Isotretinoin Effective in Treating Acne Among Transgender and Gender-Diverse Individuals Receiving Masculinizing Hormone Therapy
Key Highlights
- Isotretinoin led to acne improvement in 87.3% and clearance in 47.3% of transgender and gender-diverse patients receiving masculinizing hormone therapy.
- Higher cumulative dosing (≥120 mg/kg) was associated with improved outcomes: 97.0% improvement and 63.6% clearance.
- Premature treatment discontinuation was common and correlated with lower treatment success.
Isotretinoin therapy demonstrated high rates of clinical efficacy in transgender and gender-diverse individuals undergoing masculinizing hormone therapy for acne. Among those treated with a cumulative dose of 120 mg/kg or more, 97.0% showed improvement and 63.6% achieved complete clearance. However, early discontinuation was frequent and contributed to suboptimal outcomes.
Acne is a prevalent adverse effect of masculinizing gender-affirming hormonal therapy, yet data on effective acne treatments in this population are limited. Isotretinoin is a potent intervention for severe acne, but its safety and efficacy profile among transgender and gender-diverse individuals receiving testosterone remains underexplored.
This multicenter retrospective case series included 55 transgender and gender-diverse patients aged 12 to 49 years who received isotretinoin between 2015 and 2023 across four institutions: Mass General Brigham, University of Pennsylvania, Emory University, and Fenway Health. All participants were undergoing masculinizing hormonal therapy at the time of acne treatment. The investigators evaluated clinical response, recurrence rates, adverse effects, and reasons for treatment discontinuation.
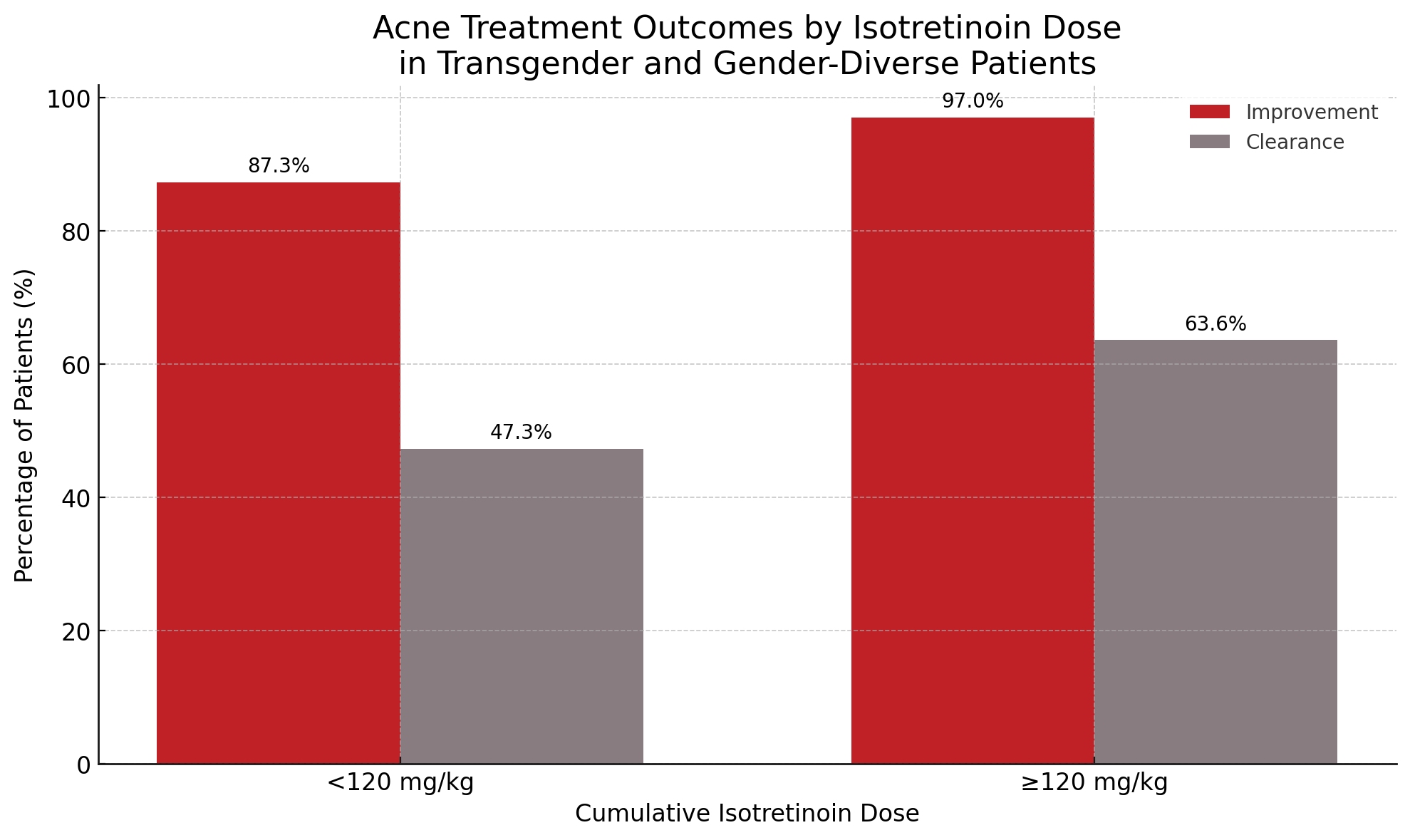
Across the cohort, the median isotretinoin course duration was 6 months, and the median cumulative dose was 132.7 mg/kg. Acne improvement occurred in 87.3% (n = 48) of patients and clearance in 47.3% (n = 26). When limited to those who received at least 120 mg/kg, outcomes improved further, with 97% (n = 32) experiencing improvement and 63.6% (n = 21) achieving clearance. Recurrence among those with follow-up was 20.0%. Adverse effects included dryness (80.0%), joint pain (14.5%), and eczema (9.1%), while lab abnormalities were uncommon. Treatment discontinuation was linked to multiple factors, such as cost, pharmacy barriers, scheduling, adverse effects, and concerns related to upcoming gender-affirming surgeries.
“In this case series study of individuals with acne who were receiving masculinizing gender-affirming hormonal therapy and underwent isotretinoin treatment, isotretinoin was often effective and well tolerated,” the study authors concluded. “However, premature treatment discontinuation was common and associated with poorer outcomes. Further efforts are needed to understand optimal dosing and treatment barriers to improve outcomes in transgender and gender-diverse individuals receiving masculinizing gender-affirming hormonal therapy.”
Reference:
Choe J, Shields A, Ferreira A, et al. Isotretinoin for acne in transgender and gender-diverse individuals receiving masculinizing hormone therapy. JAMA Dermatol. 2024;160(7):741-745. doi:10.1001/jamadermatol.2024.1420


