Oral Histoplasmosis



A 39-year-old woman complained of excruciating pain that radiated from a chronic lesion on the left upper lip to the entire left side of the face. She had AIDS (CD4+ cell count, 68/µL; HIV RNA level, greater than 750,000 copies/mL) but was not receiving antiretroviral therapy. The lesion first appeared as a blister, which ruptured after it was struck by a toy thrown by her son. It enlarged and became more painful despite antibiotic therapy and a 1-month course of valacyclovir. During this period, she had no fever. She used marijuana and alcohol for pain control.
The patient grew up in Puerto Rico and had been in prison there. There was no history of tuberculosis. She had a pet dog.
The patient was afebrile; blood pressure, 130/70 mm Hg; heart rate, 88 beats per minute; and respiration rate, 12 breaths per minute. The sclerae were anicteric. There was a perioral ulcer with significant swelling of the left upper lip (Figure 1). No oral candidiasis was seen. She had torus palatinus and an enlarged left submandibular gland with mild cervical and axillary lymphadenopathy. There were no other skin lesions and no genital lesions.
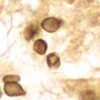
Biopsies of the lip lesion revealed findings consistent with cheilitis granulomatosa (Figure 2). Characteristic yeast forms of 2 to 3 µm in diameter, often with single buds attached by narrow necks, were seen with Gomori methenamine-silver stain (Figure 3). Culture grew Histoplasma capsulatum macroconidia (Figure 4). Results of a urine Histoplasma antigen test showed 18.29 enzyme immunoassay (EIA) units (less than 1 EIA unit is negative; greater than 10 EIA units is high positive: MiraVista Diagnostics, Indianapolis).
The patient was treated with intravenous amphotericin B for 1 week followed by oral itraconazol. After 2 weeks, the lip lesion had completely healed, the facial pain had resolved, and the urine Histoplasma antigen level had decreased to 14.7 EIA units. Itraconazole was continued for 2 more weeks, and the patient was asked to return for antiretroviral therapy. Unfortunately, she was lost to follow-up.
HISTOPLASMOSIS: AN OVERVIEW
H capsulatum exists in a yeast form at 37ºC (98.6ºF) and as mycelium at 25ºC (77ºF) to 30ºC (86ºF).1 This dimorphic soil fungus is endemic in the central and southeastern United States, in Puerto Rico, and in regions of South America. Infection results from inhalation of spores found in the excreta of pi- geons and other birds and bats and in chicken coops.1
The disease is usually classified as acute pulmonary, chronic cavitary, or disseminated.2 Disseminated disease can occur in persons who are very young, very old, or immunocompromised (such as those with HIV/AIDS). It has been observed in persons living in the United States who had previously lived in regions where H capsulatum is endemic. Some speculate that the disease in these patients may be caused by reactivation of quiescent infection.3
CLINICAL PRESENTATION
Oral presentations of disseminated histoplasmosis in patients with AIDS have been reported, even in those who have no other signs of the disseminated disease (eg, fever, weight loss, respiratory complaints, hepatomegaly, splenomegaly, anemia).4-6 The lips, palate, gingiva, tongue, and pharynx may be affected. The lesions can be single or multiple and have been described as erosive, often covered by hemorrhagic crust; nodular; papillary; ulcerative with heaped-up edges; and ulcero-vegetating, mimicking squamous cell carcinoma.2,7,8 In one series, patients with disseminated histoplasmosis who had low CD4+ cell counts (mean, 29/µL) were more likely to have oral lesions.7
DIAGNOSIS
The diagnosis is facilitated by biopsy of the oral lesions for microscopic evaluation and culture. Histological findings range from histiocytic aggregation to granuloma formation.2 Spherical to oval intracellular or extracellular yeast forms, often with a single bud attached by narrow necks, can be seen with periodic acid-Schiff or Gomori methenamine-silver stain.9
H capsulatum can develop into a hairlike white to gray-tan mold on enriched fungal culture media after 10 to 30 days of incubation at room temperature.9 Urine Histoplasma antigen has a 92% sensitivity in patients with disseminated histoplasmosis and has a turnaround time of 4 to 7 days for results.1 Special stains for mycobacterial organisms, cytomegalovirus, and herpes simplex virus, as well as stains for tumor markers, along with viral and mycobacterial cultures would exclude other conditions in the differential diagnosis.
TREATMENT
Amphotericin B, deoxycholate or liposomal, and itraconazole are used to treat histoplasmosis. For the initial treatment of disseminated histoplasmosis, amphotericin B is used. If this agent is not tolerated or if significant improvement occurs (usually after 3 to 10 days of amphotericin B therapy), itraconazole can be substituted.10 Oral lesions usually resolve within 6 weeks of therapy.7,8 However, life-long therapy with itraconazole should be maintained to prevent recurrence of disseminated histoplasmosis in patients who have AIDS, even if their CD4+ cell count increases to greater than 100/µL with antiretroviral therapy.10
1. Wheat LJ, Kauffman CA. Histoplasmosis. Infect Dis Clin North Am. 2003;17:1-19, vii.
2. Goodwin RA Jr, Shapiro JL, Thurman GH, et al. Disseminated histoplasmosis: clinical and pathologic correlations. Medicine (Baltimore). 1980;59:1-33.
3. Mandal B. AIDS and fungal infections. J Infect. 1989;19:199-205.
4. Chinn H, Chernoff DN, Migliorati CA, et al. Oral histoplasmosis in HIV-infected patients. A report of two cases. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 1995;79:710-714.
5. Economopoulou P, Laskaris G, Kittas C. Oral histoplasmosis as an indicator of HIV infection. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 1998; 86:203-206.
6. Gomes Ferreira O, Vieria Fernandes A, Sebastião Borges A, et al. Orofacial manifestations of histoplasmosis in HIV-positive patients: a case report. Med Oral. 2001;6:101-105.
7. Couppie P, Clyti E, Nacher M, et al. Acquired immunodeficiency syndrome-related oral and/or cutaneous histoplasmosis: a descriptive and comparative study of 21 cases in French Guiana. Int J Dermatol. 2002;41:571-576.
8. Cohen PR, Grossman ME, Silvers DN. Disseminated histoplasmosis and human immunodeficiency virus infection. Int J Dermatol. 1991;30:614-622.
9. Koneman EW, Allen SD, Janda WM, et al, eds. Color Atlas and Textbook of Diagnostic Microbiology. 5th ed. Philadelphia: Lippincot Williams & Wilkins; 1997:1029-1032.
10. Benson CA, Kaplan JE, Masur H, et al. Treating opportunistic infections among HIV-exposed and infected children: recommendations from CDC, the National Institutes of Health, and the Infectious Diseases Society of America. MMWR. 2004;53(RR-15): 1-112.


