What’s Causing This Infant’s Cough?
A 10-month-old, previously healthy, and fully immunized girl presented to our hospital with cough and respiratory distress. The symptoms had started 1 week before with upper respiratory infection–like symptoms, including a “croupy cough” that had been improving over the past 2 days until the time of presentation.
In the middle of the night, her parents had heard the girl crying and coughing abruptly from the next room. She had been gagging and apparently was unable to take a full breath. The parents noted an uncapped felt-tipped marker in close proximity to the infant, and they called 911 out of concern for possible foreign body aspiration or ingestion.
The girl was taken to an emergency department (ED) at another hospital, where she was noted to have stridor and persistent congested cough but no respiratory distress. Results of neck and chest radiography were read as negative for a foreign body, but given the possibility of an aspiration that was not visible on plain films, the infant was admitted to our hospital for observation and further evaluation, including contrast computed tomography (CT) of the neck and chest.
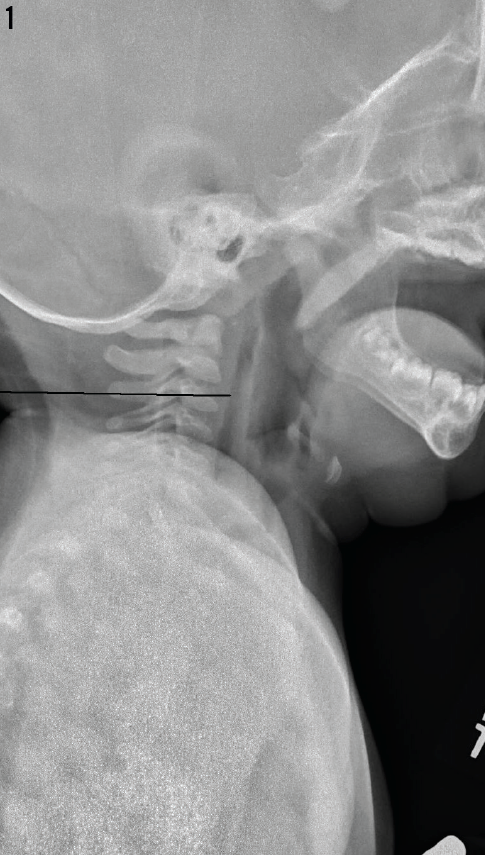
The lateral radiograph taken at the outside hospital is shown in Figure 1.
What does this image show, and what could be causing the girl’s symptoms?
(Answer and discussion on next page)
Answer: Retropharyngeal air caused by pharyngeal perforation
The patient had no prior hospitalizations or surgeries, had no allergies, and was not taking any medication. The parents could not identify any sick contacts. The girl was afebrile, had not vomited, and reportedly had appeared well before the acute onset of symptoms.
On admission, the patient appeared well; she was crying but was consolable by her parents and was in no acute distress. Physical examination findings included a temperature of 36.6°C, blood pressure of 120/59 mm Hg, pulse of 148 beats/min, respiratory rate of 32 breaths/min, and oxygen saturation of 99% to 100%. The stridor and cough observed at the outside ED had resolved.
Examination results were significant for clear nasal discharge, and examination of the mouth revealed moist mucous membranes, no erythema of the oropharynx, and no visible lesions or signs of injury. The patient’s neck was supple without appreciable lymphadenopathy, and the trachea was at the midline. The girl had normal respiratory effort without retractions or nasal flaring. Breath sounds were coarse bilaterally with transmitted upper airway noises. The rest of the physical examination findings were unremarkable.
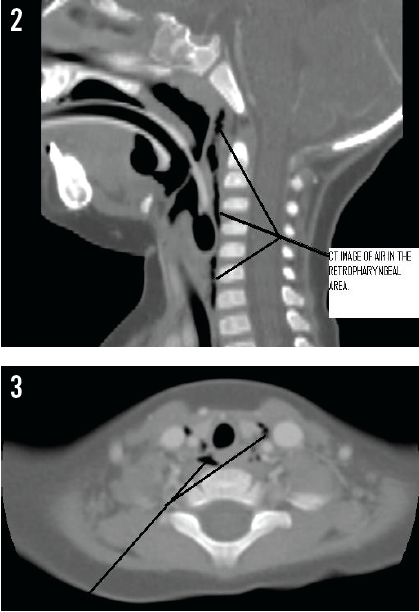
Lateral neck radiographs (Figure 1) taken at the outside hospital showed no foreign body, but the presence of a column of retropharyngeal air was concerning. Contrast computed tomography (CT) scans of the neck (Figures 2 and 3) and chest confirmed air tracking from the retropharyngeal space, through the chest, and into the mediastinum. Although the source of the air was unclear, this presentation has been seen in cases of perforation of the pharynx. Intravenous ampicillin-sulbactam was started for empiric coverage of aerobes and anaerobes to prevent mediastinitis in the context of likely perforation. Oral food and fluids were withheld.
When these findings were discussed with the parents, the mother noted that the girl had been holding an uncapped, soft-tipped marker when she had begun coughing and crying before admission. This suggested that the free air likely had resulted from self-inflicted injury with the marker to the oropharynx.
An upper GI series was done to assess for any perforation or continued leak. The study showed a normal esophagus without any observed abnormalities, indicating that the perforation had healed. An otorhinolaryngologist was consulted, who suggested overnight observation, restarting feedings in the morning, and follow-up imaging in 24 to 48 hours to look for resolution of free air. The next morning, feeding was initiated with breast milk and advanced to solid baby food within a few hours. The patient’s mother reported normal feeding and behavior.
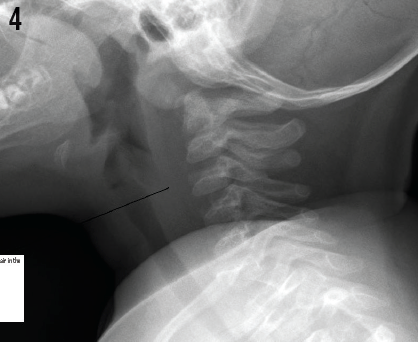
On day 3, chest radiographs (Figure 4) showed complete resolution of free air in the retropharyngeal space. The patient was discharged home that afternoon.
Discussion
Retropharyngeal free air is an uncommon finding, with limited data available on the most common etiologies and therapies in pediatrics. While the exact etiology of our patient’s injury was unclear, the most likely explanation is a small perforation of the oropharynx or hypopharynx. Her injury healed rapidly, within 24 hours of presentation, without surgery.
Our main concern was infection. We chose to use 1 day of intravenous ampicillin-sulbactam, followed by 9 days of amoxicillin clavulanate, to prevent the formation of a retropharyngeal abscess or the development of mediastinitis.
Luqman and colleagues document several pediatric cases in which failure to recognize pharyngeal injury early resulted in serious retropharyngeal infections.1 In these cases, the gravity of the injury had not been realized initially. Similar to our patient, patients in these cases had no symptoms related to pharyngeal trauma. The patients did not seek medical care until days later, after the development of swelling, fever, and odynophagia secondary to retropharyngeal abscess formation. In one case, abscess led to significant airway compromise requiring emergent intubation and surgical drainage. In another case, abscess spread downward, and the patient developed mediastinitis complicated by empyema thoracis requiring minithoracotomy and drainage. Luqman and colleagues suggest the need for conservative treatment with prophylactic antibiotics and esophageal rest to allow such injuries to heal spontaneously.1
Esophageal perforation is second only to cardiac surgery as the most common cause of mediastinitis.2 Esophageal injury presents a high risk of exposure to the aerobic and anaerobic bacteria of the oropharynx that commonly are implicated in mediastinitis.2
Pediatric oropharyngeal trauma most commonly results from a child falling on an object placed in his or her mouth or pushing an object into the mouth.3 One case-control study looked at the management of 107 patients who presented with evidence of oropharyngeal trauma over a 6-year period.3 All of the patients had clear signs of oropharyngeal trauma on physical examination, and each injury was graded based on appearance of the oral mucosa. The authors observed that the severity of the injury did not correlate with an increased risk of serious complications secondary to carotid artery damage. Therefore, they recommend that all children with oropharyngeal trauma undergo CT angiography to identify potential carotid artery damage.
In a case study of a patient found to have retropharyngeal air after presenting with severe odynophagia, the authors opted for surgical exploration before any imaging studies because of the patient’s severe discomfort.4 This course of action differs significantly from that chosen for our patient, who appeared to be in no discomfort throughout her hospitalization.
Clinical Teaching Points
This case shows the importance of maintaining a high index of suspicion for oropharyngeal or esophageal injury in children. Children may look and act well but may have a significant accumulation of air secondary to perforation with high risk of infection.1 Rapid recognition allows for antibiotic prophylaxis and esophageal rest to decrease infection risk and allow healing.
It also is essential to provide prophylactic antibiotic coverage against mediastinitis or retropharyngeal infection with aerobic and anaerobic pathogens. Infections usually are polymicrobial and derive from the oral cavity’s normal flora, including Bacteroides species, Peptostreptococcus species, Staphylococcus aureus, Staphylococcus epidermidis, and Streptococcus pyogenes.2
This case also highlights the importance of careful review of patients’ radiographs. The pediatric radiologist at our facility rapidly recognized the presence of retropharyngeal air, allowing for evaluation with repeated imaging and rapid initiation of antibiotics. The approach to pediatric patients with oropharyngeal trauma also must maintain a balance between identifying free air and limiting radiation exposure. A consulting pediatric otorhinolaryngologist recommended a second CT scan to determine whether the free air had resolved, while a consulting radiologist suggested radiography as a means to the same information while delivering less radiation. Therefore, we recommend starting with plain radiographs for an initial suspicion of esophageal perforation. If radiographic findings are positive, CT is helpful to identify the location of free air. Follow-up with a plain radiography likely is sufficient to assess for the resolution of free air in the retropharynx.
Virginia Dines, BS, is a third-year medical student at Georgetown University School of Medicine in Washington, D.C.
Mary Jane Reen, BA, is a third-year medical student at Georgetown University School of Medicine.
Yvonne Yui, MD, is a pediatric resident at Inova Children’s Hospital in Falls Church, Virginia.
Riva Kamat, MD, is a pediatric hospitalist at Inova Children’s Hospital.
William Yaakob, MD—Series Editor, is a radiologist in Tallahassee, Florida.
References
1. Luqman Z, Khan MAM, Nazir Z. Penetrating pharyngeal injuries in children: trivial trauma leading to devastating complications. Pediatr Surg Int. 2005;21(6):432-435.
2. Brook I. The role of anaerobic bacteria in mediastinitis. Drugs. 2006;66(3):315-320.
3. Soose RJ, Simons JP, Mandell DL. Evaluation and management of pediatric oropharyngeal trauma. Arch Otolaryngol Head Neck Surg. 2006;132(4):446-451.
4. Ellis DT II, Thompson JW, Godambe SA. Uncommon odynophagia: an unusual presentation of retropharyngeal free air in an adolescent. J Emerg Med. 2008;34(3):333-334.


