Peer Reviewed
A Constellation of Contemporaneous Comorbid Etiologies of Vasculopathy in a Patient With Rheumatoid Arthritis
Introduction. A 61-year-old man was hospitalized for worsening cutaneous ulcerations on his head, extremities, and trunk.
History. The patient had a 40-year medical history significant for rheumatoid arthritis (RA), Sjogren syndrome, and monoclonal gammopathy of undetermined significance (MGUS). At the time of admission, his home medication regimen included leflunomide 20 mg and prednisone 15 mg, both daily. A physical examination demonstrated broad geometric ulcerations with overlying fibrinous necrosis on the head, extremities, and trunk, along with extensive fibrosis and subcutaneous calcific changes of the trunk and shoulders (Figures 1-2). No significant abnormal pulses were noted.
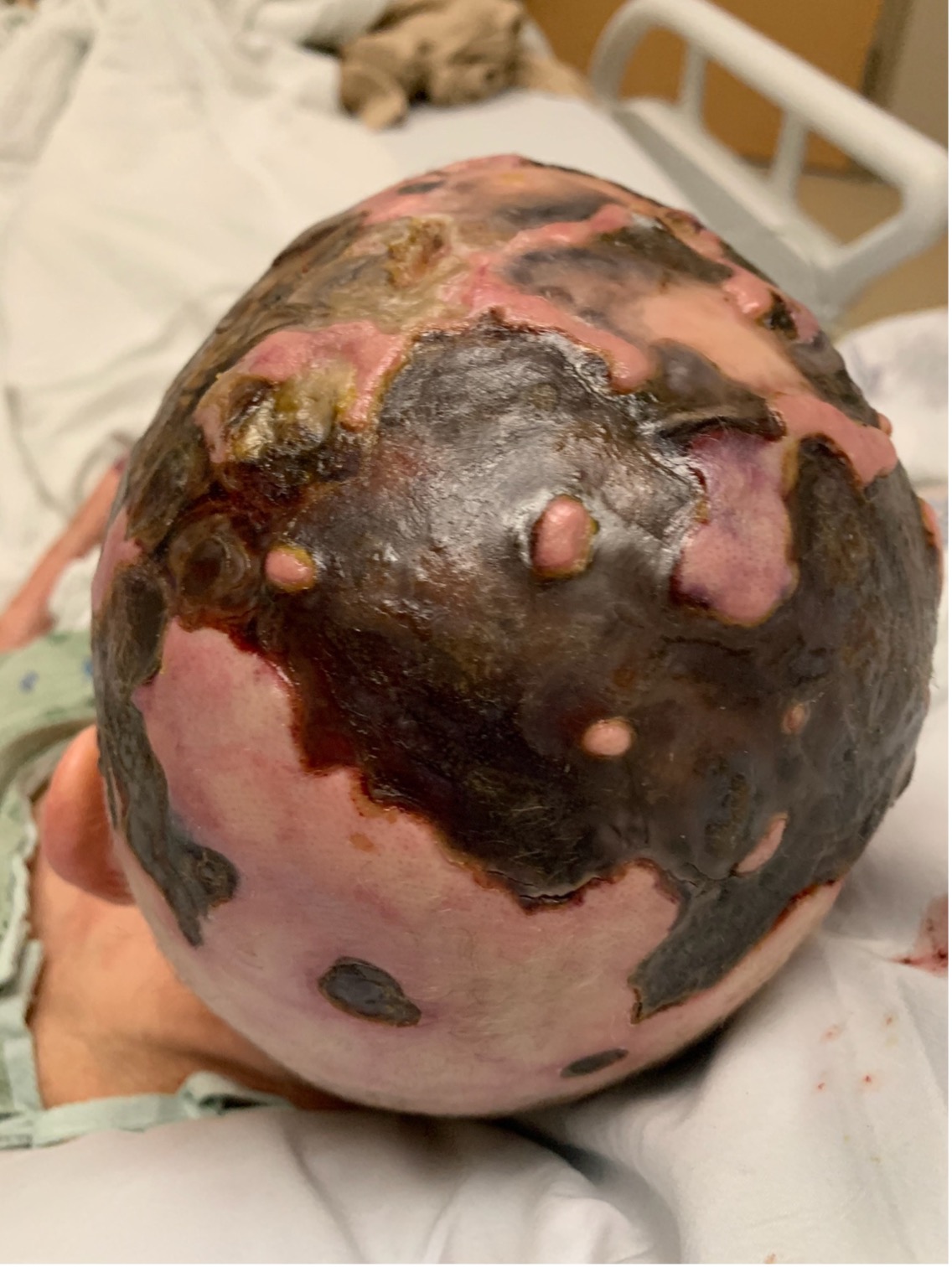
Figure 1. The patient’s initial clinical presentation of broad, geometric, ulcerated plaques with fibrinoid necrosis and perilesional erythema on the scalp.
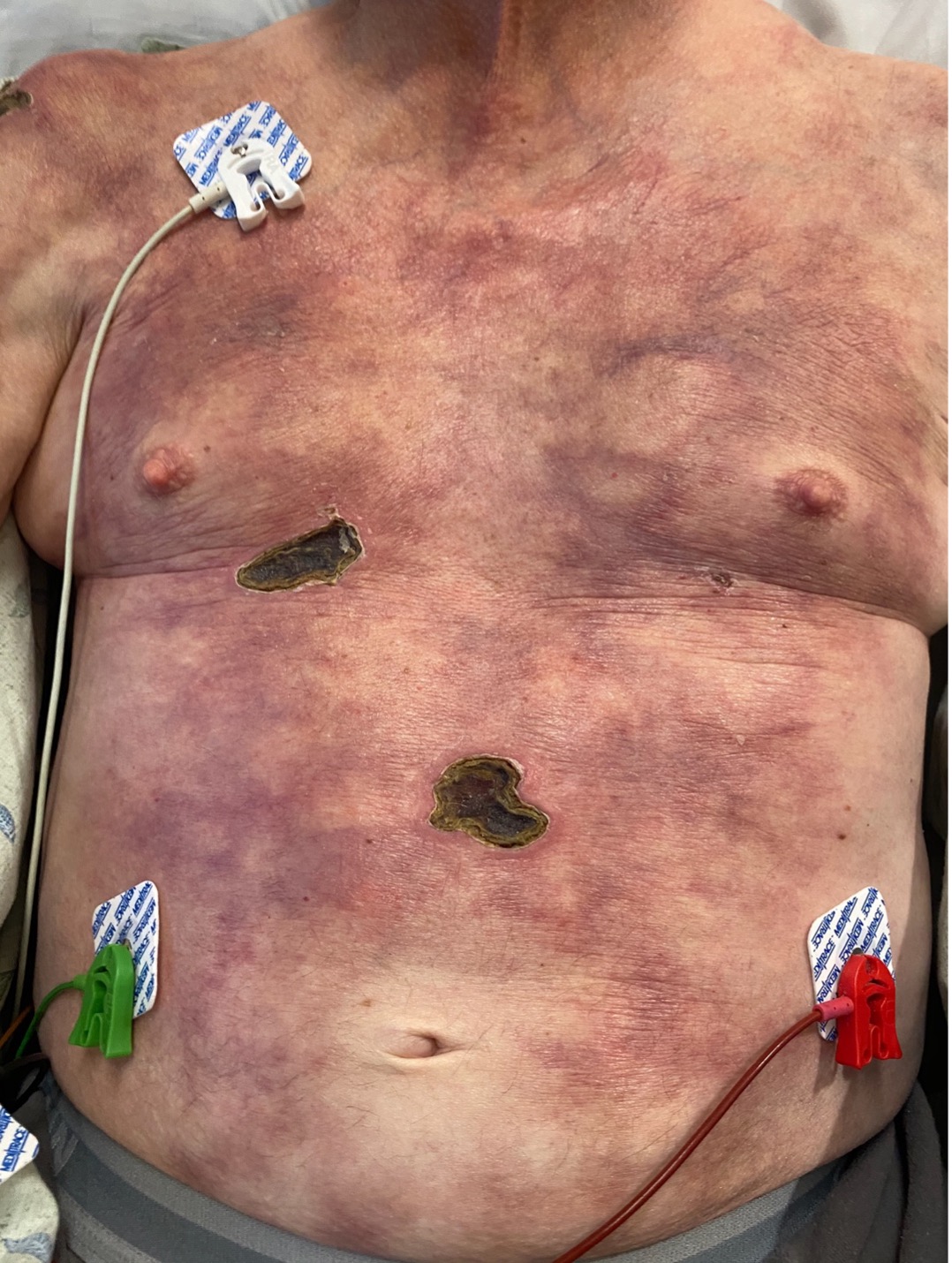
Figure 2. The patient’s initial clinical presentation of woody indurated fibrosis with calcific changes and retiform purpura of trunk and focal ulcerations with necrosis.
Diagnostic testing. Laboratory values, cultures, and skin biopsies were collected. The patient was cryoglobulin-positive (type not specified) and antinuclear antibody–positive (with negative titer). Serum protein electrophoresis demonstrated elevated free kappa and lambda light chains. Urine protein electrophoresis showed elevated gamma globulin M spike. The patient had negative immunofixation. Hypercoagulability, autoimmune, and nutritional deficiency work-up was otherwise negative. Calcium-phosphorus product was within normal limits. Scalp tissue culture grew pseudomonas aeruginosa and prevotella bivia.
Scalp and mandible biopsies demonstrated epidermal ulceration with dermal ischemia and brisk acute and chronic inflammation. Due to underlying RA and MGUS and detectable cryoglobulinemia, the patient's condition was diagnosed as thrombotic vasculopathy. Truncal biopsy demonstrated pannicular vascular calcification with thrombi and extravascular pannicular calcium deposits, diagnostic for calciphylaxis (Figure 3).
Figure 3. Pauci-inflammatory changes with extra-vascular calcifications within the panniculus.
Differential diagnosis. Given our patient’s retiform purpura, the clinical pathology was consistent with a vaso-occlusive process. The differential diagnosis of such pathology is broad, including but not limited to; frank vaso-occlusion from thrombotic disorders or intravascular protein deposition (hypercoaguable states, thrombotic thrombocytopenic purpura, cryoglobulins/cryofibrinogens); vessel wall pathology as is seen in autoimmune vasculitides (ANCA-mediated vasculitides, mixed cryoglobulinemia, and septic vasculitis); intravascular lymphoma (frank occlusion); embolic phenomenon (Libmann-Sacks type endocarditis, cholesterol emboli, or septic emboli). All differential diagnoses were ultimately ruled out by the laboratory values and biopsy results.
Treatment and management. The patient was started on empiric intravenous antibiotics (vancomycin, cefepime, and metronidazole). To substantially increase the dose bioavailability of a steroid without increasing his risk of mental health-related adverse effects, his home oral prednisone of 15 mg was transitioned to intravenous methylprednisolone 60 mg daily. He was treated for both vaso-occlusive pathologies. Rituximab was initiated for cryoglobulinemia (two 1 g doses, 2 weeks apart). For calciphylaxis, he was started on sodium thiosulfate infusions (25 g three times weekly). Additionally, hyperbaric therapy was initiated three times weekly for a total of nine treatments. Leflunomide was held on admission given initial uncertainty of active infection while he underwent acute work-up. The patient initially demonstrated both a rapid and positive response to all interventions. After 5 weeks of hospitalization, the patient was discharged and his home leflunomide was resumed to continue his baseline RA therapies.
Outcome and follow-up. His improvement plateaued post-discharge so pentoxifylline 400 mg three times daily and mycophenolate mofetil (MMF) 1 gram twice daily were added to the treatment regimen. Ultimately, the patient demonstrated significant clinical improvement in his skin wounds within 6 weeks of starting pentoxifylline and MMF, with continual improvement thereafter (Figure 4).
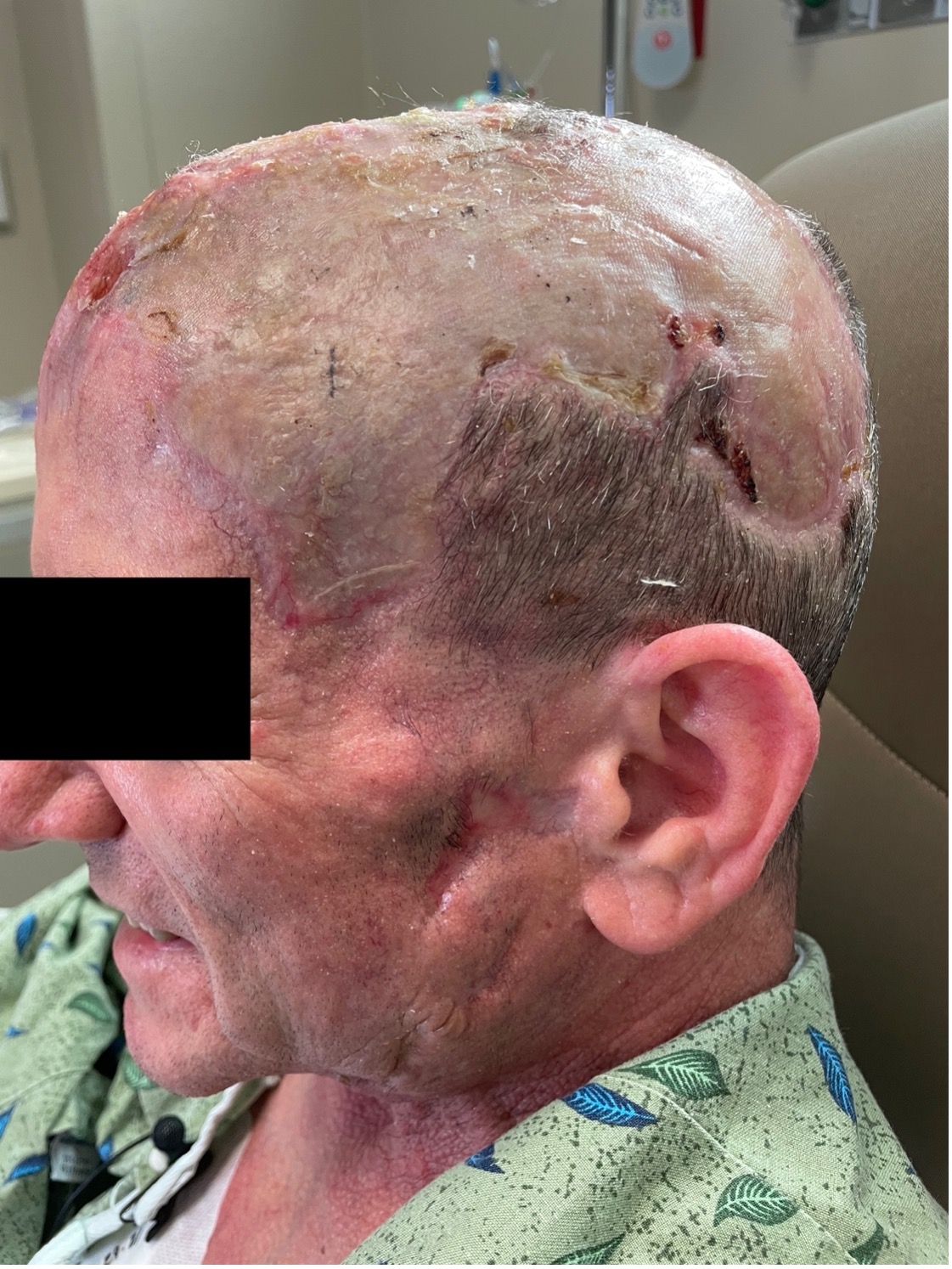
Figure 4. The patient’s clinical improvement, showing recovery of cutaneous tissue structures after therapeutic interventions for vaso-occlusive processes.
Discussion. This is a novel case of the acute coexistence of two vaso-occlusive processes, cryoglobulinemia and calciphylaxis, arising secondary to RA, a systemic inflammatory condition that can lead to severe cutaneous morbidity.1
Cryoglobulinemia is well-described in patients with RA, and is most often type II mixed cryoglobulinemia presenting as vasculitis.1 In our patient, however, type I monoclonal cryoglobulinemia with micro-thrombi induced vasculopathy remained a possibility secondary to MGUS.1 Calciphylaxis in a patient who is nonuremic is rare, albeit of higher risk in those with RA.2 Calciphylaxis causes widespread calcification and narrowing of the microvasculature resulting in cutaneous ischemia.2,3 In our patient, the combined intra- and extravascular pathology of each disease caused hypoperfusion of the skin, leading to fibrosis, necrosis, and eschar formation.
There is a wide array of treatment options for cryoglobulinemia and calciphylaxis,1,2 but we elected treatment targets that concomitantly and aggressively managed the patient’s RA while also targeting the production of cryoglobulins, reducing metastatic calcification, and reducing and reversing the process of fibrosis.
He was initially started on intravenous methylprednisolone, rituximab, and sodium thiosulfate. After one week of intravenous methylprednisolone, he became cryoglobulin-negative. We chose to use rituximab for its targeted effect on plasma globulin production.4 To reduce metastatic calcification, we added sodium thiosulfate to the patient’s treatment regimen during hospitalization.3 Previous studies have reported successful use in calciphylaxis.5-7 It is hypothesized that sodium thiosulfate functions as both a vasodilator and antioxidant, in addition to being a calcium chelator. Typical management is 25 g administered during the final hour of dialysis 3 times weekly for approximately three months. Typical responses are seen within 1 month, and pain alleviation may be appreciated in as little as 2 weeks.5-9
After discharge, when the patient reached a treatment plateau, MMF and pentoxifylline were added. MMF was added for its impact in reducing B-cell function (for cryoglobulinemia) and its effect upon TGF-beta (allowing for reduction in collagen production and fibrosis).10 Pentoxifylline was added to the treatment regimen following discharge to decrease blood viscosity and assist in fibrinolysis.11 Altogether, his treatment interventions increased his perfusion and significantly improved both fibrosis and necrosis as evidenced by his healing.
This unique case of contemporaneous calciphylaxis and cryoglobulinemia in a patient with RA demonstrates the need to be conscientious in the assessment of an individual with multiple risk factors for systemic disease consequences. It is important to note that multiple synergistic pathologies may arise concurrently, and understanding the pathophysiology of these disorders allows for targeted therapies to be implemented.
AFFILIATIONS:
1Department of Dermatology, Emory University, Atlanta, GA
2Banner University Medical Center, Phoenix, AZ
3Medical Dermatology Specialists, Phoenix, AZ
CITATION:
Koblinski JE, Porter L, Ackerman L. A constellation of contemporaneous comorbid etiologies of vasculopathy in a patient with rheumatoid arthritis. Consultant. 2023;63(9):e6. doi:10.25270/con.2023.08.000010.
Received October 9, 2022. Accepted April 12, 2023. Published online August 17, 2023.
DISCLOSURES:
The authors report no relevant financial relationships.
ACKNOWLEDGEMENTS:
None.
CORRESPONDENCE:
Jenna E. Koblinski, MD, Department of Dermatology, Emory University, 1525 Clifton Road NE, Atlanta, GA 30322 (jennakoblinski@gmail.com)
1. Firestein GS, Budd RC, Gabriel SE, McInnes IB, O'Dell JR, Koretzky G. Firestein & Kelley's Textbook of Rheumatology. 11th ed. Elsevier; 2020.
2. Dominguez ARMD, Goldman SEBA. Nonuremic calciphylaxis in a patient with rheumatoid arthritis and osteoporosis treated with teriparatide. J Am Acad of Dermatol. 2014;70(2):e41-e42. doi:1016/j.jaad.2013.10.013
3. Weenig R. Pathogenesis of calciphylaxis: Hans Selye to nuclear factor κ-B. J Am Acad of Dermatol. 2008;58(3):458-471. doi:10.1016/j.jaad.2007.12.006
4. Cacoub P, Delluc A, Saadoun D, Landau DA, Sene D. Anti-CD20 monoclonal antibody (rituximab) treatment for cryoglobulinemic vasculitis: where do we stand? Ann Rheum Dis. 2008;67(3):283-287. Doi:10.1136/ard.2006.065565
5. Hayden MR, Goldsmith DJA. Sodium thiosulfate: new hope for the treatment of calciphylaxis. Semin Dial. 2010;23(3):258-262. doi:10.1111/j.1525-139X.2010.00738.x
6. Zitt E, König M, Vychytil A, et al. Use of sodium thiosulphate in a multi-interventional setting for the treatment of calciphylaxis in dialysis patients. Nephrol Dial Transplant. 2013;28(5):1232-1240. doi:10.1093/ndt/gfs548
7. Bolognia J, Schaffer JV, Cerroni L. Dermatology. 4th ed. Elsevier; 2017.
8. Raymond CB, Wazny LD. Sodium thiosulfate, bisphosphonates, and cinacalcet for calciphylaxis. Am J Health Syst Pharm. 2008;65(15):1419-1429. doi:10.2146/ajhp070546.
9. Rick J, Rrapi R, Chand S, et al. Calciphylaxis: Treatment and outlook—CME part II. J Am Acad of Dermatol. 2022;86(5):985-992. doi:10.1016/j.jaad.2021.10.063
10. Broen JCA, van Laar JM. Mycophenolate mofetil, azathioprine and tacrolimus: mechanisms in rheumatology. Nature Rev Rheum. 2020;16(3):167-178. doi:10.1038/s41584-020-0374-8
11. Annamaraju PB, K. Pentoxifylline. StatPearls. Updated September 19, 2022. Accessed July 10, 2023. https://www.ncbi.nlm.nih.gov/books/NBK559096/.


