“Why Do I Always Feel Tired?” – Evaluating Older Patients Reporting Fatigue
Affiliations:
Division of Gerontology and Geriatric Medicine, Department of Medicine, University of Maryland Medical Center, Baltimore, MD
GRECC, Baltimore VA Medical Center, MD
Abstract: Fatigue is a common symptom in elderly persons, but it is often ignored as many patients and healthcare providers assume it is a natural progression of aging or may mistake it for somnolence, dyspnea, or muscle weakness. Since its importance is often underestimated, patients with fatigue may not receive an intervention, potentially resulting in significant functional decline. This article discusses the importance of identifying the underlying etiology or etiologies of a patient’s fatigue so that it can be eliminated, if possible, or managed appropriately. History-taking, including consideration of the patient’s symptom severity, is the most important part of evaluating fatigue. The authors present an algorithm that can be used to help identify the cause of a patient’s fatigue.
Key words: Fatigue, chronic fatigue syndrome, causes of fatigue, medication-related fatigue, physiological fatigue, algorithm for fatigue.
_____________________________________________________________________________________________________________________________________________
Although fatigue is common among older people, it is frequently underreported and often not even evaluated because, much like pain, it is often identified by both the older individual and his or her family or caregiver(s) as a natural part of the aging process. A 2010 study measuring the degree of interference with walking, work, and social interactions due to pain and fatigue showed that healthcare professionals tended to give a low priority to evaluating older persons reporting fatigue; in contrast, patients rated fatigue as one of the most important symptoms needing to be evaluated.1 Another recent study, which compared patient self-reports of symptom severity with inferences made by nurses and caregivers in a hospital chemotherapy unit, showed that nurses tended to underestimate the patients’ degree of fatigue.2 Such discrepancies delay work-up and/or intervention; therefore, it is important that healthcare professions caring for older persons not ignore symptoms of fatigue. The often-confusing manner in which the patient may express the problem of fatigue can complicate its identification. Individuals with fatigue, for example, frequently report that they are “weak.” If weakness is ruled out by physical examination, reports of weakness should be equated with fatigue and approached accordingly. This article provides an overview of fatigue in the older patient, including a discussion of its definitions, epidemiology, classification, and impact on older adults. It also offers an algorithm that can be used to evaluate and correct the etiology or etiologies of fatigue.
_______________________________________________________________________________________________________________________________________________
Related Content
Exploring Complaints of Fatigue in Older Patients
New Name, Diagnostic Criteria For Chronic Fatigue Syndrome
______________________________________________________________________________________________________________________________________________
Definitions of Fatigue
There is no universally accepted definition of fatigue because the condition is a subjective sensation. The National Institutes of Health defines fatigue as a feeling of weariness, tiredness, or lack of energy, which is different from drowsiness—a feeling of needing sleep—in that there is marked lack of motivation in one’s daily activities.3 Drowsiness and apathy can be symptoms of fatigue.3 One definition of fatigue requires the following characteristics: (1) an inability to initiate a normal activity due to perceived generalized weakness; (2) a reduced capacity to maintain activity (ie, easy fatigability); and (3) difficulty with concentration, memory, and emotional stability (ie, mental fatigability).4
At times, individuals report feeling fatigued when, in fact, they have other issues affecting their daily lives, such as boredom, distaste for work, exhaustion, lack of energy, sleepiness, tiredness, dyspnea, or weakness.5 While fatigue should be distinguished from symptoms of somnolence (ie, the quality or state of being drowsy), dyspnea (ie, difficult or labored respiration) and weakness, these symptoms may coexist with fatigue, especially in the older person, who is more likely to have multiple medical conditions. While there are many causes of dyspnea, such as chronic obstructive pulmonary disease (COPD) and congestive heart failure, fatigue itself is not associated with symptoms of dyspnea.6 In addition, an undiagnosed sleep disorder, such as narcolepsy or obstructive sleep apnea, may contribute to a patient’s fatigue.
Epidemiology of Fatigue
The current prevalence of fatigue in the US older adult population is not known because varying definitions of fatigue have been used in clinical studies.7However,population-based surveys from Britain and the United States have estimated the prevalence of fatigue to be between 6.0% and 7.5%, respectively.8An estimated 21% to 33% of patients who seek medical attention in primary care settings report having significant fatigue; further, symptoms of fatigue account for approximately 7 million office visits per year in the United States, with the majority of these patients being women.8
Classification of Fatigue
Fatigue may be categorized by its duration of symptoms (eg, recent [<1 month], prolonged [1-6 months], or chronic [>6 months]).4,9 Chronic fatigue may result from any number of causes that have evaded diagnosis and have continued without treatment for a prolonged period of time. In the absence of one of these causes, it may be identified as idiopathic chronic fatigue. Chronic fatigue syndrome has specific diagnostic criteria as defined by the Centers for Disease Control and Prevention (CDC) and should not be used to describe fatigue that does not have a specifically identified cause.4,10 Refer to the section below on chronic fatigue syndrome for detailed information on diagnosis.
Impact of Fatigue
Fatigue is of particular interest to researchers focused on geriatric and disability issues. This is not surprising when one considers the impact that this symptom has on middle-aged and older adults, especially those with medical disabilities. Self-reported fatigue has been associated with a worsening or altering of all of the following11,12:
- Physical function: reduced activities, prolonged periods of rest, uncoordinated movements, increased risk of falling, and increased need for assistance to meet basic activities of daily living and instrumental activities of daily living;
- Cognition: reduced alertness, decreased concentration, reduced clarity of thoughts, and increased forgetfulness;
- Emotional state: increased anger, emotional lability, and depression; and
- Social isolation: complete or near-complete lack of contact with other persons.
In addition, fatigue is an independent predictor of mortality and has been associated with a significant reduction in overall functional status.13
Etiologies of Fatigue
The causes of fatigue can be described under the following categories: organic (infectious, immunologic/rheumatologic), chronic fatigue syndrome, physiological, cancer-related, toxin-related, cardiovascular– and pulmonary disease–related, and psychogenic. The evaluation of a patient reporting symptoms of fatigue should address each possible cause, and healthcare professionals should recognize that older persons may have more than one cause for their presenting problem.
Organic Fatigue
Most causes of fatigue are secondary to some pathological disease process, the most common causes of which are infectious and immunologic/rheumatologic. Chronic fatigue syndrome is also considered an organic cause of fatigue by most, however, its cause remains unknown.
Infectious causes. Viral infections frequently cause fatigue. Hepatitis A, B, and C, Epstein-Barr virus (eg, mononucleosis), and HIV are common causes of fatigue. Most cases of acute hepatitis are subclinical.14 As such, patients may present with mild, nonspecific symptoms, including fatigue; therefore, it is important to consider various forms of hepatitis in these patients.
Further, while a rare problem in older persons, 95% of patients with mononucleosis present with fever, fatigue, pharyngitis, and lymphadenopathy, making the diagnosis of mononucleosis fairly obvious.15Physicians should keep in mind, however, that fever, lymphadenopathy, and pharyngitis resolve within 1 month, whereas fatigue usually persists for several months,15 which is why it is important to keep mononucleosis on the differential diagnosis list regardless of the patient’s age. The same holds true for HIV; primary HIV usually presents with nonspecific flu-like symptoms, such as fatigue.
Bacterial infections can also cause fatigue. Tuberculosis is an ever-present cause of fatigue that is frequently missed, especially in older persons who are at the highest risk for a reactivation of old disease.16 Lyme disease, occult endocarditis, and osteomyelitis are other conditions that can present as isolated fatigue and should be ruled out by careful history taking, physical examination, and appropriate testing.17 In contrast, a condition like secondary syphilis, which is being observed more frequently among older adults, has not been associated with isolated fatigue.
Immunologic/rheumatologic causes. Although fatigue is a common symptom of rheumatoid arthritis and systemic lupus erythematous, fatigue as an isolated presenting symptom in persons with these conditions has not been documented in the literature. Because fatigue is such a prominent symptom, and because an “insidious/general-onset syndrome” (ie, stiffness, fatigue, myalgia, low-grade fever) is well documented in persons who have rheumatoid arthritis,18 these immune diseases should be kept in the differential diagnosis. While most common earlier in life, rheumatoid arthritis may present during later life, and it has been associated with occult colon cancer.19
Celiac disease often presents subclinically with fatigue, mood changes, or nonspecific symptoms. A high percentage of celiac disease remains undiagnosed. A 2010 screening study reported a 7:1 ratio of undiagnosed to diagnosed celiac disease.20 In addition, as many as 15% of patients with newly diagnosed celiac disease are older than 65 years of age and have nonspecific symptoms.20 Therefore, it is important to include celiac disease in the differential diagnosis. Once a diagnosis has been made, a trial of a gluten-free diet may eliminate the patient’s symptoms.
Fibromyalgia should also be considered as a cause of fatigue. In general, the diagnosis of fibromyalgia is fairly obvious, with patients reporting fatigue along with widespread pain and tenderness at a minimum of 11 out of a possible 18 tender points.21 In addition, polymyalgia rheumatica presents with fatigue in 40% of cases and is usually not hard to distinguish from other causes of fatigue.22 The classic and telltale proximal muscle pain/stiffness is present in up to 95% of patients17; unless there is coexisting disuse atrophy, weakness is not a clinical feature of this disorder.
Chronic fatigue syndrome. Chronic fatigue syndrome, while usually classified under the organic causes of fatigue,has no known causes. Theories for this syndrome include viral infections, immune system problems, and hormonal imbalances. No proven psychiatric basis for this disorder has been identified, although there appears to be a higher rate of psychological problems in those with this disorder.23 There have been reports about an association between murine retrovirus infection and chronic fatigue syndrome, but more recent literature does not suggest any such association.24
Although chronic fatigue syndrome most commonly affects younger persons (usually women), it can occur at any age. The CDC has defined chronic fatigue syndrome as a debilitating, complex disorder characterized by profound fatigue that is not improved by bed rest and that may be worsened by physical or mental activity.25 Before being able to diagnose chronic fatigue syndrome, at least four of the following criteria must be identified and have persisted for at least 6 consecutive months without predating the fatigue26:
- Self-reported, significant impairment in short-term memory or concentration
- Frequent or recurring sore throat
- Tender cervical or axillary lymph nodes
- Muscle pain
- Multi-joint pain without redness or swelling
- Headaches of a new type, pattern, or severity
- Unrefreshing sleep
- Post-exertional malaise lasting more than 24 hours
To prevent overdiagnosis of chronic fatigue syndrome, caution is advised when making the diagnosis, and clear evidence must be identified in a patient’s medical history. Many persons are better served by having a diagnosis of idiopathic chronic fatigue rather than chronic fatigue syndrome, as there are many unproven remedies circulating on the Internet.
Medication-Related Fatigue
Although a review of the myriad medications that may contribute to fatigue is beyond the scope of this article, it should be obvious to the evaluating physician that medication imbalances need to be investigated and corrected in patients presenting with fatigue. A temporal relationship of fatigue with the initiation of medication may be a clue. The withdrawal of medication followed by a resolution of symptoms supports the diagnosis. Major medications associated with fatigue include nonsteroidal anti-inflammatory drugs, tetracycline, antipsychotics, antidepressants, sleep medications, and pain medications.27 Illicit drug and alcohol use should also be considered as a cause of fatigue.
Physiological Fatigue
Fatiguemay develop in any healthy individual experiencing any of the following circumstances:
- Inadequate sleep
- Insufficient rest
- Overactivity
- Poor physical conditioning
- Stress
- Changes in diet
Pregnant women, new parents, individuals who work at night, students, and healthcare professionals are the most prone to developing physiological fatigue because they most frequently experience the aforementioned circumstances. While older persons may not fit into these high-risk groups, healthcare providers should nevertheless conduct a detailed history regarding sleeping patterns, as arthritis and other medical conditions may interfere with an older person’s sleep, even if the patient is unaware that an underlying problem exists. Older adults frequently have atypical and/or nonspecific disease presentations, and sleep disturbances may be the earliest sign of a condition. A good history should help establish a link between fatigue and any life-changing event, such as the relocation of one’s domicile or a change in one’s job, living situation, or other influencing factors, all of which may be causing stress.
Fatigue is also closely related to frailty, a common geriatric syndrome marked by progressive physiologic decline. Although there are many definitions of frailty and no universally accepted diagnostic criteria as of yet, the two symptoms of frailty are fatigue and weakness.28 Weight loss and sarcopenia are likely contributors to these symptoms. Since fatigue and weakness are common and nonspecific in older adults, clinicians should remain vigilant to the possibility of frailty in the absence of history and physical findings suggestive of a particular illness. As frailty is associated with an increase state of vulnerability and increased risk of poor outcomes and death, it may be prudent to order a laboratory work-up to identify the patterns of change in the endocrine system and elevation in certain markers of inflammation that are associated with the underlying physiologic processes of frailty.28
Numerous studies have revealed that a diet lacking sufficient quantities of calories, protein, and/or the essential vitamins and minerals may lead to symptoms of fatigue. Even in the absence of caloric or other dietary deficiencies, any significant change in diet can result in fatigue; therefore, a detailed dietary history should not be overlooked. Vitamin B12 and vitamin D deficiencies should be examined specifically because they are common in geriatric patients.
Vitamin B12. Subclinical vitamin B12 deficiency is common in the elderly and can result from absorption problems, proton pump inhibitor overuse, excessive alcohol intake, or “tea and toast” diets. When it occurs, it can result in fatigue, weight loss, neuropathy, memory impairment, and depression. In a 1999 study, up to 15% of individuals aged 60 years and older were found to have vitamin B12 deficiency.29 It is also important to note that up to 28% of patients can have normal hemoglobin and hematocrit levels and a normal mean corpuscular volume in the setting of low levels of vitamin B12.29,30 An optimum level of vitamin B12 is higher than 300 pg/mL in persons aged 80 years and older.29,30
Vitamin D. A recent British survey found that more than 50% of adults have lower-than-normal vitamin D levels and that 16% had severe deficiency during winter months, when exposure to sunshine was limited.31 Many studies have claimed that vitamin D deficiency affects not only bones, but also muscles and the cardiovascular, respiratory, neurologic, and gastrointestinal systems.32 Vitamin D deficiency has also been associated with an increased incidence of falls and cognitive decline in the elderly.33,34In addition, a vitamin D–deficient state can cause nonspecific symptoms, such as fatigue, loss of muscle strength, bone and muscle pain, arthralgia, fibromyalgia-like syndromes, poor balance, and low mood.33 Therefore, symptoms consisting of muscle pains and weakness or fatigue only may warrant checking the patient’s vitamin D levels. An optimal level of 25-hydroxyvitamin D is considered to be higher than 30 ng/mL.32
Endocrine-Related Fatigue
Endocrine causes of fatigue include both hypothyroidism and subclinical hypothyroidism.35 Persons with subclinical hypothyroidism experiencing symptoms of fatigue may warrant a trial of low-dose thyroid hormone replacement therapy to lower their thyroid-stimulating hormone levels to normal. Hyperthyroidism may result in muscle atrophy, which can lead to nonspecific symptoms of fatigue followed by weakness.
The primary care physician should remember that fatigue is the most common symptom reported in perimenopausal/postmenopausal patients, presenting in more than 50% of these patients.36 Treatment of these cases may include exercise, testosterone, or hormone replacement therapy.37 There is a growing interest in the use ofgrowth hormone supplementation in aging patients, as this population experiences age-related decline in growth hormone levels. While supplementation reportedly improved fatigue in several small studies,37 side effects, such as high cholesterol levels, joint pain, and potential for tumorigenesis, must be considered—especially since its use has not been accepted as usual therapy. Androgen replacement therapy for andropausal men with low testosterone levels has been shown to improve sexual function, lean body mass, bone density, and strength, but has not yet demonstrated improvement in fatigue or vigor.38 Again, side effects, such as decreased testicular size, worsening of sleep apnea, stimulation of prostate gland growth, and fluid retention leading to congestive heart failure, must be taken into consideration. It is important to note that testosterone has not been advocated for elderly men with normal hormone levels. Finally, the physician may consider adrenal insufficiency as a potential cause of fatigue, especially in patients being tapered off of long-term steroid therapy.38 These individuals usually experience concomitant abnormalities in electrolyte levels and blood pressure.
Cancer-Related Fatigue
Although the literature is replete with discussions of multifactorial causes of fatigue in patients with cancer, fatigue is rarely the sole-presenting symptom in these individuals. The reasons for cancer-related fatigue are not well documented, but the disease process and treatment modalities, including side effects of chemotherapy, radiation therapy, and surgery, are contributing factors.39 For example, a tumor-induced hypermetabolic state is associated with weight loss, decreased appetite, and related fatigue; and anemia can be an adverse effect of chemotherapy, resulting in fatigue due to a reduction of hemoglobin levels in the blood.39 Many patients undergoing cancer treatment experience depression, stress, anxiety, and pain; as previously discussed, these symptoms as well as the medications used to treat them are associated with physiology-related fatigue.40 Individualized, age-appropriate screening and assessment are recommended for these patients.
Toxin-Related Fatigue
Exposure to toxins, such as carbon monoxide and heavy metals, should be considered as a potential cause of fatigue. Wood-burning stoves, kerosene heaters, automobile exhaust, and coal-burning plants produce carbon monoxide. Acute exposure to high carbon monoxide levels can cause headaches, dizziness, and flu-like symptoms.41 When chronic, low-level exposure occurs, however, more subtle symptoms may develop, such as depression, fatigue, confusion, and memory loss; thus, exposure to toxins is a vital consideration when diagnosing fatigue.
Similarly, with exposure to heavy metals, such as lead and/or arsenic, acute high-level exposure is rather easy to diagnose. For example, symptoms of acute massive exposure to lead include colic, encepatholopathy, anemia, neuropathy, and Fanconi syndrome.42 Chronic low-level exposure, however, is more difficult to detect; symptoms of excessive cumulative exposure to lead is associated with hypertension and gout, both of which are highly common in older adults.42 Again, this potential cause can be uncovered by detailed history-taking, as new onset hypertension and gout, for example, may signal the possibility of toxin-related fatigue.
Cardiovascular– and Pulmonary Disease–Related Fatigue
A strong association has been documented between chronic fatigue in the older patient and cardiac and pulmonary illnesses,43 including congestive heart failure and COPD. Such conditions should be medically optimized in patients to minimize fatigue, and long-term follow-up should be conducted.
Psychogenic Fatigue
Psychiatric problems commonly cause fatigue. One study indicated that psychiatric disorders and somatic amplification may contribute to symptoms of fatigue in approximately 50% of patients being treated in the primary care setting.44 Depression is the most commonly associated disease entity. Features suggesting that fatigue is psychogenic include fatigue being present throughout the day, fatigue being present upon awakening, fatigue that improves later in the day, and fluctuations in mood.45
Evaluation of Fatigue
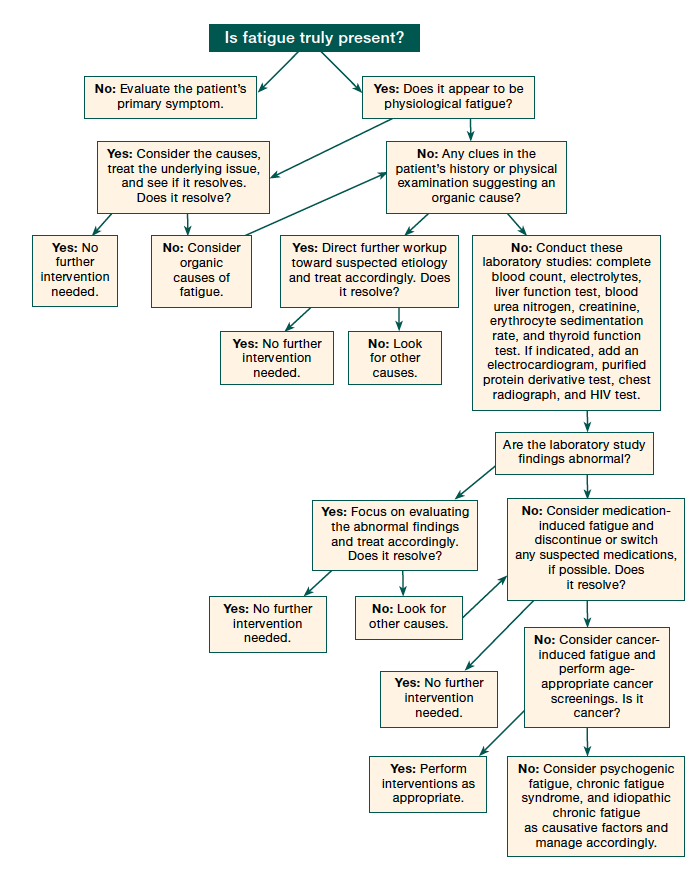
Open-ended questions that encourage patients to describe fatigue in their own words may elicit responses that help distinguish fatigue from dyspnea, somnolence, and true weakness (Figure). Onset of fatigue, whether gradual or abrupt, should be confirmed. Any relationship with a recent illness should be assessed for. The course of the symptom (ie, if stable, improving, or worsening) is also important. The duration and daily pattern of the fatigue, as well as the exacerbating and relieving factors, should be identified. Information should be obtained regarding the impact of fatigue on the person’s daily life, such as his or her ability to work and socialize. Symptoms suggesting underlying occult medical illness, including weight loss and night sweats, should be noted. Psychiatric disorders, particularly depression, anxiety disorders, somatoform disorders, and substance abuse, should be included in the history. Medication use (both prescribed and over-the-counter), recreational drug use, and alcohol use should be evaluated. A thorough and detailed physical examination should also be performed to determine the cause of fatigue.
Algorithm for a Work-up of Fatigue
Fatigue can be differentiated from sleepiness, weakness, and dyspnea by using the algorithm outlined in the Figure. We surmise that use of this algorithm can identify a cause of fatigue in more than 50% of cases.
Assessment of Severity of Fatigue (2 Head)
There are many different tools that can be administered to assess fatigue, such as the Multidimensional Assessment of Fatigue46 and the FACIT Fatigue Scale47; however, it is difficult to quantify fatigue, as no gold standard is available. The modified Chalder’s Fatigue Severity Scale can be used to measure each aspect of fatigue and key biological parameters48; this scale uses a scoring method of between 0 and 3 on the following questions:
1. Do you have problems with tiredness?
2. Do you need to rest more?
3. Do you feel sleepy or drowsy?
4. Do you have problems starting things?
5. Are you lacking in energy?
6. Do you have less strength in your muscles?
7. Do you feel weak?
8. Do you have difficulty concentrating?
9. Do you have problems thinking clearly?
10. Do you make slips of the tongue when speaking?
11. How is your memory?
A total score of greater than 18 points out of a possible 33 points is considered highly suggestive of fatigue.48
Conclusion
Fatigue is a common symptom, but one that is often ignored, especially in older adults. Since its importance is often underestimated, patients frequently have no intervention, which can lead to significant functional decline. Fatigue should be distinguished from somnolence, dyspnea, and muscle weakness. The presence of chronic fatigue syndrome as specified by the CDC guidelines should be considered. History-taking is the most important part of the evaluation of patients with chronic fatigue. Assessment should consider the impact of fatigue on the patient’s life. Laboratory studies should be limited in the absence of history or physical findings suggestive of a particular illness.
References
- Broderick JE, Schneider S, Schwartz JE, Stone AA. Interference with activities due to pain and fatigue: accuracy of ratings across different reporting periods. Qual Life Res. 2010;19(8):1163-1170.
- Akin S, Durna Z. A comparative descriptive study examining the perceptions of cancer patients, family caregivers, and nurses on patient symptom severity. Eur J Oncol Nurs. 2013;17(1):30-37.
- Fatigue. MedlinePlus Medical Encyclopedia. www.nlm.nih.gov/medlineplus/ency/article/003088.htm. Updated May 29, 2011. Accessed July 23, 2013.
- Morelli V. Fatigue and chronic fatigue in the elderly: definitions, diagnoses, and treatments. Clin Geriatr Med. 2011;27(4):673-686.
- Shen J, Barbera J, Shapiro CM. Distinguishing sleepiness and fatigue: focus on definition and measurement. Sleep Med Rev. 2005;10(1):63-76.
- Witte KK, Clark AL. Dyspnea versus fatigue: additional prognostic information from symptoms in chronic heart failure. Eur J Heart Fail. 2008;10(12):1224-1228.
- Meng H, Hale L, Friedberg F. Prevalence and predictors of fatigue among middle-aged and older adults: evidence from the Health and Retirement study. J Am Geriatr Soc. 2010;58(10):2033-2034.
- Fosnocht KM, Ende J. Approach to the adult patient with fatigue. UpToDate. www.uptodate.com/contents/approach-to-the-adult-patient-with-fatigue. Updated December 14, 2012. Accessed July 23, 2013.
- Vincent A, Brimmer DJ, Whipple MO, et al. Prevalence, incidence, and classification of chronic fatigue syndrome in Olmstead County, Minnesota, as estimated using the Rochester Epidemiology Project. Mayo Clin Proc. 2012;87(12):1145-1152.
- Demitrack MA. Chronic fatigue syndrome: a disease of the hypothalamic-pituitary-adrenal axis? Ann Med. 1994;26(1):1-5.
- Yu DS, Lee DT, Man NW. Fatigue among older people: a review of research literature. Int J Nurs Stud. 2010;47(2):216-228.
- Goedendorp MM, Knoop H, Schippers GM, Bleijenberg G. The lifestyle of the patients with chronic fatigue syndrome and the effect on fatigue and functional impairments. J Hum Nutr Diet. 2009;22(3):226-231.
- Hardy SE, Studenski SA. Fatigue predicts mortality in older adults. J Am Geriatr Soc. 2008;56(10):1910-1914.
- World Health Organization. Hepatitis B, www.who.int/csr/disease/hepatitis/whocdscsrlyo20022/en/index3.html. Accessed July 24, 2013.
- Petersen I, Thomas JM, Hamilton WT, White PD. Risk and predictors of fatigue after infectious mononucleosis in a large primary care cohort. QJM. 2006;99(1):49-55.
- Smith BM, Schwartzman K, Bartlett G, Menzies D. Adverse events associated with treatment of latest tuberculosis in the general population. CMAJ. 2011;183(3):E173-179.
- Brusch J. Infective endocarditis clinical presentation. Medscape Reference. http://emedicine.medscape.com/article/216650-clinical. Updated April 9, 2013. Accessed July 24, 2013.
- Campbell RC, Batley M, Hammond A, Ibrahim F, Kingsley G, Scott DL. The impact of disease activity, pain, disability and treatments on the fatigue in established rheumatoid arthritis. Clin Rheumatol. 2012;31(4):717-722.
- What’s the link between rheumatoid arthritis and cancer? Johns Hopkins Medicine Special Reports. www.johnshopkinshealthalerts.com/reports/arthritis/3308-1.html. Published November 2009. Accessed July 24, 2013.
- Jordá FC, López Vivancos J. Fatigue as a determinant of health in patients with celiac disease. J Clin Gastroenterol. 2010;44(6):423-427.
- Yunus MB, Aldag JC. The concept of incomplete fibromyalgia syndrome: comparison of incomplete fibromyalgia syndrome with fibromyalgia syndrome by 1990 ACR classification criteria and its implications in clinical practice. J Clin Rheumatol. 2012;18(2):71-75.
- Kermani TA, Warrington KJ. Polymyalgia rheumatic [published correction appears in: Lancet. 2013;381(9860):28]. Lancet. 2013;381(9860):63-72.
- American Accreditation Healthcare Commission. Chronic fatigue syndrome. Health Guide. New York Times. health.nytimes.com/health/guides/disease/chronic-fatigue-syndrome/print.html. Accessed July 24, 2013.
- Satterfield BC, Garcia RA, Jia H, Tang S, Zheng H, Switzer WM. Serologic and PCR testing of persons with chronic fatigue syndrome in the United States shows no association with xenotropic or poly tropic murine leukemia virus-related viruses. Retrovirology.2011;8:12.
- Centers for Disease Control and Prevention. Chronic fatigue syndrome. http://www.cdc.gov/cfs. Updated May 13, 2013. Accessed August 19, 2013.
- Centers for Disease Control and Prevention. CFS case definition. http://www.cdc.gov/cfs/case-definition/index.html. Updated May 14, 2012. Accessed August 19, 2013.
- Neel Jr, AB. 9 types of medications that can lead to chronic fatigue. AARP. www.aarp.org/health/drugs-supplements/info-06-2012/medications-that-cause-chronic-fatigue.4.html. Published June 12, 2012. Accessed July 23, 2013.
- Espinoza S, Walston JD. Frailty in older adults: insights and interventions. Cleve Clin J Med. 2005;72(12):1105-1112.
- Baik HW, Russell RM. Vitamin B12 deficiency in the elderly. Annu Rev Nutr. 1999;19:357-377.
- Appold K. Dangers of vitamin B12 deficiency. Aging Well. 2012;5(1):30.
- Chalmers JD, McHugh BJ, Docherty C. Govan JRW, Hill AT. Vitamin-D deficiency is associated with chronic bacterial colonization and disease severity in bronchiectasis. Thorax. 2013;68(1):39-47.
- Mahmoodi M, Westberg L. The importance of vitamin D in clinical practice. Journal of the Council on Nutrition. 2011;34(3):17-27.
- Kalyani RR, Stein B, Valiyil R, Manno R, Maynard JW, Crews DC. Vitamin D treatment for the prevention of falls in older adults: the cardiovascular health study. J Am Geriatr Soc. 2010;58(7):1299-1310.
- Soni M, Kos K, Lang IA, Jones K, Melzer D, Llewellyn DJ. Vitamin D and cognitive function. Scand J Clin Lab Invest Suppl. 2012;243:79-82.
- Almandoz JP, Gharib H. Hypothyroidism: etiology, diagnosis, and management. Med Clin North Am. 2012;96(2):203-221.
- O’Neill S, Eden J. The pathophysiology of menopausal symptoms. Obstetrics, Gynaecology and Reproductive Medicine. 2012;22(3):63-69.
- Schwartz E, Holtorf K. Hormone replacement therapy in the geriatric patient: current state of the evidence and questions for the future. Estrogen, progesterone, testosterone, and thyroid hormone augmentation in geriatric clinical practice: part 1. Clin Geriatr Med. 2011;27(4):541-559.
- Schwartz E, Morelli V, Holtorf K. Hormone replacement therapy in the geriatric patient: current state of the evidence and questions for the future. Estrogen, progesterone, testosterone, and thyroid hormone augmentation in geriatric clinical practice: part 2. Clin Geriatr Med. 2011;27(4):561-575.
- Fatigue and cancer fatigue. Cleveland Clinic. http://my.clevelandclinic.org/disorders/cancer/hic_cancer-related_fatigue.aspx. Updated January 6, 2011. Accessed July 23, 2013.
- Cheville AL. Cancer-related fatigue. Phys Med Rehabil Clin N Am. 2009;20(2):405-416.
- Jafri AB. Aging and toxins. Clin Geriatr Med. 2011;27(4):609-628.
- Kathuria P. Lead toxicity. http://emedicine.medscape.com/article/1174752-overview. Updated January 19, 2012. Accessed July 23, 2013.
- Whitson HE, Thielke S, Diehr P, et al. Patterns and predictors of recovery from exhaustion in older adults. J Am Geriatr Soc. 2011;59(2):207-213.
- Cathebras PJ, Robbins JM, Kirmayer LJ, Hayton BC. Fatigue in primary care: prevalence, psychiatric comorbidity, illness behavior, and outcomes. J Gen Intern Med. 1992;7(3):276-286.
- McCranie EJ. Neurasthenic neurosis: psychogenic weakness and fatigue. Psychosomatics. 1980;21(1):19-20, 23-24.
- Multidimensional Assessment of Fatigue. University of Washington Website. http://www.son.washington.edu/research/maf/. Accessed July 24, 2013.
- Tennant KF. Assessment of Fatigue in Older Adults: the FACIT Fatigue Scale (version 4). Try This General Assessment Series. Hartford Institute for Geriatric Nursing, New York University, College of Nursing. 2012;30. http://consultgerirn.org/uploads/File/trythis/try_this_30.pdf.
- Naschitz JE, Rozenbaum M, Shaviv N. Feeling of fatigue—fatigue severity by unidimensional versus composite questionnaires. Behav Med. 2004;29(4):167-172.
Disclosures: The authors report no relevant financial relationships.
Address correspondence to: Steven R. Gambert, MD, AGSF, MACP, University of Maryland Medical Center, N3E09, 22 S. Greene Street, Baltimore, MD 21201; sgambert@medicine.umaryland.edu


