Peer Reviewed
What Are These Bullous Lesions on the Extremities of a Young Woman With Crohn Disease?
AUTHORS:
Hunter T. Holloway, DO • Stephen C. Brawley, MD, PhD • Pamela C. Scott, MD
AFFILIATION:
Eastern Virginia Medical School Portsmouth Family Medicine, Portsmouth, Virginia
CITATION:
Holloway HT, Brawley SC, Scott PC. What are these bullous lesions on the extremities of a young woman with Crohn disease? Consultant. 2021;61(10):e14-e17. doi:10.25270/con.2021.04.00009
Received November 18, 2020. Accepted January 19, 2021. Published online April 19, 2021.
DISCLOSURES:
The authors report no relevant financial relationships.
CORRESPONDENCE:
Hunter T. Holloway, DO, Eastern Virginia Medical School Portsmouth Family Medicine, 3640 High Street #3b, Portsmouth, VA 23707 (hollowht@evms.edu)
A 35-year-old woman presented to our clinic with chronic bilateral lower extremity ulcerations that had worsened over the past 2 weeks. The lesions had started as small, tender nodules that subsequently formed superficial bullae that broke down to ulcerations, which released serosanguinous fluid. At the time of presentation, her lesions were at different stages of evolution. She reported pain with dressing changes and weakness ambulating with a rolling walker. She also denied fever.
History. Her medical history was significant for Crohn disease status post-proctocolectomy, type 2 diabetes, morbid obesity, and hidradenitis suppurativa. She was not taking any immunemodulating medications or biologic agents for Crohn disease.
Approximately 1 month prior to presentation, the patient was referred by her primary care provider to a vascular surgeon for the lower extremity ulcers. The surgeon then prescribed an Unna boot (zinc oxide compression bandages).
The only prior diagnostic studies the patient had were lower extremity arterial and venous ultrasonography scans, results of which were unremarkable. The results of a biopsy of a lower extremity ulcer showed underlying neutrophilic and granulomatous dermatosis and fibrosis.
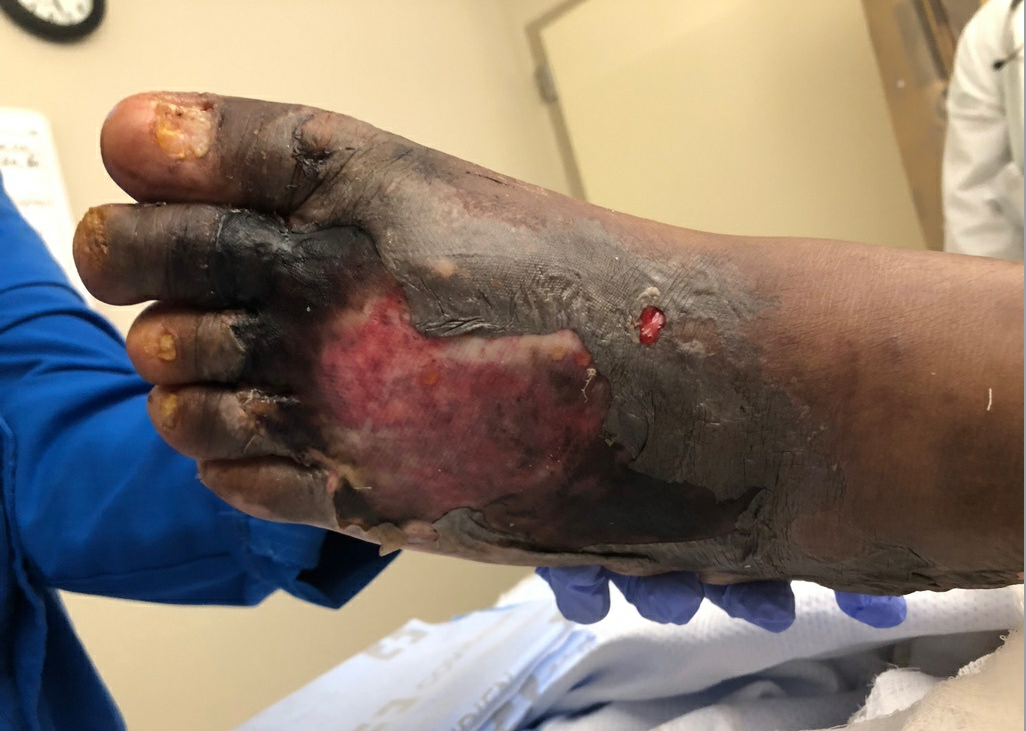
Physical examination. Numerous ulcerations of varying size were sharply demarcated on the patient’s bilateral lower extremities, and remnants of the Unna boot therapy were noted (Figures 1 and 2). In addition, crops of erythematous nodules were noted on the patient’s bilateral lower and upper extremities (Figure 3).
Figure 1. Bullous and ulcerative lesions on the patient’s right leg. Note the varying stages of lesion evolution.
Figure 2. Ulcerative lesion on the dorsal surface of the patient’s left foot. Note the surrounding areas of violaceous induration.
Figure 3. Crops of erythema nodosum were noted on the patient’s left upper thigh. Similar lesions were found on patient’s upper extremities.
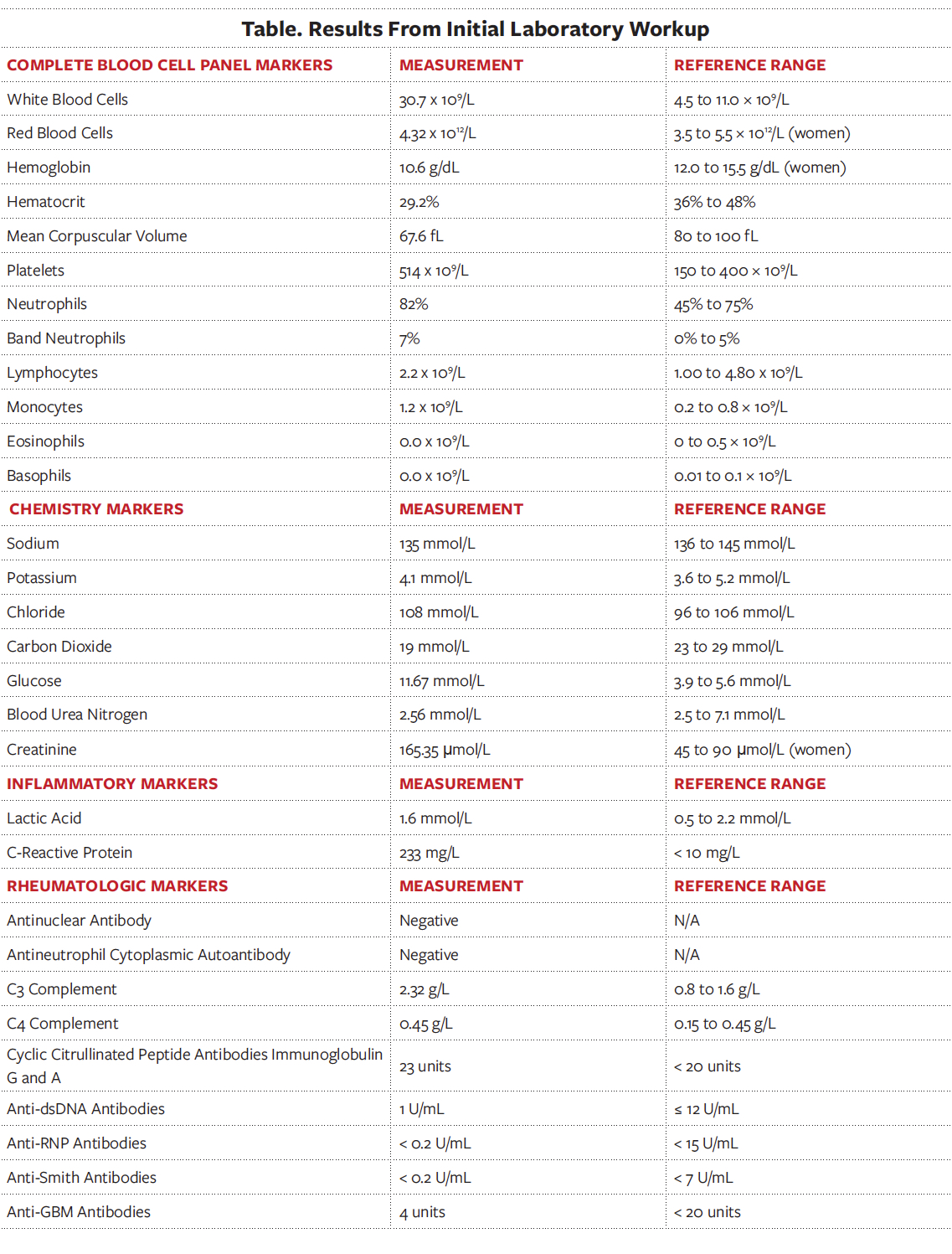
The results of initial hematology, chemistry, and rheumatologic tests are listed in the Table (click to enlarge).
Answer and discussion on next page.
Answer: B. Pyoderma gangrenosum
Diagnostic testing. Initial laboratory evaluation showed leukocytosis with left shift, elevated renal indices, and elevated inflammatory markers. Accordingly, the patient was admitted to the hospital for sepsis and was placed on broad-spectrum antibiotic therapy. Surgery and infectious disease specialists were consulted at admission. The patient underwent operating room debridement, and intraoperative biopsies were obtained. The extent of debridement required was extensive (Figure 4).
Figure 4. Appearance of the patient’s bilateral lower extremities after operating room debridement and prior to skin grafting.
Results of the intraoperative wound cultures revealed polymicrobial infection, including with Citrobacter koseri, Providencia stuartii, Klebsiella pneumoniae, Escherichia coli, Enterococcus faecalis group D, Proteus mirabilis, and Staphylococcus epidermidis. The pathology of the skin biopsies from the ulcer borders was significant for heavy neutrophilic inflammatory infiltrate throughout the interstitium. Laboratory results also showed elevated complement levels (Table). Given the pathology findings and wound culture results, pyoderma gangrenosum with secondary bacterial infection was diagnosed.
Discussion. Several elements from the patient’s history—including a diagnosis of Crohn disease and recent traumatic insult from treatment with an Unna boot—physical examination findings of erythema nodosum, and pathologic evidence of an inflammatory neutrophilic response suggest the diagnosis of pyoderma gangrenosum.
Pyoderma gangrenosum is a chronic, noninfectious, ulcerative, and neutrophilic dermatosis.2,5 Approximately half of patients with pyoderma gangrenosum have an underlying chronic inflammatory or malignant disease such as ulcerative colitis, rheumatoid arthritis, Crohn disease, or a hematologic malignancy.3,5 Among patients with ulcerative colitis, lesions typically appear during active disease but may appear after colectomy. Patients typically develop erythema nodosum 5 years into the disease course of ulcerative colitis, and pyoderma gangrenosum will manifest after approximately 10 years.5 Crohn disease was diagnosed in our patient approximately 7 years prior to presentation.
The lesions typically develop on the bilateral lower extremities in more than 50% of cases but can develop anywhere on the skin, including on mucosal surfaces.3-5 There are 4 described variants of pyoderma gangrenosum: ulcerative, pustular, bullous, and vegetative.1-4 A patient can exhibit multiple variants at the same time. The lesions start as tender, red macules/papules that evolve into pustules or vesicles.2,5 The irregular borders form a violaceous halo of indurated skin surrounding an area of necrotizing ulceration with a purulent base.1,3,4
Pyoderma gangrenosum is regarded as a diagnosis of exclusion.1,2,4,5 Establishing a diagnosis of pyoderma gangrenosum is complicated by varied presentation and ulceration severity, nonspecific histological findings, and a lack of established diagnostic criteria or associated serologic markers.1,3,5 A broad differential includes a variety of vasculitides (eg, Behçet disease, antiphospholipid syndrome, lupus-associated neutrophilic dermatoses), vascular ulcerations, neutrophilic disorders (eg, Sweet syndrome), cutaneous malignant processes, primary cutaneous infections (ranging from bacterial ecythyma to deep fungal infections such as blastomycosis or sporotrichosis), and drug-induced (eg, serum bromide or iodide) or exogenous tissue injury (eg, inspect bite).1,3 A thorough history, physical examination, and guided work-up are required to exclude possible differential diagnoses. Biopsy is required to make a definitive diagnosis. An elliptical biopsy that includes an inflamed border and ulcer edge is preferred over a punch biopsy technique.1,2,3
As the diagnosis had not been established in this case, primary management considerations were given to a working diagnosis of chronic arterial insufficiency ulcerations. In addition to an evaluation by a rheumatologist and initiating high-dose steroid therapy, the superimposed bacterial infection and underlying necrotic tissue necessitated surgical debridement.
The role of surgery in managing pyoderma gangrenosum has been debated.1-3 Surgery is often avoided because of the potential for additional pathergy, and the degree to which improvements in the patient’s condition can be seen with solely medical therapy.
Treatment options. Common treatments for milder forms of disease include intralesional administration of corticosteroids or a calcineurin inhibitor.5 For more advanced disease, first-line therapies include systemic corticosteroids and immunosuppressive agents including cyclosporine.1,2,4,5 Dutiful wound care with nonadherent dressings is an important component of treatment, as ulcers may take months to heal.1,2 Second-line therapies include tumor necrosis factor-α inhibitors (namely, infliximab) and other biologic agents with activity against interleukin 12/23 and 1.1,2 These and other cytokines prompt the heavy neutrophilic response that is characteristic of pyoderma gangrenosum and are among primary targets of therapy.1,2,4
Research is ongoing comparing the efficacy of these agents; investigational therapeutics targeting other proinflammatory interleukins are also being studied.1,2 As previously stated, trauma must be avoided.2,4 Surgery to salvage threatened underlying connective tissues can involve flap procedures or skin grafting.6 As traditional autologous split-thickness grafting causes another wound from the donor site, graft selection of bioengineered skin products is a potential treatment consideration.3 Finally, treatment of comorbid bowel disease or other medical conditions associated with pyoderma gangrenosum may improve response to treatment.
Patient outcome. As seen in other case reports,3,6 our patient required skin grafting because of the extensive level of debridement. The patient completed approximately 3 weeks of antibiotic therapy. After she completed inpatient rehabilitation, the patient was referred to a tertiary medical center for interdisciplinary care involving coordinated gastroenterology, dermatology, and plastic surgery services. She will require ongoing medical management for Crohn disease and interval follow-up with dermatology.
References
1. Ahronowitz I, Harp J, Shinkai K. Etiology and management of pyoderma gangrenosum: a comprehensive review. Am J Clin Dermatol. 2012;13(3):191-211. http://doi.org/10.2165/11595240-000000000-00000
2. Alavi A, French LE, Davis MD, Brassard A, Kirsner RS. Pyoderma gangrenosum: an update on pathophysiology, diagnosis and treatment. Am J Clin Dermatol. 2017;18(3):355-372. http://doi.org/10.1007/s40257-017-0251-7
3. Eisendle K, Thuile T, Deluca J, Pichler M. Surgical treatment of pyoderma gangrenosum with negative pressure wound therapy and skin grafting, including xenografts: personal experience and comprehensive review on 161 cases. Adv Wound Care (New Rochelle). 2020;9(7):405-425. http://doi.org/10.1089/wound.2020.1160
4. George C, Deroide F, Rustin M. Pyoderma gangrenosum - a guide to diagnosis and management. Clin Med J (London). 2019;19(3):224-228. https://doi.org/10.7861/clinmedicine.19-3-224
5. Hypersensitivity syndromes and vasculitis. In: Habif TP. Clinical Dermatology: A Color Guide to Diagnosis and Therapy. 4th ed. Elsevier; 2004: 653-655.
6. Shen J, Zhang W, Jiang X. Pyoderma gangrenosum after cesarean section treated with skin graft: a case report. Medicine (Baltimore). 2019:98(18):e15380. http://doi.org/10.1097/MD.0000000000015380