Peer Reviewed
Vasculitis Presenting as Calf Pain With Muscle-Limited Involvement
AUTHORS:
Aasia Ferdous, DO
Adena Health System, Chillicothe, Ohio
Kenneth Van Dyke, DO
Adena Health System, Chillicothe, Ohio
CITATION:
Ferdous A, Van Dyke K. Vasculitis presenting as calf pain with muscle-limited involvement. Consultant. 2020;60(2):62-63. doi:10.25270/con.2020.02.00009
A 37-year-old woman with no significant medical history was referred to the rheumatology clinic by her primary care provider for unexplained right calf pain and elevated inflammatory markers. She described the pain as sharp and stabbing, which worsened with activity. She also reported intermittent swelling of the lower part of the leg, which also was tender to the touch.
At her earlier primary care visit, findings of a review of systems were negative for any constitutional, cardiopulmonary, gastrointestinal, or neurological complaints. Vital signs were normal. Physical examination revealed a shiny and taut appearance to the right lower extremity with exquisite tenderness to palpation to the musculature of the calf.
Findings of the initial workup by the primary care provider were negative for deep vein thrombosis on Doppler ultrasonography and negative for arterial insufficiency on ankle-brachial pressure index. Electromyography findings were negative for myopathic or neuropathic abnormalities. Magnetic resonance imaging (MRI) scans of the lower extremity showed hyperintensity on fat-suppressed T1-weighted images of the musculature with associated subcutaneous nodularity (Figures 1 and 2).
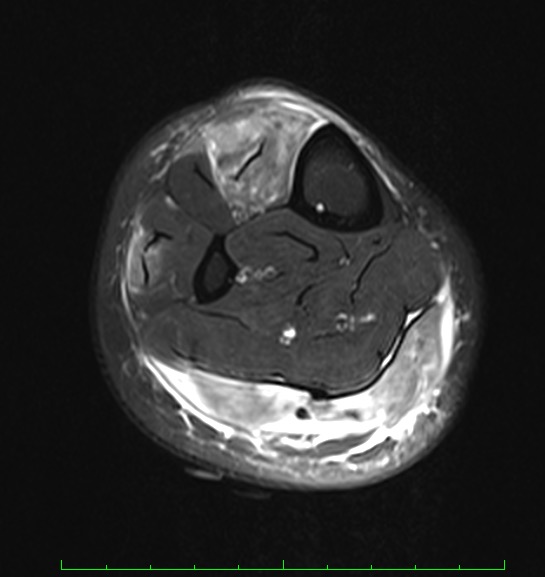
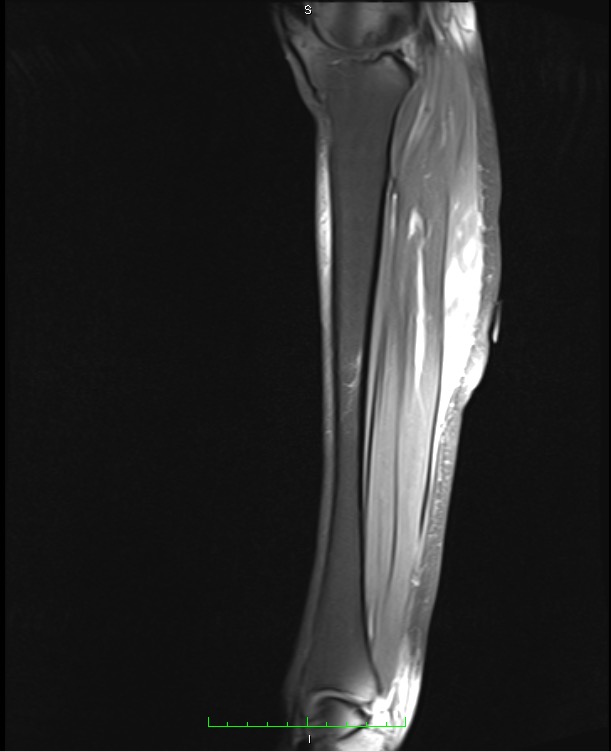
Figures 1 and 2. MRI scans of the right lower extremity showed nodularities and nonspecific inflammation within the leg muscles, particularly the tibialis anterior and gastrocnemius muscles.
At that time, malignancy was a concern, so the patient was referred to an orthopedic oncologist, who performed a biopsy of the subcutaneous nodule. The biopsy showed nonspecific fibrotic changes, and the results were nondiagnostic. She was then referred to the rheumatology clinic for further evaluation.
The results of an autoimmune panel—including antinuclear antibodies, anti-Sjogren syndrome-related antibodies, rheumatoid factor, anticyclic citrullinated peptide, anti-Jo-1 antibodies, antineutrophil cytoplasmic antibodies, lupus anticoagulant, anti-β2 glycoprotein antibodies, anticardiolipin antibodies, and cryoglobulin levels—were negative. Infectious serology test results—including hepatitis B viral serum antigen and core antibody, hepatitis C virus antibody, HIV 1/2 p24 antigen, Treponema pallidum antibodies, and interferon-γ release assay for tuberculosis—also were negative.
Results of other laboratory studies, including a complete blood cell count, a comprehensive metabolic panel, urinalysis, serum protein electrophoresis, and measurements of thyrotropin, creatinine kinase, aldolase, and lactate dehydrogenase, were all unremarkable. Chest radiography and transthoracic echocardiography findings were also unremarkable. The only significant serologic finding was an elevated erythrocyte sedimentation rate of 92 mm/h and an elevated C-reactive protein level of 10 mg/L.
After the initial workup and nondiagnostic initial biopsy of the subcutaneous nodule, we then felt it was important to obtain a biopsy specimen of the muscle tissue that appeared abnormal on the MRI, since the first biopsy had little muscle tissue and also had not been performed with a muscle biopsy protocol. The resulting muscle biopsy from the right gastrocnemius muscle revealed multifocal muscle-limited medium-vessel vasculitis (Figure 3).
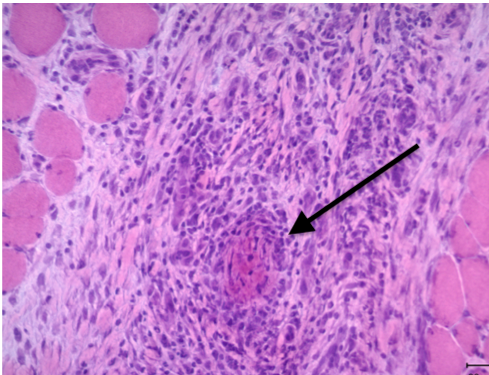
Figure 3. Pathology slide from the right gastrocnemius muscle biopsy using hematoxylin-eosin staining showing a vessel with complete obliteration of its lumen (arrow). Increased endomysial capillaries/neovascularization is appreciated in the area surrounding the vessel. Notable inflammation and perimysial connective tissue are appreciated. (Image courtesy of Zarife Sahenk, MD, Department of Pathology, Children’s Hospital, Ohio State University, Columbus, Ohio.)
Discussion. Vasculitides are a group of inflammatory conditions in which damage to the vessel wall can lead to life-threatening tissue and organ dysfunction. The diagnosis of vasculitis can be difficult because the presenting symptoms are often very generalized and nonspecific, and the diagnosis often requires biopsy of the affected organ.1-3 Diagnosis can be further complicated by the fact that several medical conditions mimic vasculitis.3
The affected organs often can give clues to the type of vasculitis.1 Our patient’s case was unique in that her only symptom was lower extremity pain and swelling, without systemic organ system involvement. Further investigation was considered with either computed tomography angiography of the abdomen or arteriography of the mesenteric or renal system, but given the lack of symptoms such as fever, weight loss, abdominal pain or angina, hypertension, renal insufficiency, hematuria, or proteinuria, we did not feel there was any indication. Furthermore, our patient desired a very conservative approach, and was even hesitant to get a muscle biopsy at first. Additionally, she required 2 tissue biopsies before a diagnosis could be reached. Vasculitis localized to a specific muscle without other systemic manifestations is rare, and very few cases have been reported in the literature.2
Our patient had a delay of diagnosis for months, as did many of the patients in published cases.2 After a muscle biopsy revealed vasculitis, she was promptly placed on prednisone, 60 mg, for 1 month, which led to a prompt resolution of her symptoms. She was then tapered to 5 mg by month 6 and was continued at this dose for the next 6 months. At nearly 1 year after initiation of treatment, our patient’s vasculitis relapsed, and she again developed calf pain; the corticosteroid-sparing agent methotrexate was added to her regimen.
While many cases of muscle-limited vasculitis respond to corticosteroids alone, cases have been reported in which patients had relapse or systemic symptoms requiring corticosteroid-sparing agents such as azathioprine, cyclophosphamide, or methotrexate.2,4
As illustrated by this case, the diagnosis of muscle-limited vasculitis can be extremely challenging. MRI can aid in the diagnosis by showing increased signal intensity in the affected calf muscles and subcutaneous tissue on fat-suppressed images, which indicates edema from an inflammatory process.4-7 Moreover, MRI findings give clues as to which area of the muscle must be biopsied and also can guide response to therapy. All of the reviewed cases of muscle-limited vasculitis involve the lower extremities. Most often, the gastrocnemius and soleus muscles are involved.2,4-7 MRI comparison images in one case report have shown decreased signal intensity after treatment.4
Although a rare diagnosis, muscle-limited vasculitis should always be included in the differential diagnosis of unexplained lower extremity pain. Because of the nature and complexity of its presentation, clinical vigilance and awareness of muscle-limited vasculitis is critical in order to provide a prompt diagnosis and to begin treatment as soon as possible.
References:
- Blaes F. Diagnosis and therapeutic options for peripheral vasculitic neuropathy. Ther Adv Musculoskelet Dis. 2015;7(2):45-55.
- Khellaf M, Hamidou M, Pagnoux C, et al. Vasculitis restricted to the lower limbs: a clinical and histopathological study. Ann Rheum Dis. 2006;66(4):554-556.
- Suresh E. Diagnostic approach to patients with suspected vasculitis. Postgrad Med J. 2006;82(970):483-488.
- Yang SN, Cho NS, Choi HS, Choi SJ, Yoon ES, Kim DH. Muscular polyarteritis nodosa. J Clin Rheumatol. 2012;18(5):249-252.
- Ahmed S, Kitchen J, Hamilton S, Brett F, Kane D. A case of polyarteritis nodosa limited to the right calf muscles, fascia, and skin: a case report. J Med Case Rep. 2011;5:450.
- Aoshima M, Fukuchi K, Tatsuno K, Ito T, Tokura Y. Ectopic adipose tissue with vasculitis in the calf muscle explaining systemic symptoms in leg-limited cutaneous polyarteritis nodosa. Acta Derm Venereol. 2016;96(1):142-143.
- Nakamura T, Tomoda K, Yamamura Y, Tsukano M, Honda I, Iyama K. Polyarteritis nodosa limited to calf muscles: a case report and review of the literature. Clin Rheumatol. 2003;22(2):149-153.


