Peer Reviewed
What’s Causing This Man’s Folliculitis Barbae?
Authors:
Aunna Pourang, MD
Department of Dermatology, University of California, Davis, Sacramento, California, and Faculty Practice Group, University of California, Los Angeles, California
Simran Sandhu, BS
School of Medicine, University of California, Davis, Sacramento, California
Raja K. Sivamani, MD, MS, AP
Department of Dermatology, University of California, Davis, and Pacific Skin Institute, Sacramento, California
Citation:
Pourang A, Sandhu S, Sivamani RK. What’s causing this man’s folliculitis barbae? Consultant. 2020;60(1):19-22. doi:10.25270/con.2020.01.00006
A healthy 38-year-old man presented to a walk-in clinic for evaluation of a rash on his upper neck that his primary care physician had diagnosed as a possible skin abscess 2 days prior. The patient was concerned that the area was not improving despite his taking cephalexin and using topical mupirocin.
His symptoms had begun 4 days earlier after he had shaved the ingrown hairs in the area with an older razor while on a business trip. He did not recall any other stress, illness, or other trauma to the area. He described the area as being painful and having “come to a head,” but the lesion was otherwise asymptomatic (Figure 1). He also reported having a similar but milder rash in the same area 8 years prior after having shaved with an old razor, but he did not remember how the area was treated.
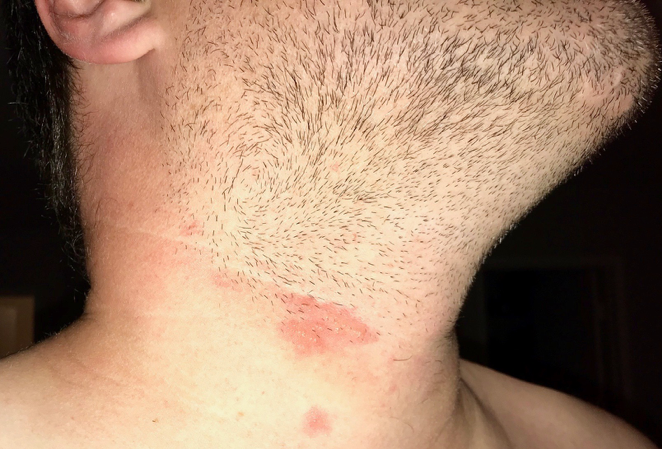
Figure 1. Initial photo taken by patient before his first office visit to his primary care provider. Vesicles with surrounding erythema were present with a satellite lesion inferiorly.
On examination, a tender, indurated, vesiculopapular rash was noted at the right inferior aspect of the neck at the beard line (Figure 2). The patient also had tender right anterior and posterior cervical lymphadenopathy.
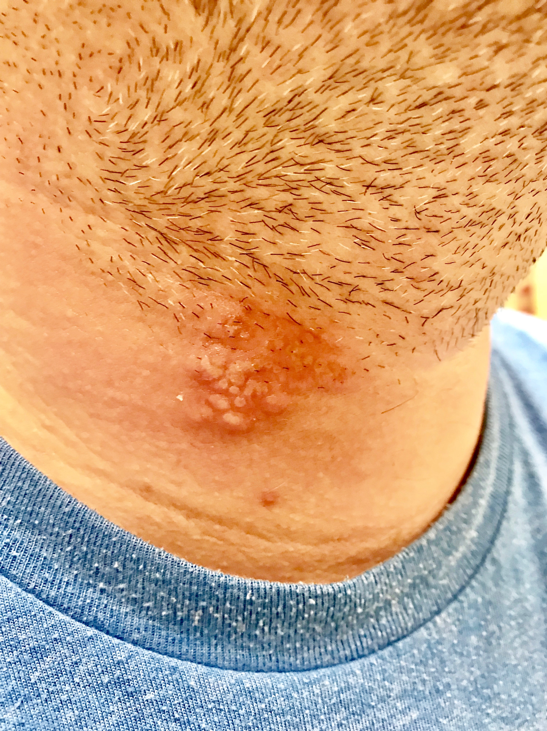
Figure 2. Photo taken at the follow-up visit at the walk-in clinic. Vesicles were more prominent, and induration was present.
Upon further questioning, the patient reported that while he had no known history of herpes infection, his wife had a history of herpes labialis, with no recent active lesions, but he had not had any recent oral contact in the affected area.
The patient was started empirically on acyclovir, 400 mg, 3 times a day for 5 days. The affected area was swabbed; polymerase chain reaction (PCR) results returned positive for herpes simplex virus (HSV), but bacterial and fungal cultures came back negative.
One week later, during telephone follow-up, the patient reported resolution of the pain and that the affected area had crusted over and was healing well (Figure 3).
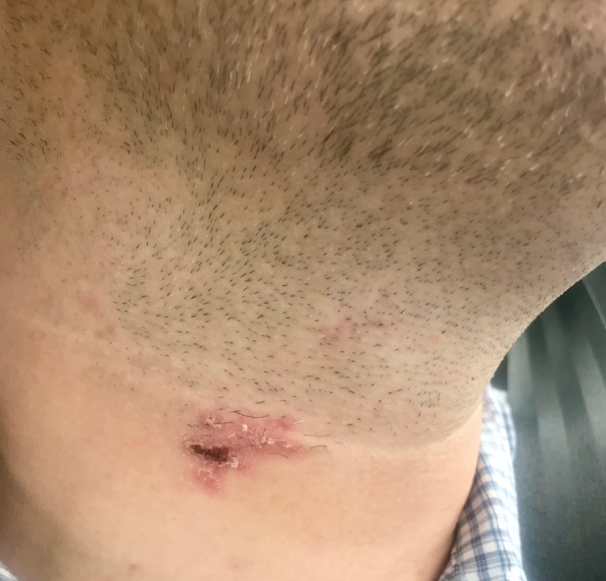
Figure 3. Resolving rash 2.5 weeks after the initial eruption. The vesicles had resolved with crusting, and resolving erythema was present.
DISCUSSION
HSV infection is common, with reports that HSV-1 affects 67% of the global population younger than 49 years.1 Infection usually occurs in areas of the oropharyngeal mucosa, as seen with herpes gingivostomatitis and herpes labialis; the virus remains latent in the trigeminal nerve and usually reactivates with illness (ie, “cold sore”), UV radiation exposure, or trauma.2,3 HSV-1 infections are typically diagnosed based on the prototypical presentation of multiple vesicular lesions residing on an inflammatory erythematous base.3
The use of such heuristics, however, can lead to diagnostic pitfalls, resulting in clinicians overlooking other less common cutaneous manifestations of HSV-1. Such presentations include herpes keratoconjunctivitis, herpetic whitlow, herpes gladiatorum, genital herpes (typically caused by HSV-2), eczema herpeticum, and herpes barbae.3
The term folliculitis barbae describes inflammation of the deep portions of the hair follicle in the beard area (Latin, barba, “beard”), leading to follicular pustules and erythematous papules.4 Etiologies of folliculitis barbae include acne vulgaris, viral infections (eg, HSV, herpes zoster virus, molluscum contagiosum), fungal infections, and bacterial infections, the latter of which—specifically Staphylococcus aureus—are the usual culprit for infectious folliculitis.4,5 As such, empiric treatment with antibiotics is usually started in suspected cases of beard infections, and alternative diagnoses such as tinea barbae and herpes barbae are not usually considered until after the initial treatment is found to be ineffective.
Pseudofolliculitis barbae, an inflammatory condition of the hair follicles of the beard that is often a result of shaving, is another cause of folliculitis to consider in the differential diagnosis of folliculitis barbae.6 Asteatosis, syphilis, Sweet syndrome, syringoma, eosinophilic folliculitis, pseudolymphoma, cutaneous lymphoma, seborrheic dermatitis, impetigo, acne rosacea, allergic contact dermatitis, and irritant contact dermatitis are other conditions to consider in individuals presenting with inflammation of the beard (Table 1).
|
Table 1. Differential Diagnosis of Inflammatory Beard Lesions |
|
Acne vulgaris |
|
Acne rosacea |
|
Bacterial folliculitis (most commonly S aureus) |
|
Impetigo |
|
Viral folliculitis (HSV, varicella zoster virus, molluscum contagiosum) |
|
Fungal folliculitis (Candida, Malassezia [Pityrosporum]) |
|
Parasitic folliculitis (Demodex folliculorum) |
|
Syphilis |
|
Pseudofolliculitis barbae |
|
Follicular occlusion |
|
Asteatosis |
|
Eczema herpeticum |
|
Syringoma |
|
Pseudolymphoma |
|
Cutaneous lymphoma |
|
Seborrheic dermatitis |
|
Contact dermatitis |
|
Eosinophilic folliculitis |
|
Sweet syndrome |
The term sycosis (Greek, sykōsis, “fig”) is also used to describe folliculitis and is synonymous with infections of the beard area. It is not to be confused with the older name sycosis barbae, which was used to describe bacterial infections of the beard.7,8
Herpes barbae is a rare presentation of HSV-1 that is infrequently reported in the literature. Because the clinical presentation is similar to that of other types of infectious folliculitis, the diagnosis may be elusive. Thus, it is imperative for clinicians to suspect HSV infection in the differential diagnosis of folliculitis barbae.
From the existing literature reports on herpes barbae, it is clear that clues in a patient’s history can aid in making the proper diagnosis. Between 1972 and 2004, 8 cases of herpetic folliculitis on the face in immunocompetent men have been reported, many of which shared similarities to the patient’s case described here (Table 2).5,7,9-12 No cases have been reported in this patient population in the English literature since 2004. The ages of the men in the reported cases ranged from 21 to 47 years. Five patients initially had been treated with antibiotics for what had been initially diagnosed as a bacterial infection before presenting for follow-up after symptoms did not improve. Six of the 8 patients reported symptoms after shaving, often noting a burning sensation while shaving over the area before the appearance of the rash. Three men had a personal history of herpes labialis without any outbreaks at the time of the presentation, and 2 had been recently exposed to a partner with an active herpes labialis infection. All 8 patients had presented similarly with a follicular or vesiculopustular rash on the face, and 5 were reported to have cervical lymphadenopathy. In most cases, symptoms lasted between 1.5 and 3 weeks and resolved with antiviral treatment, but the dose and duration varied among cases. Interestingly, the first cases reported by Izumi et al in 1972 had been diagnosed correctly initially, but given that acyclovir was not available until 1982,13 antibiotics and corticosteroids were used as a treatment without improvement of symptoms.7
|
Table 2. Cases of Immunocompetent Men With Herpes Infections of the Beard Reported From 1972-2005 |
|||||
|
Age (y) |
History of herpes labialis? |
Association with shaving? |
Initially diagnosed as bacterial infection? |
Treatment |
Reference |
|
21 |
Yes, but without recent outbreak; exposure to partner with active herpes labialis infection |
Yes |
No |
Acyclovir, 200 mg, 5 times daily for 10 days |
12 |
|
24 |
No |
Not reported |
Yes |
Famciclovir, 125 mg, 3 times daily for 1 week |
9 |
|
26 |
Yes, with recent outbreak |
Yes |
Yes |
Acyclovir not available at the time; lesions resolved on their own |
5 |
|
30 |
No, but exposure to partner with recent herpes labialis infection |
Not reported |
Yes |
Valacyclovir, 500 mg, twice daily, number of days not reported |
10 |
|
32 |
Lesion on nasolabial fold was thought to be a primary infection |
Yes |
Yes |
Intravenous acyclovir, 5 mg/kg, 3 times daily for 1 week in association with intravenous flucloxacillin to treat superficial bacterial infection |
11 |
|
35 |
No |
Yes |
No |
Antibiotics and steroids (case reported in 1972, before availability of acyclovir) |
7 |
|
39 |
Yes, but without recent outbreak |
Yes |
Yes |
Acyclovir, 200 mg, 5 times daily for 5 days |
5 |
|
47 |
Yes, but without recent outbreak |
Yes |
No |
Antibiotics and steroids (case reported in 1972, before availability of acyclovir) |
7 |
As in our patient’s case, a known history of herpes infection may not be evident. Viral shedding of HSV often occurs without clinical symptoms and can still occur for a few days after vesicles appear during the crusting stage, if a lesion appears at all.14,15 Furthermore, herpes folliculitis has been reported to present without surface epithelial changes, making occult herpes infections another diagnostic challenge.16
Herpes barbae should be considered as a possible diagnosis in patients whose symptoms are not responding to antifungal or antibacterial treatment for the infections of their beard area, especially when considering relevant history, such as history of herpes labialis, shaving history, and recent exposure to herpes labialis. Herpes barbae is often thought to be a disease seen in immunocompromised patients such as those with eczema or HIV but can occur in immunocompetent patients, as well. PCR assay of a sample of the affected areas allows for accurate determination of the causal pathogen, whether viral, fungal, or bacterial.17 If a high suspicion exists for HSV infection, and PCR results are negative for HSV, it may be worth checking HSV antibodies, especially in cases with no known history of HSV infection.
No clinical trials have been done to recommend the standard treatment for herpes barbae, although it is likely that the treatment for herpes gingivostomatitis, as reported in the cases above, would be sufficient. The patient in this case would have likely experienced spontaneous resolution of his symptoms given that he started antiviral treatment later in the course of his illness, so it is not clear whether the acyclovir he began taking improved the outcome.
Given that a major risk factor for herpes barbae is close shaving with a razor in the presence of an acute orolabial infection,18 it is imperative to educate patients on shaving practices in order to avoid irritation or trauma of the hair follicle, especially in men with a history of herpes infections of the mouth or face. As noted in this case, it would be best to recommend that patients avoid using old razors in order to not only reduce skin trauma, but also reduce the possibility of autoinoculation and spreading, since the razor can also serve as a fomite.19,20
REFERENCES:
- Looker KJ, Magaret AS, May MT, et al. Global and regional estimates of prevalent and incident herpes simplex virus type 1 infections in 2012. PLoS One. 2015;10(10):e0140765.
- Whitley R, Kimberlin DW, Prober CG. Pathogenesis and disease. In: Arvin A, Campadelli-Fiume G, Mocarski E, et al, eds. Human Herpesviruses: Biology, Therapy, and Immunoprophylaxis. Cambridge, England: Cambridge University Press; 2007:chap 3
- Mendoza N, Madkan V, Sra K, Willison B, Morrison LK, Tyring SK. Human herpesviruses. In: Bolognia JL, Jorizzo JL, Schaffer JV, eds. Dermatology. Vol 1. 3rd ed. Philadelphia, PA: Elsevier Saunders; 2012;chap 80.
- Laureano AC, Schwartz RA, Cohen PJ. Facial bacterial infections: folliculitis. Clin Dermatol. 2014;32(6):711-71
- Weinberg JM, Mysliwiec A, Turiansky GW, Redfield R, James WD. Viral folliculitis: atypical presentations of herpes simplex, herpes zoster, and molluscum contagiosum. Arch Dermatol. 1997;133(8):983-986.
- Gray J, McMichael AJ. Pseudofolliculitis barbae: understanding the condition and the role of facial grooming. Int J Cosmet Sci. 2016;38(suppl 1):24-27.
- Izumi AK, Kim R, Arnold H Jr. Herpetic sycosis: report of two cases. Arch Dermatol. 1972;106(3):372-374.
- Greenbaum SS. Folliculitis barbae traumatica. Arch Derm Syphilol. 1935;32(2):237-241.
- Al-Dhafiri SAM, Molinari R. Herpetic folliculitis. J Cutan Med Surg. 2002;6(1):19-22.
- Anliker MD, Itin P. Herpetic folliculitis barbae. A rare cause of folliculitis [in German]. Hautarzt. 2003;54(3):265-267.
- Campanelli A, Marazza G, Stucki L, et al. Fulminant herpetic sycosis: atypical presentation of primary herpetic infection. Dermatology. 2004;208(3):284-286.
- Parlette EC, Polo JM. Case study: inoculation herpes barbae. Skinmed. 2005;4(3):186-187.
- King DH. History, pharmacokinetics, and pharmacology of acyclovir. J Am Acad Dermatol. 1988;18(1 pt 2):176-179.
- Ramchandani M, Kong M, Tronstein E, et al. Herpes simplex virus type 1 shedding in tears and nasal and oral mucosa of healthy adults. Sex Transm Dis. 2016;43(12):756-760.
- Spruance SL, Overall JC Jr, Kern ER, Krueger GG, Pliam V, Miller W. The natural history of recurrent herpes simplex labialis: implications for antiviral therapy. N Engl J Med. 1977;297(2):69-75.
- Sexton M. Occult herpesvirus folliculitis clinically simulating pseudolymphoma. Am J Dermatopathol. 1991;13(3):234-240.
- Yang S, Rothman RE. PCR-based diagnostics for infectious diseases: uses, limitations, and future applications in acute-care settings. Lancet Infect Dis. 2004;4(6):337-348.
- Saleh D, Sharma S. Herpes simplex type 1. StatPearls. https://www.ncbi.nlm.nih.gov/books/NBK482197/. Updated May 6, 2019. Accessed June 12, 2019.
- Nerurkar LS, West F, May M, Madden DL, Sever JL. Survival of herpes simplex virus in water specimens collected from hot tubs in spa facilities and on plastic surfaces. JAMA. 1983;250(22):3081-3083.
- Douglas JM, Corey L. Fomites and herpes simplex viruses: a case for nonvenereal transmission? JAMA. 1983;250(22):3093-3094.


