Peer Reviewed
An Atlas of Lumps and Bumps, Part 4
AUTHORS:
Alexander K. C. Leung, MD1,2 —Series Editor • Benjamin Barankin, MD3 • Joseph M. Lam, MD4 • Kin Fon Leong, MD5
AFFILIATIONS:
1Department of Pediatrics, University of Calgary, Calgary, Alberta, Canada
2Alberta Children’s Hospital, Calgary, Alberta, Canada
3Toronto Dermatology Centre, Toronto, Ontario, Canada
4Department of Pediatrics and Department of Dermatology and Skin Sciences, University of British Columbia, Vancouver, British Columbia, Canada
5Pediatric Institute, Kuala Lumpur General Hospital, Kuala Lumpur, Malaysia
CITATION:
Leung AKC, Barankin B, Lam JM, Leong KF. An atlas of lumps and bumps, part 4. Consultant. 2021;61(5):e20-e22. doi:10.25270/con.2021.05.00001
DISCLOSURES:
Dr Leung is the series editor. He was not involved with the handling of this paper, which was sent out for independent external peer review.
CORRESPONDENCE:
Alexander K. C. Leung, MD, #200, 233 16th Ave NW, Calgary, AB T2M 0H5, Canada (aleung@ucalgary.ca)
EDITOR’S NOTE:
This article is part of a series describing and differentiating dermatologic lumps and bumps. To access previously published articles in the series, visit https://bit.ly/35J1I1v.
Angiokeratoma of Fordyce
“Angiokeratoma” (derived from 3 Greek words meaning vessels, horn, and tumor, respectively) refers to a benign vascular lesion in the papillary dermis characterized by ectasia of blood vessels often accompanied by overlying hyperkeratosis.1-3 In angiokeratoma of Fordyce, the angiokeratoma is most often situated on the scrotum in men and labia majora in women.3 Angiokeratoma of Fordyce usually develops in individuals aged older than 40 years.4,5 The condition is most common in White and Japanese populations.2 In a cross-study of 213 White/European American adults (127 men and 86 women), angiokeratomas of Fordyce were detected in 47 (37.0%) men and 17 (19.8%) women.6 Presence of at least 1 angiokeratoma of Fordyce was significantly associated with male sex (OR, 2.4; 95% CI, 1.3-4.5; p < 0.001) and age older than 50 years (OR, 3.4; 95% CI, 1.7-6.7; p < 0.008).6 In the older age group, the condition may be associated with conditions with increased localized venous pressure such as inguinal hernia, thrombophlebitis of the scrotum, and varicocele.3,7-9 However, in patients younger than age 20 years, usually no such association exists.9 On the other hand, angiokeratoma of Fordyce may be the first sign of Fabry disease, a rare inherited lysosomal storage disorder caused by deficiency of α-galactosidase A.7,10
Clinically, angiokeratoma of Fordyce presents as multiple, well-circumscribed, dome-shaped papules, 2 to 5 mm in diameter mainly on the scrotum in men (Figures 1 and 2) and labia majora in women (Figure 3).1,3,11,12 Rarely, the lesions can be found on the prepuce, glans penis, and penile shaft in men and clitoris in women.1,3 Lesions on the inguinal folds, lower abdomen, buttocks, and inner thighs have very rarely been reported.2-4,10 The lesions are usually bilateral, although unilateral angiokeratomas have rarely been reported.4,10,13
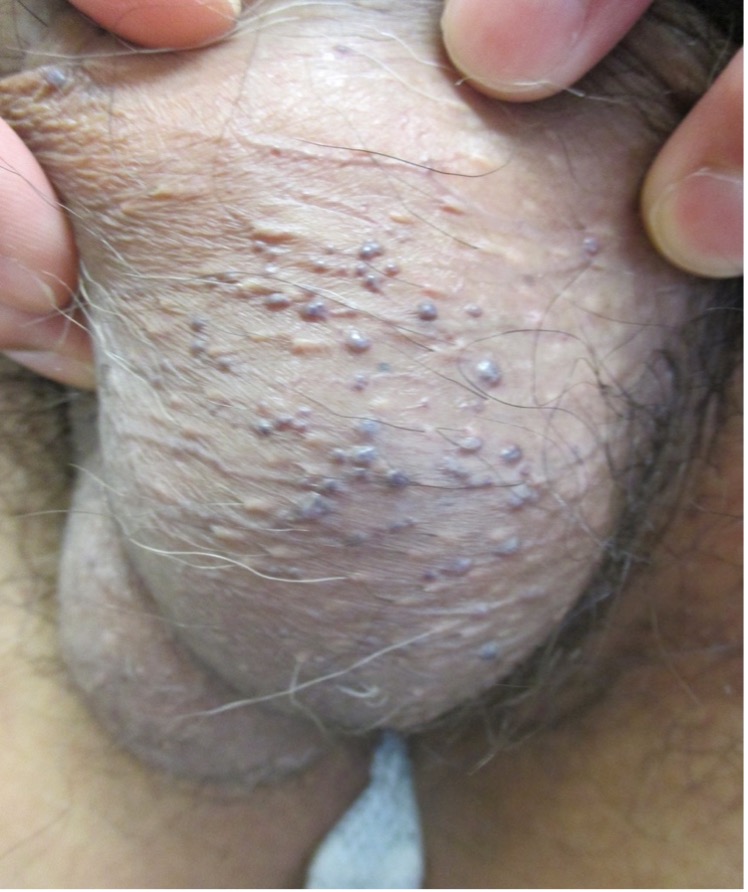
Figure 1. Angiokeratoma of Fordyce presents as multiple, well-circumscribed, dome-shaped papules mainly on the scrotum in men.

Figure 2. Angiokeratoma of Fordyce presents as multiple, well-circumscribed, dome-shaped papules mainly on the scrotum in men.

Figure 3. Angiokeratoma of Fordyce presents as multiple, well-circumscribed, dome-shaped papules mainly on the labia majora in women.
The color of the lesions may be black, bluish-black, dark red, red, purple, or blue.3,7 Newer lesions are often smaller, red, shiny, soft, compressible, and smooth, while longstanding lesions are often larger, darker, firm, noncompressible, keratotic, scaly, and sometimes warty.3,6,7 Confluence of telangiectases may lead to a red scrotum.3,7 Most lesions are asymptomatic but irritation, pain, burning sensation, pruritus, and bleeding may occasionally occur.5
The diagnosis is mainly clinical. The use of dermoscopy facilitates visualization of dark or red lacunae, whitish veil, peripheral erythema, and hemorrhagic crusts, which are features of angiokeratomas.3,10,15
Idiopathic Scrotal Calcinosis
Scrotal calcinosis refers to deposits of insoluble calcium salts (in particular, calcium phosphate) in the scrotal skin leading to the formation of papules and nodules within the scrotal skin. Idiopathic scrotal calcinosis is a rare condition; the exact incidence of which is not known, as information on this condition is mostly derived from case reports.16 The condition typically presents in the third to fourth decades of life.17-19 Idiopathic scrotal calcinosis is more common in dark-skinned individuals, suggesting an ethnic susceptibility.20-22
Scrotal calcinosis may result from dystrophic calcification of an epidermal inclusion cyst, an eccrine epithelial cyst, or a degenerated dartos muscle of the scrotum.18,22,23 Rarely, scrotal calcinosis may result from metastatic calcification secondary to abnormal calcium and phosphate metabolism that predisposes to calcium precipitation, or it may develop de novo.16 When scrotal calcinosis develops de novo, the condition is referred to as idiopathic scrotal calcinosis. Idiopathic scrotal calcinosis occurs in the absence of known tissue injury or systemic disease.16 In particular, the serum calcium, phosphate and parathyroid hormone levels are normal in patients with idiopathic scrotal calcinosis.23 There is no evidence of residual cyst and epithelial lining around the calcified nodule.23-25
Scrotal calcinosis is characterized by multiple, slow-growing, firm to hard, papules or nodules within the scrotal skin (Figures 4 and 5).18,24,26 However, lesions may be solitary or pedunculated.18 The lesions tend to increase in size and number with time.27 They are initially skin-colored but may become whitish to yellowish or brownish over time (Figures 4 and 5).26,27 The lesions vary from 2 mm to 2 cm in diameter.16 Scrotal calcinosis is usually bilateral and asymptomatic.18 Uncommonly, the lesions may be mildly itchy or painful.18,27 Some patients may experience a feeling of heavy or dragging sensation in the scrotum.17 Lesions may break down spontaneously or when compressed to produce a white chalky material.17

Figure 4. Scrotal calcinosis is characterized by multiple, slow-growing, firm to hard, papules or nodules within the scrotal skin.
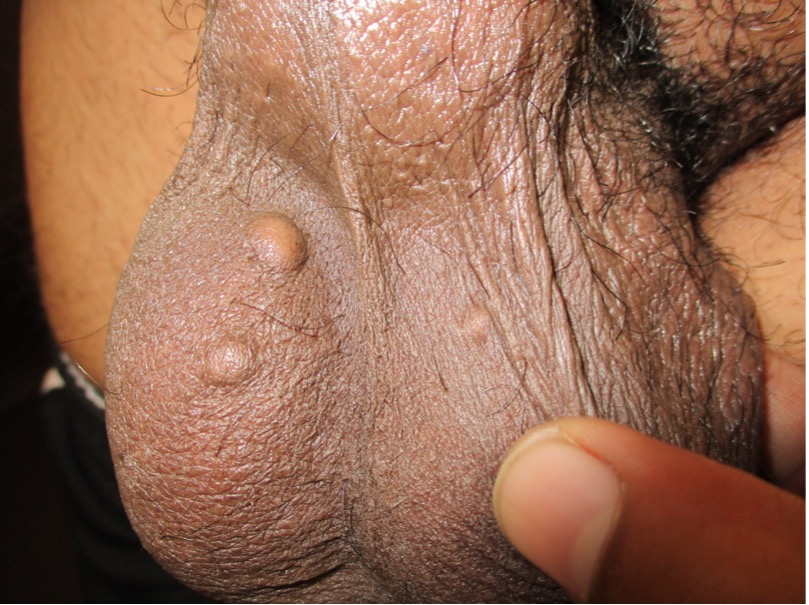
Figure 5. Nodules are initially skin-colored but may become whitish to yellowish or brownish over time.
Idiopathic scrotal calcinosis is benign but can be socially embarrassing. Affected individuals may have low self-esteem and fear of sexual dysfunction, which may affect intimate relationships with sexual partners.17,20 As such, the condition may have an adverse effect on quality of life.18,20 Superimposed infection, inflammation, and ulceration of the lesion may also, albeit seldom, occur.22,26,27
The diagnosis is usually a clinical one. A biopsy of the lesion is usually not necessary unless the diagnosis is in doubt. The condition is benign, and the prognosis is good.
References
1. Cohen PR, Celano NJ. Penile angiokeratomas (PEAKERs) revisited: a comprehensive review. Dermatol Ther (Heidelb). 2020;10(4):551-567. https://doi.org/10.1007/s13555-020-00399-3
2. Ibrahim SM. Pulsed dye laser versus long pulsed Nd:YAG laser in the treatment of angiokeratoma of Fordyce: A randomized, comparative, observer-blinded study. J Dermatolog Treat. 2016;27(3):270-274. https://doi.org/10.3109/09546634.2015.1094180
3. Leung AKC, Barankin B. Angiokeratoma of Fordyce. Clin Case Rep Rev. 2015;1(1):4-5. doi:10.15761/CCRR.1000102
4. González-López MA, Consuegra G, Lacalle M, González-Vela MC. Unilateral angiokeratoma of the scrotum (Fordyce's type) associated with a contralateral varicocele. Indian J Dermatol Venereol Leprol. 2017;83(4):470-472. https://doi.org/10.4103/ijdvl.ijdvl_850_14
5. Zeng Y, Zhan K, Xie WL, Lin QZ. Angiokeratoma of Fordyce response to long pulsed Nd:YAG laser treatment. Dermatol Ther. 2016;29(1):48-51. https://doi.org/10.1111/dth.12296
6. Sadowsky LM, Socik A, Burnes A, Rhodes AR. Genital angiokeratomas in adult men and women: prevalence and predisposing factors. J Cutan Med Surg. 2019;23(5):513-518. https://doi.org/10.1177/1203475419861072
7. Baumgartner J, Šimaljaková M. Genital angiokeratomas of Fordyce 595-nm variable-pulse pulsed dye laser treatment. J Cosmet Laser Ther. 2017;19(8):459-464. https://doi.org/10.1080/14764172.2017.1343953
8. Doğan F, Bucak İH. Rare giant angiokeratoma of the vulva: a case report. Balkan Med J. 2017;34(2):163-164. https://doi.org/10.4274/balkanmedj.2014.0724
9. Patrizi A, Neri I, Trevisi P, Landi C, Bardazzi F. Congenital angiokeratoma of Fordyce. J Eur Acad Dermatol Venereol. 1998;10(2):195-196. https://doi.org/10.1111/j.1468-3083.1998.tb00731.x
10. Ghosh SK, Ghosh S, Agarwal M. Multiple giant angiokeratoma of Fordyce on the shaft of the penis masquerading as keratoacanthoma. An Bras Dermatol. 2015;90(3 Suppl 1):150-152. https://doi.org/10.1590/abd1806-4841.20153876
11. Bechara FG, Jansen T, Wilmert M, Altmeyer P, Hoffmann K. Angiokeratoma Fordyce of the glans penis: combined treatment with erbium: YAG and 532 nm KTP (frequency doubled neodynium: YAG) laser. J Dermatol. 2004;31(11):943-945. https://doi.org/10.1111/j.1346-8138.2004.tb00633.x
12. Pianezza ML, Singh D, Van der Kwast T, Jarvi K. Rare case of recurrent angiokeratoma of Fordyce on penile shaft. Urology. 2006;68(4):891.e1-891.e8913. https://doi.org/10.1016/j.urology.2006.05.018
13. Piqué-Duran E, Pérez-Cejudo JA, Cameselle-Martínez D, García-Vázquez O. Unilateral angiokeratoma of Fordyce. Actas Dermosifiliogr. 2013;104(2):163-164. https://doi.org/10.1016/j.ad.2012.02.013
14. Erkek E, Basar MM, Bagci Y, Karaduman A, Bilen CY, Gokoz A. Fordyce angiokeratomas as clues to local venous hypertension. Arch Dermatol. 2005;141(10):1325-1326. https://doi.org/10.1001/archderm.141.10.1325
15. Zaballos P, Daufí C, Puig S, et al. Dermoscopy of solitary angiokeratomas: a morphological study. Arch Dermatol. 2007;143(3):318-325. https://doi.org/10.1001/archderm.143.3.318
16. Leung AKC, Barankin B. An adolescent with asymptomatic nodules of the scrotum. Consultant Pediatr. 2014;13(8):374. https://www.consultant360.com/articles/adolescent-asymptomatic-nodules-scrotum
17. Akinboro AO, Onilede DA, Babatunde TO, Oiwoh SO, Suleiman OA, Olabode OP. Idiopathic scrotal calcinosis: report of 2 cases, and review of pathogenesis and factors that determine patients' acceptance of surgical treatment. Clin Cosmet Investig Dermatol. 2018;11:333-337. https://doi.org/10.2147/ccid.s142101
18. Pompeo A, Molina WR, Pohlman GD, Sehrt D, Kim FJ. Idiopathic scrotal calcinosis: a rare entity and a review of the literature. Can Urol Assoc J. 2013;7(5-6):E439-E441. https://doi.org/10.5489/cuaj.1387
19. Sahoo N, Sethy M, Mishra P, Patra S, Purkait S, Giri SK. Idiopathic scrotal calcinosis diagnosed by fine needle aspiration cytology-report of a rare case. Diagn Cytopathol. 2017;45(10):922-924. https://doi.org/10.1002/dc.23757
20. Hedhli H, Hermi A, Raboudi M, et al. Idiopathic scrotal calcinosis: a new case report. Urol Case Rep. 2020;32:101225. https://doi.org/10.1016/j.eucr.2020.101225
21. Noël B, Bron C, Künzle N, De Heller M, Panizzon RG. Multiple nodules of the scrotum: histopathological findings and surgical procedure. A study of five cases. J Eur Acad Dermatol Venereol. 2006;20(6):707-710. https://doi.org/10.1111/j.1468-3083.2006.01578.x
22. Tela UM, Ibrahim MB. Scrotal calcinosis: a case report and review of pathogenesis and surgical management. Case Rep Urol. Published online July 22, 2012. https://doi.org/10.1155/2012/475246
23. Kyei MY, Djagbletey R, Abrahams AD, Mensah JE. Idiopathic scrotal calcinosis: a case report and review of postoperative outcomes. Case Rep Urol. Published online September 14, 2020. https://doi.org/10.1155/2020/8877695
24. Tareen A, Ibrahim RM. Idiopathic scrotal calcinosis - a case report. Int J Surg Case Rep. 2018;44:51-53. https://doi.org/10.1016/j.ijscr.2018.02.010
25. Wollina U, Schönlebe J, França K, Tchernev G, Lotti T. Idiopathic scrotal calcinosis - a case report. Open Access Maced J Med Sci. 2018;6(1):108-109. https://doi.org/10.3889/oamjms.2018.032
26. Al-Gonaim A, El-Tholoth HS, AlJafaar M, Sunbuli MG, Jad A. Scrotal calcinosis effect - case report and review of literature. Urol Case Rep. 2020;33:101347. https://doi.org/10.1016/j.eucr.2020.101347
27. Jayarajah U, de Silva L, de Silva C, Seneviratne S. Idiopathic scrotal calcinosis: a case report of a rare entity. Case Rep Urol. Published online December 16, 2019. https://doi.org/10.1155/2019/6501964


