Lead Toxicity in a Young Boy
 A 3-year-old Hispanic boy with a history of pica presented for a well-child checkup. He had missed numerous checkups, and his immunizations were delayed. His development was appropriate for age.
A 3-year-old Hispanic boy with a history of pica presented for a well-child checkup. He had missed numerous checkups, and his immunizations were delayed. His development was appropriate for age.
The child was fed regular milk at age 7 months. He lived in a 100-year-old house with leaded glass windows and some chipping paint. He started eating paint chips from the wall at around age 9 months. His history was negative for abdominal pain, vomiting, constipation, irritability, headache, and lethargy. The only pertinent physical findings were multiple dental carries.
Results of a blood workup from a capillary sample showed a lead level of 70 μg/dL. A radiograph of the extremities showed “lead lines” (Figure 1). The patient was hospitalized for treatment of lead poisoning. After consultation with the hematologist and department of health, the decision was made to start chelation therapy with oral succimer and hold off on calcium disodium ethylenediaminetetraacetic acid (EDTA), pending a venous sample. The venous level was slightly lower than the capillary level, and oral treatment alone was continued. Further workup revealed severe iron deficiency anemia, and treatment with ferrous sulfate was started after completion of chelation therapy.
The family moved out of the home. However, the child required a total of 5 hospitalizations for chelation therapy over 6 months because of continued high levels of lead.
LEAD POISONING: AN OVERVIEW
Lead poisoning is one of the most important chronic environmental illnesses in children younger than 6 years. Children between 12 and 36 months are particularly susceptible to lead exposure and its toxic effects.1 Although the prevalence of lead toxicity has decreased because of preschool screening programs, increased public awareness, and the removal of lead from gasoline and paint products, it has remained high among inner-city children who live in housing that was built before the 1970s.2 Common sources of exposure include chips or dust from lead-based paint, food or beverages in lead-soldered cans or lead-glazed pottery, water from lead-soldered plumbing, automobile emissions, and lead-using industry.1,3 Products imported into the United States are occasional sources of lead exposure.
The 2008 guidelines of the American Academy of Pediatrics (AAP) and Bright Futures recommend risk assessment at ages 6, 9, and 18 months and at 3, 4, 5, and 6 years.4 At ages 1 and 2 years, risk assessment or lead screening is recommended as appropriate or as mandated for patients with Medicaid and those who live in areas of high prevalence.
CLINICAL MANIFESTATIONS
 The early symptoms of acute lead poisoning in children are episodic and nonspecific (eg, anorexia, decreased activity, irritability, insomnia); no pathognomonic symptoms exist. Some children with severely elevated lead levels may be asymptomatic. No organ system is immune to the effects of lead poisoning, and the blood lead level at which these effects may occur may be low. Research shows that significant insult to the brain can occur at blood lead levels of less than 10 µg/dL.5 Neurological effects of lead poisoning range from developmental delay (particularly in language) to encephalopathy (at blood lead levels of 100 to 150 µg/dL). Severe neurological damage may follow lead encephalopathy.
The early symptoms of acute lead poisoning in children are episodic and nonspecific (eg, anorexia, decreased activity, irritability, insomnia); no pathognomonic symptoms exist. Some children with severely elevated lead levels may be asymptomatic. No organ system is immune to the effects of lead poisoning, and the blood lead level at which these effects may occur may be low. Research shows that significant insult to the brain can occur at blood lead levels of less than 10 µg/dL.5 Neurological effects of lead poisoning range from developmental delay (particularly in language) to encephalopathy (at blood lead levels of 100 to 150 µg/dL). Severe neurological damage may follow lead encephalopathy.
Lead poisoning can also cause hearing loss, peripheral neuropathy, and decreased nerve conduction
velocity. Lead nephropathy is a potential complication of prolonged high-level lead exposure. Lead colic, which includes sporadic vomiting, intermittent abdominal pain, and constipation, may occur with a lead level as low as 60 µg/dL.
DIAGNOSIS
Laboratory studies. The AAP defines lead poisoning as a venous blood lead level of 10 μg/dL or higher.6 Anemia secondary to lead toxicity is rare and usually mild and microcytic. Anemia in children with lead poisoning is more often caused by iron deficiency,7 as was the case in this patient. Basophilic stippling, which is characteristic of lead intoxication, is uncommon in children. Erythrocyte protoporphyrin testing may be done in select patients, although it is not used as a primary screening tool.
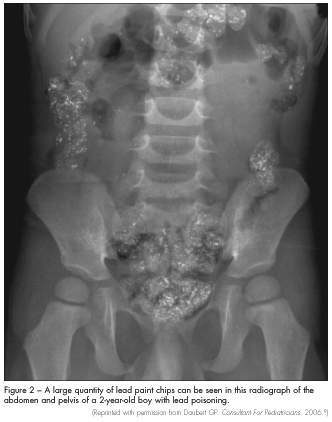
Imaging studies. Abdominal radiography may show the presence of radiopaque flakes, which is a clear indicator of pica (Figure 2). Radiographs of the long bones may show “lead lines.”2 Lead lines—which are abnormal calcium deposits, not actual lead deposition—may be detected at the distal metaphysis in children with lead levels greater than 45 µg/dL; these represent growth arrest associated with long-term lead exposure. This radiological finding is not required for diagnosis. Head CT scanning may be needed in patients who present with altered mental status to exclude cerebral edema and structural lesions.
MANAGEMENT
Treatment of lead toxicity requires prevention of further lead exposure, chelation therapy, and careful follow-up. The most important first step is to reduce the child’s lead exposure. This requires notification of the local public health department. The CDC recommends home inspection and environmental remediation for all children with blood lead levels persistently greater than 15 µg/dL and education of the family about sources of lead exposure, prevention of exposure, and ways to decrease intestinal  absorption of lead (Table).1
absorption of lead (Table).1
Chelating agents can reduce the immediate effects of lead toxicity; however, their ability to reverse the neurocognitive effects of long-term lead ingestion is limited.8 The use of chelating agents is not recommended for patients with blood lead levels of less than 45 μg/dL. According to the AAP guidelines for screening and treatment of lead toxicity, chelation therapy with oral succimer or parenteral calcium
disodium EDTA can be given to children with blood lead levels between 45 and 69 μg/dL.5 Chelation with parenteral dimercaprol and calcium disodium EDTA is the mainstay of therapy for children with severe lead toxicity (blood lead levels of 70 μg/dL or higher). Hepatic and renal function must be observed carefully during chelation therapy.
All children treated for lead poisoning need close follow-up care and monitoring of their blood lead levels. Prognosis depends on the patient’s blood lead level and symptoms at presentation. Children with lead poisoning are at risk for developmental delay and may be eligible for early intervention services.
1. Binns HJ, Campbell C, Brown MJ; Centers for Disease Control and Prevention Advisory Committee on Childhood Lead Poisoning Prevention. Interpreting and managing blood lead levels of less than 10 microg/dL in children and reducing childhood exposure to lead: recommendations of the Centers for Disease Control and Prevention Advisory Com-mittee on Childhood Lead Poisoning Prevention. Pediatrics. 2007;120:e1285-e1298.
2. Centers for Disease Control and Prevention. Children with elevated blood lead levels related to home renovation, repair, and painting activities—New York State, 2006-2007. MMWR. 2009;58:55-58.
3. Agency for Toxic Substances and Disease Registry. Case Studies in Environmental Medicine (CSEM): Lead Toxicity Cover Page. http://www.atsdr.cdc.gov/csem/lead/pbcover_page2.html. Accessed March 11, 2010.
4. American Academy of Pediatrics and Bright Futures. Recommendations for Preventive Pediatric Health Care. 2008. http://pediatrics. aappublications.org/cgi/data/120/6/1376/DC1/1. Accessed April 7, 2011.
5. Canfield RL, Henderson CR Jr, Cory-Slechta DA, et al. Intellectual impairment in children with blood lead concentrations below 10 microg per deciliter. N Engl J Med. 2003;348:1517-1526.
6. American Academy of Pediatrics Committee on Environmental Health. Lead exposure in children: prevention, detection, and management. Pediatrics. 2005;116:1036-1046.
7. Wright RO, Tsaih SW, Schwartz J, et al. Association between iron deficiency and blood lead level
in a longitudinal analysis of children followed in an urban primary care clinic. J Pediatr. 2003;142:9-14.
8. Rogan WJ, Dietrich KN, Ware JH, et al; Treatment of Lead-Exposed Children Trial Group. The effect of chelation therapy with succimer on neuropsychological development in children exposed to lead. N Engl J Med. 2001;344:1421-1426.
9. Daubert GP. Lead poisoning in a young boy. Consultant For Pediatricians. 2006;5:147-149.


