Peer Reviewed
Skin Signs of Vascular Disorders
Author:
Robert P. Blereau, MD
Morgan City, Louisiana
Citation:
Blereau RP. Leukocytoclastic vasculitis. Consultant. 2013;53(3):250-251.
Leukocytoclastic Vasculitis
A 16-year-old girl was bothered by ankle pain and “red spots” on her lower legs. These symptoms cleared in a few days without treatment. Six weeks later, after returning from an all-day outing at a fair, she noticed that the spots had reappeared (A) and hemorrhagic lesions had developed on the right ankle (B) and left heel (C). After removing her shoes, the teenager felt severe pain in both ankles, particularly the right.



Unable to walk, the patient was taken to the emergency department the following morning. She was afebrile, had no other lesions or joint pain, and was taking no medications. The complete blood cell count and sedimentation rate were normal. Antinuclear antibody titer was negative.
An elliptical incisional biopsy was performed on the large left heel lesion, and an excisional biopsy was done on the purpuric lesion on the same leg. Microscopically, both sites revealed small vascular structures, primarily capillaries, surrounded by abundant polymorphonuclear leukocytes and few eosinophils, evidence that confirmed the diagnosis of leukocytoclastic vasculitis.
Leukocytoclastic, or hypersensitivity, vasculitis is a neutrophilic inflammation of small blood vessels.1 Symptoms may include purpura, malaise, myalgias, and fever; oligoarthritis or monarthritis is associated with 40% of cases.2 Three characteristics are significant in making this diagnosis:
- The purpura is nonblanching.
- Purpuric patches are found on dependent areas of the body; symmetric distribution on the legs, thighs, and buttocks is typical.
- Each macule is regular and approximately circular.
The course of leukocytoclastic vasculitis generally is benign. This patient was treated with oral prednisone, and her condition promptly improved.
REFERENCES
- Habif TP. Clinical Dermatology: A Color Guide to Diagnosis and Therapy. 3rd ed. St Louis: Mosby; 1996:579-582.
- Olewiler SD. Photoclinic: leukocytoclastic vasculitis. Consultant. 1994;34:1482-1483.
Atrophie Blanche
Authors:
Charles E. Crutchfield III, MD
Eagan, Minnesota
Eric J. Lewis, MD
Morris, Minnesota
Humberto Gallego, MD
La Mesa, California
Citation:
Crutchfield CE, Lewis EJ, Gallego H. Atrophie blanche. Consultant. 2013;53(3):251.

A 57-year-old man with a history of venous stasis leg ulceration wondered about the “white spots” on his leg. The condition is atrophie blanche, which manifests as smooth, ivory-white macules and plaques of sclerosis stippled with telangiectasia that often are surrounded by mild to moderate pigmentation.
Atrophie blanche is seen most commonly in association with the healing phase of livedo vasculopathy and hypertensive vasculopathy, but it is noted also as a nonspecific finding in diabetes mellitus, dysproteinemic states, lupus erythematosus, and venous stasis.
Treatment for atrophie blanche is directed at prevention by addressing the underlying medical condition.
Polycythemia Vera
Author:
Reynold C. Wong, MD
Roseville, California
Citation:
Wong RD. Polycythemia vera. Consultant. 2013;53(3):252.

Four months after a patchy, macular, erythematous spot erupted on the dorsum of a 63-year-old woman’s left foot, the area became ulcerated, tender, and painful. The 1.2-cm ulcer was covered by a hemorrhagic crust surrounded by a cyanotic reticular discoloration of the skin.
The patient’s white blood cell count was 15,500/µL; red blood cells, 7.7 million/µL; hemoglobin, 18.5 g/dL; hematocrit, 59.9%; and platelet count, 845,000/µL. Her distal pedal pulses were strong. A biopsy of tissue from the affected area revealed superficial thrombophlebitis.
Polycythemia vera, characterized by an abnormal proliferation of bone marrow elements—erythrocytes, leukocytes, and platelets—was diagnosed. This disorder is also marked by increased red cell mass and total blood volume. The cause is unknown.
Some patients with polycythemia vera are asymptomatic; others may exhibit a range of symptoms, including a ruddy complexion, pruritus, weakness, headache or light-headedness, visual disturbances, and dyspnea. Petechiae, ecchymoses, arterial thrombosis, thrombophlebitis, leg ulcers, and livedo reticularis are also seen.
After the patient underwent phlebotomy for several months, her leg ulcer healed.
Alkylating agents and interferon also may be used to treat polycythemia vera. Treatment of this disorder can reduce the incidence of superficial thrombophlebitis.
Nasal Hemangioma
Author:
Youn W. Park, MD
Barberton, Ohio
Citation:
Park YW. Nasal hemangioma. Consultant. 2013;53(3):253.
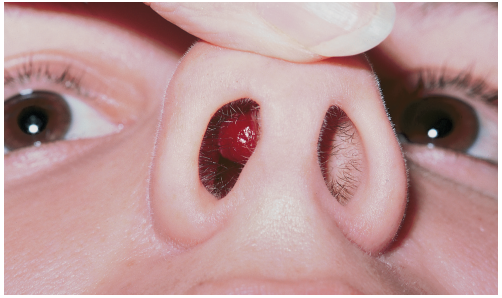
A 21-year-old woman had suffered recurrent nosebleeds and pain in her nose for the previous 2 months. Physical examination revealed an extremely vascular, slowly enlarging intranasal growth on the anterior surface of the septum.
The tumor and surrounding normal mucosa and perichondrium were resected, with the patient under local anesthesia. Nasal packing was applied following closure of the wound.
Nasal hemangiomas occur four times as often in women as in men and are rare before puberty. They arise as polypoid or sessile lesions of the anterior septal mucosa; occasionally, they may develop from the mucosa of the paranasal sinuses.
Osler-Weber-Rendu disease, inflammatory polyp, granuloma gravidarum, and pyogenic granuloma are among the other vascular or inflammatory lesions that need to be considered in the differential diagnosis.
Complete excision of the nasal hemangioma prevents recurrence.
Erythema Elevatum Diutinum
Authors:
Charles E. Crutchfield III, MD
Eagan, Minnesota
Eric J. Lewis, MD
Morris, Minnesota
Humberto Gallego, MD
La Mesa, California
Citation:
Crutchfield CE, Lewis EJ, Gallego H. Erythema elevatum diutinum. Consultant. 2013;53(3):253.

This rare condition affects both men and women. The average age at onset is 53 years.1 The lesions are deep brownish red to purple papules, nodules, and plaques. Blisters and ulcers also can occur, as pictured here.
Eruptions may be seen anywhere on the body but are often found on the extensor surfaces of the extremities and, particularly, the joints. Erythema elevatum diutinum lesions can clinically resemble those of Kaposi’s sarcoma and Sweet’s syndrome.
Most likely, this disease is caused by immune complex deposition (Arthus reaction) in the dermal vessels. Excessive exposure to antigens, as from recurrent infections, or situations in which high levels of antibody occur (paraproteinemias) are likely to cause immune complexes with subsequent vessel deposition. Medical problems, such as myeloproliferative disorders and chronic or recurrent infections, also may be associated with the condition.
Histologically, erythema elevatum diutinum represents a localized vasculitis accompanied by a rich neutrophilic and histiocytic infiltrate. Dermal fibrosis and lipid deposits may be seen in older lesions.
Dapsone is the treatment of choice.
REFERENCE
- Habif TP. Clinical Dermatology: A Color Guide to Diagnosis and Therapy. 3rd ed. St Louis: Mosby; 1996:591.
Schamberg’s Disease
Author:
Robert P. Blereau, MD
Morgan City, Louisiana
Citation:
Blereau RP. Schamberg's disease. Consultant. 2013;53(3):254.
These orange-to-brown macules with red puncta, or cayenne pepper spots, are typical of Schamberg’s disease (progressive pigmented purpuric dermatosis). The cause of this disorder is unknown, but it may be related to a cellular immune reaction or drug reaction.
A biopsy of tissue from the affected areas of a 70-year-old man’s legs (A) revealed perivascular lymphohistiocytic infiltrate of the epidermis with focal red blood cell extravasation. These findings confirmed the diagnosis of Schamberg’s disease.

An asymptomatic purpura developed on the lower legs and feet of a 60-year-old man (B). When this picture was taken, the patient’s international normalized ratio was 2.45. He was taking warfarin for chronic atrial fibrillation and nabumetone for osteoarthritis. It was thought that one or both of these medications contributed to this patient’s disease.

A 31-year-old woman’s nonpruritic purpura also involved both legs and feet (C), but it was not attributed to medication. Birth control pills were the only drugs she was taking. Laboratory findings, including complete blood cell count, platelet count, prothrombin time, and partial thromboplastin time, were normal, thereby ruling out a coagulopathy.

There are no hematologic disorders, venous insufficiencies, or internal diseases associated with Schamberg’s disease. It occurs more often in men than in women, and children may be affected. The eruption may last months or years.
The purpura most commonly appears on the lower legs but may erupt on the upper body as well. Usually Schamberg’s disease is asymptomatic, but mild pruritus and scaling may be present. The cayenne pepper spots apparently result from capillary leakage of hemosiderin.
Reassure patients that Schamberg’s purpura is not associated with serious disease. Topical corticosteroids may be applied if itching is bothersome.


