An Atlas of Lumps and Bumps, Part 51: Diffuse Cutaneous Mastocytosis
Diffuse Cutaneous Mastocytosis
Diffuse cutaneous mastocytosis, a rare but potentially fatal form of cutaneous mastocytosis, accounts for approximately 1% to 5% of pediatric cutaneous mastocytosis cases.1-5 The condition is characterized by extensive mast cell infiltration of the entire skin, which can result in significant mast cell mediator release leading to systemic reactions that can be severe or even fatal.5-7 Onset of the disease is usually at birth or shortly thereafter (usually before 6 months of age).2,7
Children with diffuse cutaneous mastocytosis typically present with pruritus (especially after exposure to a trigger), flushing, widespread recurrent episodes of urticaria evolving into blisters, bullae, erosions, and crusts (Figure 1).1,8 The blisters/bullae contain clear fluid initially but may become hemorrhagic with time (Figure 2).1,8
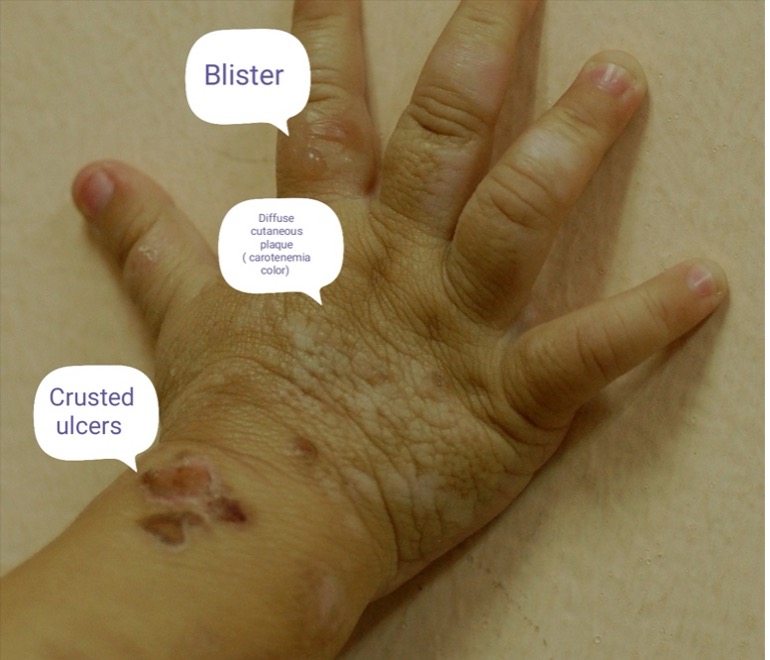
Fig. 1. Children with diffuse cutaneous mastocytosis typically present with pruritus, flushing, widespread recurrent episodes of urticaria evolving into blisters, bullae, erosions, and crusts.
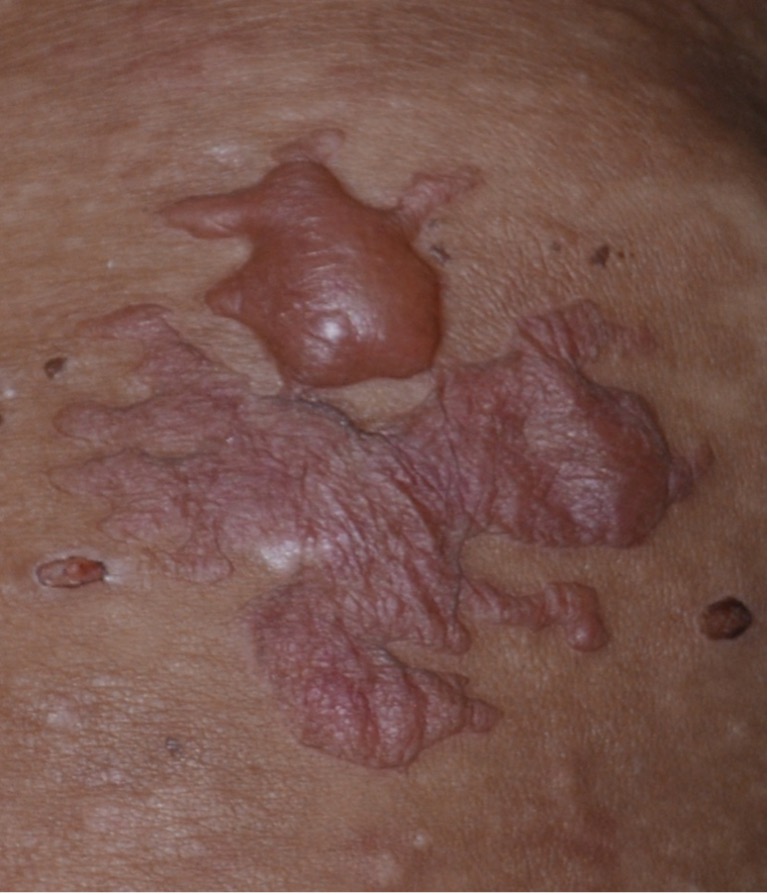
Fig. 2. Patients with blisters/bullae contain clear fluid initially but may become hemorrhagic with time.
Affected children may experience nausea, vomiting, abdominal pain, diarrhea, bronchospasm, dyspnea, tachycardia, and hypotension.7,9 Darier sign (localized erythema and urticaria) can be elicited by gentle stroking, scratching, or rubbing of the skin but should be avoided as such skin manipulation may trigger massive mast cell mediator release.6 Darier sign and marked dermographism are hallmarks of diffuse cutaneous mastocytosis.1 Generally, children with diffuse cutaneous mastocytosis do not have individually discernible lesions such as pigmented plaques.1,3,10,11 Rather, these children have generalized redness or darkening of the skin, accentuation of hair follicles and skinfolds (Figure 3), and induration and thickening of almost the entire skin (pachyderma) and a leathery appearance traditionally referred to as a “peau d’orange” appearance, “crocodile-like pachydermia”, and “elephant skin”.1,8,10,12-15
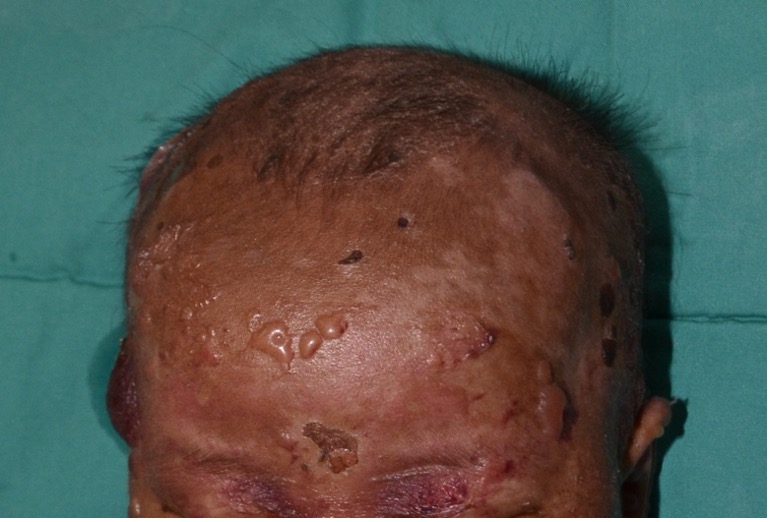
Fig. 3. Children have generalized redness or darkening of the skin, accentuation of hair follicles and skinfolds, and induration and thickening of almost the entire skin.
Organomegaly and lymphadenopathy are characteristically absent. Affected children are at risk of anaphylaxis and shock.7,12 Several variants have been recognized including the small vesicular variant, large bullous variant, and superimposed nodules and plaques at sites of dense mast cell infiltration.1,8,14
Most children with diffuse cutaneous mastocytosis have normal serum tryptase levels. However, serum tryptase levels may be elevated in the early stages of the disease with or without systemic involvement.15 Despite the severity of the disease, children with diffuse cutaneous mastocytosis often outgrow the disease by adolescence.1,15,16 In some patients, diffuse cutaneous mastocytosis persists into adulthood (Figure 4) and may have systemic involvement affecting other organs.1,7,15
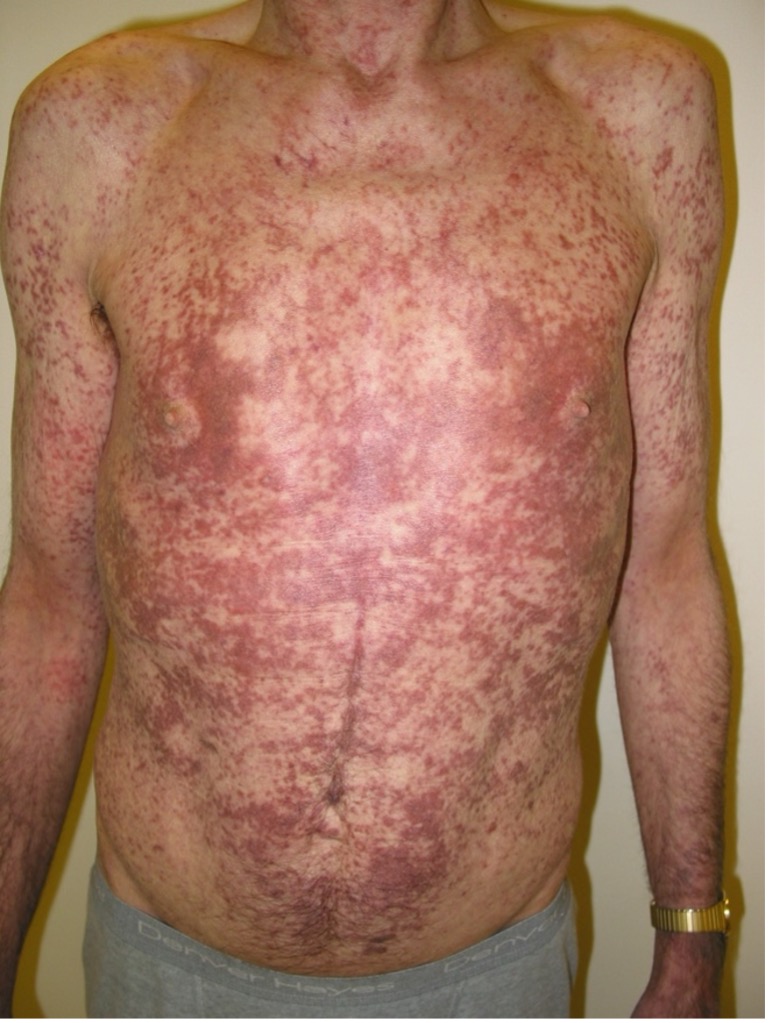
Fig. 4. In some patients, diffuse cutaneous mastocytosis persists into adulthood.
AUTHORS:
Alexander K.C. Leung, MD1,2, Benjamin Barankin, MD3, Joseph M. Lam, MD4, Kin Fon Leong, MD5
AFFILIATIONS:
1Clinical Professor of Pediatrics, the University of Calgary, Calgary, Alberta, Canada
2Pediatric Consultant, the Alberta Children’s Hospital, Calgary, Alberta, Canada
3Dermatologist, Medical Director and Founder, the Toronto Dermatology Centre, Toronto, Ontario, Canada
4Associate Clinical Professor of Pediatrics, Dermatology and Skin Sciences, the University of British Columbia, Vancouver, British Columbia, Canada.
5Pediatric Dermatologist, the Pediatric Institute, Kuala Lumpur General Hospital, Kuala Lumpur, Malaysia
CITATION:
Leung AKC, Barankin B, Lam JM, Leong KF. An Atlas of Lumps and Bumps, Part 51: Solitary Diffuse Cutaneous Mastocytosis Consultant. 2025;65(6). doi: 10.25270/con.2025.06.000002
CORRESPONDENCE:
Alexander K. C. Leung, MD, #200, 233 16th Ave NW, Calgary, AB T2M 0H5, Canada (aleung@ucalgary.ca)
EDITOR’S NOTE:
This article is part of a series describing and differentiating dermatologic lumps and bumps. To access previously published articles in the series, visit: https://www.consultant360.com/resource-center/atlas-lumps-and-bumps.
References
- Leung AKC, Barankin B, Leong KF. A 6-week-old girl with recurrent bullous lesions and erosions. Pediatr Rev. 2019;40(Suppl 1):34-36. doi:10.1542/pir.2017-0265
- Di Raimondo C, Del Duca E, Silvaggio D, et al. Cutaneous mastocytosis: A dermatological perspective. Australas J Dermatol. 2021;62(1):e1-e7. doi:10.1111/ajd.13443
- Hosking AM, Makdisi J, Ortenzio F, de Feraudy S, Smith J, Linden K. Diffuse cutaneous mastocytosis: Case report and literature review. Pediatr Dermatol. 2018;35(6):e348-e352. doi:10.1111/pde.13651
- Méni C, Bruneau J, Georgin-Lavialle S, et al. Paediatric mastocytosis: a systematic review of 1747 cases. Br J Dermatol. 2015;172(3):642-651. doi:10.1111/bjd.13567
- Shibata Y, Hirota S, Saito I, Asahina A. Diffuse cutaneous mastocytosis: Identification of KIT mutation and long-term follow-up with serum tryptase level. J Dermatol. Published online January 31, 2021. doi:10.1111/1346-8138.15764
- Otani IM, Carroll RW, Yager P, et al. Diffuse cutaneous mastocytosis with novel somatic KIT mutation K509I and association with tuberous sclerosis. Clin Case Rep. 2018;6(9):1834-1840. doi:10.1002/ccr3.1607
- Sun J, Xu JS, Xiang X, Ma L. Bullae on the extremities of a newborn: a case of diffuse cutaneous mastocytosis mimicking epidermolysis bullosa. J Eur Acad Dermatol Venereol. 2020;34(11):e703-e705. doi:10.1111/jdv.16438
- Bankova LG, Walter JE, Iyengar SR, et al. Generalized bullous eruption after routine vaccination in a child with diffuse cutaneous mastocytosis. J Allergy Clin Immunol Pract. 2013;1(1):94-96. doi:10.1016/j.jaip.2012.08.008
- Chaudhary N, Shapiro N, Bhutada A, Rastogi S. c-KIT-positive fatal diffuse cutaneous mastocytosis with systemic manifestations in a neonate. J Pediatr Hematol Oncol. 2019;41(5):e338-e340. doi:10.1097/MPH.0000000000001271
- Castells M, Akin C. Mastocytosis (cutaneous and systemic): epidemiology, pathogenesis, and clinical manifestations. In: Post TW, ed. UpToDate. Waltham, MA. Accessed March 12, 2021.
- Castells M, Akin C. Mastocytosis (cutaneous and systemic): evaluation and diagnosis in children. In: Post TW, ed. UpToDate. Waltham, MA. Accessed March 12, 2021.
- Cardoso JM, Cabral CAS, Lellis RF, Ravelli FN. Bullous congenital diffuse cutaneous mastocytosis. An Bras Dermatol. 2020;95(2):255-256. doi:10.1016/j.abd.2019.01.012
- Hussain SH. Pediatric mastocytosis. Curr Opin Pediatr. 2020;32(4):531-538. doi:10.1097/MOP.0000000000000922
- Kleewein K, Lang R, Diem A, et al. Diffuse cutaneous mastocytosis masquerading as epidermolysis bullosa. Pediatr Dermatol. 2011;28(6):720-725. doi:10.1111/j.1525-1470.2011.01479.x
- Matito A, Azaña JM, Torrelo A, Alvarez-Twose I. Cutaneous mastocytosis in adults and children: New classification and prognostic factors. Immunol Allergy Clin North Am. 2018;38(3):351-363. doi:10.1016/j.iac.2018.04.001
- Gupta M, Akin C, Sanders GM, et al. Blisters, vaccines, and mast cells: A difficult case of diffuse cutaneous mastocytosis. J Allergy Clin Immunol Pract. 2019;7(4):1370-1372. doi:10.1016/j.jaip.2018.11.046
©2025 HMP Global. All Rights Reserved.
Any views and opinions expressed are those of the author(s) and/or participants and do not necessarily reflect the views, policy, or position of Consultant360 or HMP Global, their employees, and affiliates.


