CDC Recommendations for Limiting Exposure to Opportunistic Pathogens in HIV-Infected Patients
Primary Care Update
Brief Summaries for Clinical Practice
Despite the widespread use of potent combination antiretroviral therapy, opportunistic infections continue to cause considerable morbidity and mortality in persons with HIV infection.1 Thus, the exposure of HIV-infected patients to opportunistic pathogens remains a concern.
Should you recommend that an HIV-infected patient give up a pet cat? What advice would you offer a patient who works at a correctional institution? And what precautions are necessary for a patient who plans an extended stay in Honduras?
Answers to these and related questions about preventing opportunistic infections in HIV-infected persons can be found in updated recommendations from the CDC, the National Institutes of Health, and the Infectious Diseases Society of America.2 Highlights follow.
SEXUALLY TRANSMITTED INFECTIONS
Condoms. Emphasize the importance of using a male latex condom during every act of sexual intercourse to prevent the transmission of HIV and reduce the risk of acquiring other sexually transmitted infections (STIs), including syphilis, chlamydia, gonorrhea, and trichomoniasis. The data regarding the effectiveness of female condoms in preventing transmission are limited.
Oral-anal contact. Advise patients to avoid sexual practices that may result in oral exposure to feces. This reduces the risk of intestinal infections, such as cryptosporidiosis, shigellosis, campylobacteriosis, amebiasis, giardiasis, and hepatitis A.
Screening. Screen all HIV-infected patients, including those who are asymptomatic, at least once for STIs. Screening should include testing for syphilis, trichomoniasis in women, urogenital gonorrhea and chlamydia, and oral and rectal gonorrhea and chlamydia for patients who engage in receptive sex.
Immunization. Recommend hepatitis B vaccination to all susceptible (hepatitis B core antibody-negative) patients with HIV infection. Also recommend hepatitis A vaccination to susceptible men who have sex with men, as well as to other patients with indications for the hepatitis A virus vaccine (eg, injection-drug users, persons with chronic liver disease, and those who are infected with hepatitis B and/or C).
 INJECTION DRUG USE
INJECTION DRUG USE
Injection drug use increases the risk of exposure to hepatitis B and C viruses, drug-resistant strains of HIV, and other blood-borne pathogens. Encourage patients who use illegal drugs to enter and complete substance-abuse treatment, including relapse-prevention programs. Advise patients who continue to inject drugs about strategies to minimize their risk of infection and of transmitting infectious agents to others (Table).3
WORK-RELATED AND ENVIRONMENTAL RISKS
Health care and correctional institutions and homeless shelters. Workers and volunteers at these facilities may be at increased risk for exposure to tuberculosis. In determining the level of risk—and whether an HIV-infected patient should continue working in these environments—consider his or her job duties, the prevalence of tuberculosis in the community, and the extent of tuberculosis-transmission precautions in the workplace. These factors can also help you decide how often to screen the patient for tuberculosis.
Child care settings. Care providers, parents, and children alike are at risk for cytomegalovirus infection, cryptosporidiosis, and other infections (eg, hepatitis A and giardiasis). Good hygienic practices, such as hand washing after any contact with feces, urine, or saliva, can reduce the likelihood of transmission.
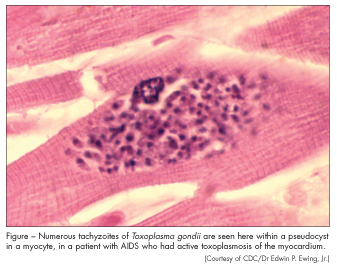
Working with animals. HIV-infected patients who work with animals, such as veterinarians and farm workers, are at risk for cryptosporidiosis, toxoplasmosis (Figure), salmonellosis, campylobacteriosis, and bartonellosis. However, the available data are insufficient to justify a recommendation against such work.
Other activities. Advise patients who garden to wash their hands after soil exposure. This precaution may reduce the risk of cryptosporidiosis and toxoplasmosis.
Tell patients who live in areas where histoplasmosis is endemic to avoid cleaning chicken coops; disturbing soil beneath bird-roosting sites; cleaning, remodeling, or demolishing old buildings; and exploring caves. In coccidioidomycosis-endemic areas, advise patients to avoid exposure to disturbed soil, such as at an excavation site.
PETS
General precautions. Discuss with your patients the risks of owning a pet—especially a cat, which is a potential source of toxoplasmosis and bartonellosis, as well as enteric infections. Weigh the psychological benefits of pet ownership against these risks.
Pets that belong to HIV-infected patients require veterinary care if diarrhea develops. Fecal samples from the pet should be examined for Cryptosporidium, Salmonella, Campylobacter, and Shiga toxin–producing Escherichia coli. Tell patients to avoid contact with the pet until the diarrheal illness has resolved.
 New pets. Advise patients to avoid strays and animals younger than 6 months (cats younger than 1 year), especially those with diarrhea. Tell patients to use caution if they are considering acquiring a pet from a breeding facility, a pet store, or an animal shelter, because the sanitary conditions can vary widely.
New pets. Advise patients to avoid strays and animals younger than 6 months (cats younger than 1 year), especially those with diarrhea. Tell patients to use caution if they are considering acquiring a pet from a breeding facility, a pet store, or an animal shelter, because the sanitary conditions can vary widely.
Hygiene. Stress the importance of hand washing after handling pets (especially before eating); ask parents and other caretakers to supervise HIV-infected children when they wash their hands. Handling pet feces should be avoided to reduce the risk of such diseases as cryptosporidiosis, salmonellosis, and campylobacteriosis.
Cats. Litter boxes should be cleaned daily, preferably by an HIV-negative person who is not pregnant; if the patient performs this task, recommend thorough hand washing afterward to reduce the risk of toxoplasmosis. To further reduce the risk, cats should be kept indoors, not allowed to hunt, and not fed raw or undercooked meat. Tell patients to try to avoid cat bites and scratches, which pose the risk of Bartonella infection.
Exotic and cold-blooded pets. Warn patients to avoid contact with exotic pets (eg, monkeys) and reptiles. Advise them to wear gloves while cleaning aquariums to decrease the risk of infection with Mycobacterium marinum.
FOOD AND WATER
Food. Tell patients to avoid foods that may contain raw eggs (eg, certain salad dressings and mayonnaise); raw or undercooked poultry, meat, or seafood; unpasteurized dairy products and fruit juices; and raw seed sprouts. Advise them to cook meat and poultry until no longer pink in the middle (internal temperature greater than 82.2°C [180°F] for poultry and greater than 73.8°C [165°F] for red meat). Produce should be washed thoroughly before being eaten.
Warn patients of the risk of cross-contamination of food. Uncooked meats should not be allowed to come into contact with other foods. Hands, cutting boards, counters, and knives and other utensils should be washed thoroughly after contact with uncooked foods.
Some soft cheeses and ready-to-eat foods, such as hot dogs and cold cuts, can cause listeriosis. To reduce the risk of this serious disease, advise patients to reheat food until it is steaming.
Water. Tell patients to try to avoid swallowing water while swimming in lakes and rivers because of the risk of cryptosporidiosis and giardiasis. Also, warn them not to swim in water that may be contaminated with sewage or animal waste.
During outbreaks of cryptosporidiosis and in other situations in which a community “boil water” advisory is issued, boiling water for at least 1 minute will eliminate the risk of this disease. Use of submicron personal-use water filters and consumption of bottled water may reduce the risk.
Currently, insufficient data exist to recommend that all HIV-infected persons boil or otherwise avoid drinking tap water in nonoutbreak settings. However, to reduce the risk of waterborne cryptosporidiosis, advise patients to follow precautions similar to those recommended during outbreaks.
TRAVEL
Travel, especially to developing countries, may expose HIV-infected patients to opportunistic infections; those who are severely immunosuppressed are at greatest risk. Consultation with an expert in travel medicine may be useful when the patient plans to visit areas beyond the usual tourist destinations.
General preventive measures. Discuss risks specific to the area, and inform patients of appropriate preventive measures (such as chemoprophylaxis for malaria, protection against arthropod vectors, and treatment with immune globulin). Tell them to avoid direct contact of the skin with soil and sand (eg, by wearing shoes and protective clothing and by using towels on beaches) in areas where fecal contamination of the soil is likely.
Geographically focal infections that pose a high risk to HIV-infected patients include visceral leishmaniasis and several fungal infections,
including Penicillium marneffei infection, coccidioidomycosis, and histoplasmosis. Many tropical and developing areas have high rates of tuberculosis.
Immunizations. Include a review and update of routine vaccinations, including diphtheria-tetanus for adults and all routine immunizations for children. Avoid all live virus vaccines, except for the measles vaccine in nonimmune persons who are not severely immunosuppressed and the varicella vaccine in nonimmunosuppressed adults with asymptomatic HIV infection. Cholera vaccine, which is not available in the United States, is not routinely recommended. Although the yellow fever vaccine has uncertain safety and efficacy in HIV-infected persons, consider offering it to patients with asymptomatic infection who must travel to areas where they are likely to be exposed to the disease.
Food-related and waterborne infections. In developing countries, HIV-infected persons are at even higher risk for food-related and waterborne infections than they are in the United States. Foods and beverages (particularly raw fruits and vegetables, raw or undercooked seafood or meat, tap water, ice made with tap water, unpasteurized milk and dairy products, and items purchased from street vendors) may be contaminated. Generally safe foods include steaming-hot foods, fruits that are peeled by the traveler, bottled beverages, beer, wine, hot coffee or tea, and water brought to a rolling boil for at least 1 minute. Treating water with iodine or chlorine may not be as effective as boiling but can be used—perhaps in conjunction with filtration—when boiling is not practical.
Traveler’s diarrhea. All HIV- infected patients who travel to developing countries should carry a sufficient supply of an antimicrobial agent to be taken empirically if diarrhea develops. One appropriate regimen is ciprofloxacin, 500 mg bid, for 3 to 7 days. An alternative antibiotic in regions with fluoroquinolone resistance is azithromycin. Consider alternative antibiotics (eg, azithromycin) as empirical therapy for use by pregnant women.
Advise patients to consult a local physician if:
•Diarrhea is severe and does not respond to empiric therapy.
•Stools contain blood.
•Fever is associated with shaking chills.
•Dehydration develops.
Warn patients not to use antiperistaltic agents, such as diphenoxylate and loperamide, if they have high fever or blood in the stool. Advise them to discontinue these agents if symptoms persist beyond 48 hours. Antiperistaltic agents are not recommended for children.
Because of the risk of adverse effects and the potential emergence of drug-resistant organisms, antimicrobial prophylaxis for traveler’s diarrhea is not routinely advised for HIV-infected persons who plan to travel to developing countries. However, in selected circumstances, such as when the risk of infection is very high and the period of travel brief, antibiotic prophylaxis may be warranted. Consider a fluoroquinolone, such as ciprofloxacin, 500 mg/d, or rifaximin, 200 mg/d. Fluoroquinolones should not be given to pregnant women. Trimethoprim-sulfamethoxazole (1 double-strength tablet daily) is also effective against traveler’s diarrhea, but resistance is now common in tropical areas.
Travel health reference. The CDC regularly publishes recommendations for prevention of disease in travelers (CDC Health Information for International Travel 2012, “the Yellow Book”) and also maintains a website that allows users to locate prevention recommendations according to geographic destination and to find updates on international disease outbreaks. A detailed review of specific concerns faced by immunocompromised persons who travel abroad is available at this website and in the Yellow Book.4
1. Palella FJ Jr, Baker RK, Moorman AC, et al. Mortality in the highly active antiretroviral therapy era: changing causes of death and disease in the HIV outpatient study. J Acquir Immune Defic Syndr. 2006;43:27-34.
2. Centers for Disease Control and Prevention. Recommendations to help patients avoid exposure to or infection from opportunistic pathogens. MMWR.2009;58(RR04):199-207.
3. US Public Health Service. HIV Prevention Bulletin: Medical Advice for Persons Who Inject Illicit Drugs. May 8, 1997. Rockville, Md: US Public Health Service; 1997. Accessed December 15, 2011.
4. Centers for Disease Control and Prevention. Health Information for International Travel, 2012. Atlanta, GA: US Department of Health and Human Services, Public Health Service. 2011. Available at http://wwwnc.cdc.gov/travel/page/yellowbook-2012-home.htm.


