What’s the Cause of a 7-Year-Old’s Anogenital Pain and Pruritus?
The mother of a 7-year-old girl brought her into the clinic for evaluation of a 1-year history of itching of the vulva and painful bowel movements. The girl was otherwise in excellent health.
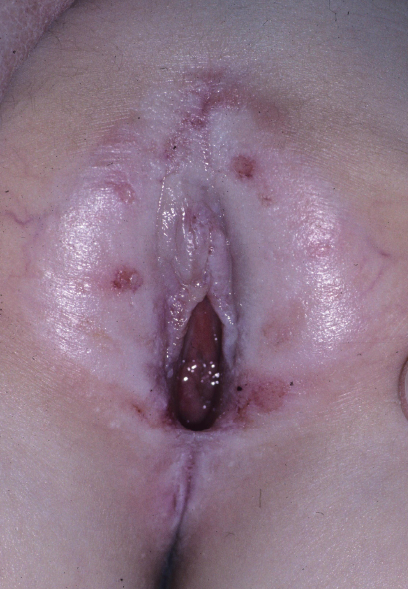
Physical examination revealed white, sclerotic appearing, wrinkled skin inside the labia majora, on the clitoral hood, and in the perianal area. A few areas of ecchymosis also were present in those areas. A painful fissure extended from the fourchette to the anus (Figure).
What is the cause of this girl’s pain and itching?
Answer: Lichen Sclerosus
The mother of a 7-year-old girl brought her into the clinic for evaluation of a 1-year history of itching of the vulva along with painful bowel movements. The girl was otherwise in excellent health.
Physical examination revealed white, sclerotic appearing, wrinkled skin inside the labia majora, on the clitoral hood, and in the perianal area. A few areas of ecchymosis also were present in those areas. A painful fissure extended from the fourchette to the anus (Figure).
The girl received a clinical diagnosis of lichen sclerosus, a chronic inflammatory dermatosis that can manifest on any region of the body but that most commonly occurs on the anogenital region, including the vulva, perianal area, and the foreskin of the penis.1 Lichen sclerosus most frequently is found in prepubertal girls and postmenopausal women.1
Persons with vulvar lichen sclerosus present with white wrinkled or scaly patches around the vulva, anus, or both. These lesions are susceptible to easy tearing and bruising. For this reason, lichen sclerosus in children can be misdiagnosed as trauma related to sexual abuse.1 Lesions that involve the perineum and anus can form a notable figure-8 or hourglass shape.2,3
While the etiology of lichen sclerosus is unknown, it may be related to hormonal, genetic, and autoimmune factors.3
The progression of lichen sclerosus can lead to severe scarring that can cause narrowing of the vaginal opening and resorption of the labia minora and clitoral hood.2 Less commonly, the head of the penis and the foreskin of uncircumcised males can be involved, leading to phimosis.2
Lichen sclerosus may be asymptomatic but usually is pruritic, leading to excoriations and thickening of the vulvar skin.3 Other symptoms include dysuria, and discomfort from anal involvement leading to constipation and bleeding from skin tears and fissures.2
The diagnosis of lichen sclerosus in children is usually made clinically, because vulvar biopsy may be traumatic for these patients.
Treatment is focused on relieving symptoms and preventing scarring. A potent topical corticosteroid such as clobetasol or fluocinonide is applied to the involved area once a day until symptoms resolve.2 While lichen sclerosus generally is quite resistant to corticosteroid atrophy, it nonetheless is important to avoid applying a topical corticosteroid to uninvolved skin, so as to prevent atrophy. The sclerotic skin may revert to normal-appearing mucosa with corticosteroid therapy, but treatment will not reverse any scarring and/or atrophy that already has occurred.1 Topical corticosteroids should be tapered as signs and symptoms of lichen sclerosus improve. Patients should be followed up closely for signs of corticosteroid atrophy such as striae, telangiectasia, or thin skin. A topical corticosteroid ointment often is preferred over a cream, because an ointment may be less likely to cause burning, stinging, or allergic reactions.3
Skin tears and fissures associated with lichen sclerosus can be treated with mupirocin ointment twice a day until they heal. A stool softener may be used to prevent the pain and tearing that can occur with bowel movements. In boys, circumcision is the best treatment for phimosis resulting from lichen sclerosus.1,3
Although there is no known prophylactic treatment for lichen sclerosus, it is important to treat lichen sclerosus in its early stages to prevent disease progression and irreversible degeneration and scarring of the skin in the urogenital areas.
Shaunte McKay, BA, is a student at the University of Virginia School of Medicine in Charlottesville, Virginia.
Barbara B. Wilson, MD, is an associate professor and chair of the Department of Dermatology at the University of Virginia School of Medicine.
References
1. National Institute of Arthritis and Musculoskeletal and Skin Diseases, National Institutes of Health, US Department of Health and Human Services. Questions & Answers about … Lichen Sclerosus. Bethesda, MD: National Institute of Arthritis and Musculoskeletal and Skin Diseases; 2004. NIH publication 04-5585.
2. Hengge UR. Lichen sclerosus. In: Goldsmith LA, Katz SI, Gilchrest BA, Paller AS, Leffell DJ, Wolff K, eds. Fitzpatrick’s Dermatology in General Medicine. Vol 1. 8th ed. New York, NY: McGraw-Hill; 2012:702-706.
3. Hoffman BL, Schorge JO, Schaffer JI, et al. Benign disorders of the lower reproductive tract. In: Hoffman BL, Schorge JO, Schaffer JI, et al, eds. Williams Gynecology. 2nd ed. New York, NY: McGraw- Hill; 2012:110-131.


