Peer Reviewed
Enhancing Annual Physical Examinations: Patient Perceptions of Integrating Grip Strength Testing and Its Impact on Exercise Habits
ABSTRACT
Introduction. Grip strength is a well-established marker of overall health, functional status, and mortality risk, yet its role in routine ambulatory care remains unclear. This study evaluated the feasibility of integrating grip strength testing into annual physical examinations in an ambulatory care setting, with a focus on patient perceptions and self-reported changes in exercise habits.
Methods. A retrospective chart review identified 223 patients aged 18-75 who completed a general medical examination with documented grip strength in an academic ambulatory care setting. Patients were invited to complete an anonymous electronic survey assessing comfort with grip strength testing, understanding of results, satisfaction with the assessment, and perceived impact on exercise habits.
Results: Out of 223 surveys, 40 were returned (18% response rate). Among respondents, 74% of patients reported being completely comfortable taking a grip strength test and 71% had a complete understanding of the information after the test was completed. Overall satisfaction with the assessment was high, with 55% reporting being completely satisfied with grip strength testing and approximately half (52%) reported an increase in exercise resulting from the grip strength measurement.
Conclusions. Introducing grip strength testing in the primary care setting was well accepted by patients, and a slight majority of respondents reported an increase in exercise habits. Despite the limitations of our study, including the low response rate and self-reported data, grip strength assessment may serve as a practical educational tool in primary care, though additional strategies and further studies are warranted to better define its clinical utility.
Reduced grip strength is associated with sarcopenia, muscle wasting, joint dysfunction, or compromised tendon integrity, and is associated with frailty, functional decline, and increased mortality.4 Meta-analyses and large cohort studies have shown that reduced grip strength is strongly linked to all-cause mortality, with even after adjusting for traditional risk factors such as age, sex, and comorbidities.
As an indicator of musculoskeletal health, grip strength provides clinically meaningful insight into upper body strength and function, which are critical for maintaining mobility and independence, especially in adults 65 years of age or older.2,8 Additionally, studies have shown that greater grip strength is associated with a lower risk of cardiovascular diseases, reduced mortality, and a decreased incidence of chronic conditions such as diabetes and arthritis.1,2,5,6,7 These associations are likely mediated through vascular function, metabolic health and muscle strength.
Despite its clinical significance, the utilization of grip strength assessment in ambulatory care has been limited.9 Most prior studies have examined grip strength as a predictor of morbidity and mortality, with limited focus on its integration into routine ambulatory care.10 The aim of this study is to evaluate the integration of handgrip testing into routine general medical examinations in an ambulatory setting, focusing on patient’s perceptions, understanding and the influence of grip assessment on exercise habits. By assessing these factors, the study seeks to explore the feasibility and potential clinical value of incorporating grip strength measurement into everyday health care practices.
Methods. This cross-sectional study combined a retrospective chart review and prospective survey of patients aged 18 to 75 who completed a general medical examination (GME) at an academic ambulatory care practice between June 2023 and December 2023. A total of 223 patients with documented grip strength measurements were included in the chart review.
Grip strength testing was performed using a calibrated handheld dynamometer during the general medical examination for all consenting patients. The test was conducted with participants seated upright with their feet flat on the floor, and their hips and knees flexed at approximately 90º. The tested arm was positioned with the elbow flexed at 90º, the forearm held perpendicular to the upper arm, and the wrist in neutral position. Each participant completed 2 maximal grip strength trials with both the dominant and non- dominant hands. For each trial, the dynamometer was squeezed with maximum effort for approximately 3 to 5 seconds. A rest period of 30 to 60 seconds was provided between trials to minimize muscular fatigue (Figure 1). The test was completed in approximately 3 minutes.
After completing grip strength assessments, patients were provided with their results interpreted using established normative data stratified by age and sex, in addition to brief counseling on the relevance of grip strength to overall health and longevity, along with guidance on exercises to improve muscle strength on the test day.
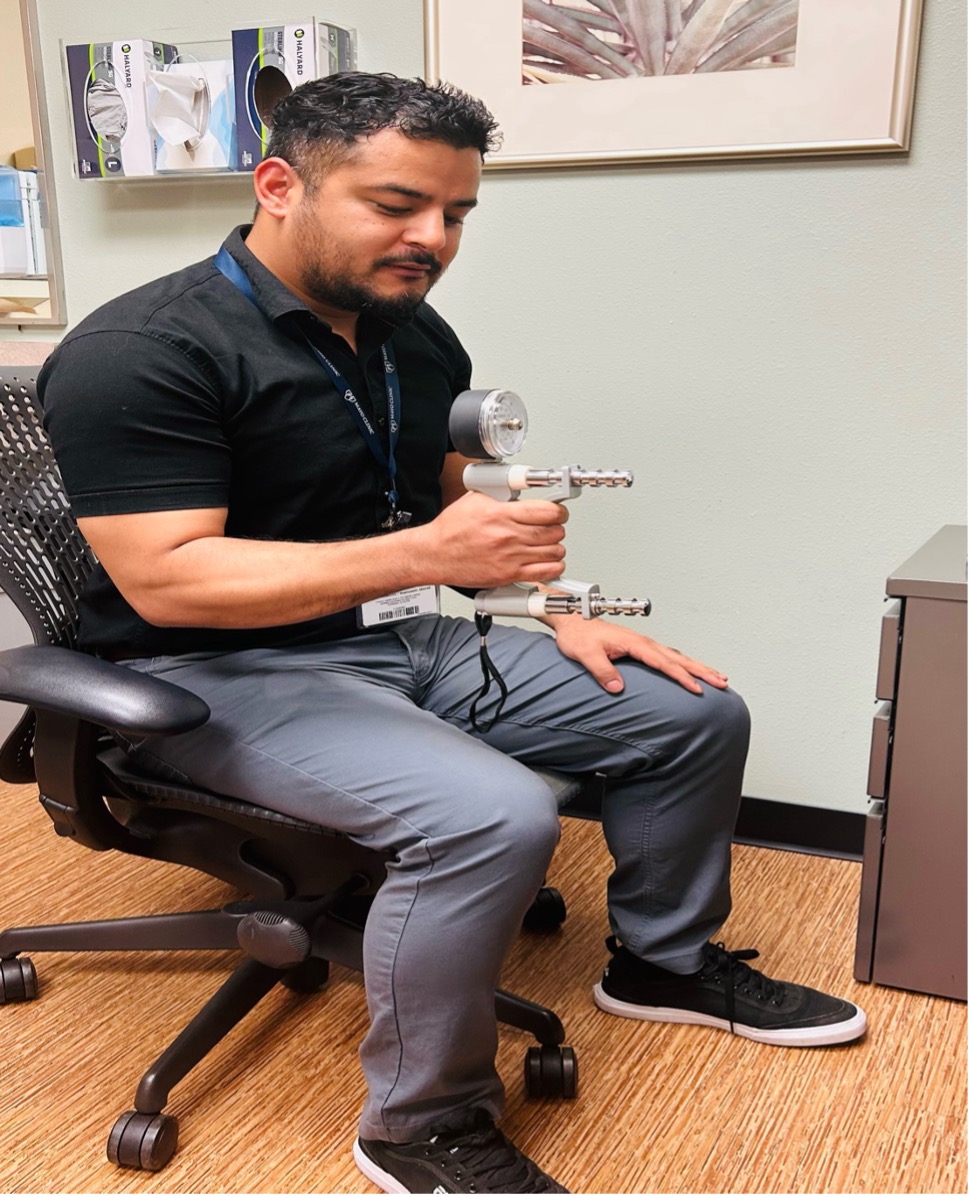
Figure 1. Physician demonstrating how to use a calibrated handheld dynamometer during the general medical examination. (The subject in the figure is the corresponding author, Sandip Raj Pradhan, MBBS, who gave Consultant permission to show his face.)
Patients identified through the chart review were invited to participate in the study via a recruitment message sent through the electronic patient portal. The survey included Likert-scale questions developed by authors, non-validated with Grade 7 readability assessing perceptions of grip strength testing and self-reported exercise habits. Exercise habits were assessed via self-reported comparison to prior activity levels, without standardized documentation of exercise type or duration. Participants were sent reminders every 2 weeks for a total of 3 times to complete the survey. Descriptive statistics were used to analyze the survey responses and clinical data. The study was reviewed and approved by the Institutional Review Board of the affiliated tertiary academic medical center.
Results
A total of 40 surveys out of 223 were returned, yielding a response rate of 18%. Most respondents reported a clear understanding of the grip strength measurement (Figure 2) and its relevance to evaluating physical health and functional capacity. Specifically, 70% indicated complete understanding of the information provided, while the remaining respondents reported partial understanding. The explanation provided was widely regarded as clear and informative, contributing to a positive perception of the procedure.
Comfort during the measurement was also extensively reported (Figure 3), with 73% of respondents reporting complete comfort during the assessment and no respondents reporting discomfort.
The perceived usefulness of the results varied among participants (Figure 4). While many participants found feedback on the results helpful in understanding their physical condition, others felt it offered limited actionable insight.
Overall satisfaction with the grip strength assessment was high (Figure 5), with 63% of respondents reporting complete satisfaction and the remainder reporting moderate satisfaction.
Self-reported changes in exercise behavior following grip strength testing were mixed (Figure 6). Approximately half of respondents (52%) reported an increase in exercise activity after the assessment, whereas 48% reported no change in their exercise habits.
Discussion. This study evaluated the integration of grip strength testing into annual physical examinations in an ambulatory care setting, focusing on patients’ perceptions and potential changes in exercise behavior. Although grip strength is recognized as an indicator of general health, morbidity, and mortality, its use in regular primary care is still not widespread. The findings of this survey suggest that grip strength testing is a feasible, well-accepted, and easily incorporated into routine workflows, but its influence on exercise behavior is mixed.
Most patients reported feeling completely comfortable during grip strength testing, with no patients indicating discomfort. These findings support grip strength testing as a non-invasive and well-tolerated procedure and is suitable for integration into standard clinical workflows in the primary care setting. Furthermore, most respondents reported complete understanding of the grip strength results and their implications for health, particularly muscle function and overall vitality, with 95% finding the information helpful. Patient satisfaction was high, with 96% reporting at least moderate satisfaction.
The primary outcome—whether grip strength testing influenced exercise habits—revealed mixed results. For example, 52% of patients reported increased exercise engagement following the test, while 48% of respondents reported no change, highlighting variability in behavioral response. This discrepancy suggests that while grip strength testing may serve as an educational tool, additional interventions (e.g., structured counseling or goal setting) may be needed to drive significant behavioral change.
From an implementation perspective, grip strength testing required minimal resources. During the grip strength testing, 2 physicians shared a single dynamometer, which can cost between $300 to $600. Each session took approximately 3 minutes to complete. As this was a pilot investigation, no reimbursement was sought. However, Medicare reimburses grip strength testing (CPT 97750) only when it is medically necessary, such as when conducted as part of therapy evaluation, functional capacity assessment, or management of musculoskeletal or neuromuscular conditions. Proper billing requires clear clinical justification and separate documentation of the specific test performed and its results. This code is not intended for routine assessments, including range of motion or manual muscle testing, as these are typically included in the standard evaluation and are not separately billable.11 Given its simplicity, affordability, and predictive value for health outcomes, clinicians considering incorporation of grip strength testing should view it as a low-cost adjunct rather than a reimbursable screening tool.
Prior studies have shown that lower grip strength independently predicted all-cause mortality, and that physically active individuals with low to moderate grip strength experienced the greatest mortality reduction.12 One potential implication is integrating grip strength testing with existing patient education initiatives, such as personalized exercise counseling based on test results. While this study cannot draw definitive conclusions due to its pilot nature, it can serve as a foundation for future research exploring whether combining grip strength assessment with structured interventions improved long-term adherence to exercise programs.
Several limitations must be acknowledged. The study had a low response rate (18%), which raises concerns about selection bias and limits the generalizability of the findings. Respondents may have been more engaged with their health or more receptive to the concept of grip strength testing than non-respondents. There was also a reliance on self-reported survey data, which introduces potential recall bias and social desirability bias. Future studies should consider objective measures of physical activity, such as wearable fitness trackers, to provide more accurate assessments of behavioral change. The study also lacked a control group, making it difficult to isolate the effect of grip strength testing on exercise habits. Randomized controlled trials comparing patients who receive grip strength testing with those who do not would help clarify its true impact. Finally, the follow-up period was short, capturing only immediate or short-term behavior changes. Future research should assess whether grip strength testing leads to sustained increases in physical activity over months or years.
Conclusion. Grip strength testing during annual physical examinations was well received by patients in an ambulatory setting. While a little more than half of survey respondents reported increased exercise habits, a substantial proportion reported no behavioral change, indicating the need for complementary interventions to maximize its effectiveness as a motivational tool. Given its feasibility and potential benefits, further studies should explore strategies to enhance its clinical utility in promoting long-term health outcomes.
AUTHORS:
Michael Underhill, DO1, Sandip Raj Pradhan, MBBS1, Jesse Bracamonte, DO1, Michael Bryan, MD1, Nick Allen, MD1, Gretchen Anderson, APRN, FNP, MSN1
AFFILIATIONS:
Mayo Clinic, Department of Family Medicine, Glendale, AZ 85308
CITATION:
Underhill M, Pradhan SR, Bracamonte J, Bryan M, Allen N, Anderson G. Enhancing annual physical examinations: patient perceptions of integrating grip strength testing and its impact on exercise habits. Consultant. Published online January 26, 2026. DOI: 10.25270/con.2026.01.000009
Received May 27,2025. Accepted September4, 2025
DISCLOSURES:
The author(s) report no conflicts of interest and no funding sources related to this work.
ACKNOWLEDGMENTS:
None.
CORRESPONDENCE:
Sandip Raj Pradhan, MBBS, Mayo Clinic, 20199 N 75TH Ave, Glendale, AZ 85308 (Email: Pradhan.sandip@mayo.edu)
- García-Hermoso A, Cavero-Redondo I, Ramírez-Vélez R, et al. Muscular strength as a predictor of all-cause mortality in an apparently healthy population: a systematic review and meta-analysis of data from approximately 2 million men and women. Arch Phys Med Rehabil. 2018;99(10):2100-2113.e5. doi:10.1016/j.apmr.2018.01.008
- Syddall HE, Westbury LD, Dodds R, Dennison E, Cooper C, Aihie Sayer A. Mortality in the Hertfordshire Ageing Study: association with level and loss of hand grip strength in later life. Age Ageing. 2017;46(3):407-412. doi:10.1093/ageing/afw222
- Wang YC, Bohannon RW, Li X, Sindhu B, Kapellusch J. Hand-grip strength: normative reference values and equations for individuals 18 to 85 years of age residing in the United States. J Orthop Sports Phys Ther. 2018;48(9):685-693. doi:10.2519/jospt.2018.7851
- Kothari R, Johny MP, Mistry D, Irfana M, Yogesh S, Vemparala SS. Grip to health: unlocking the clinical potential of isometric hand grip strength—a narrative review. J Pharm Bioallied Sci. 2024;16(suppl 4):S3102-S3104. doi:10.4103/jpbs.jpbs_1040_24
- Celis-Morales CA, Welsh P, Lyall DM, et al. Associations of grip strength with cardiovascular, respiratory, and cancer outcomes and all-cause mortality: prospective cohort study of half a million UK Biobank participants. BMJ. 2018;361:k1651. doi:10.1136/bmj.k1651
- Mainous AG III, Tanner RJ, Anton SD, Jo A. Grip strength as a marker of hypertension and diabetes in healthy-weight adults. Am J Prev Med. 2015;49(6):850-858. doi:10.1016/j.amepre.2015.05.025
- Lee J, Lee MG. Associations of handgrip strength with prevalence of rheumatoid arthritis and diabetes mellitus in older adults. J Obes Metab Syndr. 2019;28(4):271-277. doi:10.7570/jomes.2019.28.4.271
- Bohannon RW. Grip strength: an indispensable biomarker for older adults. Clin Interv Aging. 2019;14:1681-1691. doi:10.2147/CIA.S194543
- Reeve TE IV, Craven TE, Goldman MP, et al. Outpatient grip strength measurement predicts survival, perioperative adverse events, and nonhome discharge among patients with vascular disease. J Vasc Surg. 2021;73(1):250-257. doi:10.1016/j.jvs.2020.03.060
- Vaishya R, Misra A, Vaish A, Ursino N, D’Ambrosi R. Hand grip strength as a proposed new vital sign of health: a narrative review of evidence. J Health Popul Nutr. 2024;43(1):7. doi:10.1186/s41043-024-00500-y
- Centers for Medicare & Medicaid Services. Billing and coding: outpatient physical and occupational therapy services (A56566). Medicare Coverage Database. Updated January 1, 2025. Accessed August 11, 2025. https://www.cms.gov/medicare-coverage-database/view/article.aspx?articleId=56566
- Polo-López A, Calatayud J, Palau P, et al. Joint associations of handgrip strength and physical activity with incident cardiovascular disease and overall mortality in the UK Biobank. Clin Nutr. 2024;43(12):218-224. doi:10.1016/j.clnu.2024.10.022
©2026 HMP Global. All Rights Reserved.
Any views and opinions expressed are those of the author(s) and/or participants and do not necessarily reflect the views, policy, or position of Consultant360 or HMP Global, their employees, and affiliates.


