What Is This Ulcerated Nodule on an Older Man’s Scalp?
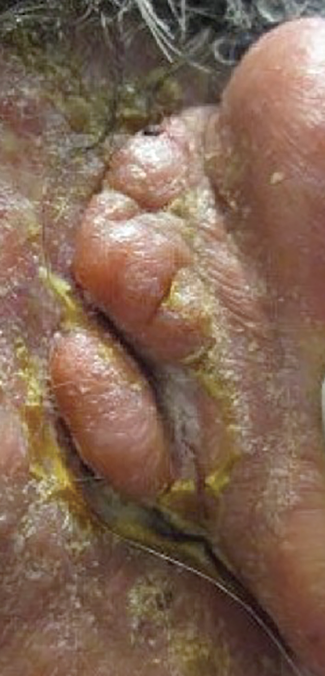
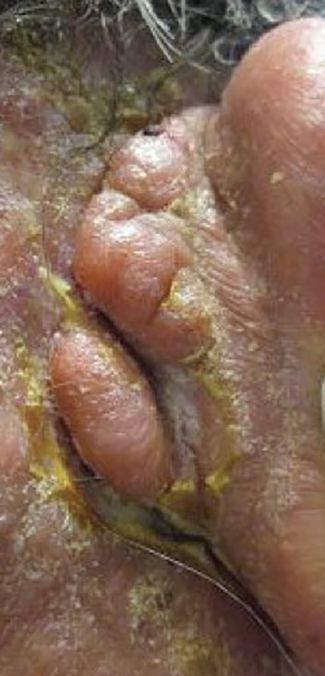
A 74-year-old white man with a history of severe plaque psoriasis presented for establishment of care; incidentally, an enlarging mass was found on the right posterior scalp.
The patient stated that the lesion had been present for approximately 1 month. He explained that the lesion had been evaluated in multiple urgent care settings, and he had been told that it was a traumatic wound, and no further workup had been pursued.
Examination at the time of his first dermatology evaluation revealed a 6-cm, skin-colored and pink to erythematous, ulcerated nodule draining malodourous yellow fluid and scant blood (Figure). The patient reported localized pain and tenderness of moderate severity. As the patient tilted his head downward and toward the right, the lesion became more brightly erythematous. Periorbital edema was noted on the right side.
The patient denied any constitutional symptoms, history of skin cancer, or known occupational chemical or radiation exposure. His medical history was significant for chronic obstructive lung disease, cardiovascular disease, atrial fibrillation, diabetes mellitus with chronic renal impairment, and gastroesophageal reflux disease. He had been a previous heavy smoker.
Answer and discussion on next page
Answer: Angiosarcoma
A shave biopsy of the scalp lesion was performed and stained with hematoxylin and eosin, as well as immunohistochemical stains for ERG, CD31, CD34, CD163, and S100 (Figures 2-4). The biopsy revealed morphologically high-grade epithelioid angiosarcoma. Immunohistochemistry showed lesional cells positive for CD31 and ERG, and negative for CD34 and S-100. Scattered histiocytes were positive for CD163. Metastases to regional lymph nodes and the spine were evident on positron emission tomography scan.
After discussion with surgical oncology, medical oncology, radiation oncology, and palliative care specialists, and after consideration of his multiple medical comorbidities, the patient elected for radiation therapy. After 2 fractions, the patient’s scalp was noted to have clinical improvement with decreased edema and ulceration, although the overall size of the mass did not change.
The patient’s clinical course was complicated by multiple hospitalizations for congestive heart failure exacerbation, altered mental status, and hospital-acquired pneumonia, as well several occasions where the patient refused radiation treatment. After discussion of goals of care, the patient ultimately elected for hospice care.
Discussion
Cutaneous angiosarcoma is a rare, aggressive, malignant tumor of vascular endothelial cells in the dermis, occurring on the head and neck in 60% of cases.1 Angiosarcoma is seen most often in elderly white men and notoriously carries a poor prognosis. While the etiologic factors of cutaneous angiosarcoma remain unknown, well-established associated risk factors include sun damage, radiation exposure, chronic lymphedema (Stewart-Treves syndrome), and exposure to chemicals such as polyvinyl chloride, thorium dioxide, radium, and arsenic.1
Cutaneous angiosarcoma is difficult to diagnose clinically, since it can mimic benign skin conditions in its early stages. Reports of delayed diagnosis describe cutaneous angiosarcoma having been mistaken for trauma-related bruising and abscesses.2 Previous studies have also identified cutaneous angiosarcoma in the setting of diverse benign skin conditions such as port-wine stains, lymphangioma circumscriptum, and epidermolysis bullosa dystrophica.3,4
Although angiosarcoma may be difficult to differentiate clinically from basal cell carcinoma or amelanotic melanoma, the location on the scalp in an elderly man supports the diagnosis of angiosarcoma over other cutaneous malignancies. Due to its lymphatic origin, cutaneous angiosarcoma may invade or obstruct lymphatic channels, leading to the physical examination findings of ipsilateral edema. This phenomenon of lymphatic obstruction is also demonstrated by the positive tilt test: The lesion becomes more brightly erythematous and edematous due to pooling of lymphatic fluid with gravity when the head is tilted downward toward the ipsilateral side.
Histologically, the epithelioid subtype of angiosarcoma can be distinguished from other forms of angiosarcoma by characteristic sheets of epithelioid cells resembling macrophages with abundant eosinophilic cytoplasm, vesicular nuclei, and prominent nucleoli.5 The grading of angiosarcoma is based on microscopic evaluation of mitotic activity and necrosis, and the grade independently indicates the probability of distant metastases and death from angiosarcoma.6 Epithelioid angiosarcoma is always considered to be histologic grade 3.
Upon immunohistochemical staining, ERG and CD-31 positivity in cases of angiosarcoma are nearly 100% sensitive.7 The lack of S-100 staining serves to rule out melanoma as a cause of this ulcerated mass. Basal cell carcinoma characteristically stains basophilic and exhibits features such as palisading and retraction artifact. In the case bacterial infection, organisms and characteristic inflammatory infiltrate would be seen; likewise, in the case of chronic fungal infections, hyphae, a characteristic inflammatory infiltrate, and remodeling of the tissues due to chronic inflammation (eg, hyperplasia or thickening of the epidermis) would be seen. The combination of histologic evidence of an epithelioid tumor combined with immunohistochemical staining for vascular markers supports the diagnosis of epithelioid angiosarcoma.
Cutaneous epithelioid angiosarcoma is difficult to diagnose clinically, but histologic diagnosis is straightforward after recognition of epithelioid cells in concert with selection of appropriate immunohistochemical stains for vascular cell-surface molecules.
This patient had presented to multiple providers and urgent care centers without further workup before the growth behind his ear was incidentally noted on examination by a dermatologist, when he presented for another skin condition. Had this tumor been biopsied and evaluated microscopically at an earlier stage, perhaps other treatment modalities beyond palliative measures could have been options for this patient.
This case illustrates how clinical observation must be combined with referral to a dermatologist and microscopic evaluation in order to make a timely and accurate diagnosis. This case also serves to bring awareness to the importance of a thorough examination, including behind the ears, which can identify diseases in which a delay in diagnosis can lead to significant morbidity and mortality.
The author discusses the case in this podcast:
Molly A. Storer, MS, is a student at the University of Massachusetts Medical School in Worcester.
Scott H. Bradshaw, MD, is a pathologist at Kingston General Hospital in Kingston, Ontario, Canada.
A. Shadi Kourosh, MD, is a dermatologist in the Department of Dermatology at Massachusetts General Hospital in Boston.
References:
- Albores-Saavedra J, Schwartz AM, Henson DE, et al. Cutaneous angiosarcoma: analysis of 434 cases from the Surveillance, Epidemiology, and End Results Program, 1973-2007. Ann Diagn Pathol. 2011;15(2):93-97.
- Rich AL, Berman P. Cutaneous angiosarcoma presenting as an unusual facial bruise. Age Ageing. 2004;33(5):512-514.
- King DT, Duffy DM, Hirose FM, Gurevitch AW. Lymphangiosarcoma arising from lymphangioma circumscriptum. Arch Dermatol. 1979;115(8):969-972.
- Schmutz JL, Kue E, Baylac F, Reichert-Penetrat S, Barbaud A. Angiosarcoma complicating Hallopeau–Siemens-type hereditary epidermolysis bullosa. Br J Dermatol. 1998;138(5):910-912.
- Ceyhan K, Percinel S, Kinkli G, Karaca E, Umudum H. Epithelioid angiosarcoma. Acta Cytol. 54(1):109-112.
- Rubin BP, Fletcher CDM, Inwards C, et al. Protocol for the examination of specimens from patients with soft tissue tumors of intermediate malignant potential, malignant soft tissue tumors, and benign/locally aggressive and malignant bone tumors. Arch Pathol Lab Med. 2006;130(11):1616-1629.
- Sullivan HC, Edgar MA, Cohen C, Kovach CK, HooKim K, Reid MD. The utility of ERG, CD31 and CD34 in the cytological diagnosis of angiosarcoma: an analysis of 25 cases. J Clin Pathol. 2015;68(1):44-50.


