Wrist-Ankle Acupuncture Enhances Acute Herpes Zoster Pain Relief When Combined With Standard Therapy
Key Highlights
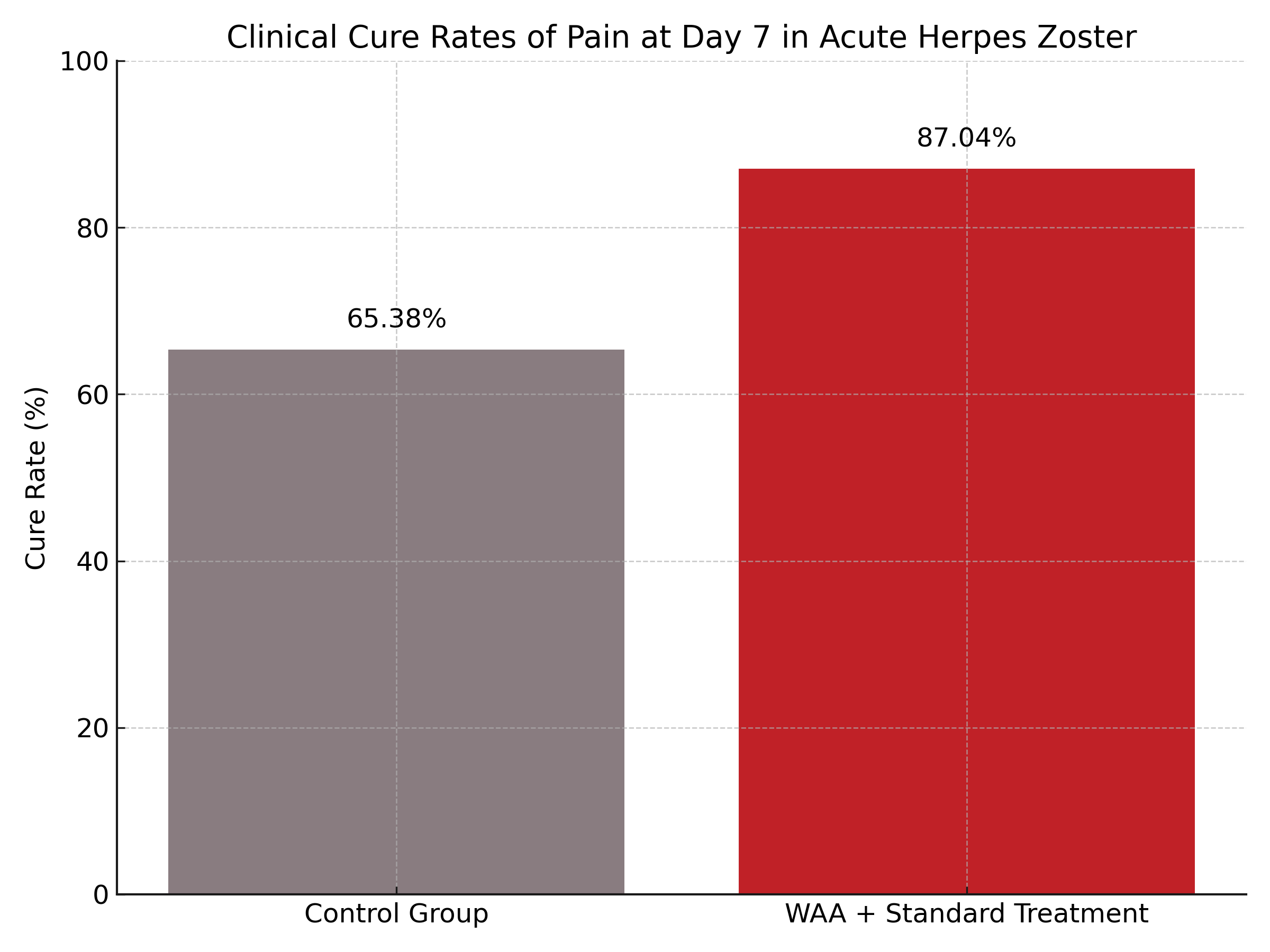
- Wrist-ankle acupuncture (WAA) combined with standard pharmacological treatment significantly improved pain cure rates at day 7 (87.04% vs 65.38%, P < .005).
- Pain scores were significantly lower in the WAA group from days 2–6 of treatment (P < .05).
- Dermatology Life Quality Index scores improved more in the WAA group at discharge (P < .05).
- No increase in adverse effects was observed with the addition of WAA.
In a randomized controlled trial evaluating pain relief strategies for acute herpes zoster (HZ), the combination of wrist-ankle acupuncture (WAA) and standard pharmacological therapy demonstrated superior outcomes compared with pharmacologic treatment alone. The addition of WAA significantly enhanced clinical pain cure rates by day 7 and resulted in faster pain reduction during the early days of treatment, without increasing adverse events.
Despite antiviral and analgesic therapies being standard for acute HZ, many patients continue to experience substantial pain, and current treatment regimens carry risks of nephrotoxicity and other side effects. There is limited exploration of alternative, non-pharmacological interventions. Acupuncture, including the WAA technique, has emerged as a promising candidate due to its safety profile and potential for systemic pain relief. This study sought to determine whether the integration of WAA into conventional treatment could yield improved outcomes in acute HZ management.
This open-label, randomized, controlled clinical trial enrolled 106 adult inpatients with confirmed acute HZ and baseline VAS pain scores of 2 or more. Participants were randomly assigned to either receive standard pharmacological treatment (antivirals and pain relievers) or the same regimen plus daily 30-minute WAA for 7 days. VAS scores were measured on days 1–7 and day 28, and Dermatology Life Quality Index (DLQI) scores were assessed before treatment and at discharge. Clinical cure was defined as complete pain resolution, and outcomes were evaluated using intention-to-treat analysis.
Results showed a significantly higher clinical cure rate in the WAA group by day 7 (87.04% vs 65.38%, P < .005). VAS scores from days 2 through 6 were consistently lower in the WAA group compared to controls (P < .05), although differences diminished by day 28. DLQI scores, which assess the impact of skin disease on quality of life, significantly improved in both groups, with greater reductions observed in the WAA group at discharge (P < .05). Importantly, the incidence of side effects, including nephrotoxicity and gastrointestinal symptoms, did not differ significantly between groups.
Limitations of the study include its open-label design, potential placebo effects from increased healthcare interaction in the WAA group, and single-center setting. Additionally, pain assessments relied on subjective patient reporting, and the study's post-hoc power narrowly missed the predefined threshold of 0.80.
“The findings suggest that WAA combined with standard pharmacological treatment may potentially improve the pain cure rate at 7 days post-treatment, thus providing a novel approach for pain management in patients in the acute phase of HZ,” the study authors concluded.
Reference:
Pu J, Li D, Luo X, et al. Wrist-ankle acupuncture alleviates pain in the acute phase of herpes zoster: A randomized controlled trial. PLoS One. 2025;20(5):e0318386. Published 2025 May 29. doi:10.1371/journal.pone.0318386


