 |
|
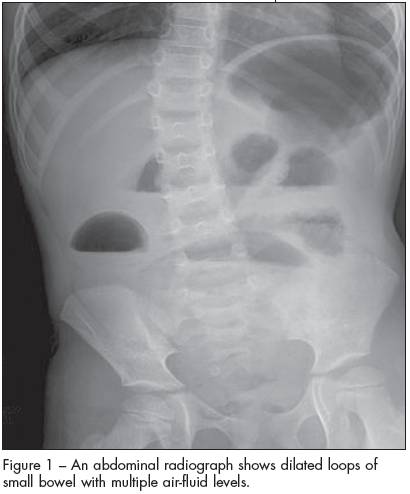
Figure 1 – An abdominal radiograph shows dilated loops of small bowel with multiple air-fluid levels. |
Case In Point
An Intriguing Diagnosis
A 4-year-old Hispanic girl presented with abdominal pain of 2 months' duration that had been increasing in intensity for the past 2 days. The pain was localized to the epigastric area and was associated with episodic nonbilious vomiting and a 4-lb weight loss within the past month. The child had normal bowel movements and no recent travel or change in diet.
A month earlier, the child was hospitalized for similar symptoms. Abdominal radiographic and CT findings were nonspecific. Postviral dysmotility was diagnosed. The patient was treated with ranitidine and sent home to follow up with a gastroenterologist. Further investigation during that admission revealed that a family member had reportedly seen the child pull out strands of her hair and put them in her mouth.
The child appeared anorexic and was mildly dehydrated, afebrile, and tachycardic. A prominent area of alopecia was noted on the right parietal region, and several smaller areas of alopecia with broken hairs in various stages of growth were present throughout the scalp. The abdomen was benign except for diffuse epigastric tenderness.
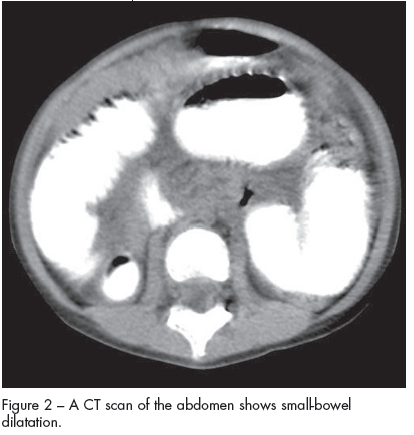
Results of a complete blood cell count and a comprehensive metabolic panel, including amylase and lipase, were normal. An abdominal radiograph showed dilated loops of small bowel with multiple air-fluid levels (Figure 1). Upper GI series with small-bowel follow-through showed dilated small-bowel loops--suggestive of distal small-bowel obstruction. CT scans of the abdomen revealed a distended stomach and significant small-bowel dilatation (Figure 2) with no mass.
 |
|
Figure 2 - A CT scan of the abdomen shows small-bowel dilatation. |
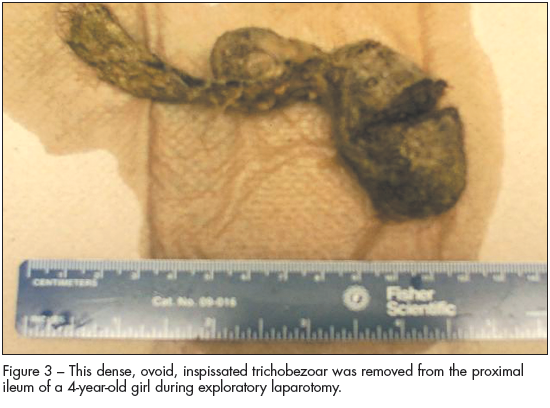
This child was treated conservatively with bowel rest and a nasogastric tube for partial small-bowel obstruction; however, her symptoms persisted. After 5 days without clinical improvement and the patient's possible history of pulling her hair, she was taken to the operating room for an exploratory laparotomy. A 7.5 × 2.8 × 2-cm bezoar was removed from the proximal ileum. Pathological examination revealed a dense, ovoid, inspissated trichobezoar (Figure 3).
The patient did well postoperatively and was discharged after 9 days. She was referred to a psychiatrist to explore for emotional stress or personality disorder.
TRICHOBEZOAR: AN OVERVIEW
Of the more than 400 reported cases of trichobezoar, most have occurred in young women, aged 15 to 20 years, who swallow their hair. Cases have been reported in children as young as 1 year and in adults up to 56 years.1
 |
|
Figure 3 – This dense, ovoid, inspissated trichobezaoar was removed from the proximal ileum of a 4-year-old girl during exploratory laparotomy. |
In about 10% of all patients, trichophagia is associated with a psychological disorder or mental retardation.1 Trichophagia also may be related to emotional stress.
A trichobezoar results when swallowed hairs retained by mucus become enmeshed into a mass. The "hair ball" is often in the shape of the stomach, where trichobezoars are usually found. A trichobezoar is thought to form initially in the gastric folds, because the slippery surfaces of the hair strands prevent propulsion by peristalsis.2 As more hair is swallowed, peristalsis causes the ingested hairs to mesh into a ball. Mucus gives the bezoar its shiny surface.
The putrid smell of a trichobezoar results from decomposition and fermentation of fats in the hair. Acidic contents of the stomach denature the hair proteins and cause the hairs to turn black--irrespective of the original hair color.1 Rarely, a trichobezoar may extend to the small intestine as a tail--known as Rapunzel syndrome.3 The finding of a trichobezoar in the ileum without a parent bezoar in the stomach, as in this case, is also rare.
DIAGNOSIS
Small trichobezoars are usually asymptomatic. Large trichobezoars are often palpable and may cause malaise, weight loss, vague abdominal pain associated with meals, anorexia, halitosis, vomiting, wasting, and cachexia. Complications include gastritis (which can cause occult blood loss and secondary anemia), ulceration, intestinal obstruction, necrosis, peritonitis, and perforation.
Plain abdominal films are typically nonspecific, as in this case. A large gastric bezoar, however, may appear as an opacified round density that protrudes into the stomach gas bubble. Barium studies may show an intestinal or gastric mass with barium in the honeycomb interstices. CT scans may demonstrate a well- defined intraluminal mass with interspersed gas; dilated intestinal loops may be present.4 Rarely, a CT scan of the abdomen does not show a mass, as in this case, and exploratory laparotomy or laparoscopy must be performed. Why both studies were negative in this patient is unknown; possibly, the ovoid shape of the bezoar was a factor.
MANAGEMENT
When diagnosed early, gastric bezoars can be managed conservatively with fragmentation, endoscopic extraction, or enzymatic destruction. However, most intestinal trichobezoars require surgical removal via laparotomy or laparoscopy.
A thorough exploration of the small intestine and stomach for retained bezoars is recommended for patients with intestinal trichobezoars.5 In one study, 23 of 87 patients with intestinal bezoars had concomitant gastric bezoars.6 The mortality rate in patients with untreated intestinal bezoars is 47%.7
Because trichobezoars are associated with psychological disorders, referral to a psychiatrist for behavior modification or antipsychotic therapy may be warranted to prevent recurrence.8 This is also true in young children because many of them may have some underlying emotional stress. *


