Nitrous Oxide Shows Antidepressant Effects for Treatment-Resistant Depression
In this video, Charles Conway, MD, professor of psychiatry, Washington University School of Medicine, director, Center for the Advancement of Research in Resistant Mood Disorders, St Louis, Missouri, summarizes new research supporting the use of nitrous oxide for the treatment of treatment-resistant major depression (TRMD).
In a recent study, Dr Conway and co-researchers analyzed the effect of nitrous oxide, an NMDA antagonist, on patients with TRMD and found that certain dosages had antidepressant effects.
Watch part 2 of this video where Dr Conway covers possible side effects of this novel treatment, and next steps for continued research.
Read the Transcript:
Charles Conway: Hello. I'm Charles Conway. I'm a psychiatrist and professor of psychiatry at Washington University, School of Medicine. I also head up the Center for the Advancement of Research in Resistant Mood Disorders at Washington University.
The idea that nitrous oxide could be an antidepressant treatment evolved over many years. There was a group ‑ Steve Mennerick, Chuck Zorumski, and Peter Nagele from our department and department of anesthesiology here at Washington University who have been studying nitrous oxide for many years in a laboratory‑level research as well as animal research.
Over the course of the past 15, 20 years or so, there's been a huge spike in interest in ketamine, which is an NMDA antagonist, and nitrous oxide also is an NMDA antagonist. I was approached about 10 years ago or so by Peter Nagele from the department of anesthesiology about pursuing exploration of nitrous oxide as a treatment for treatment‑resistant depression.
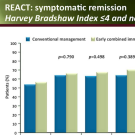
We did our first trial, a double‑blind prospective trial in a group of people with severe treatment‑resistant depression. We had some good results with that, and that led to this most recent study where we actually gave different dosages of nitrous oxide, 0%, 25%, and 50%. We found that 25% and 50% seemed to have roughly equivalent antidepressant effects.
There's some evidence from the basic science studies done in Zorumski and Mennerick's lab that the percentage of nitrous oxide that would be required would be considerably less than 50%.
Fifty percent is the approximate dosage that dentists give for anxiety with dental procedures, but we were noticing when we did the first trial at 50% that a pretty significant percentage of the patients, probably about 5, 10% were experiencing fairly severe nausea. A couple of patients developed vomiting.
We thought it would be good to better define what would be the optimal dose or would be a better tolerated dose. We did this trial. Again, this was a double‑blind prospective trial, so neither the patients or the raters knew who was getting what dose. Only the anesthesiologist knew.
The other thing that we found interesting from the first trial is that the antidepressant effects linger on well beyond the day that you give the treatment. In that first trial, we only gave two weeks separation between placebo and 50%. The second trial, we decided to give an entire month so that we wouldn't get any residual carryover from one treatment to the next.
Probably the most significant finding...There were several findings that were pretty key. One was that 25 and 50% had roughly equivalent efficacy over the course of the entire two weeks that we observed these patients. We knew that 25% likely was going to have some benefit, but we didn't expect it to be about the same as 50%.
The other good thing that we found was that those in the 25% arm had significantly lower side effects. I believe about a 4:1 nausea. The rate of nausea was very low in both groups, but the rate of nausea was higher by about a 4:1 rate in the 50% group versus the 25% group.
The other thing that was interesting was that in both groups, there was sustained benefit, but there seemed to be slightly better sustained benefit in the 50% group, which would suggest that there may be some advantage to a higher concentration, but if a patient doesn't tolerate the higher concentration, there's still some potential benefit from a lower concentration.
One of the big differences in this trial and the first trial is that in both trials, we went after a population of very treatment‑resistant patients. In the first trial, we had a mean number of failed antidepressant trials to get into the trial was 2, but the average number over the first trial was 8 failed trials of antidepressant.
The second trial, we went after a slightly less severe but still very severe population. I believe it's about 4.5 average failed treatments. The results we got on the second trial were significantly better in terms of the percentage of patients who were responding.
I didn't expect to see it this high, but we were seeing about 40%, somewhere around 40, 50% of the patients in both arms were responding to the treatment that over the course of the entire trial, about 85% of the patients had a reduction in their depression scores. The biggest surprise for me probably was that we had this big of effect in a very resistant population.
I think the primary practical application is that we have...It's clear ketamine has been very beneficial, helped a lot of people throughout the country and the world who have this really severe depression, but there are limitations to ketamine and there are some risks associated with ketamine.
It's good that we have lots of options. I would argue that at this point, nitrous oxide is probably not ready for prime time yet. The 2 trials that we've done are relatively small trials, 20 subjects in the first trial and 24 subjects in the second trial. We also have another study ongoing that we've yet to publish.
We need a much larger replication of this. Now that we have some idea about dosing, that gives us an idea of how to pursue a larger trial. The good news is there are a lot of areas emerging in the resistant depression realm that there's hope for a population that really desperately needs hope.
Reference
Charles Conway, MD, received his medical degree at the University of Missouri-Columbia, and served his residency in psychiatry at Duke University Medical Center in Durham, North Carolina. He is a professor of psychiatry at the Washington University School of Medicine in St. Louis, Missouri, in addition to serving as the director of the Center for the Advancement of Research in Resistant Mood Disorders at Washington University, and the director of the Treatment Resistant Depression and Neurostimulation Clinic. His areas of clinical interest include treatment-resistant mood disorders, bipolar disorders, and mood disorders while his research expertise includes treatment-resistant depression, bipolar disorders, and neuroimaging of mood disorders.