Peer Reviewed
Squamous Cell Carcinoma of Unknown Primary
AUTHORS:
Alexis E. Carrington, MD1 • Nadia Solomon MD, MSc, MA2 • Raja K. Sivamani, MD, MS, AP1,3,4,5,6
AFFILIATIONS:
1Department of Dermatology, University of California-Davis, Sacramento, California
2Mount Sinai Icahn School of Medicine, Elmhurst Hospital Center, Queens, New York
3Department of Biological Sciences, California State University, Sacramento, California
4College of Medicine, California Northstate University, Sacramento, California
5Pacific Skin Institute, Sacramento, California
6Zen Dermatology, Sacramento, California
CITATION:
Carrington AE, Solomon N, Sivamani RK. Squamous cell carcinoma of unknown primary. Consultant. 2021;61(11):e40-42. doi:10.25270/con.2021.02.00011
Received August 28, 2020. Accepted November 18, 2020. Published online February 23, 2021.
DISCLOSURES:
Dr Sivamani serves as a scientific advisor for LearnHealth and Arbonne and as a consultant to Regeneron Pharmaceuticals and Abbvie Pharmaceuticals.
CORRESPONDENCE:
Alexis Carrington, MD, University of California-Davis, 3301 C Street, Suite #1300, Sacramento, CA, 95816 (aecarrington@ucdavis.edu)
A 60-year-old Hispanic man presented to the hospital with a painful, enlarging left inguinal mass that had persisted for 4 months.
History. He had a medical history of hypertension, type 2 diabetes, and benign prostatic hyperplasia (BPH). The patient denied any history of tuberculosis, cough, dyspnea, or fever. He did not have a social history of smoking, alcohol abuse, or multiple sexual partners. The patient also denied any family history of skin cancer or tanning bed use.
Physical examination. At presentation, a review of systems was significant for weight loss and night chills that had persisted for 5 months. The patient’s vital signs were within normal limits. The dermatologist noted a large, erythematous, firm-to-hard inguinal lymph node masquerading as a cyst on the left inguinal fold with overlying erosions and few satellite erythematous papules (Figure 1).
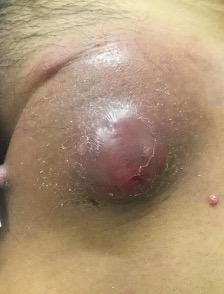
Diagnostic testing. Laboratory test results were notable for a white blood cell count of 12 mg/dL (reference range, 4.8-10.8 mg/dL) with 83% polymorphonuclear leukocytes and an elevated calcium level of 11.4 mg/dL (reference range, 8.6-10.3 mg/dL). The patient’s parathyroid hormone (PTH) level was notably low at 7.7 pg/mL (reference range, 10-65 pg/mL), with a mild elevation in PTH-related protein level (PTHrP; reference range, ≤ 4.2 pmol/L).
While the physical examination results were unrevealing for a definitive lesion consistent with primary cutaneous squamous cell carcinoma (SCC), the left inguinal nodules appeared consistent with metastatic SCC. This prompted further workup to better characterize the lesions and try to identify a primary neoplasm. Abdominal and pelvic computed tomography (CT) scans showed enlargement of the left inguinal lesion, appearing as a heterogeneous soft tissue mass measuring 11.2 × 7.4 cm, with adjacent smaller soft tissue masses extending slightly into the lower pelvis and multiple new enlarged lymph nodes vs masses (Figure 2). Results of a subsequent biopsy via interventional radiology confirmed the diagnosis of metastatic SCC. Results of a whole-body positron emission tomography (PET)/CT scan showed a metabolically active mass in the left groin.
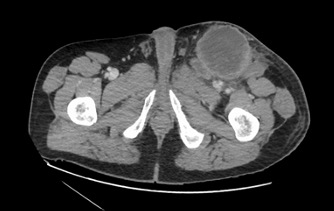
The primary site of the patient’s SCC was investigated, but results of a scrotal ultrasound esophagogastroduodenoscopy, colonoscopy, and laryngoscopy were all negative. Cystoscopy demonstrated bladder trabeculations, but a consultation with urology determined that a bladder outlet obstruction in the setting of BPH caused the bladder wall thickening.
Treatment and management. The tumor board at our institution advised against surgical intervention given the extent of the disease. Therefore, the patient began chemotherapy (taxol/carboplatin weekly) and radiation therapy for 3 weeks with later re-evaluation for possible surgical intervention.
Discussion. Cancer of unknown primary (CUP) refers to a classification of metastatic disease of various histologic subtypes that cannot be traced to an identifiable primary tumor despite extensive workup.1,2 CUPs comprise approximately 3% to 5% of invasive cancers and 2% to 3% of all epithelial malignancies.1,2,3 The majority of these are adenocarcinomas and undifferentiated carcinomas.1,2,3 SCC, neuroendocrine carcinomas, and other uncommon histologies account for 10% of the 2% to 3% of epithelial malignancies.1
The diagnostic workup for CUP is dependent on immunohistological analysis for tumor characterization, along with the aid of molecular techniques. However, efforts to determine the molecular biology of CUP and gene expression profiling have been unsuccessful.1 CUP is associated with poor survival and is identified as the fourth most common cause of cancer deaths.1 Among the histologic subtypes, poorly differentiated carcinomas show the most favorable outcomes.1
As a histologic subtype, SCC is rare, accounts for only about 5% of CUPs, and are noted to occur most frequently in the head and neck.1,2,4 The outcomes are considered favorable.
As in our case, patients with SCC involving inguinal nodes should receive clinical and endoscopic examination and biopsy of suspicious lesions in anal vulva, vagina, uterine cervix, penis, or scrotum.2
Finally, patients with either isolated inguinal lymph-nodal metastatic SCC or one metastatic lesion are classified as having restricted disease. After undergoing typical management with local dissection, with or without local radiation treatment, patients usually have long, disease-free survival.2
When traditional methods are unsuccessful, workup of CUP is advanced by new imaging and endoscopic technologies including PET/CT, magnifying endoscopy in combination with narrow band imaging, and transoral robotic surgery.5 These can identify the primary site in 44% to 71% of cases.5 Fluorodeoxyglucose-PET/CT is an effective method of conducting one-time whole-body imaging in SCC of unknown primary, although it has low specificity.4 Not only can variations in physiologic uptake and inflammatory-related uptake in common potential locations of a primary affect false-positive rates, but also image indication bias (radiologists’ or nuclear medicine physicians’ tendency to call more abnormal findings for SCC of unknown primary than for other indications) may contribute to high false-positive rates as well.4
Human papillomavirus (HPV) status is associated with SCC of unknown primary in the abdomen, pelvis, and retroperitoneum.1 In a previous study, researchers conducted a Medline search and found 51 publications including 24 patients with SCC of unknown primary in the abdomen, pelvis, and retroperitoneum.1 The female-to-male ratio was 3:1 in these studies.1 Ten of the patients were assessed for HPV status. Nine were positive for p16, and 2 were positive for HPV. The patients were more commonly women and were diagnosed at a younger age.1 The patient in our case study was not evaluated for HPV, but his sex and age make this association significantly less likely.
Conclusions. SCC of unknown primary is unusual and documented infrequently in the literature, as is the physical skin manifestation of such an extensive malignancy. While very few epithelial malignancies are without a known primary, an exceedingly small subset of these are SCCs diagnosed based on immunohistological analysis and molecular techniques. Because of the rarity of SCC of unknown primary, the affected population is poorly characterized, particularly in regard to management and outcomes.
Patient outcome. At follow-up, the primary source was still unknown. Radiation therapy and weekly taxol/carboplatin were completed. The patient is currently receiving chemotherapy with gemcitabine/cisplatin.
References
- El Rassy E, Kattan J, Pavlidis N. A new entity of abdominal squamous cell carcinoma of unknown primary. Eur J Clin Invest. 2019;49(7):e13111. https://doi.org/10.1111/eci.13111
- Pavlidis N, Pentheroudakis G. Cancer of unknown primary site. Lancet. 2012;379(9824):1428-1435. https://doi.org/10.1016/s0140-6736(11)61178-1
- Bochtler T, Löffler H, Krämer A. Diagnosis and management of metastatic neoplasms with unknown primary. Semin Diagn Pathol. 2018;35(3):199-206. https://doi.org/10.1053/j.semdp.2017.11.013
- Liu Y. FDG PET/CT for metastatic squamous cell carcinoma of unknown primary of the head and neck. Oral Oncol. 2019;92:46-51. https://doi.org/10.1016/j.oraloncology.2019.03.014
- Kang H, He H, Ma J, et al. Carcinoma of unknown primary detected by whole-body diffusion-weighted imaging: a case report and review of the literature. Radiol Case Rep. 2020;15(7):983-987. https://doi.org/10.1016/j.radcr.2020.04.002


