Peer Reviewed
Temporal Triangular Alopecia
Introduction. An 8-year-old boy presents with symmetric bald patches in the temporal area which have been present his entire life.
History. The patient’s past medical history is significant for a prolonged neonatal intensive care unit (NICU) stay due to atrial and ventricular septal defects, which were repaired at 1 month, and a large congenital sacrococcygeal teratoma and tethered cord, which were repaired shortly after birth. Subsequently, he has developed a neurogenic bladder requiring regular catheterization. In addition, he had a duplication of the right thumb which was surgically resected at 11 months of age.
The boy’s parents have always noticed a lack of hair bilaterally in the temporal region since birth, which was thought to be due to having multiple scalp IVs placed during his NICU course. At his 8-year-old well visit, his father was concerned that the bald patches were becoming more prominent and noted that the boy’s hair has yet to grow back (Figure 1).
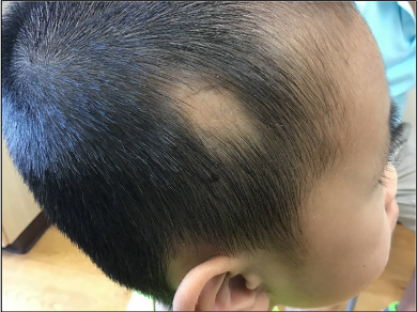
Figure 1. An 8-year-old boy presents with symmetric bald patches since birth in the temporal area.
Physical examination. The patient is a well-appearing boy in no acute distress. His vital signs and growth parameters are within normal ranges. His skin examination shows symmetric geometric alopecia at the temporal scalp bilaterally. No other skin abnormalities were noted on the examined areas. During the examination, a midline sternotomy scar and a 1/6 systolic ejection murmur was noted. He has a scar on his lower back and on his right thumb.
Diagnostic testing. Due to the specific shape, location, and symmetry of the patches of hair loss, the diagnosis of temporal triangular alopecia (TTA) was made clinically. Given that these lesions had been present since he started growing hair, no further testing was needed.
Differential diagnosis. The differential diagnosis of focal hair loss includes alopecia areata, tinea capitis, trichotillomania, traction alopecia, friction alopecia, and androgenetic alopecia1. These potential diagnoses were unlikely given that the patches of alopecia had been present his entire life and were bilateral and symmetric in appearance. The area of alopecia also lacked any hair regrowth and did not have any scaling, making tinea capitis less likely.
Treatment and management. There is no treatment indicated for TTA, and reassurance was provided to the family. The parents were accepting of the diagnosis. They do not expect that the hair will grow back. He has continued to wear his hair very short which reveals the patches. In the future he may choose a different hairstyle that may conceal the areas of alopecia.
Discussion. Temporal triangular alopecia (TTA), also known as congenital triangular alopecia (CTA), is a benign pattern of hair loss that typically affects the frontotemporal region1. The first mention of TTA was described by Raymond Sabouraud in 19052. Although not a common diagnosis in medical literature, there is the possibility that this diagnosis has been underreported due to misdiagnosis as alopecia areata or not diagnosed at all since for many it has been present for most of their lives. In a review of 6200 patients, the frequency of TTA was determined to be 0.11%3.
The patches of alopecia noted in patients with TTA are most often unilateral but may present bilateral in a small subset of patients. Although originally considered a congenital condition, a 2010 review of 53 cases found that 55.8% were diagnosed between the ages of 2 and 9 years, whereas 36.5% of cases were diagnosed at birth1,4. Previous reports do not mention any gender preference, and although most patients with TTA are White, there have been diagnoses involving Black and Asian patients as well1.
TTA is a non-scarring form of alopecia, and the lesions are not accompanied by any inflammation, atrophy, or discoloration1. Although the name suggests that the lesions are in a triangular shape, there have been reports of oval, dome, and lancet-shaped patches1. In most instances, there are a few terminal hairs present at the periphery of the lesion, most of them being vellus1,4. On histology, there is a normal amount of hair follicles however the normal hair follicles are replaced by sparse vellus particles. Histological analysis of the epidermis, dermis, collagen bundles, sweat, and sebaceous glands show no abnormalities1. There has been evidence on histology of miniaturized hair follicles with an increased proportion of indeterminate hairs, which may be attributed to abnormalities in follicle morphogenesis1. These findings support the hypothesis that TTA may be a type of hamartomatous mosaic disease with links to an abnormal epithelial-mesenchymal interaction1,4.
Although there are characteristic histological findings associated with TTA, a diagnosis can be made on clinical evidence alone due to the distinct appearance and location. To rule out other similar diagnoses such as alopecia areata, it is important that there is no significant hair regrowth after 6 months since the presence of vellus hairs have been confirmed5.
TTA is an asymptomatic condition and has not shown to change or progress over the course of one’s life. Besides cosmetic reasons, there are not any indications in which to treat TTA. Hair restoration therapy has been found to have long-term sustained benefits and can be helpful for patients who desire certain cosmetic results1.
Conclusion. Temporal triangular alopecia is a non-scarring, asymptomatic form of alopecia that may be misdiagnosed due to its clinical similarities to other forms of alopecia. While the exact etiology is unknown, there is thought that this condition may be a type of mosaic disease. In this specific case, no treatment was warranted, and the parents were reassured that it was a benign condition.
AUTHORS:
Shae Margulies, MD1 • Stephanie Ryan, MD2
AFFILIATIONS:
1Resident Physician, Internal Medicine, University of Florida College of Medicine, Gainesville, FL
2Associate Professor, Department of Pediatrics, University of Florida College of Medicine, Gainesville, FL
CITATION:
Margulies S, Ryan S. Temporal triangular alopecia. Consultant. Published online April 11, 2025. DOI: 10.25270/con.2025.06.000004
Received: April 29, 2024. Accepted: September 27, 2024.
DISCLOSURES:
The authors report no relevant financial relationships.
ACKNOWLEDGEMENTS:
None.
CORRESPONDENCE:
Stephanie Ryan, MD, Associate Professor, Department of Pediatrics, University of Florida College of Medicine, 7046 SW Archer RD, Gainesville, FL 32608 (sfryan@ufl.edu)
References
- Yin Li VC, Yesudian PD. Congenital Triangular Alopecia. Int J Trichology. 2015 Apr-Jun;7(2):48-53. doi: 10.4103/0974-7753.160089.
- Trakimas C, Sperling LC, Skelton HG 3rd, Smith KJ, Buker JL. Clinical and histologic findings in temporal triangular alopecia. J Am Acad Dermatol. 1994;31(2 Pt 1):205-209. doi:10.1016/s0190-9622(94)70147-4
- García-Hernández MJ, Rodríguez-Pichardo A, Camacho F. Congenital triangular alopecia (Brauer nevus). Pediatr Dermatol. 1995;12(4):301-303. doi:10.1111/j.1525-1470.1995.tb00187.x
- Yamazaki M, Irisawa R, Tsuboi R. Temporal triangular alopecia and a review of 52 past cases. J Dermatol. 2010;37(4):360-362. doi:10.1111/j.1346-8138.2010.00817.x
- Inui S, Nakajima T, Itami S. Temporal triangular alopecia: trichoscopic diagnosis. J Dermatol. 2012;39(6):572-574. doi:10.1111/j.1346-8138.2011.01348.x


