Peer Reviewed
Mycobacterium Chelonae Infection Diagnosed by PCR in a Patient with Chronic Leg Nodules
Mycobacterium Chelonae Infection Diagnosed by PCR in a Patient with Chronic Leg Nodules
Introduction: A 68-year-old woman presented to the dermatology clinic with a 3-year history of purpuric nodules on the right lower extremity.
History. The patient’s past medical history was notable for breast cancer, rheumatoid arthritis, Sjögren syndrome, and thyroid nodules. The patient also had a history of deep vein thrombosis of the right leg and bilateral pulmonary emboli. She reported a persistent, tender lesion on her right lower leg that had been draining intermittently for 3 years. She recalled trauma to the area 4 years earlier from a car door injury. On physical examination, the right lower leg showed red to violaceous nodules with central ulceration, accompanied by a scar and signs of chronic stasis. (Figure 1A-C)
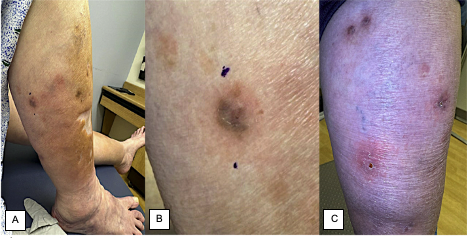
Figure 1A-C. Red to violaceous nodules with central ulceration and stasis changes on the right lower legDiagnostic testing. We performed a punch biopsy on the right calf for hematoxylin and eosin staining. (Figure 2) The Periodic Acid-Schiff (PAS) and Gram stains did not identify fungal organisms or bacteria. We also performed an acid-fast bacilli (AFB) stain (Figure 3) and an additional biopsy for tissue culture, which failed to reveal infectious organisms. A broad-range polymerase chain reaction (PCR) showed Mycobacterium (M) chelonae.
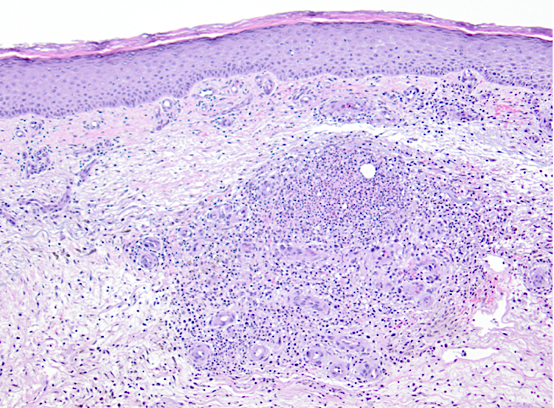
Figure 2. Hematoxylin and eosin–staining (original magnification ×100) revealed fibrosis, abundant hemosiderin, lipocysts of varying sizes, increased number of blood vessels arranged in a tufted fashion and collections of neutrophils in the dermis.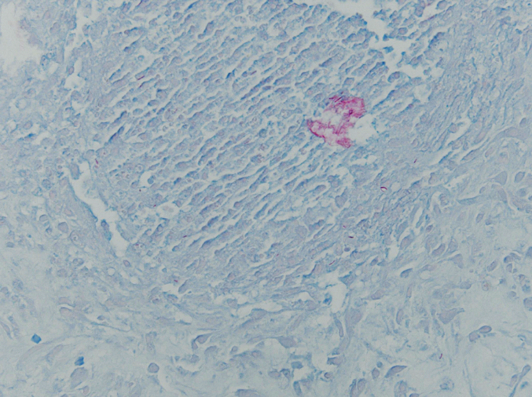
Figure 3. Acid-fast bacilli stain (original magnification ×400) identified mycobacteria within the dermis


