Infant With Fever and Vesicular Rash
What's Your Diagnosis?
Sharpen Your Physical Diagnostic Skills

HISTORY
A 3-month-old girl was brought to the emergency department with fever (temperature, maximum of 40ºC [104ºF]) of 2 days’ duration and a vesicular rash on the neck that had appeared 2 days before the onset of the fever. The parents reported that the infant was sleeping 1 to 2 hours at a time, down from her normal 3 to 4 hours, and nursing 5 to 10 minutes every 2 hours, about a 25% decrease. No change in number of wet diapers reported. The infant had no sick contacts or previous similar rashes; however, she had been treated for atopic dermatitis on her cheeks and arms with 1% hydrocortisone cream, as needed.
PHYSICAL EXAMINATION
Fussy but consolable infant. Blood pressure, 80/52 mm Hg; heart rate, 135 beats per minute; respiration rate, 36 breaths per minute; and rectal temperature, 38.3ºC (100.9ºF). Height, 24 in (70th percentile); weight, 13.7 lb (70th percentile); and head circumference, 16 in (75th percentile). Vesiculopustular rash with erythematous base mainly on the neck, a few satellite lesions on the cheeks and preauricular area. Areas of mild eczema on the elbows, lower extremities, and cheeks.Normocephalic infant with open, soft anterior fontanel, positive red reflex. Tympanic membranes intact. Nares patent. Mucous membranes moist. No lymphadenopathy. Heart, lung, and abdomen findings unremarkable.
WHAT'S YOUR DIAGNOSIS?
What's Your Diagnosis?
ANSWER: ECZEMA HERPETICUM
This patient’s presentation is pathognomonic of eczema herpeticum (EH), also known as Kaposi varicelliform eruption—herpes simplex virus (HSV) infection of eczematous skin. This rare, potentially life-threatening condition is characterized by high fevers, malaise, and numerous skin vesicles.1 Infants and children with preexisting epidermal dysfunction, most commonly those with atopic dermatitis, are susceptible to EH.
INCIDENCE AND PATHOPHYSIOLOGY
EH remains more common in children than in adults, although it can occur at any age. The true incidence of EH is unknown.
Although EH is often caused by HSV type 1 or 2, it rarely may be caused by Coxsackievirus A16 and vaccinia virus. In addition to atopic dermatitis, EH is associated with many other skin diseases, including contact and seborrheic dermatitis, pemphigus, and Darier disease. EH may also occur on skin affected by burns and other injuries, skin grafts, sunburns, or other conditions that compromise the skin barrier and render it vulnerable to infection.
Systemic immune defects and an impaired cutaneous immune response are proposed mechanisms for EH in patients with atopic dermatitis. Increased production of interleukin-4 may result in a lower level of interferon-g (a peripheral blood lymphocyte with antiviral activities that allows for virus overgrowth).2-4 Decreased expression of cathelicidin peptides (multifunctional peptides with antimicrobial and antiviral activities) may result in a defective cutaneous immune response.5-7
CLINICAL MANIFESTATIONS
The rash of EH usually begins as clusters of umbilicated vesiculopustules on areas of the skin affected by an underlying skin disease, most commonly the head and neck. Fever, chills, and malaise may accompany the rash. As the disease progresses, the lesions become painful, crusted, or hemorrhagic erosions with a punched-out appearance. The lesions may coalesce into larger eroded areas subject to secondary bacterial infection.8 Rarely, EH may spread beyond the area of dermatosis and cause complications, such as herpes keratitis, encephalitis, meningitis, and disseminated infection with visceral involvement.1,9
DIAGNOSIS
The diagnosis of EH is primarily clinical. Treatment can begin without laboratory confirmation when there is a history of atopic dermatitis and specific clinical manifestations, including punched-out lesions—as in this patient. In cases in which the diagnosis is not clear, the most sensitive and quick tests are direct fluorescent antibody staining and amplification of viral DNA using polymerase chain reaction. Serology assays to detect HSV antibodies are used only when other techniques are impractical or ineffective.
MANAGEMENT
In young infants, EH is a dermatological emergency. Early treatment with antiviral medications is necessary to prevent life-threatening complications. Intravenous acyclovir, 1500 mg/m2/d, and oral acyclovir, 25 to 30 mg/kg/d given in 3 divided doses, have been shown to be effective in infants and children. Standard doses of other oral antiviral drugs, such as oral valacyclovir, are equally effective.10 Parenteral foscarnet can be used in immunocompromised children who may be resistant to acyclovir.3
Treatment of EH also consists of adequate hydration and fever reduction. A topical antibiotic cream, such as silver sulfadiazine, may be given to prevent secondary bacterial infection.5,11 Oral antistaphylococcal antibiotics also play an important role in the prevention of secondary bacterial infection. EH usually resolves within 2 to 3 weeks. Immunocompromised children or those with recurrent infection should receive prophylactic antiviral therapy.
PATIENT OUTCOME
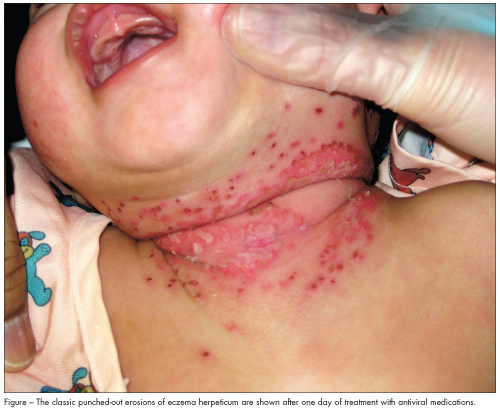
This infant was treated with acyclovir, intravenously for 4 days and orally thereafter for a total of 14 days. She was also treated with intravenous oxacillin, which was switched to oral cephalexin. Within the first 24 hours of treatment, the patient defervesced, and the lesions began to crust (Figure). At 2-week follow-up, the rash had almost completely resolved with minimal scarring. ■
References
1. Leung DY. Atopic dermatitis. In: Kliegman RM, Behrman RE, Jenson HB, Stanton BF, eds. Nelson Textbook of Pediatrics. Philadelphia: Saunders Elsevier; 2007:974-975.
2. Murray HW. Interferon-gamma and host antimicrobial defense: current and future clinical applications. Am J Med. 1994;97:459-467.
3. Chilukuri S, Rosen T. Management of acyclovir-resistant herpes simplex virus. Dermatol Clin.2003;21:311-320.
4. Hassan-Zahraee M, Wu J, Gordon J. Rapid synthesis of IFN-gamma by T cells in skin may play a pivotal role in the human skin immune system. Int Immunol. 1998;10:1599-1612.
5. Mackley CL, Adams DR, Anderson B, Miller JJ. Eczema herpeticum: a dermatologic emergency.Dermatol Nurs. 2002;14:307-310, 323.
6. Beck LA, Boguniewicz M, Hata T, et al. Phenotype of atopic dermatitis subjects with a history of eczema herpeticum. J Allergy Clin Immunol. 2009;124:260-269.
7. Howell MD, Wollenberg A, Gallo RL, et al. Cathelicidin deficiency predisposes to eczema herpeticum. J Allergy Clin Immunol. 2006;117:836-841.
8. Davis HW, Michaels MG. Infectious disease. In: Zitelli BJ, Davis HW, eds. Atlas of Pediatric Physical Diagnosis. Philadelphia: Mosby Elsevier; 2007:452-453.
9. Wollenberg A, Wetzel S, Burgdorf WH, Haas J. Viral infections in atopic dermatitis: pathogenic aspects and clinical management. J Allergy Clin Immunol. 2003;112:667-674.
10. Habif TP. Clinical Dermatology: A Color Guide to Diagnosis and Therapy. 5th ed. St Louis: Mosby; 2010:473.
11. Marshall DS, Linfert DR, Draghi A, et al. Identification of herpes simplex virus genital infection: comparison of a multiplex PCR assay and traditional viral isolation techniques. Mod Pathol.2001;14:152-156.


