Peer Reviewed
Infant Botulism in a Low-Incidence Area: Clinical Recognition and Management
AUTHORS:
Ankhi Dutta, MD, MPH
Assistant Professor, Pediatric Infectious Diseases, Texas Children's Hospital and Baylor College of Medicine, Houston, Texas
Jesus G. Vallejo, MD
Professor, Department of Pediatrics, Pediatric Infectious Diseases, Texas Children's Hospital and Baylor College of Medicine, Houston, Texas
CITATION:
Dutta A, Vallejo JG. Infant botulism in a low-incidence area: clinical recognition and management. Consultant. 2019;59(11):323-326.
ABSTRACT:
Introduction: Infant botulism (IB) is a life-threatening disease that requires prompt clinical diagnosis and treatment. While California reports the highest number of reported IB cases in the United States, Texas ranks fourth in the number of reported cases.
Methods: We conducted a retrospective review of cases of botulism in infants admitted to a tertiary care hospital in Texas from January 2010 to May 2018. We describe the epidemiology of IB in Texas, along with demographics, exposures, clinical features, hospital course, management, and outcome in these patients.
Results: Eight infants with botulism were admitted to our institution from January 2010 to May 2018. The median age of patients with IB was 120.5 days (range, 34-147 days). All patients in our series presented with constipation and signs of symmetric bulbar paralysis. Except for 1 patient with known exposure to raw honey, none of the other patients had a specific known risk factor for IB. Four of the 8 patients had acute respiratory failure secondary to botulism, and 7 of the 8 required nasogastric tube feeding. All patients were treated with intravenous botulism immune globulin and showed improvement in bulbar paralysis at a median of 6.5 hospital days (range, 4-15 days).
Conclusion: Early recognition of IB is crucial to the prompt diagnosis and management of the disease. Clinicians in areas where IB is relatively rare, such as Texas, should be aware of the key clinical signs and symptoms and the diagnostic and treatment plan to prevent associated morbidity and mortality.
Infant botulism (IB) is the most common form of human botulism in the United States. It is caused by Clostridium botulinum and results from ingestion of C botulinum spores, which germinate and produce botulinum toxin and colonize the large intestinal mucosa.1 The toxin causes intestinal immobility and blocks the release of acetylcholine at the neuromuscular junction, leading to descending paralysis.1 The course of IB is very variable but causes significant morbidity and, if untreated, death. Early recognition of IB is crucial for initiating prompt treatment. We aimed to describe the patients with IB admitted to our institution over an approximately 8-year period.
METHODS
We conducted a retrospective review of infants aged 12 months or younger admitted with a diagnosis of IB from January 2010 to May 2018 at Texas Children's Hospital, which is the largest tertiary care hospital in Texas. Cases were identified by ICD-9/ICD-10 codes for botulism, and cases with a diagnosis of wound botulism or foodborne botulism were excluded. We reviewed the electronic medical records for demographics, clinical features, exposures, hospital course, laboratory and imaging results, management, and follow-up (up to 30 days postdischarge). Our study was approved by the institutional review board.
RESULTS
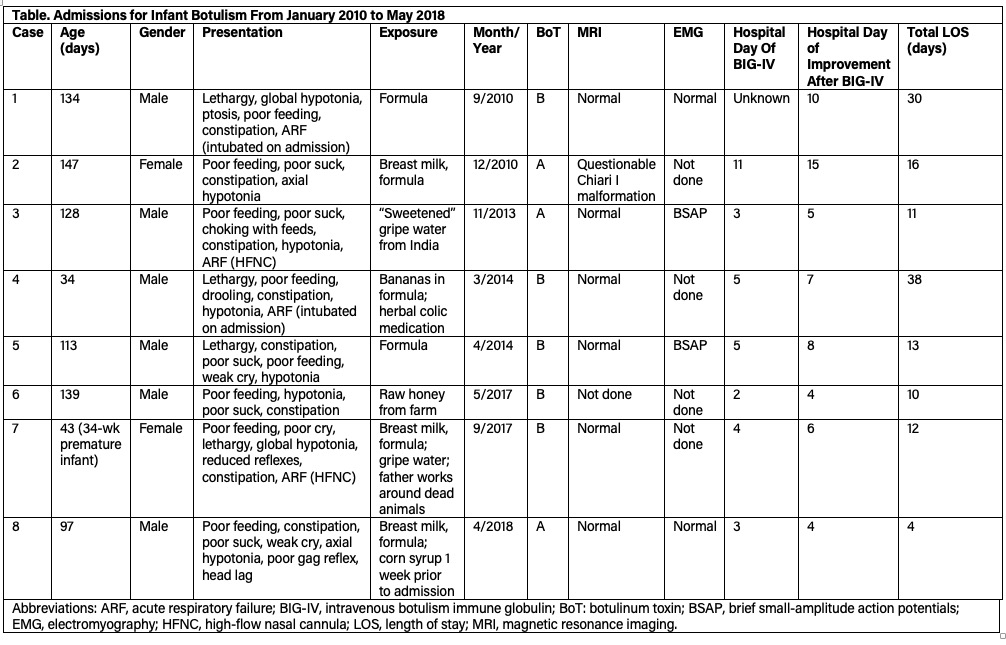
We identified 8 patients with IB who were admitted to our hospital from January 2010 to May 2018 (Table).
The median age of patients with IB was 120.5 days (range, 34-147 days). Infants in the cohort presented with symptoms of 2 to 21 days’ duration (not shown in the Table). All patients in our series presented with constipation and signs of symmetric bulbar paralysis, such as poor feeding, weak suck, decreased gag reflex, and axial hypotonia, which prompted the evaluation for botulism. Ptosis was documented in only 2 patients.
Only 1 patient had a history of exposure to raw honey, 1 patient had a history of store-bought corn syrup ingestion, and 3 patients had a history of some medication or remedy for colic. All of the patients were on formula for term infants (3 of whom were also breastfeeding). No patients had a history of honey pacifier use. We did not conclusively document dust or soil exposure in the patients. However, 2 patients may have been exposed to the local dust or soil through occupational exposures of family members.
A complete blood cell count, a comprehensive metabolic panel, and brain imaging were performed on all of the patients, and all results were unremarkable. All patients in our series had positive stool studies for C botulinum culture and botulinum toxin. Other studies performed are listed in the Table.
Two patients were intubated on admission, while 2 others were on a high-flow nasal cannula for respiratory support. All but 1 patient were on nasogastric tube feedings. The mean hospital length of stay (LOS) was 16.75 days (range, 4-38 days), with intubated patients accounting for the longest stays. Except for the 2 patients who were intubated at presentation, the duration of stay in the intensive care unit (ICU) was 48 hours. In our series, the age distribution was equal between both botulinum toxins A and B. Regardless of toxin type, all the infants showed improvement in their bulbar paralysis at a median of 6.5 hospital days (range 4-15 days) and approximately 48 hours after intravenous botulism immune globulin (BIG-IV) administration. All of the patients recovered and had normal neurological examination findings and normal oral motor skills at follow-up.
DISCUSSION
Clinical features, diagnosis, and management. According to the Centers for Disease Control and Prevention (CDC), IB is defined as clinical illness in children younger than 12 months of age that is characterized by constipation, poor feeding, and failure to thrive that may be followed by progressive weakness, impaired respiration, and death.2
The diagnosis of IB is confirmed by the identification of C botulinum toxin in serum or stool or by isolation of C botulinum from stool.3 IB occurs when the ingested spores colonize the large intestine and produce botulinum neurotoxins. C botulinum is known to produce 8 different toxins, A through H, of which types A, B, E, and F are known to cause human disease.1,4,5 The neurotoxins are transported to the neuromuscular junction where they block the release of acetylcholine, resulting in flaccid paralysis. The treatment of IB relies on replenishing the acetylcholine in the neuromuscular junction. BIG-IV neutralizes circulating botulinum toxin and has a half-life of 28 days (it remains in the circulation for approximately 6 months after administration), which allows the nerve endings to regenerate.1,5
Serum assays for botulinum toxin are usually negative in cases of IB. Since results of stool or serum testing for botulinum toxin are not available for days, it is recommended that health care providers contact the Infant Botulism Treatment and Prevention Program, administered by the California Department of Public Health (https://www.cdph.ca.gov/Programs/CID/DCDC/Pages/InfantBotulism.aspx; [510] 231-7600) as soon as a diagnosis of IB is suspected, to obtain BIG-IV.3
IB most commonly occurs in children between 1 and 6 months of age. The youngest IB patient reported in the literature was 38 hours old, and IB was caused by Clostridium baratii type F toxin.6 Infants in our cohort presented with symptoms of 48 hours to 21 days. In a series of cases from California, the duration of symptoms prior to presentation ranged from 0 to 22 days, and the median age at admission was 91 days (range, 20-247 days).4 Consistent with other studies, all of the infants in our series presented with constipation and signs of symmetric bulbar paralysis.
Epidemiology. IB results from the ingestion of C botulinum spores, mostly found in dust and soil. In the United States, B type toxin is most prevalent east of the Mississippi River and A type toxin west of the Rocky Mountains,1,4,7,8 In cases reported from California over a period of 20 years, the most commonly isolated toxins were A and B.3
While California has the highest reported US incidence of IB, 65 cases of IB were reported in Texas from 2007 to 2017—8 cases in 2017, and 7 cases in each of the years from 2013 to 2016.9 One case was reported in 2012, and 4 cases in 2011, according to the Texas Department of State Health Services.
Although honey ingestion is still considered a predominant source of botulism in infants in Europe (58%), most cases of IB in the United States are idiopathic, with only 20% of cases attributed to honey ingestion.10 However, between August 2018 and November 2018, 4 cases of IB were reported in Texas linked to honey pacifiers bought from Mexico.11 Two clades have been identified in IB cases reported from California associated with honey consumption: A2 and B5.12 Only 1 of the infants in our study had a history of possible honey consumption, and the disease was caused by type B toxin. However, amplified fragment-length polymorphism (AFLP) studies were not performed to identify the clade. Only 2 of the formulas in our cohort were tested for botulinum toxin, and both were negative. The “sweetened” gripe water of 1 of the patients also was tested for botulinum toxin and was negative.
Dust and soil exposure also are considered risk factors for IB. Geographic temporal clustering of the clades of botulism suggests that local soil and climatic conditions contribute to the spread of botulism spores.12 Dusts and soil specimens from the home environment of affected infants have demonstrated similar C botulinum clades by AFLP.12 IB seems to have a seasonal pattern in California, with a higher incidence during drier months. Most of the cases occurred in Los Angeles County, and an increase in the incidence of IB occurred after the Northridge earthquake of 1994, highlighting the role of dust and dirt in dissemination of C botulinum spores into the air.13 In Philadelphia, the peak months for IB cases were October and November; however, the overall incidence was similar throughout the year.7 We did not find a seasonal pattern in our cases. The number of IB cases in Texas was highest in drier areas and in areas where the probability of dust is higher and the relative humidity lower, which possibly helps the spores to germinate and spread.
Hospital course and the utility of BIG-IV. In a 12-year study done in Philadelphia from 1976 to 1987, prior to the introduction of BIG-IV, the mean duration of hospital LOS reported was 44 days (range, 9-201 days), with most patients (54/57) admitted to the ICU.7 The mean LOS in the ICU was 25 days (range, 1-149 days).
There has been a significant improvement in these parameters after the introduction of BIG-IV. In treated patients, the LOS was significantly reduced from 27 days vs 15 days in one study and from 5.7 weeks to 2.2 weeks in a second study.13,14 The ICU LOS also was reduced from 27 days to 9 days when BIG-IV was administered.13 The shortened LOS has been shown to reduce hospital charges by an average of $88,900 per patient.14 The reduction in LOS was associated with the timing of BIG-IV administration. Treatment on hospital days 0 through 3 reduced the mean LOS by 3.7 weeks compared with treatment on hospital days 8 through 10, which reduced the mean LOS by only 1 week.14,15
Interestingly, the rates of intubation and ventilator support or nasogastric feeding in patients with IB were not significantly different before and after the introduction of BIG-IV, suggesting that supportive care is still critical in the management of IB.4,13 In our study, except for the 2 patients who were intubated at presentation, LOS in the ICU was only 48 hours, which is lower than in most reported studies. Patients with IB caused by botulinum toxin A have been shown to be older, have increased LOS, and increased duration of intubation.13 In our series, the age distribution was equal between both botulinum toxin A and B. Due to the small number of cases in our series, the significance of the toxin type on disease severity cannot be ascertained. As with the patients in our series, all patients with IB improved and had normal neurological examination findings at follow-up.4,8
Differential diagnosis. Several neurological diseases and infections can mimic IB. The most common is spinal muscular atrophy (SMA), accounting for 19% of IB cases in one study.15 Generally, the duration of symptoms of IB is acute, occurring within hours to a few days, whereas symptoms of SMA run an indolent course and are present for weeks to months preceding admission. Additionally, SMA typically spares sphincter and extraocular muscles, whereas IB generally involves both.
Other considerations in a child with hypotonia and bulbar palsy are hypothyroidism, metabolic disorders, Guillain-Barré syndrome, and infections.1,5,16
Conclusion. IB is a rare but life-threatening disease. However, if treated promptly, outcomes are excellent. Clinical suspicion of IB should be high in infants presenting with constipation and symmetric bulbar paralyses, even in the absence of traditional honey exposure. Careful history and physical examination followed by prompt administration of BIG-IV while awaiting confirmatory stool studies for botulinum toxin should be undertaken. Because other diseases can mimic IB, simultaneous testing, especially to rule out SMA, could be performed. A multidisciplinary team approach should be initiated promptly, including close neurological monitoring, nutritional support, occupational and physical therapy, neurology, and infectious diseases consultation.
- Khouri JM, Arnon SS. Infant botulism. In: Cherry JD, Harrison GJ, Kaplan SL, Steinbach WJ, Hotez PJ, eds. Feigin and Cherry’s Textbook of Pediatric Infectious Diseases. Vol 8th ed. Philadelphia, PA: Elsevier; 2019:chap 147.
- Botulism (Clostridium botulinum): 2011 case definition. Centers for Disease Control and Prevention. https://wwwn.cdc.gov/nndss/conditions/botulism/case-definition/2011/. Accessed September 25, 2019.
- Botulism: Information for health professionals. Centers for Disease Control and Prevention. https://www.cdc.gov/botulism/health-professional.html. Reviewed October 4, 2018. Accessed September 25, 2019.
- Tseng-Ong L, Mitchell WG. Infant botulism: 20 years’ experience at a single institution. J Child Neurol. 2007;22(12):1333-1337.
- Pifko E, Price A, Sterner S. Infant botulism and indications for administration of botulism immune globulin. Pediatr Emerg Care. 2014;30(2):120-124.
- Barash JR, Tang TWH, Arnon SS. First case of infant botulism caused by Clostridium baratii type F in California. J Clin Microbiol. 2005;43(8):4280-4282.
- Schreiner MS, Field E, Ruddy R. Infant botulism: a review of 12 years’ experience at the Children’s Hospital of Philadelphia. Pediatrics. 1991;87(2):159-165.
- Thompson JA, Glasgow LA, Warpinski JR, Olson C. Infant botulism: clinical spectrum and epidemiology. Pediatrics. 1980;66(6):936-942.
- Reported botulism cases and incidence rates in Texas, 2007-2017. Texas Department of State Health Services. https://dshs.texas.gov/IDCU/disease/botulism/Data.aspx. Updated March 17, 2019. Accessed September 25, 2019.
- Fox CK, Keet CA, Strober JB. Recent advances in infant botulism. Pediatr Neurol. 2005;32(3):149-154.
- Health alert: infant botulism and risk of honey pacifiers botulism. Texas Department of Health Services. https://www.dshs.state.tx.us/news/releases/2018/HealthAlert-11162018.aspx. November 16, 2018. Accessed September 25, 2019.
- Dabritz HA, Hill KK, Barash JR, et al. Molecular epidemiology of infant botulism in California and elsewhere, 1976-2010. J Infect Dis. 2014;210(11):1711-1722.
- Underwood K, Rubin S, Deakers T, Newth C. Infant botulism: a 30-year experience spanning the introduction of botulism immune globulin intravenous in the intensive care unit at Childrens Hospital Los Angeles. Pediatrics. 2007;120(6):e1380-e1385.
- Payne JR, Khouri JM, Jewell NP, Arnon SS. Efficacy of human botulism immune globulin for the treatment of infant botulism: the first 12 years post licensure. J Pediatr. 2018;193:172-177.
- Arnon SS, Schechter R, Maslanka SE, Jewell NP, Hatheway CL. Human botulism immune globulin for the treatment of infant botulism. N Engl J Med. 2006;354(5):462-471.
- Khouri JM, Payne JR, Arnon SS. More clinical mimics of infant botulism. J Pediatr. 2018;193:178-182.