Persistent Skin Disorders: Can You Identify the Cause?
Photo Quiz
Self-Test Your Diagnostic Acumen

Case 1:
Erythematous Papules
A 28-year-old man presents with pruritic lesions on his forearms of 4 to 6 weeks’ duration. Over-the-counter hydrocortisone 1% cream has provided some relief.
Several erythematous papules and excoriations are noted on the forearms. No other areas are affected. The patient has a history of anxiety with obsessive-compulsive features and is undergoing psychotherapy.
What is your clinical impression?
(Answer on next page.)
Photo Quiz–Answer
Case 1: Neurotic excoriation

This patient’s lesions are neurotic excoriations, a classic example of a psychodermatosis. This relatively common phenomenon results from habitual picking of the skin with the fingernails. Although no data on prevalence are available, this condition seems to be more common in women and usually occurs during the third to fifth decades of life. Patients may relate the onset to a specific event or to an ongoing stress; for example, in this patient, the stressor was a death in the family. They often deny picking or scratching and state that the pruritus disappears after the epidermis has been picked away.
Examination reveals excoriation with or without crust. Scarring and a linear pattern are common. The term “prurigo nodularis” is used to describe an eruption of nodular lesions. A careful workup for serious causes of pruritus is sometimes necessary unless the presentation is obvious.
Psychiatric counseling is helpful. Because this patient was already undergoing psychotherapy, he was not referred for further counseling. However, short-term anxiolytic therapy will be considered if no improvement is noted at follow-up. ■
(Case and photograph courtesy of Robert Levine, DO.)
 Case 2:
Case 2:
Asymptomatic Ulcers
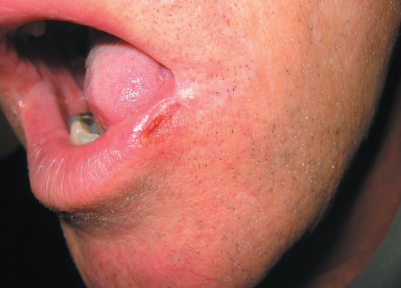
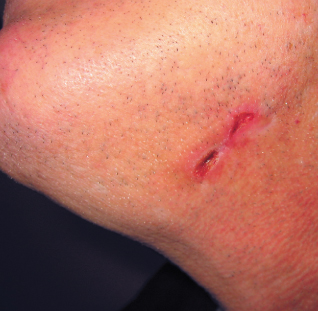
A 34-year-old man is concerned about 2 nonhealing, asymptomatic ulcers—one on his lower lip and one on his anterior neck—that have persisted for 2 years despite treatment with various corticosteroid creams and topical antibiotics.
Results of a previous swab for culture and biopsy showed no clear pathology.
What do you suspect is responsible for these lesions?
(Answer on next page)
Photo Quiz–Answer
Case 2: Dermatitis artefecta

During a thorough history taking, the patient revealed that he thought there were “slivers” stuck in his lip and neck and that the ulcers would heal only if he continued to remove them. He believed that splinters remained in his skin after an injury he had sustained when he ran into a tree 2 years earlier. The clinical diagnosis of dermatitis artefacta, or factitious dermatitis, was made.
The lesions of dermatitis artefacta are produced by the patient’s own actions. The disorder is commonly a result or manifestation of a psychological problem.
 The lesions are difficult to recognize and do not conform to those of well-established dermatoses. Frequently, they are bizarrely shaped and clearly demarcated; they can be produced by the hand or a variety of objects. Affected areas (eg, face, hands, arms, or legs) are usually readily accessible to the patient’s hands; the midback is spared. The patient often denies causing
The lesions are difficult to recognize and do not conform to those of well-established dermatoses. Frequently, they are bizarrely shaped and clearly demarcated; they can be produced by the hand or a variety of objects. Affected areas (eg, face, hands, arms, or legs) are usually readily accessible to the patient’s hands; the midback is spared. The patient often denies causing
the problem.
Treatment is difficult and frustrating. Avoid direct confrontation. An empathic, nonjudgmental approach is encouraged, with symptomatic management as needed. Psychiatric referral is usually refused. Management with a low-dose antipsychotic is often helpful; present this option carefully to the patient. Consider referral to a dermatologist to rule out a true pathology.
For this patient, an atypical antipsychotic agent was prescribed. He was told the medication was being used to numb the nerve endings that cause his symptoms. ■
(Case and photographs courtesy of Benjamin Barankin, MD.)


