.
Key Counseling Point: Preparation methods, including cooking technique and the use of added fats, sodium, and sugars, often have a greater impact on cardiometabolic risk than the cultural origin of the food itself. Many traditional dishes are nutritionally balanced in composition but become less health-promoting when prepared using deep-frying, excessive added sodium, or sugar-sweetened sauces. Counseling that focuses on preparation modifications, such as baking or grilling instead of frying, reducing added salt, or adjusting portion size, allows clinicians to support evidence-based dietary goals while preserving cultural relevance and improving long-term adherence.1-5
Common Counseling Pitfalls to Avoid
Clinicians should be mindful of counseling approaches that may unintentionally undermine patient trust or adherence, including:
-
Labeling traditional foods as inherently unhealthy
-
Recommending substitutions that are culturally unfamiliar or difficult to access
-
Overlooking food affordability, availability, and customary preparation methods
-
Applying Western dietary patterns as the default standard
Key Counseling Point: A strengths-based approach that recognizes existing healthy elements within traditional diets is more likely to support sustained behavior change.³
⬇️ Download: The Cultural Food Swap Guide
Practical Counseling Language: Clinician Script Box
Use familiar foods and patient-centered language to frame nutrition counseling as an adaptation, not a restriction.
Opening the conversation1,2
“Many traditional meals already include the same food groups we recommend for health. Let’s look at how your usual foods fit into your nutrition goals.”
Discussing modifications3
“Rather than changing what you eat, we can focus on preparation methods, portion sizes, and balance on the plate.”
Addressing concerns about restriction¹
“This is not about giving up cultural foods. It is about helping those foods support blood sugar control, blood pressure management, or heart health.”
Key Counseling Point: Focus conversations on preparation methods, portion balance, and achievable modifications that support clinical goals while preserving cultural relevance. These scripts reflect evidence supporting patient-centered, culturally responsive counseling approaches in primary care.3-5
⬇️ Download: The Culturally Responsive Nutrition Counseling Toolkit
Condition-Specific Applications
-
Emphasize carbohydrate quality and portion distribution within traditional meals
-
Highlight fiber-rich vegetables and legumes common across many cultural diets
-
Discuss meal timing and balance rather than elimination of staple foods
-
Identify major dietary sodium sources, including preserved or packaged traditional foods
-
Encourage heart-healthy fats within customary cooking practices
-
Reinforce the cardioprotective aspects of plant-forward dietary patterns already present in many cuisines
Obesity and Metabolic Syndrome
-
Focus counseling on energy density and preparation methods
-
Reinforce satiety through fiber- and protein-rich traditional foods
Key Counseling Point: When addressing chronic conditions, prioritize how traditional meals can be adjusted to support disease-specific goals rather than recommending food elimination. Emphasize preparation methods, portion distribution, and food quality to align culturally diverse eating patterns with cardiometabolic risk reduction. When applying these strategies, clinicians should also consider behavioral, social, and economic factors that influence food access and dietary choices, as these factors often shape the feasibility and sustainability of nutrition recommendations.
Clinician FAQ: Culturally Inclusive Nutrition Counseling
Q: Can traditional cultural foods fit into plate-based nutrition frameworks?
Yes. Plate-based frameworks emphasize food groups, portion balance, and preparation methods rather than specific foods. Many cultural diets already include vegetables, legumes, whole grains, and lean protein sources. Counseling typically focuses on optimizing balance and preparation rather than eliminating customary foods.1,2
Q: How should primary care clinicians counsel patients on cultural diets?
Counseling should be patient-centered and culturally respectful, with an emphasis on achievable modifications aligned with clinical goals. Effective strategies include asking patients about customary meals, identifying existing healthy components, and collaboratively discussing preparation methods that support cardiometabolic health and long-term adherence.3-5
Q. When should primary care clinicians refer patients to a registered dietitian?
Referral to a registered dietitian is appropriate for patients with complex nutrition needs, such as insulin-treated diabetes, advanced chronic kidney disease, significant food insecurity, disordered eating, or when culturally tailored dietary counseling requires more intensive support than can be provided during routine visits. Dietitians can provide individualized meal planning while reinforcing culturally relevant eating patterns.
For more clinician FAQs, visit our FAQ page on culturally inclusive nutrition counseling
Key Counseling Point: Culturally inclusive nutrition counseling improves adherence when clinicians apply flexible, plate-based principles instead of rigid dietary rules. Anchor recommendations in balance and preparation, tailor guidance to individual preferences and health needs, and reinforce that traditional foods can remain part of a healthy dietary pattern.
References
-
U.S. Department of Agriculture Center for Nutrition Policy and Promotion. MyPlate: Build Healthy Eating Habits. Updated 2024. Available at: https://www.myplate.gov/. Accessed February 2, 2026.
-
U.S. Department of Health and Human Services. Dietary Guidelines for Americans, 2020–2025. Available at: https://www.dietaryguidelines.gov/. Accessed February 2, 2026.
-
Balakrishnan S. MPH, RD, Benea C. MPH, RD, Banerjee A. PhD, Mahajan A. PhD, MPH, RD. Exploring the Social Determinants of Health in Nutrition Care for South Asian Communities: A Narrative Review. Can J Diet Pract Res. 2025;86(1):462-470. doi:10.3148/cjdpr-2024-024
-
Hawthorne K, Robles Y, Cannings-John R, Edwards AG. Culturally appropriate health education for type 2 diabetes mellitus in ethnic minority groups. Cochrane Database Syst Rev. 2008;(3):CD006424. Published 2008 Jul 16. doi:10.1002/14651858.CD006424.pub2
-
Cross V, Stanford J, Gómez-Martín M, Collins CE, Robertson S, Clarke ED. Do Personalized nutrition interventions improve dietary intake and cardiovascular disease risk factors? A systematic review and meta-analysis of randomized controlled trials. Nutr Rev. 2025;83(7):e1709–e1721. doi:10.1093/nutrit/nuae149.
©2026 HMP Global. All Rights Reserved.
Any views and opinions expressed are those of the author(s) and/or participants and do not necessarily reflect the views, policy, or position of Consultant360 or HMP Global, their employees, and affiliates.


