What Is the Cause of This Girl’s Knee Pain?
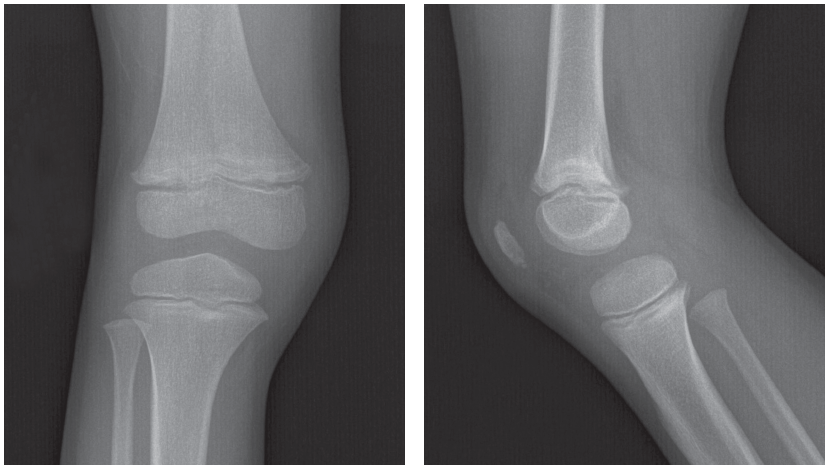
A 3-year-old girl has had intermittent fevers for the past 3 months and right knee pain for the past week. The day before the onset of the knee pain, she had fallen from a bed but denied any pain at that time. She has temporary relief of symptoms with ibuprofen; however, the right knee pain has been worsening and she is refusing to walk. A month before presentation, the child had left shoulder pain that spontaneously resolved in 2 weeks. She has no significant past medical history. Her immunizations are up-to-date.
The patient’s temperature is 36.7°C (98.2°F); heart rate, 125 beats per minute; blood pressure, 100/63 mm Hg; and respiration rate, 22 breaths per minute. On physical examination, she is in pain and has limited flexion and extension of the right knee. There is no warmth, erythema, swelling, or point of tenderness and no abnormalities of other joints. She has conjunctival pallor. The results of oral, skin, lymph node, pulmonary, cardiac, abdominal, and neurological examinations are unremarkable.
Anteroposterior and lateral views of the right knee are shown.
How do you read these images?
A. Lead poisoning.
B. Leukemia.
C. Normal variant.
D. Juvenile idiopathic arthritis.
E. Osteomyelitis.
(Answer and discussion on next page.)
ANSWER: B, leukemia
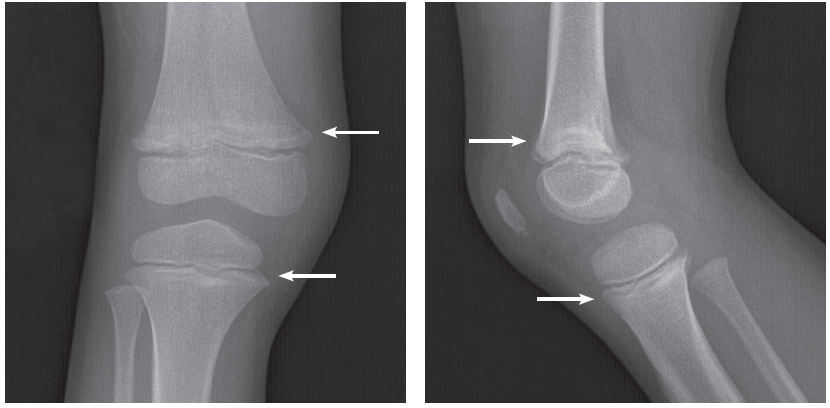
The radiographs show transverse radiolucent metaphyseal bands, uniform and regular across the metaphyses of the distal right femur and proximal right tibia. These transverse bands of radiolucency are suggestive of an infiltrative process such as leukemia. No fracture or dislocation is apparent.
The patient’s laboratory data included a white blood cell count of 5000/µL, with differential of 4% segments and 4 blast cells; hemoglobin level of 5.6 g/dL, with reticulocyte count of 1.4%; platelet count of 95,000/µL; erythrocyte sedimentation rate, 135 mm/h; C-reactive protein, 6.92 mg/L; and lactate dehydrogenase, 482 U/L. Flow cytometric analysis of a bone marrow aspirate sample detected 20% B lymphoblasts. Precursor B-cell acute lymphoblastic leukemia was diagnosed.
Radiographic abnormalities of the metaphysis are common in children with systemic and local disease. In the metaphysis, ossification of physeal cartilage occurs by a combination of osteoclastic resorption and osteoblastic formation of bone, nourished by metaphyseal vessels.1,2
Radiolucent metaphyseal bands are common radiographic findings in children with acute lymphoblastic leukemia (40% to 53% of cases).2 Radiolucent bands are thought to be caused by inadequate osteoblastic formation from malnutrition and/or accumulation of leukemic cells.1,3,4 The bands are usually noted in a distal femur, a rapid growth site.
In contrast, radiopaque metaphyseal bands in children are most commonly a normal variant, which is the result of abundant calcification involving the distal femur and proximal tibia. Radiopaque metaphyseal bands are also associated with lead poisoning, in which inhibition of osteoclastic remodeling results in increased osteoblastic bone deposition of the distal femur, proximal tibia, and proximal fibula.
Basic radiographic changes in juvenile idiopathic arthritis include bony erosions, joint-space narrowing, subchondral cysts, and epiphyseal overgrowth from hyperemia. Juvenile idiopathic arthritis is diagnosed after exclusion of other causes.5
In children, bone and joint infections typically affect the metaphysis, which is highly vascularized, and radiographs can reveal a lytic lesion in the metaphysis, periosteal new bone, and widening of the joint.6
Acute lymphoblastic leukemia is the most common childhood leukemia, with an incidence of 2.8 cases per 100,000 children in the United States.7 Peak incidence is between 2 and 5 years. Precursor B-cell acute lymphoblastic leukemia has a good prognosis.
Acknowledgment: Special acknowledgment is given to Dr Katherine Ender, assistant clinical professor of pediatric hematology and oncology at Harlem Hospital Center.


