Will recurrent knee pain hinder a teenage athlete's sports career?
How Do You Read These Images?

A 16-year-old boy has had recurrent right knee pain for the past few months. A few months earlier, he had a minor injury to the knee, which caused minimal pain. However, the knee continued to hurt on and off, and he now feels “something inside the knee.” The patient is an athlete, and the parents are concerned that the pain will hinder his participation in sports. He has had no knee swelling or redness. He denies pain in any other joint.
On physical examination, he sits comfortably. He has full range of motion of the knee and no crepitation. There is some tenderness on the medial aspect of the femoral condyle. Lachman, anterior drawer, and posterior drawer tests are negative. The knee is stable to varus and valgus stress.
Anteroposterior, lateral, and tunnel views of the right knee are shown.
What is the cause of this boy’s recurrent knee pain?
A. Fracture of the femoral condyle.
B. Osgood-Schlatter disease.
C. Osteochondritis dissecans.
D. Avulsion fracture of the patella.
E. Synovial osteochondromatosis.
(Answer and discussion on next page.)
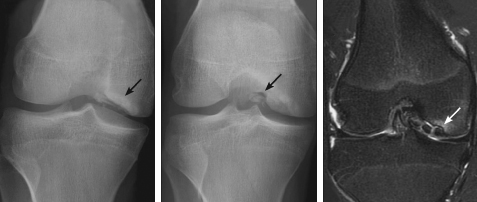
Answer: C, Osteochondritis dissecans
The radiographs show an osteochondral defect in the lateral aspect of the medial femoral condyle with intraarticular loose bodies. MRI of the knee, to delineate the extent of the lesion, shows an unstable, stage 4 osteochondral defect that involves the distal medial femoral condyle with at least 3 intraarticular loose bodies. In addition, there is small knee joint effusion with changes of mild synovitis.
In patients with osteochondritis dissecans (OCD), a portion of the cartilage and underlying subchondral bone separate from the joint and may become loose. The knee is by far the most commonly affected joint. The lateral portion of the medial femoral condyle is involved in three-fourths of the cases. The lesion may also occur at the elbow, ankle, and patella.
The prevalence of OCD is 0.3 cases per 1000 persons. It is far more common in boys than in girls (about 3:1). The incidence peaks in children and teens aged 10 to 15 years and is rare before age 10 years and after age 50 years.
OCD can be classified based on skeletal maturity: juvenile, adolescent, and adult. Each class has a distinct natural history and prognosis. OCD is staged radiographically to define the stability of the lesion:
•Stage 1: small, compressed, and nondisplaced.
•Stage 2: partially detached.
•Stage 3: fully detached but nondisplaced.
•Stage 4: fully detached and displaced.
A similar staging system is applied for bone scans and MRI. The bone scan staging system is particularly helpful in cases of juvenile OCD.
Although the exact cause of OCD is unknown, the 3 major possible causes are hereditary, vascular, and traumatic. About 40% to 60% of cases precede trauma. OCD is bilateral in 20% to 25% of cases, which suggests genetic or endocrine involvement. OCD is observed in a variety of hereditary conditions (Legg-Calvé-Perthes disease, Stickler syndrome, tibia vara). A vascular cause is most often suspected in adults.
The site and stage of the lesion determine the clinical presentation. Patients usually report vague knee pain, although some may be asymptomatic. They may experience intermittent locking if the lesion becomes loose. With unstable lesions, loose bodies may be palpable. On examination, the site of the lesion may be tender. Range of motion may be somewhat restricted. When the knee is involved, the Wilson sign is often positive (pain on extension and internal rotation of the knee).
Diagnosis is established with a plain radiograph. The tunnel view is particularly helpful in cases that involve the knees. MRI and bone scans help clarify the stage of the lesion, which determines the management and prognosis.
The natural history and the eventual outcome depend on the skeletal age in addition to the stability of the lesion. About 50% of lesions in young children tend to heal spontaneously. When OCD occurs in a mature skeleton, degenerative joint disease is more likely to develop.
The treatment protocol is based on the age, location, and disease stage. Asymptomatic patients are monitored closely every 4 to 6 months. Symptomatic juvenile and adolescent OCD is managed with activity restriction (non-weight–bearing, immobilization) for 6 to 12 weeks. Once symptoms resolve, gradual resumption of activity is advised. If the lesion is unstable (stages 3 and 4) or if conservative measures fail, the patient is referred to orthopedic surgery. Our patient underwent arthroscopic removal of the loose bodies and surgical correction of the osteochondral defect with an autograft.


