Cough, Chest Pain, and Dyspnea in a Woman With Rheumatoid Arthritis
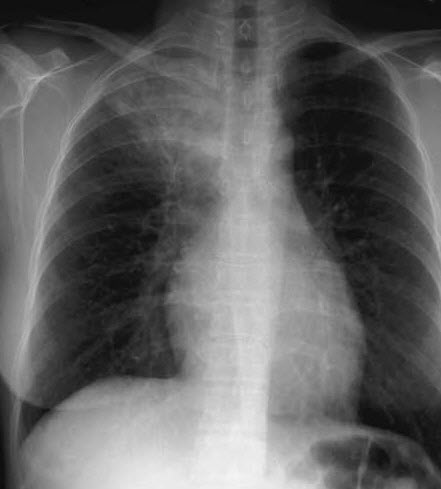 A 40-year-old Hispanic homemaker is admitted with a 3-week history of high fever, chest pain, and a dry, irritating cough.
A 40-year-old Hispanic homemaker is admitted with a 3-week history of high fever, chest pain, and a dry, irritating cough.
Her illness began insidiously with increasing right upper chest pain that is sharp, pleuritic, and rates a 6 on a pain scale of 1 to 10. The pain is associated with temperatures of up to 38.8°C (102°F) and chills, rigors, and profuse sweating that increase in the evening. Worsening dyspnea has been accompanied by a drop in effort tolerance.
The patient was seen at a local urgent care center and treated with levofloxacin for a week. A chest radiograph showed infiltrates in the right upper lobe. The symptoms worsened and the medication was switched to clarithromycin, but there was no marked improvement.
The patient has a history of rheumatoid arthritis (RA) and has been under the care of a rheumatologist. Initially, she was treated with ibuprofen, then with corticosteroids and hydroxychloroquine. During the past 12 months, she has received a weekly injection of infliximab. No tuberculin skin test was done before the initiation of infliximab therapy because the patient told the rheumatologist that results of a tuberculin skin test the year before were negative.
The patient's appetite is poor and she has lost 6 lb in the past 3 weeks. She denies hemoptysis, palpitations, ankle edema, lymphadenopathy, rash, and joint swelling. She has no history of nausea, vomiting, diarrhea, abdominal pain, jaundice, hematemesis, melena, headache, vision problems, seizures, syncope, weakness, paresthesias, urinary symptoms, or bleeding diathesis.
Both of her parents have type 2 diabetes; a younger brother has bronchial asthma. The patient smokes half a pack of cigarettes a day; she does not drink alcohol or use illicit drugs. She is sexually monogamous. She visited her grandparents in Mexico for 2 weeks a year ago.
 Examination. This thin woman appears chronically ill. Her hands show changes consistent with chronic RA, including swan-neck deformity.
Examination. This thin woman appears chronically ill. Her hands show changes consistent with chronic RA, including swan-neck deformity.
Heart rate is 122 beats per minute and regular; temperature, 38.8°C (102°F); respiration rate, 24 breaths per minute; blood pressure, 118/68 mm Hg. Her weight is 104 lb. Hydration status is good. Examination of the head and neck shows no icterus, erythema, or evidence of candidal infection. The mucosa and skin are pale; there are no rashes or tattoos. There is no palpable lymphadenopathy or ankle edema; the thyroid is not palpable. Chest movements are symmetric and equal bilaterally. The trachea is centrally located and the chest is resonant to percussion. Breath sounds are harsh in the right upper zone and coarse rales are heard. The jugular venous pressure and heart sounds are normal. The abdomen is soft and nontender with no organomegaly or fluid. Results of a neurologic examination are normal.
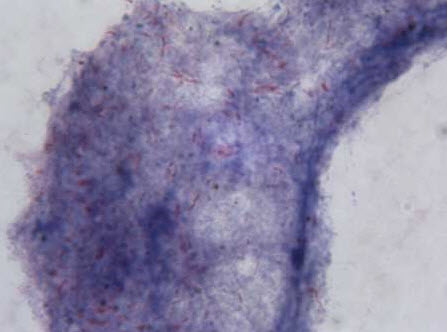
 Laboratory studies. White blood cell count, 12,800/µL, with 80% polymorphonuclear leukocytes and 20% lymphocytes. Hemoglobin level, 10.2 g/dL; platelet count, 156,000/µL. A peripheral smear shows normocytic normochromic anemia. Erythrocyte sedimentation rate, 124 mm/h. Urinalysis results are normal. Blood glucose level, 92 mg/dL; blood urea nitrogen, 12 mg/dL; creatinine, 0.8 mg/dL; serum sodium, 138 mEq/L; potassium, 4 mEq/L; chloride, 100 mEq/L. Total bilirubin, 1 mg/dL; conjugated bilirubin, 0.6 mg/dL. Total protein, 7.8 g/dL; albumin, 3.2 g/dL; alkaline phosphatase, 118 U/L; aspartate aminotransferase, 24 U/L; alanine aminotransferase, 21 U/L. Two blood cultures are negative for organisms. Serologic evaluation for Coccidioides yields negativeresults. Serum ferritin, 350 ng/mL. Serum iron, 38 µg/dL. Total iron-binding capacity, 200 µg/dL.
Laboratory studies. White blood cell count, 12,800/µL, with 80% polymorphonuclear leukocytes and 20% lymphocytes. Hemoglobin level, 10.2 g/dL; platelet count, 156,000/µL. A peripheral smear shows normocytic normochromic anemia. Erythrocyte sedimentation rate, 124 mm/h. Urinalysis results are normal. Blood glucose level, 92 mg/dL; blood urea nitrogen, 12 mg/dL; creatinine, 0.8 mg/dL; serum sodium, 138 mEq/L; potassium, 4 mEq/L; chloride, 100 mEq/L. Total bilirubin, 1 mg/dL; conjugated bilirubin, 0.6 mg/dL. Total protein, 7.8 g/dL; albumin, 3.2 g/dL; alkaline phosphatase, 118 U/L; aspartate aminotransferase, 24 U/L; alanine aminotransferase, 21 U/L. Two blood cultures are negative for organisms. Serologic evaluation for Coccidioides yields negativeresults. Serum ferritin, 350 ng/mL. Serum iron, 38 µg/dL. Total iron-binding capacity, 200 µg/dL.
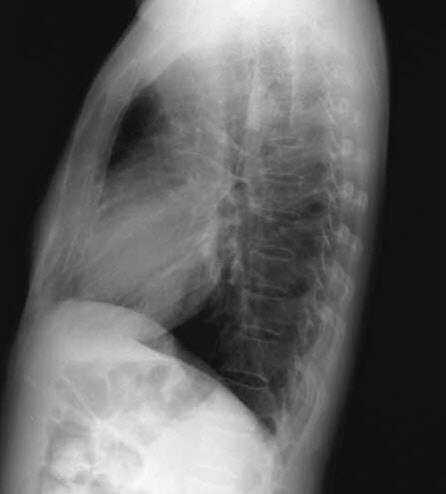
A chest radiograph and sputum evaluation for acid-fast bacteria (AFB) are ordered.
In view of the clinical picture and laboratory and radiographic findings, what is the most likely diagnosis?
A. Community-acquired pneumoniaB. Rheumatoid lung disease
C. Pulmonary coccidioidomycosis
D. Pulmonary tuberculosis
E. Idiopathic pulmonary fibrosis
OVERVIEW
The pathogenesis of rheumatoid disease progression involves high concentrations of tumor necrosis factor (TNF), the central component in the cascade of cytokines induced in RA that stimulates production of additional inflammatory mediators such as chemokines, prostaglandins, proteases, and growth factors that activate neutrophils, b cells, and endothelial cells.
The TNF inhibitors infliximab, etanercept, and adalimumab are widely used to reduce the erosive damage of RA. TNF inhibitors are usually given to patients with active, progressive RA who have not responded satisfactorily to one or more conventional disease-modifying antirheumatic drugs, such as methotrexate, sulfasalazine, hydroxychloroquine, and cyclosporine.
Although the TNF inhibitors are effective, neutralization of TNF significantly suppresses the immune response. This has led to an increased risk of such infections as tuberculosis (TB), Pneumocystis infection, and disseminated histoplasmosis.
About half a million patients have undergone TNF therapy; mycobacterial infections have been reported in about 300 of these. Most infections appear in the first 6 to 8 months of treatment.
CLINICAL MANIFESTATIONS
Extrapulmonary presentations, which have been reported in 30% to 50% of cases, include fever of unknown origin, miliary TB, TB-associated lymphadenopathy, peritonitis, enteritis, meningitis, and vertebral and bladder disease.
Pulmonary manifestations usually consist of chronic productive cough, hemoptysis, pleuritic chest pain, and dyspnea associated with constitutional symptoms such as fever, night sweats, lack of energy, and weight loss.
DIAGNOSIS AND TREATMENT
A high index of suspicion is warranted. The diagnosis is confirmed by demonstration of AFB either in biopsy material or sputum, in conjunction with sputum culture. Chest radiography or CT can be helpful.
Once the diagnosis is established, prompt and aggressive therapy is started with isoniazid, rifampin, ethambutol, and pyrazinamide. The regimen is continued for 2 months, followed by isoniazid and rifampin therapy for an additional 7 to 10 months.
GUIDELINES FOR HIGH-RISK PATIENTS
According to American Thoracic Society and CDC guidelines, patients with active RA who are being considered for TNF inhibitor therapy may be at high risk for TB and should undergo tuberculin skin testing.1 Induration of more than 5 mm is considered a positive result. Antituberculosis prophylaxis should be considered for any high-risk patient before TNF inhibitors are administered. Suggested courses of therapy are 1 month if the tuberculin skin test is positive and 3 to 4 months if the patient has active TB.1
Patients should also be evaluated for evidence of other preexisting infections. TNF inhibitors are best avoided in patients with chronic infections such as hepatitis B; concomitant illnesses such as optic neuritis, multiple sclerosis, aplastic anemia, interstitial lung disease, and systemic lupus erythematosus may be exacerbated by TNF inhibitor therapy. Live vaccination is contraindicated in patients receiving TNF inhibitors.
1. American Thoracic Society, Centers for Disease Control and Prevention. Targeted tuberculin testing and treatment of latent tuberculosis infection. Am J Respir Crit Care Med. 2000;161:221-247.
FOR MORE INFORMATION:
- Askling J, Fored CM, Brandt L, et al. Risk and case characteristics of tuberculosis in rheumatoid arthritis associated with tumor necrosis factor antagonists in Sweden. Arthritis Rheum. 2005;52:1986-1992.
- Brassard P, Kezouh A, Suissa S. Antirheumatic drugs and the risk of tuberculosis. Clinic Infect Dis. 2006;4:717-722.
- Hochberg MC, Lobwohl MG, Plevy SE, et al. The benefit/risk profile of TNF-blocking agents: findings of a consensus panel. Semin Arthritis Rheum. 2005;34: 819-836.
- Keane J, Gershon S, Wise RP, et al. Tuberculosis associated with infliximab, a tumor necrosis factor alpha-neutralizing agent. N Engl J Med. 2001;345:1098-1104.
- Kroesen S. Widmer AF, Tyndall A, Hasler P. Serious bacterial infections in patients with rheumatoid arthritis under anti-TNF-alpha therapy. Rheumatology (Oxford). 2003;42:617-621.
- Scott DL, Kingsley GH. Tumor necrosis factor inhibitors for rheumatoid arthritis. N Engl J Med. 2006;355:704-712.


