Demystifying Psoriatic Arthritis for the Primary Care Provider
Up to 30% of patients with psoriasis develop psoriatic arthritis (PsA), and approximately 75% of patients with PsA also have psoriasis before a diagnosis of PsA is made. This was the topic of discussion this afternoon at Practical Updates in Primary Care 2021.
In his session, Joseph Merola, MD, discussed screening methods for PsA among patients with psoriasis, which patients are most at risk, and the different domains of disease. Dr Merola is a dermatologist and rheumatologist at Brigham and Women’s Hospital in Boston, Massachusetts.
Screening for PsA Among Patients With Psoriasis
Many of the manifestations seen on the skin also are present in the joints. PsA is characterized by joint pain and stiffness, limited mobility, and reduced range of motion. PsA can deform joints in 40% to 60% of patients, Dr Merola said.
There is no definitive diagnostic test; diagnosis remains clinical. The differential diagnosis includes osteoarthritis, rheumatoid arthritis, crystal arthropathy, fibromyalgia, and Lyme arthritis.
Dr Merola then talked about inflammatory arthritis vs degenerative arthritis. Patients presenting with inflammatory arthritis will usually have stiffness after 30 to 60 minutes of inactivity, but their symptoms improve with activity. For degenerative arthritis, patients will have worse symptoms after activity and at the end of the day.
Patients with inflammatory arthritis also present with redness, warmth, and swelling of the joint(s); with systemic symptoms like fatigue or uveitis; and a family history, whereas patients with degenerative arthritis will present with specific joint patterns.
Physical examination, laboratory tests screening for erythrocyte sedimentation rate and C-reactive protein, and radiology tests such as magnetic resonance imaging or ultrasound can help make a diagnosis. However, absence of inflammatory markers does not rule out a PsA diagnosis.
During the physical examination, if 2 or more of the following “PSA” signs are present, a diagnosis of PsA is probable:
- Pain in the joints
- Stiffness after waking in the morning or after a period of 30 minutes or more of inactivity
- Axial/spine pain associated with stiffness but improves with activity
Other screening tools include the Psoriasis Epidemiology Screening Tool and Psoriatic Arthritis Impact of Disease test, Dr Merola said.
At-Risk Psoriasis Phenotypes for Advancement to PsA
Scalp psoriasis is one of the most common manifestations of PsA, along with inverse disease and nail psoriasis. Risk factors for developing PsA include a family history of a first-degree relative with PsA, severe psoriasis, obesity, subclinical musculoskeletal inflammation, and increased levels of inflammatory cells.
Moreover, there is a wide range of comorbidities associated with PsA, including cardiometabolic disease, chronic obstructive pulmonary disease, and depression.

Domains of Disease
The diverse clinical features of PsA include peripheral arthritis, axial disease, enthesitis, dactylitis, skin manifestations, and nail manifestations. The domain of disease impacts treatment efficacy; responses are variable among patients, Dr Merola said.
For patients with enthesitis, swelling is not always present, Dr Merola said. Commonly involved joints include the shoulder, elbow, hips, knees, and heel. Dactylitis involves tissue surrounding the joint as well. It is sometimes referred to as “sausage fingers.”
Dr Merola said that about 25% of patients with PsA will have axial disease. To help diagnose axial disease, think of “IPAIN”:
- Insidious onset
- Pain worse at night and/or in the morning
- Age of onset, younger than 40 years
- Improves with activity
- Not relieved with rest
PsA treatment options offer limited ability to predict response to a given mechanism, although psoriasis treatments are known to be highly effective, Dr Merola said.
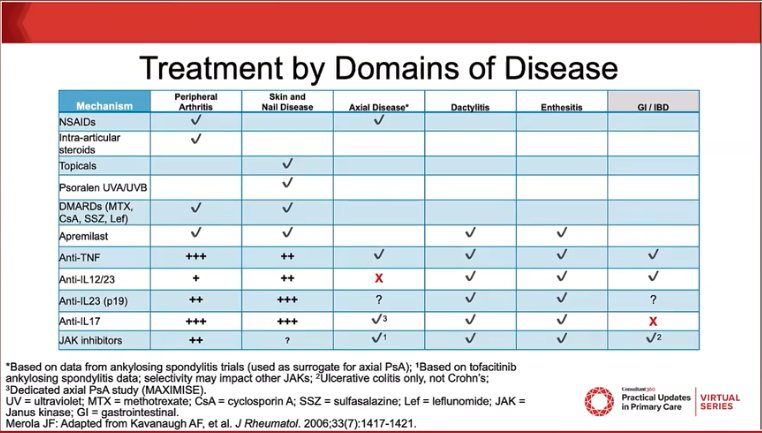
“A team collaborative approach is needed to manage patients with psoriatic disease given the wide range of comorbidities,” Dr Merola concluded. “Treatment considerations highly depend on which domain of disease is present.”
—Amanda Balbi
Reference
Merola J. Early detection of psoriatic arthritis. Talk presented at: Practical Updates in Primary Care 2021 Virtual Series; May 13-15, 2021; Virtual


