PCOS Linked to Lower Risk of Acute Kidney Injury in Hospitalized Women With Diabetes
Key Highlights:
- Women with both polycystic ovary syndrome (PCOS) and diabetes were younger and had lower unadjusted hospital mortality rates and healthcare costs than those without PCOS.
- After adjusting for demographics and comorbidities, differences in mortality, length of stay, and cost were not statistically significant.
- PCOS was independently associated with significantly reduced risk of acute kidney injury.
- No significant differences were observed in rates of diabetic ketoacidosis, hyperosmolar hyperglycemic state, myocardial infarction, cerebral infarction, sepsis, or respiratory failure.
Women with diabetes and concurrent polycystic ovary syndrome (PCOS) experienced similar in-hospital mortality and healthcare utilization compared to compared to women with diabetes but without PCOS after statistical adjustment, but were found to have a significantly lower risk of developing acute kidney injury.
PCOS often coexists with diabetes mellitus (DM), yet its influence on hospital outcomes for women with diabetes has remained unclear. Given the increasing prevalence of both conditions, this study was conducted to evaluate how PCOS might affect hospital mortality, complications, and resource utilization in diabetic female patients.
Researchers performed a retrospective analysis using the National Inpatient Sample database from 2016 to 2020. The cohort consisted of adult women hospitalized with a primary diagnosis of diabetes. Patients were categorized based on the presence or absence of a secondary diagnosis of PCOS. Key measured outcomes included in-hospital mortality, length of stay (LOS), total cost of care (TOC), and a range of hospital complications. Multivariable logistic regression models were employed to adjust for potential confounders and determine adjusted odds ratios (aOR) and adjusted mean differences (aMD).
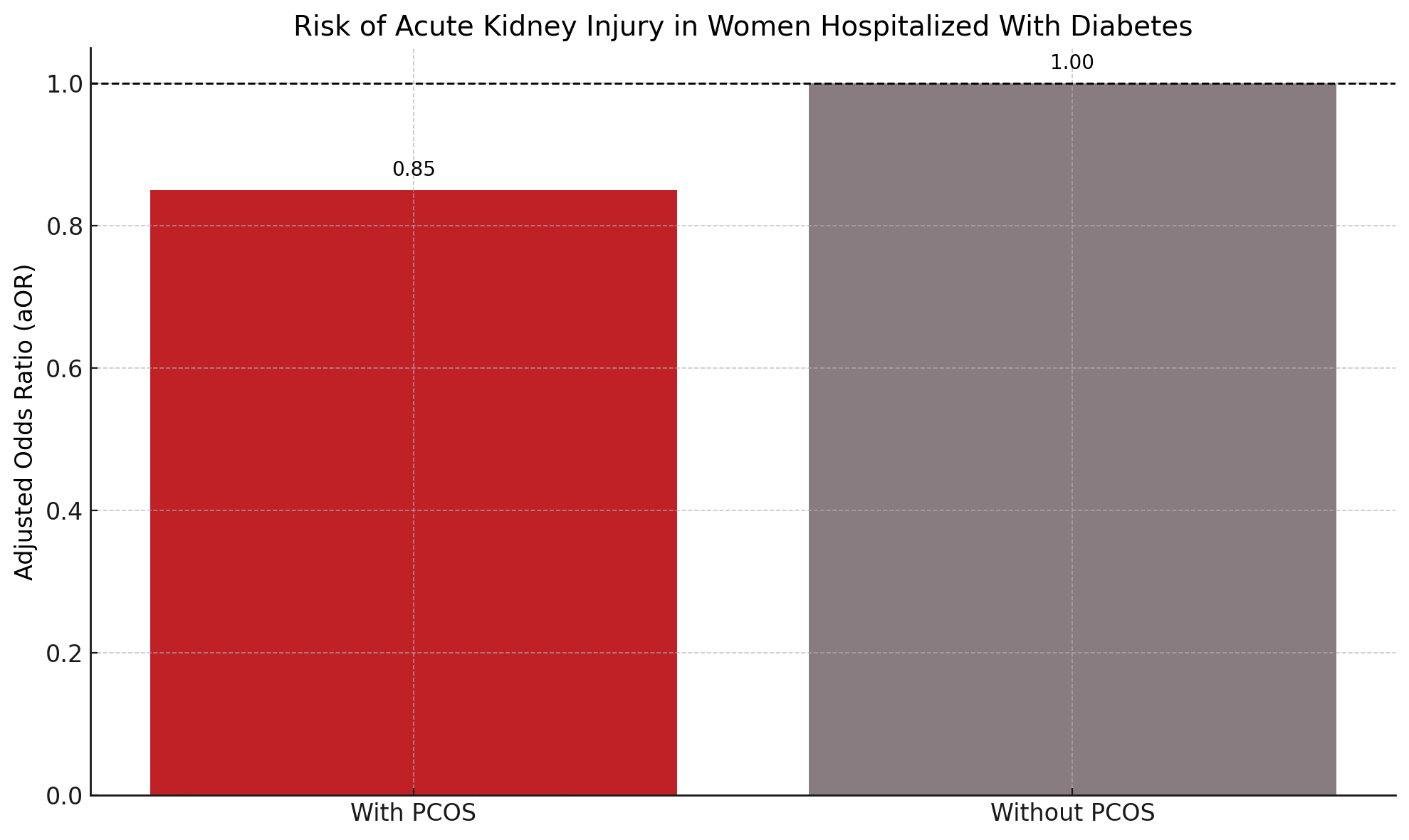
Among 1,347,925 women with diabetes, only 0.4% (n = 5670) had PCOS. These women were significantly younger (mean age 34.7 vs. 53.9 years, P < .001). Unadjusted analyses suggested better outcomes in the PCOS group, with lower mortality (0.26% vs. 0.64%), shorter LOS (3.84 vs. 4.72 days), and reduced TOC ($36,485 vs. $48,749). However, these differences did not remain statistically significant after adjustment: mortality (aOR 0.65; P = .692), LOS (aMD 0.017 days; P = .881), and TOC (aMD -$2,283; P = .127). A notable exception was acute kidney injury, where PCOS patients had a significantly lower risk (aOR 0.85; 95% CI 0.73–0.99; P = .046). Other complications, including diabetic ketoacidosis, hyperosmolar hyperglycemic state, myocardial infarction, cerebral infarction, sepsis, and respiratory failure, did not differ significantly between groups.
“The younger age of women with PCOS may partly explain these findings,” the study authors wrote. “Further research is needed to explore the underlying mechanisms and to identify targeted strategies for optimizing hospital outcomes in this population.”
Reference:
Alrosan S, Al-Ahmad M, Barthel B. Hospital outcomes in women with diabetes mellitus and polycystic ovary syndrome: insights from National Inpatient Sample (2016-2020). Poster presented at: ENDO 2025; July 12-15, 2025; San Francisco, CA. https://www.endocrine.org/meetings-and-events/endo-2025


