Systemic Lupus Erythematosus
Photoclinic
Foresee Your Next Patient
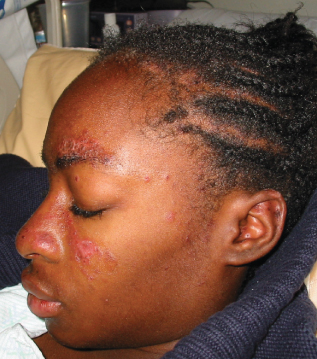
 For 2 weeks, this 13-year-old girl felt tired and achy. She had persistent fevers (temperature up to 38.8°C [102°F]) and an erythematous facial rash above her eyebrows that extended to her cheeks and nasal bridge and spared the nasolabial folds. She had applied a topical acne medication to the rash but noted no improvement. She also reported decreased oral intake because of discomfort from palatal ulcers. She had no significant medical or family history.
For 2 weeks, this 13-year-old girl felt tired and achy. She had persistent fevers (temperature up to 38.8°C [102°F]) and an erythematous facial rash above her eyebrows that extended to her cheeks and nasal bridge and spared the nasolabial folds. She had applied a topical acne medication to the rash but noted no improvement. She also reported decreased oral intake because of discomfort from palatal ulcers. She had no significant medical or family history.
Results of laboratory studies included a white blood cell (WBC) count of 3100/µL; hemoglobin,
10.3 g/dL; hematocrit, 31%; platelet count, 158,000/µL; blood urea nitrogen, 20 mg/dL; creatinine, 1.2 mg/dL; aspartate aminotransferase, 47 U/L (range, 0 to 35 U/L); alanine aminotransferase, 75 U/L (range, 1 to 30 U/L); antinuclear antibody (ANA) titer, 1:1280; C3, 32 mg/dL (range, 90 to 180 mg/dL); C4, 8 mg/dL (range, 16 to 47 mg/dL); complement CH50, less than 13 U/mL (range, 31 to 66 U/mL); direct Coombs IgG-positive, Smith antibodies indirect hemagglutination assay titer, 1:800; erythrocyte sedimentation rate, 45 mm/h (range, 0 to 20 mm/h). Routine urinalysis showed proteinuria (100 mg/dL), 15 WBCs, and 8 red blood cells, with moderate values for leukocyte esterase and blood. An echocardiogram showed normal valve function and no vegetations. An abdominal ultrasonogram revealed hepatomegaly.
The patient was hospitalized, and the rheumatology team was consulted. Systemic lupus erythematosus (SLE) was diagnosed on the basis of the clinical history and physical findings, particularly the malar facial rash and oral ulcers. Laboratory studies supporting the diagnosis included the elevated ANA titer; hypocomplementemia; anemia; nephritis, with an elevated creatinine level for age; elevated levels of hepatic transanimases; the positive direct Coombs test result, reflective of a hemolytic process; and the presence of anti-Smith antibodies.1 After treatment with intravenous methylprednisolone sodium succinate, she clinically improved and was discharged. Her daily medications included prednisone, hydroxychloroquine, and an H2 blocker for gastric coverage while taking oral corticosteroids.2 Outpatient follow-up with rheumatology and ophthalmology were scheduled because of the increased risk of retinitis with use of hydroxychloroquine.3
 SLE (lupus) is a chronic autoimmune disorder characterized by multisystem microvascular inflammation, with the production of autoantibodies. Recurrent episodes of relapse and remittance occur. A defined cause is unknown. Factors involved in the development of SLE are race, genetics, hormonal changes, and the environment.4 The incidence in patients aged 10 to 18 years varies among different populations; in the United States, it is highest among African Americans.5 As with other autoimmune diseases, females are affected more often than males. Onset of symptoms typically occurs after age 5 years; the incidence increases after age 10 years.1 Hormonal changes associated with puberty and pregnancy can trigger the disease.6 Genetic probability is increased in first-degree relatives with lupus and in identical twins.4
SLE (lupus) is a chronic autoimmune disorder characterized by multisystem microvascular inflammation, with the production of autoantibodies. Recurrent episodes of relapse and remittance occur. A defined cause is unknown. Factors involved in the development of SLE are race, genetics, hormonal changes, and the environment.4 The incidence in patients aged 10 to 18 years varies among different populations; in the United States, it is highest among African Americans.5 As with other autoimmune diseases, females are affected more often than males. Onset of symptoms typically occurs after age 5 years; the incidence increases after age 10 years.1 Hormonal changes associated with puberty and pregnancy can trigger the disease.6 Genetic probability is increased in first-degree relatives with lupus and in identical twins.4
Commonly reported symptoms of lupus at initial presentation are fever, fatigue, and malaise of several months’ duration. Arthritis of the small joints in the hands and wrists and renal disease (nephritis or nephrosis) may manifest during this time.1 Presence of a malar rash is helpful for diagnosis; however, it occurs in only two-thirds of patients with SLE. The rash is usually a fixed (flat or raised) erythema that tends to spare the nasolabial folds. It can be painful or pruritic. Other cutaneous features are photosensitivity, a discoid rash that develops in sun-exposed areas (which may appear plaquelike with follicular plugging and scarring), and alopecia of the temporal regions.1 Hematological abnormalities of SLE are anemia, cytopenia, and thrombocytopenia.7 Associated cardiopulmonary conditions include pericarditis, endocarditis, coronary artery disease (early-onset atherosclerosis), and pleural disease.4
Neuropsychiatric manifestations (such as loss of academic performance, depression, and social isolation) can be indicators of SLE; thus, it is important to perform a workup for lupus in patients with isolated neuropsychiatric findings.8 More severe neurological presentations are seizures (20% of patients), and psychosis.9
Overall, the prognosis for patients with lupus is good. Poor outcomes are a result of limited access to health care and nonadherence to treatment regimens, which can lead to neurological complications, intercurrent infections, and extensive renal disease (such as diffuse proliferative glomerulonephritis).10 Survival rates are cited as 100% at 5 years and 85% at 10 years after diagnosis.11 The Lupus Foundation of America (http://www.lupus.org) is a helpful resource for clinicians and families. ■
1. Hiraki LT, Benseler SM, Tyrrell PN, et al. Clinical and laboratory characteristics and long-term outcome of pediatric systemic lupus erythematosus: a longitudinal study. J Pediatr. 2008;152:550-556.
2. Carreno L, Lopez-Longo FJ, Gonzalez CM, Monteagudo I. Treatment options for juvenile-onset systemic lupus erythematosus. Paediatr Drugs. 2002;4:241-256.
3. Bernstein HN. Ocular safety of hydroxychloroquine sulfate (Plaquenil). South Med J. 1992;85:
274-279.
4. D’Cruz DP, Khamashta MA, Hughes GR. Systemic lupus erythematosus. Lancet. 2007;369:
587-596.
5. Lim SS, Drenkard C, McCune WJ, et al. Population-based lupus registries: advancing our epidemiologic understanding. Arthritis Rheum. 2009;61:1462-1466.
6. Costenbader KH, Feskanich D, Stampfer MJ, Karlson EW. Reproductive and menopausal factors and risk of systemic lupus erythematosus in women. Arthritis Rheum. 2007;56:1251-1262.
7. McNeil HP, Chesterman CN, Krilis SA. Immunology and clinical importance of antiphospholipid antibodies. Adv Immunol. 1991;49:193-280.
8. Brunner HI, Ruth NM, German A, et al. Initial validation of the Pediatric Automated Neuropsychological Assessment Metrics for childhood-onset systemic lupus erythematosus. Arthritis Rheum. 2007;57:1174-1182.
9. Steinlin MI, Blaser SI, Gilday DL, et al. Neurologic manifestations of pediatric systemic lupus
erythematosus. Pediatr Neurol. 1995;13:191-197.
10. McCurdy DK, Lehman TJ, Bernstein B, et al. Lupus nephritis: prognostic factors in children.
Pediatrics. 1992;89:240-246.
11. Ruperto N, Ravelli A, Cuttica R, et al; Pediatric Rheumatology International Trials Organization (PRINTO); Pediatric Rheumatology Collaborative Study Group (PRCSG). The Pediatric Rheumatology International Trials Organization criteria for the evaluation of response to therapy in juvenile systemic lupus erythematosus: prospective validation of the disease activity core set. Arthritis Rheum. 2005;52:2854-2864.


