Jason Ong, PhD, MBBS, on the Burden of STIs Among PrEP Users
A high burden of sexually transmitted infections (STIs) exists among people initiating pre-exposure prophylaxis (PrEP) and persistent users of PrEP for HIV, according to findings from a recent study.1 These findings highlight the opportunities for active integration of services for STIs and PrEP for HIV.
To dive deeper into these findings, Infectious Diseases Consultant reached out to lead author Jason J. Ong, PhD, MBBS, who is a sexual health physician and researcher in the Department of Clinical Research at the London School of Hygiene and Tropical Medicine in the United Kingdom.
Here are his answers to our burning questions.
ID CON: What is the burden of STIs among individuals using emtricitabine and tenofovir disoproxil fumarate for the prevention of HIV infection?
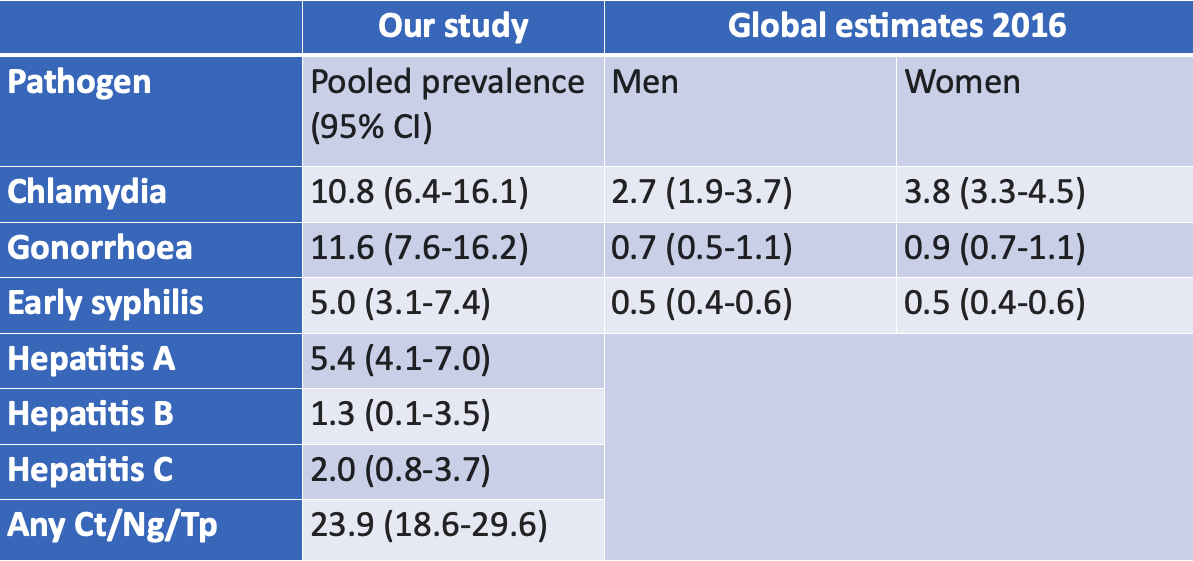
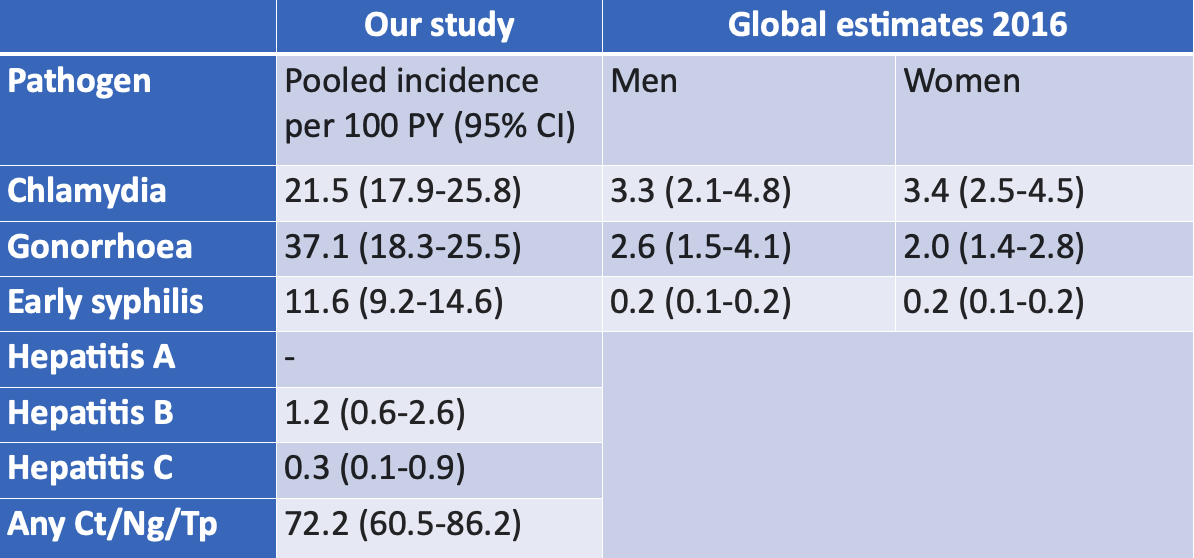
Jason Ong: Our study reviewed 88 studies from 26 countries. We show that for studies reporting a composite outcome of chlamydia, gonorrhea, and/or syphilis, the pooled prevalence for individuals starting PrEP was 24% (95% CI: 19-30), and the pooled incidence for those continuing to take PrEP was 72 per 100 person-years (95% CI: 61-86). This is very high compared with the World Health Organization’s recent estimates.2 The tables below show the comparisons between PrEP users (our study) and non-PrEP users (Global estimates 2016).This high prevalence and incidence of STIs reflects the high-risk populations that are now accessing PrEP.
ID CON: Among your findings was a high burden of STIs among individuals initiating PrEP and persistent users of PrEP for the prevention of HIV infection. How might these findings impact clinical practice and how PrEP is prescribed?
JO: Even in resource-rich settings (but especially in resource-limited settings), PrEP programs might focus only on protecting participants from HIV. This study highlights the opportunities to also strengthen comprehensive sexual health services to individuals using PrEP. We now have an unprecedented opportunity to regularly engage (every 3 months) with people whom we have previously struggled to engage with in our health systems. Comprehensive sexual health services should not only diagnose and treat STIs, but also offer vaccinations (HPV, Hepatitis A/B), mental health support, substance use support, reproductive health, and so on.
ID CON: What is the key take-home message from your study?
JO: We demonstrate high prevalence and incidence of STIs in PrEP programs globally. We should not miss the opportunity to harness the growing interest in providing PrEP, a game-changing HIV prevention tool. PrEP programs can be a gateway for empowering comprehensive sexual health services globally.
References:
- Ong JJ, Baggaley RC, Wi TE, et al. Global epidemiologic characteristics of sexually transmitted infections among individuals using preexposure prophylaxis for the prevention of HIV infection: a systematic review and meta-analysis. JAMA Netw Open. 2019;2(12):e1917134. https://doi.org/10.1001/jamanetworkopen.2019.17134.
- Rowley J, Vander Hoorn S, Korenromp E, et al. Chlamydia, gonorrhoea, trichomoniasis and syphilis: global prevalence and incidence estimates, 2016. Bull World Health Organ. 2019;97(8):548-56 https://dx.doi.org/10.2471%2FBLT.18.228486.


