Peer Reviewed
Erythema Multiforme
Author:
Joe R. Monroe, MPAS, PA
Epiphany Dermatology, Tulsa, Oklahoma
Citation:
Monroe JR. Erythema multiforme [published online February 11, 2019]. Consultant360.
A 34-year-old man was referred to a dermatology practice by an urgent care provider for evaluation of a mildly pruritic rash that had been present for a week on his hands and knees. The patient had not been ill in the period leading up to the appearance of the rash. The only change had been the initiation of ibuprofen therapy for newly diagnosed mild osteoarthritis.
Physical examination. Discrete, round, targetoid, pink, edematous papules and patches were present on the patient’s palms (Figure). They ranged in size from 5 mm to 2 cm and covered most of both palms. Similar but smaller lesions were present on both knees. There was no epidermal component (eg, scale, broken skin) and no tenderness on palpation.
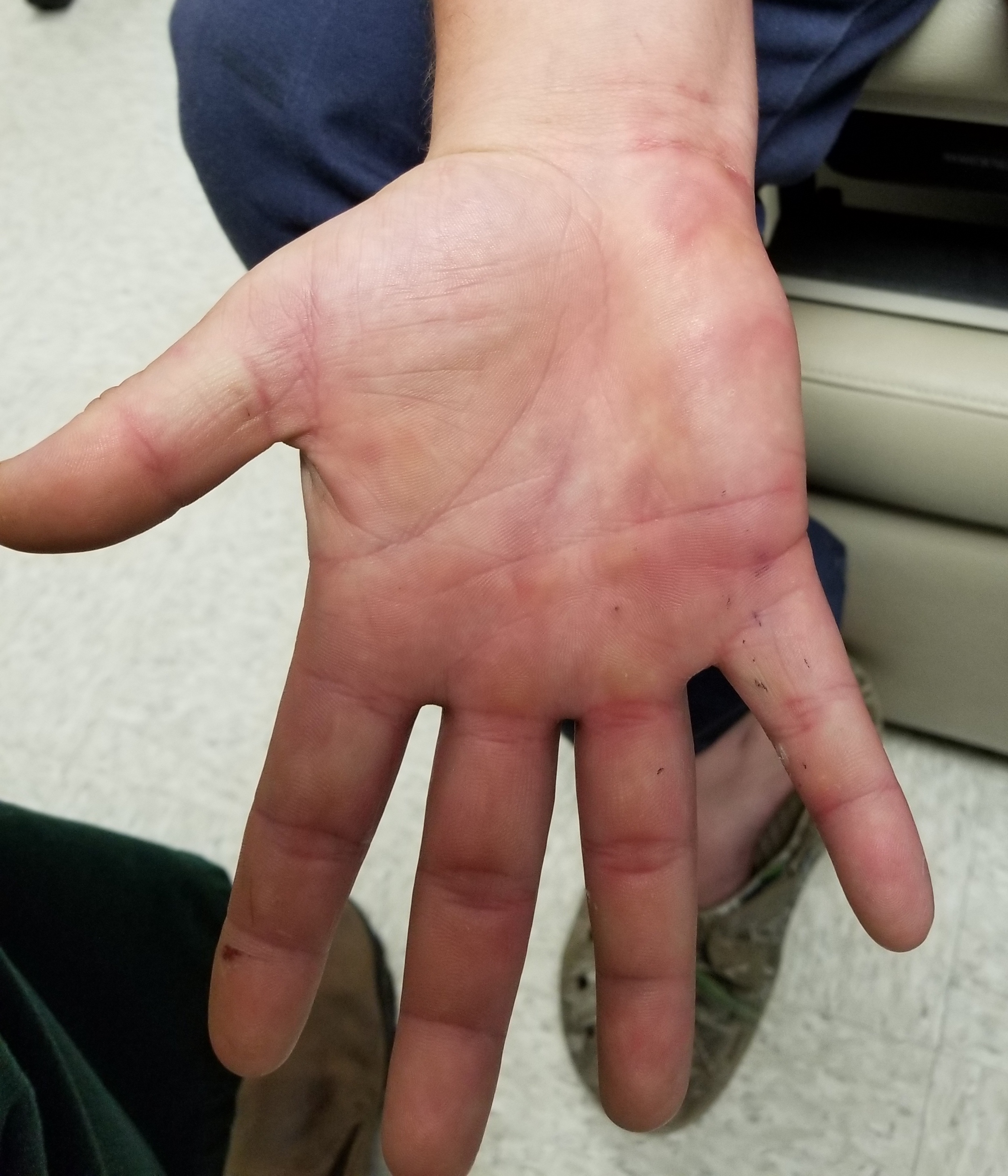
Discussion. This is a typical case of erythema multiforme (EM), a reactive hypersensitivity reaction triggered by microorganisms or drugs. At least 50% of EM cases are thought to be triggered by herpes simplex virus (HSV) infection, and among drugs, nonsteroidal anti-inflammatory drugs, penicillin, tetracycline, anticonvulsants, and sulfa-based drugs predominate as triggers.
The pathophysiologic mechanism of EM appears to be the deposition of immune complexes, mostly immunoglobulin M-bound, in the superficial microvasculature of skin, and occasionally, in mucous membranes.
This patient’s case would be classified as EM minor, but a minority of EM cases are more serious, causing frank blistering and covering larger areas of the body, including mucous membranes or even the conjunctivae.
Until recently, EM minor had been viewed as being at the low end of a continuum that included the more serious conditions of EM major, Stevens-Johnson syndrome, and toxic epidermal necrolysis. However, the consensus is now that EM minor is its own distinctive entity.
The term multiforme implies that this condition can take on many morphologic appearances, but in any given case, the lesions are typically monomorphic. In many cases, including this one, EM lesions can appear urticarial; however, the lesions persist for up to 2 or even 3 weeks, whereas episodes of true urticaria arise suddenly and clear within 12 hours at most. In addition, EM lesions are often more obviously targetoid than in the ones in this case. The bilateral symmetric palmar involvement is classic for EM, which can also affect the soles and mucous membranes.
Because of the broad differential diagnosis, biopsies are occasionally necessary, the results of which show dermal edema and necrotic keratinocytes. Urticaria, fixed drug eruption, and a wide variety of blistering diseases can present somewhat similarly.
Treatment is usually a matter of either recognizing and treating HSV infection (which can be chronic or even subclinical, requiring prophylactic therapy) or discontinuing the offending medication.


