Sacroiliitis
A 23-month-old girl was admitted to the hospital with a history of refusing to bear weight on her right leg. She presented with a 1-day history of pain in the right hip, limping, fever, decreased appetite, and fussiness. Significant findings on examination included a temperature of 38.1°C (100.6°F), tachycardia (heart rate, 130 beats per minute), and pain on palpation of the posterior right hip and buttocks. There was no pain on hyperextension or external rotation of the right hip, and no erythema or warmth over the joint.
Plain radiographs of the pelvis and ultrasonography of the hips were normal. Laboratory findings on admission showed a leukocyte count of 12,200/µL, with 60% segmented neutrophils and no banded neutrophils; erythrocyte sedimentation rate of 61 mm/hour, and a normal C-reactive protein (CRP) level. The patient had no significant past medical history other than mild asthma. There was no history of immunosuppression or trauma. The patient was admitted for observation and intravenous hydration with a diagnosis of toxic synovitis versus possible osteomyelitis.
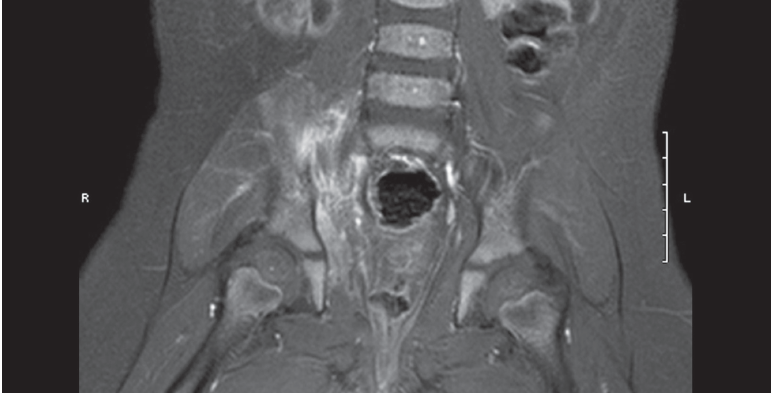
By day 2 of hospitalization, the patient’s temperature spiked to 38.5°C (101.3°F), and she continued to refuse to bear weight on the right leg. Her CRP had elevated to 79 mg/L, and blood cultures were obtained. After 3 days in the hospital, the patient was refusing to sit up and had developed tenderness with passive range of motion on her right side. A nuclear bone scan demonstrated increased 3-phase activity in the right sacroiliac joint compatible with sacroiliitis. The child was started on clindamycin (40 mg/kg/day), with daily blood cultures. Magnetic resonance imaging (MRI) of the pelvis was also obtained and demonstrated right sacroiliitis with extensive myositis involving the right iliacus, obturator internus, and the gluteal musculature at the sacroiliac joint. There was no evidence of a drainable abscess or fluid collection.
Sacroiliitis is rare in children, representing only 1% to 2% of osteoarticular infections.1 Typical features include limping gait, fever, and buttocks pain. Most cases of sacroiliitis are unilateral. Because the typical signs and symptoms of sacroiliitis can be difficult to differentiate from other conditions such as trauma, septic arthritis, and osteomyelitis, considerable delay can occur between presentation and diagnosis. Such delays can lead to complications such as sepsis, abscess, or sequestration formation, and long-term joint deformity.2 Plain radiographs and ultrasonograms often are negative. Isotope bone scanning is helpful for early diagnosis, and MRI has the highest sensitivity and specificity.2 Management includes early diagnosis, antibiotic therapy with coverage against Staphylococcus aureus, and bed rest.2
By day 4 of parenteral antibiotic therapy, the patient was afebrile, crawling in bed, and bearing some weight on her right lower extremity. Her CRP was decreasing, and all of her blood culture results were negative. The child was discharged home on clindamycin via a peripherally inserted central catheter due to failure to tolerate oral therapy. The parents were instructed to follow up with infectious disease for a weekly leukocyte count and CRP level test, and to continue clindamycin for 4 weeks.
REFERENCES:
1. Molinos Quintana A, Morillo Gutiérrez B, Camacho Lovillo MS, Neth O, Obando Santaella I. Pyogenic sacroiliitis in children—a diagnostic challenge. Clin Rheumatol. 2011;30(1):107-113.
2. Ghedira Besbes L, Haddad S, Abid A, Ben Meriem C, Gueddiche MN. Pyogenic sacroiliitis in children: two case reports. Case Rep Med. 2012;2012:415323.


