Right-Sided Infective Endocarditis
 For a week, a 39-year-old woman with a history of intravenous heroin use had generalized pain, fever, chills, and a nonproductive cough. She rated the pain at 10 on a scale of 1 to 10; it was sharp, constant, and unrelieved by heroin. She also reported dyspnea at rest, pleuritic chest pain, and a 15-lb weight loss over the past month. She had no significant medical history or drug allergies, smoked a half pack of cigarettes per day, and denied alcohol use.
For a week, a 39-year-old woman with a history of intravenous heroin use had generalized pain, fever, chills, and a nonproductive cough. She rated the pain at 10 on a scale of 1 to 10; it was sharp, constant, and unrelieved by heroin. She also reported dyspnea at rest, pleuritic chest pain, and a 15-lb weight loss over the past month. She had no significant medical history or drug allergies, smoked a half pack of cigarettes per day, and denied alcohol use.
Temperature was 38.3°C (100.9°F); heart rate, 134 beats per minute; blood pressure, 165/112 mm Hg; respiration rate, 22 breaths per minute; and oxygen saturation, 89% while breathing room air. A grade 2/6 systolic murmur was loudest over the left fourth intercostal space. Other findings included jugular venous distention with a striking cardiovascular wave, a right ventricular lift, and a pulsatile liver. Rales and decreased breath sounds were noted bilaterally. The abdomen was soft and diffusely tender; bowel sounds were normal. There was no pitting edema of the lower extremities.
 The white blood cell count was 28,600/µL, with 13% bands. Abnormal laboratory values included sodium, 124 mEq/L; bicarbonate, 19 mEq/L; and creatinine, 4.1 mg/dL. Arterial blood gas levels on room air were pH, 7.35; PCO2, 39 mm Hg; PO2, 72 mm Hg; and bicarbonate, 22 mm Hg, which showed the patient had a mixed high anion gap metabolic acidosis and respiratory acidosis. Western blot analysis was negative for HIV; cardiac enzyme levels were normal. Three sets of blood cultures were positive for methicillin-sensitive Staphylococcus aureus (MSSA).
The white blood cell count was 28,600/µL, with 13% bands. Abnormal laboratory values included sodium, 124 mEq/L; bicarbonate, 19 mEq/L; and creatinine, 4.1 mg/dL. Arterial blood gas levels on room air were pH, 7.35; PCO2, 39 mm Hg; PO2, 72 mm Hg; and bicarbonate, 22 mm Hg, which showed the patient had a mixed high anion gap metabolic acidosis and respiratory acidosis. Western blot analysis was negative for HIV; cardiac enzyme levels were normal. Three sets of blood cultures were positive for methicillin-sensitive Staphylococcus aureus (MSSA).
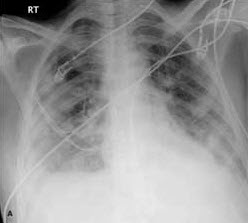
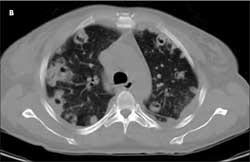
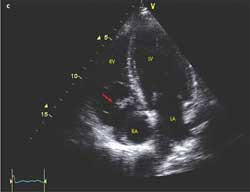
Christopher C. Brodkin, MD, of Chicago reports that a chest radiograph showed diffuse patchy infiltrates suggestive of septic emboli resulting from right-sided infective endocarditis (A). A chest CT scan revealed multiple cavitary septic emboli causing multilobar pneumonias (B). An echocardiogram demonstrated a large vegetation, a 1 3 1-cm, mobile echo density attached to the atrial surface of the tricuspid valve (red arrow), and severe tricuspid regurgitation with an estimated pulmonary artery pressure of 60 to 65 mm Hg (C).
 The incidence of right-sided infective endocarditis is 1% to 5% per year among injection drug users. Parenteral cocaine users are at highest risk. Up to 20% of hospitalizations for right-sided infective endocarditis involve injection drug users. The disease is responsible for 5% to 10% of all deaths among injection drug users.1
The incidence of right-sided infective endocarditis is 1% to 5% per year among injection drug users. Parenteral cocaine users are at highest risk. Up to 20% of hospitalizations for right-sided infective endocarditis involve injection drug users. The disease is responsible for 5% to 10% of all deaths among injection drug users.1
The tricuspid valve is affected in 70% of patients with right-sided endocarditis, followed by mitral and aortic valves in 20% to 30%. However, only 10% to 30% of affected injection drug users have underlying cardiac pathology.
Patients often present with septic pulmonary emboli. Symptoms include cough, fever, pleuritic chest pain, hemoptysis, and dyspnea. The tricuspid murmur is soft and frequently inaudible. Other findings may include splinter hemorrhages, Osler nodes, and Roth spots.
The initial diagnostic test is transthoracic echocardiography (TTE). Transesophageal echocardiography (TEE) is recommended when TTE results are nondiagnostic; TEE can detect tricuspid valve vegetations with 80% sensitivity.2 Based on the Duke diagnostic criteria, a positive echocardiogram in conjunction with 3 positive blood cultures establishes the diagnosis of infective endocarditis.1
In 60% to 70% of patients, blood cultures grow S aureus; the organisms are from skin flora and are usually methicillin-sensitive. Pseudomonas aeruginosa is often cultured in persons who abuse combination pentazocine and tripelennamine (T's and Blues).3
1. Durack DT, Lukes AS, Bright DK, et al. New criteria for diagnosis of infective endocarditis: utilization of specific echocardiographic findings. Duke Endocarditis Service. Am J Med. 1994;96:200-209.
2. Crawford MH, Durack DT. Clinical presentation of infective endocarditis. Cardiol Clin. 2003;21: 159-166.
3. Miro JM, del Rio A, Mestres CA. Infective endocarditis and cardiac surgery in intravenous drug abusers and HIV-1 infected patients. Cardiol Clin. 2003;21;167-184.
FOR MORE INFORMATION:
- Baddour LM, Wilson WR, Bayer AS, et al. Infective endocarditis: diagnosis, antimicrobial therapy and management of complications: a statement for health care professionals. Circulation. 2005;111: e394-e434.


