Peer Reviewed
What Is Causing This Woman’s Swollen, Red, and Tingling Finger?
Authors:
Jonathan Frommelt, MD, and David Effron, MD—Series EditorCitation:
Frommelt J, Effron D. What is causing this woman’s swollen, red, and tingling finger? Consultant. 2018;58(6):e186.
A 60-year-old woman presented to the emergency department (ED) with a 2-week history of swelling, rash, and a tingling sensation in her left middle finger. The symptoms had begun after she had removed a splinter from the tip of that finger a few days after having worked in her garden. Several days after the splinter’s removal, she had begun to experience constant aching pain the finger, radiating to her hand and forearm, with subsequent mild progressive swelling and a lacy rash. These symptoms did not improve with the use of over-the-counter triple antibiotic ointment or warm soaks, prompting her to come to the ED.
The patient denied having fever, chills, nausea, vomiting, diarrhea, or numbness, but she did report having myalgias, arthralgias, swelling, color change, and tingling in the finger. She had a history of irritable bowel syndrome, low back pain, and radiation exposure, as well as a remote history of basal cell carcinoma of the face, which had been surgically excised.
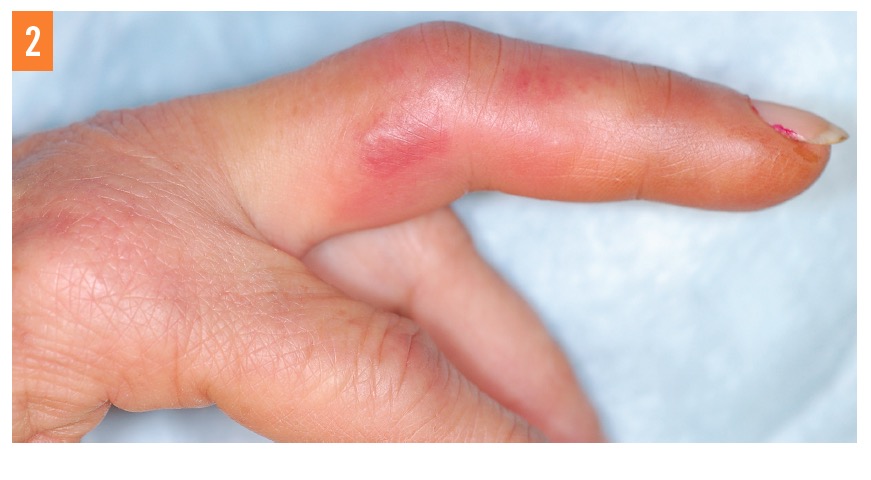
Physical examination findings were notable only for an old, well-healed puncture wound to the ulnar aspect of the volar fat pad of the distal long digit without obvious foreign body; a mottled, erythematous, lacy rash; and mild swelling of the entire digit extending to the metacarpophalangeal joint (Figure 1). The long digit was held in a flexed position, but she did not have any limitation in range of motion (Figure 2). Capillary refill was normal, and there was no notable lymphangitic streaking. Otherwise, she appeared well, with normal vital signs.