Peer Reviewed
An Infant With Café au Lait Macules, Vitiligo, and a Hemangioma: A Case of Neurofibromatosis 1
Authors:
Feryal Elorr, BS; Shruti Sakhuja, BS, MD; and Lynnette Mazur, MD, MPH
Department of Pediatrics at McGovern Medical School at University of Texas Health Science Center, Houston, Texas
Children’s Memorial Hermann Hospital, Houston, Texas
Citation:
Elorr F, Sakhuja S, Mazur L. An infant with café au lait macules, vitiligo, and a hemangioma: a case of neurofibromatosis 1 [published online April 16, 2018]. Consultant for Pediatricians.
A 12-month-old black Hispanic girl presented to our pediatrics clinic for a checkup. The mother reported that the girl had no health concerns.
Physical examination. Upon physical examination, the patient’s height was 75 cm (64th percentile), weight was 7.75 kg (12th percentile), and head circumference was 48 cm (>99th percentile). She had frontal bossing; café au lait macules measuring 1 to 8 cm on the abdomen (Figure 1), the dorsal surface of the right foot (Figure 2), the left leg (Figure 3), and the chest (Figure 4); café au lait macules and vitiligo on the right axillae (Figure 5) and café au lait macules on the left axilla (Figure 6); a hypopigmented macule measuring 8 cm on the left upper left back (Figure 7); and a hemangioma measuring 6 cm.



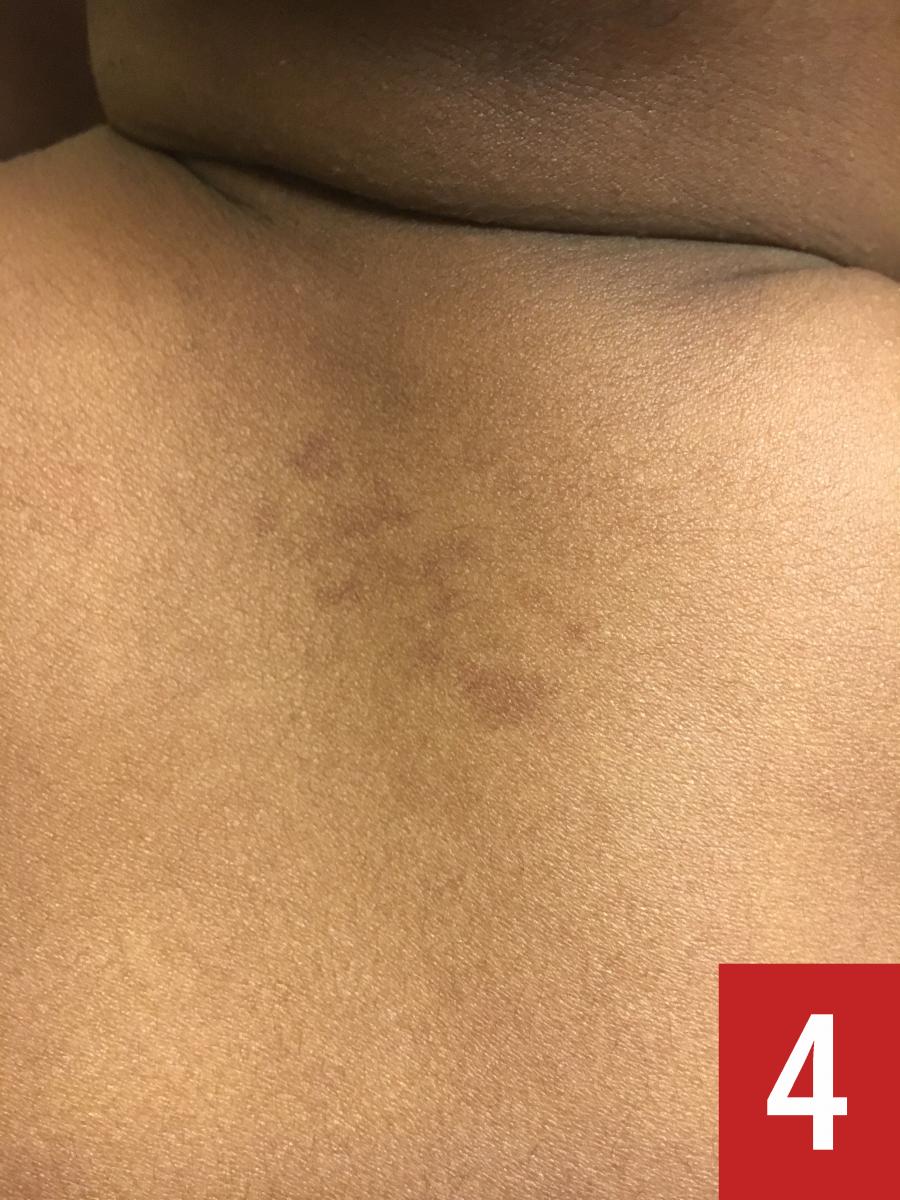
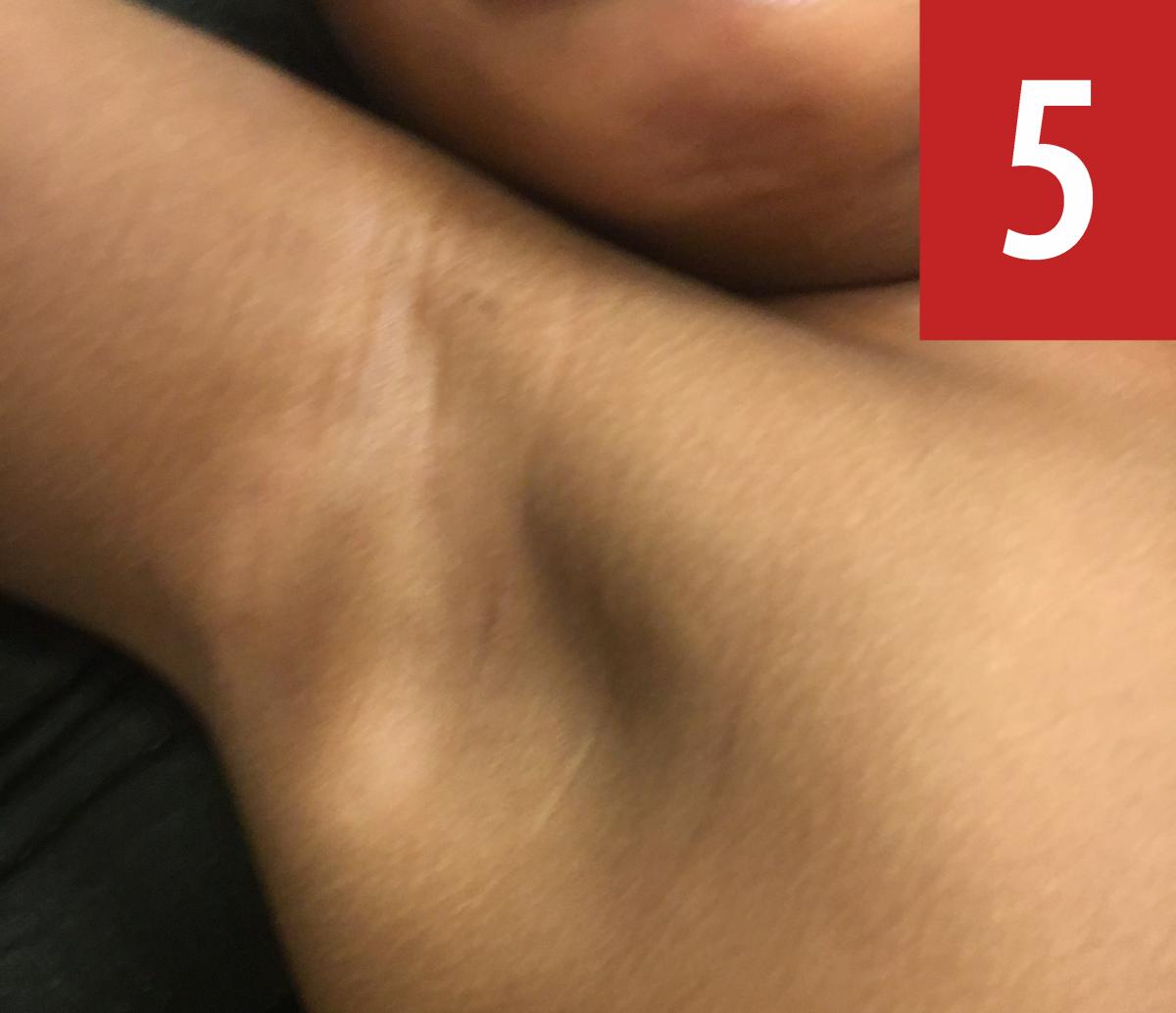
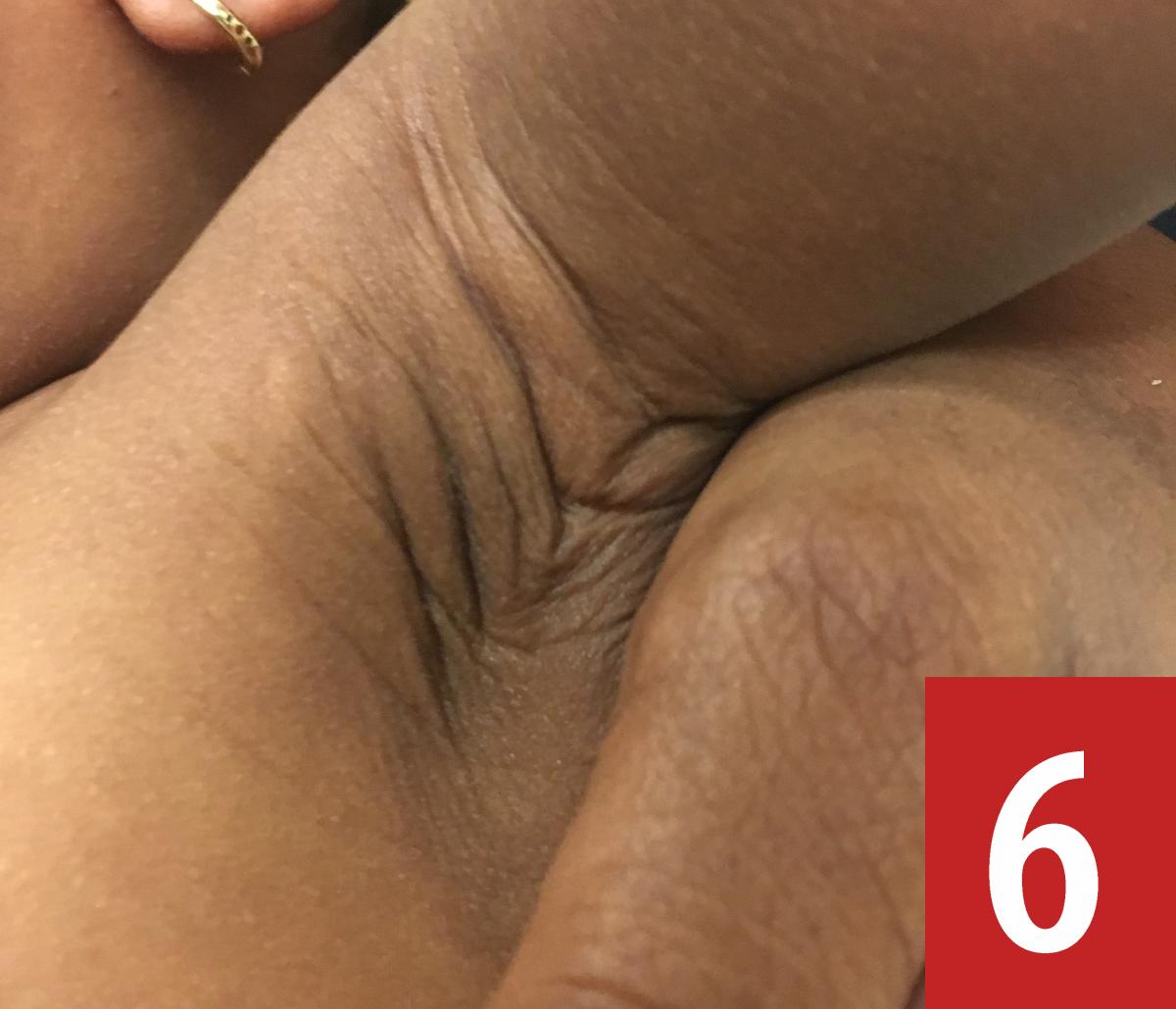

Diagnostic tests. Although there was no family history of neurofibromatosis, the girl was referred for magnetic resonance imaging (MRI) of the brain and for genetic and ophthalmologic consultation.
The results of the patient’s MRI scan of the brain were normal, and no Lisch nodules were noted on ophthalmologic examination. However, at a follow-up visit, despite again reporting a negative family history for NF, the patient’s mother permitted the pediatrician to examine her. More than 6 café au lait macules, as well as axillary and inguinal freckling, were noted on the mother. Therefore, a diagnosis of neurofibromatosis type 1 (NF1) was made for both the mother and the daughter at this visit.
Discussion. NF1 is an autosomal dominant disorder characterized by various types of tumors, both benign and malignant, with most involving the nervous system. The condition affects up to 1 in 3000 individuals, and about 50% of cases are due to random de novo mutations.1 NF1 is caused by a mutation of NF1 on the long arm of chromosome 17, subband 11.2, which codes for neurofibromin, a guanosine triphosphatase (GTPase)-activating protein. The loss of function of this protein causes an increase in GTPase activity within affected cells and a resultant dysregulation of cell growth.2
The diagnosis requires the meeting of 2 of 7 criteria (Table).3 Other manifestations can include macrocephaly, hypertension, short stature, and learning disabilities. These can be present at birth or can develop later in childhood; 80% to 85% of NF1 cases are diagnosed by 6 years and 90% by 8 years. Café au lait macules are usually the first to appear, followed by freckling, neurofibromas, and, finally, Lisch nodules. Treatment is based on symptomatology.2

Vitiligo is a loss of melanocytes that results in depigmented patches of skin. Although the cause is unknown, it may be due to an autoimmune process and may involve genetic and environmental etiologies.4 Diagnosis is based on clinical examination, and management consists of immunosuppressants including corticosteroids, calcineurin inhibitors, and UV radiation.5 The coexistence of NF1 and vitiligo, although rare, has been reported.6,7 It is hypothesized that a decrease in functional neurofibromin may reduce expression of Fas ligand, a molecule necessary for apoptosis. This decreases CD4+ lymphocyte apoptosis and contributes to the autoimmune process in vitiligo.7 Studies show that NF1 is also associated with other autoimmune diseases.8,9
NF1 can coexist with cutaneous and visceral hemangiomas, as documented in reports in both pediatric and adult patients.10,11,12 The mechanism is not fully understood, although several genes have been implicated.13 Patients can present with café au lait macules and hemangiomas as early as 2 to 3 weeks of age.10 Hemangiomas may slowly involute, and they have been treated with corticosteroids, interferons and other biologic agents, and, more recently, oral propranolol or topical timolol.11
References:
- Friedman JM. Epidemiology of neurofibromatosis type 1. Am J Med Genet. 1999;89(1):1-6.
- Boyd KP, Korf BR, Theos A. Neurofibromatosis type 1. J Am Acad Dermatol. 2009;61(1):1-14.
- Ferner RE, Huson SM, Thomas N, et al. Guidelines for the diagnosis and management of individuals with neurofibromatosis 1. J Med Genet. 2007;44(2):81-88.
- Passeron T, Ortonne J-P. Physiopathology and genetics of vitiligo. J Autoimmun. 2005;25 suppl:63-68.
- Hossani-Madani AR, Halder RM. Topical treatment and combination approaches for vitiligo: new insights, new developments. G Ital Dermatol Venereol. 2010;145(1):57-78.
- Bukhari I, Al Mulhim F. Neurofibromatosis type 1 associated with vitiligo and left occipital bone defect. Internet J Dermatol. 2006;6(1). https://print.ispub.com/api/0/ispub-article/4167. Accessed April 4, 2018.
- Yalcın B, Tamer E, Gür G, Öztas P, Polat MÜ, Allı N. Neurofibromatosis 1/Noonan syndrome associated with Hashimoto’s thyroiditis and vitiligo. Acta Derm Venereol. 2006;86(1):80-81.
- Nabi J. Neurofibromatosis type 1 associated with Hashimoto’s thyroiditis: coincidence or possible link. Case Rep Neurol Med. 2013;2013:910656. doi:10.1155/2013/910656
- Nanda A. Autoimmune diseases associated with neurofibromatosis type 1. Pediatr Dermatol. 2008;25(3):392-393.
- Oiso N, Iba Y, Kawara S, Kawada A. Halo phenomenon in neurofibromas and generalized vitiligo in a patient with neurofibromatosis type 1. Clin Exp Dermatol. 2007;32(2):207-208.
- Pascual-Castroviejo I, Parrón Pajares M, Pascual-Pascual S-I, Jara P, Velázquez-Fragua R. Cutaneous, mediastinal and hepatic hemangiomas in a girl followed during 12 years. Neuropediatrics. 2011;42(1):24-27.
- Haitz K, Mikailov A, Foreman R, Zimarowski MJ, Seo S-J. Recurrent lobular capillary hemangiomas in a patient with neurofibromatosis type 1 (NF1) and von Hippel-Lindau syndrome (VHL). JAAD Case Rep. 2015;1(6):368-370.
- Kansal R, Li X, Shen J, et al. An infant with MLH3 variants, FOXG1-duplication and multiple, benign cranial and spinal tumors: a clinical exome sequencing study. Genes Chromosomes Cancer. 2016;55(2):131-142.


