An Atlas of Lumps and Bumps, Part 32: Linear Epidermal Nevus
Linear Epidermal Nevus
Linear epidermal nevus (LEN), also known as keratinocytic epidermal nevus or linear verrucous epidermal nevus, is a hamartomatous growth of the skin composed primarily of keratinocytes.1
The lesion is usually present at birth, with an estimated prevalence of 1:1000 live births.2,3 The lesion grows slowly during childhood, but it usually does not extend any further by adolescence. While most LEN are present at birth, it may also present during the first year of life, 1,4-7 or it may not be recognized until either later in childhood or during adulthood.2,6 There is no sex predilection associated with LEN.1,4,5 Although most cases occur sporadically, some instances of LEN may occur in association with a variety of developmental abnormalities.5 Familial cases have also been reported.5
The nevus appears to represent populations of ectodermal cells displaying somatic mosaicism that follows Blaschko lines. Activating mutations in fibroblast growth factor receptor 3 (FGFR3) gene and in the PIK3CA and HRAS oncogenes have been identified in some epidermal nevi.8,9 Histological findings include epidermal hyperplasia with hyperkeratosis, acanthosis with elongation of the rete ridges, and papillomatosis.10
Typically, LEN presents as a linear plaque consisting of well-circumscribed, confluent or discrete, pebbly, skin-colored, brown or yellow, closely set or coalescing, noninflammatory papules (Figure 1).1,4

Figure 1. LEN presents as a linear plaque consisting of well-circumscribed, confluent or discrete, pebbly, skin-colored, brown or yellow, closely set or coalescing, noninflammatory papules.
The nevus may have a white and macerated appearance at birth and later as a subtle, linear thin plaque consisting of closely set or coalescing, skin-colored or brown papules.1,9 The lesion tends to become hyperpigmented, thicker, and verrucous over time, particularly around the time of puberty (Figure 2).1,4,10 Rarely, it remains hypopigmented.1

Figure 2. The lesion tends to become hyperpigmented, thicker, and verrucous over time, particularly around the time of puberty.
Sites of predilection include the trunk, neck, and extremities (Figure 3).1,9 LEN tends to follow the lines of Blaschko but can occur anywhere on the skin or oral mucosa.1,2,5,10-12 Typically, the lesions are single and unilateral (nevus unius lateris), although rarely, multiple unilateral or bilateral lesions may occur.1,4,12 Extensive bilateral lesions are referred to as ichthyosis hystrix.1,10
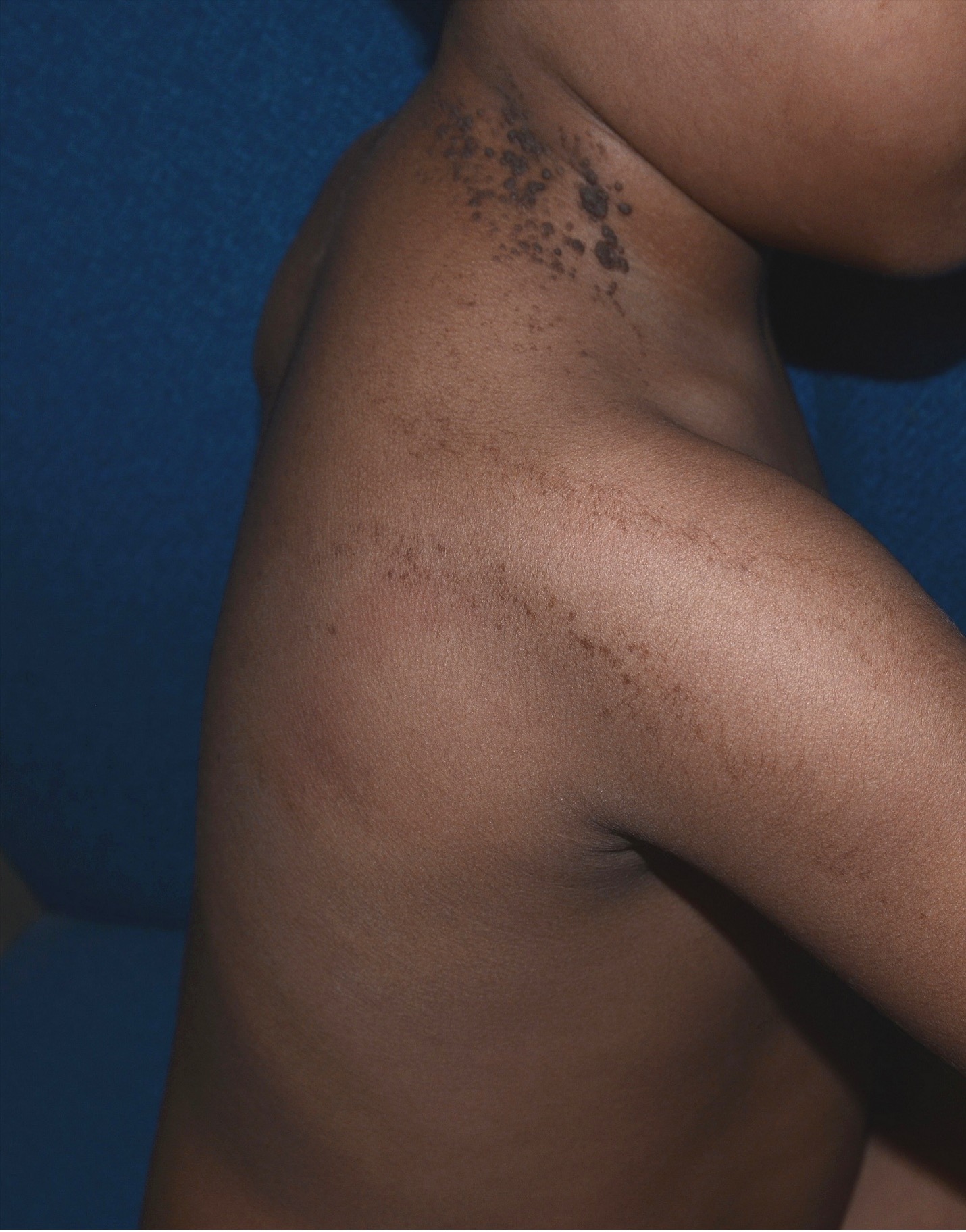
Figure 3. Sites of predilection include the trunk, neck, and extremities.
Although LEN is usually asymptomatic,1,6 scaling and pruritus are common in the inflammatory variant–inflammatory linear verrucous epidermal nevus, which is characterized by erythematous and hyperkeratotic papules often coalescing into plaques. This is generally first noted on a limb in early childhood.6
When LEN occurs in conjunction with other systemic manifestations (eg, neurological, ocular, musculoskeletal, renal, and cardiovascular), the term epidermal nevus syndrome is used.1,13 Syndromes associated with LEN include type 2 (segmental) Cowden syndrome, Proteus syndrome, FGFR3 syndrome, cutaneous skeletal hypophosphatemia syndrome, and congenital hemidysplasia with ichthyosiform nevus and limb defects (CHILD) syndrome.1,8,13
The diagnosis is mainly clinical, based on the finding of a linear verrucous plaque consisting of well circumscribed, discrete or confluent, pebbly, skin-colored, brown or yellow, closely set or coalescing papules along Blaschko lines. It may be misdiagnosed and mistreated as verruca vulgaris. A skin biopsy may be considered if the diagnosis is in doubt.
LEN is cosmetically unsightly and may adversely affect quality of life if in a highly visible area such as the face. Although LEN has no malignant potential per se, there are rare reports of the development of basal cell carcinoma, keratoacanthoma, squamous cell carcinoma, Bowen disease, eccrine poroma, and eccrine porocarcinoma in some of these lesions.1,3,14-16
The prognosis is good overall as the lesions tend to regress or become less noticeable at approximately 40 years of age and older.1,14
AFFILIATIONS:
1Clinical Professor of Pediatrics, the University of Calgary, Calgary, Alberta, Canada
2Pediatric Consultant, the Alberta Children’s Hospital, Calgary, Alberta, Canada
3Dermatologist, Medical Director and Founder, the Toronto Dermatology Centre, Toronto, Ontario, Canada
4Associate Clinical Professor of Pediatrics, Dermatology and Skin Sciences, the University of British Columbia, Vancouver, British Columbia, Canada.
5Pediatric Dermatologist, the Pediatric Institute, Kuala Lumpur General Hospital, Kuala Lumpur, Malaysia
CITATION:
Leung AKC, Barankin B, Lam JM, Leong KF. An atlas of lumps and bumps, part 32: linear epidermal nevus. Consultant. 2023;63(10):e8. doi:10.25270/con.2023.09.000007.
CORRESPONDENCE:
Alexander K. C. Leung, MD, #200, 233 16th Ave NW, Calgary, AB T2M 0H5, Canada (aleung@ucalgary.ca)
EDITOR’S NOTE:
This article is part of a series describing and differentiating dermatologic lumps and bumps. To access previously published articles in the series, visit: https://www.consultant360.com/resource-center/atlas-lumps-and-bumps.
1. Leung AKC, Barankin B. What is this asymptomatic linear eruption behind a girl’s right ear? Linear epidermal nevus. Consultant for Pediatricians. 2016;15:117-121.
2. Alonso-Castro L, Boixeda P, Reig I, de Daniel-Rodríguez C, Fleta-Asín B, Jaén-Olasolo P. Carbon dioxide laser treatment of epidermal nevi: response and long-term follow-up. Actas Dermosifiliogr. 2012;103(10):910-918. doi:10.1016/j.adengl.2012.10.001.
3. Mordovtseva VV. Multifocal basal cell carcinoma arising within a linear epidermal nevus. Indian Dermatol Online J. 2015;6(1):37-38. doi:10.4103/2229-5178.148936.
4. Brandling-Bennett HA, Morel KD. Epidermal nevi. Pediatr Clin North Am. 2010;57(5):1177-1198. doi:10.1016/j.pcl.2010.07.004.
5. Callahan AB, Jakobiec FA, Zakka FR, Fay A. Isolated unilateral linear epidermal nevus of the upper eyelid. Ophthal Plast Reconstr Surg. 2012;28(6):e135-e138. doi:10.1097/IOP.0b013e318248e66e.
6. Wright TS. Epidermal nevus and epidermal nevus syndrome. In: Post TW, ed. UpToDate. Waltham, MA. Accessed on January 26, 2021.https://medilib.ir/uptodate/show/13728.
7. Haberland-Carrodeguas C, Allen CM, Lovas JGL, Hicks J, Flaitz CM, Carlos R, et al. Review of linear epidermal nevus with oral mucosal involvement - series of five new cases. Oral Dis. 2008;14:131-137. doi:10.1111/j.1601-0825.2006.01355.x.
8. Hafner C, van Oers JM, Vogt T, Landthaler M, Stoehr R, Blaszyk H, et al. Mosaicism of activating FGFR3 mutations in human skin causes epidermal nevi. J Clin Invest. 2006;116(8):2201-2207. doi:10.1172/JCI28163.
9. Hafner C, Lopez-Knowles E, Luis NM, Toll A, Baselga E, Fernández-Casado A, Hernández S, et al. Oncogenic P1K3CA mutations occur in epidermal nevi and seborrheic keratoses with a characteristic mutation pattern. Proc Natl Acad Sci USA. 2007;104(33):13450-13454. doi: 10.1073/pnas.0705218104.
10. Adams D, Athalye L, Schwimer C, Bender B. A profound case of linear epidermal nevus in a patient with epidermal nevus syndrome. J Dermatol Case Rep. 2011;5(2):30-33. doi:10.3315/jdcr.2011.1069.
11. Santos MD, Duarte AS, Carvalho GM, Guimaraes AC, Zappelini CEM, Rio ACC, et al. Linear epidermal nevus of the oral cavity: a rare diagnosis. Case Rep Med. 2012;2012:206836. doi:10.1155/2012/206836.
12. Tesi D, Ficarra G. Oral linear epidermal nevus: a review of the literature and report of two new cases. Head Neck Pathol. 2010;4:139-143. doi:10.1007/s12105-010-0165-7.
13. Maly C, Olmo H, Stokes S, Cole H. Linear epidermal nevus: A case report with oral and facial manifestations. J Oral Maxillofac Surg. 2016;74(10):2000-2006. doi: 10.1016/j.joms.2016.04.004.
14. Jeon J, Kim JH, Baek YS, Kim A, Seo SH, Oh CH. Eccrine poroma and eccrine porocarcinoma in linear epidermal nevus. Am J Dermatopathol. 2014;36(5):430-432. doi:10.1097/DAD.0000000000000012.
15. Litaiem N, Toumi A, Zeglaoui F. Keratoacanthoma arising within a linear epidermal nevus. Indian J Dermatol Venereol Leprol. 2020;86(5):531-532. doi:10.4103/ijdvl.IJDVL_842_18.
16. Masood Q, Narayan D. Squamous cell carcinoma in a linear epidermal nevus. J Plast Reconstr Aesthet Surg. 2009;62:693-694. doi:10.1016/j.bjps.2007.11.075.


