The Uncontrollable Child: Family and Educational Interventions
The Uncontrollable Child:
Family and Educational Interventions
______________________________________________________________________________________________________________________________________________________
ABSTRACT: The therapeutic goal of psychosocial treatments for children with disruptive behavior problems, such as attention-deficit/hyperactivity disorder, is to improve relationships and communication among children, parents, and teachers. The bulk of therapy involves “parent training”—instructing parents on how to regulate their children’s behavior and implement behavior management skills. This can be delivered via group, parents-only, or individualized family therapy in 10 to 20 weekly or biweekly sessions. Helping parents establish a partnership with teachers through the use of a daily report card and homework intervention can improve school performance. When addressing developmental differences, encourage parents of preschoolers to provide a “curriculum of the home” and stress to parents of adolescents the importance of including the teen in the treatment process.
It is estimated that about 20% of children and adolescents meet criteria for a mental health disorder, and a high percentage of these youths are impaired by disruptive behavior problems. Children with disruptive behavior problems include those who meet criteria for attention-deficit/hyperactivity disorder (ADHD), oppositional defiant disorder (ODD), or conduct disorder (CD), as well as those who have impairments related to disruptive behavior who may not meet formal criteria for one of these diagnoses. While medication is generally an effective treatment for children with disruptive behavior problems, in particular ADHD,1 some form of nonpharmacological treatment is often necessary to help these children function normally in academic and social settings.
______________________________________________________________________________________________________________________________________________________
RELATED CONTENT
Treatment of ADHD: A Developmental Approach
Disruptive Behavior Disorders: What's Normal--What's Not?
______________________________________________________________________________________________________________________________________________________
A wide range of nonpharmacological inter ventions have been shown to be effective in managing family and school impairments associated with disruptive behavior problems. Psychosocial interventions can be family-based or school-based. (For a description of school-based interventions, see the review by Power and colleagues.2) In this article, we summarize empirically supported family-based psychosocial treatments for children aged 5 to 12 years with disruptive behavior problems, including ADHD, ODD, and CD. We emphasize family-based interventions that can have an effect on children’s functioning in both family and school settings and that can be delivered within the pediatric primary care setting or in connection with a mental health practice. Because these interventions require slight adjustments depending on developmental stage and economic background of the child,3 we also review adaptations for working with preschool children, adolescents, and families from underserved populations.
Unfortunately, well below 50% of children who need mental health care actually receive services. Children and adolescents who are least likely to receive services are those belonging to racial and ethnic minority groups, who are disproportionately represented among the poor and uninsured in this nation.4 Barriers to mental health care can be divided into access problems (cost of services, availability of care) and family beliefs (lack of trust in health care system or providers, unfavorable views about evidence-based treatments) that may preclude engagement in services.5
Pediatric primary care practices and schools are major venues for the delivery of mental health services to children and adolescents. Providing mental health services in these settings can improve access and help overcome some of the barriers to care. Nonetheless, when addressing the needs of youths with disruptive behavior problems, pediatric providers face substantial challenges, including limited time, reimbursement issues, and lack of mental health care training.6 Models of collaborative practice with mental health providers have been developed to address these limitations and are discussed in this article in an effort to help pediatricians implement evidence-based interventions.
EVIDENCE-BASED PSYCHOSOCIAL TREATMENT
Family-based behavioral interventions. More than 4 decades of research indicate that family-based psychosocial interventions are effective treatments for children with ADHD, ODD, or CD.7-9 These interventions are guided primarily by attachment theory, social learning principles, and cognitive-behavioral theories of change that involve both altering antecedents and consequences of behavior and building cognitive skills. Often referred to as “parent training” programs, effective family-based interventions are typically parent-mediated in that the bulk of therapeutic work is conducted face-to-face with parents in an effort to modify the home environment and patterns of parent-child interaction.
Parent training protocols involve a number of common elements in that they:
- Educate parents about their child’s condition and how symptoms lead to concerns at home, at school, and with peers.
- Teach parents ways to establish or maintain a warm and positive relationship that facilitates attempts to regulate their children’s behavior.
- Help parents implement behavior management skills at home. Specific skills include the use of effective commands and positive reinforcement/ praise in response to appropriate behavior, the development of a contingency management system (ie, token economy, point system), and the use of strategic punishment.
The goal of parent training protocols that address childhood ADHD, ODD, antisocial behavior, and other externalizing problems is to improve relationships among family members and teach effective behavior management strategies. Depending on the nature of the problem, parent training programs can be delivered via group treatment with parents and children, individual treatment with parents only, or individualized family treatment. Parent training programs typically last between 10 and 20 weekly or biweekly sessions, with follow-up “booster sessions” to track progress and problem-solve future challenges.
Techniques used to reach treatment goals include didactic instruction, skill-building exercises, roleplaying, coaching, and homework assignments. Homework assignments involve the implementation and monitoring of a new strategy between sessions. A number of excellent Web sites (eg, www.pcit.org, www.incredibleyears.com) and books provide more detailed descriptions of parent training programs.10,11 Forchildren with severe conduct problems,parent training approaches are often accompanied by evidencebased problem-solving skills training delivered directly to the child.12
Educational interventions involving the family. Family involvement in education has been shown to improve school performance of children with disruptive behavior problems. Table 1 provides an example of a 12-session family-school intervention program. An important component of successful family involvement is the establishment of a partnership between parent and teacher.13 Conjoint behavioral consultation is an evidenced-based method of building such a partnership that can be integrated into traditional parent training programs.14 A core feature of this method is the recognition that the parent-teacher partnership can improve the school performance of children with disruptive behavior problems.

Daily report card. One way children with a wide range of disruptive behavior problems can benefit from conjoint behavioral consultation is through the use of a daily report card. This typically includes 3 to 5 target behaviors or goals that specify clear behavioral expectations (eg, raises hand to speak, completes work quietly). Teachers then rate the child’s achievement on these goals throughout the school day. Finally, parents provide positive reinforcement contingent on performance on the daily report card. Use of a daily report card has been found to decrease disruptive behaviors and associated impairments among children with ADHD in special education. 15 A school-based intervention program that included the use of daily report cards also led to improvement in parent and teacher ratings of attention, social functioning, and organizational skills.16
Homework intervention. Homework can be quite challenging for many children and families, particularly if the child exhibits defiant or inattentive behavior. Children with attention problems often forget materials necessary to complete assignments, do not record assignments correctly, procrastinate during homework sessions, and make careless mistakes on assignments.17,18 Behavioral interventions have been shown repeatedly to be effective in improving homework performance.19,20
If families present with concerns about homework completion, pediatricians can help by providing suggestions about:
- Goal setting (ie, breaking assignments into manageable units and setting time limits for completion).
- Positive reinforcement (ie, providing tokens or rewards contingent on timely homework completion or sustained effort during the homework session).
- Environmental modifications (ie, identifying a consistent, quiet location or homework sessions and ensuring that necessary supplies are available).
Homework is also a mechanism for promoting ongoing home-school communication through daily assignments.21 For children with attention problems or disruptive behavior, communication between home and school often is strained.22 Health care providers can encourage families to discuss homework issues directly with teachers (eg, amount of work assigned, difficulty level of assignments). For cases in which the home-school relationship appears to be particularly strained, physicians might recommend that the family work with a consultant (eg, school psychologist, guidance counselor) to develop homework strategies while supporting a collaborative homeschool relationship.
Homework is also a mechanism for promoting ongoing home-school communication through daily assignments.21 For children with attention problems or disruptive behavior, communication between home and school often is strained.22 Health care providers can encourage families to discuss homework issues directly with teachers (eg, amount of work assigned, difficulty level of assignments). For cases in which the home-school relationship appears to be particularly strained, physicians might recommend that the family work with a consultant (eg, school psychologist, guidance counselor) to develop homework strategies while supporting a collaborative homeschool relationship.
Other interventions. Interventions for disruptive behavior not discussed in this article include those that are intended for implementation in alternative settings or require a level of care and resources not typically available in primary care. Examples of these are school-based approaches to improve attention, behavior, and social behavior2,27; comprehensive summer treatment programs that provide behavioral parent training, social activities, and academic instruction in a camp-like setting28; and multisystemic therapyb to decrease the risk of out-of-home placement for children who exhibit a persistent pattern of serious antisocial behavior.29
ADAPTATIONS FOR DIFFERENT AGE-GROUPS AND THE UNDERSERVED
Working with preschool-aged children. Although the principles underlying psychosocial treatment for preschool-aged children with disruptive behavior problems are the same as those for older children, strategies need to be adjusted to address developmental differences. For instance, when implementing a token reinforcement system with young children, remind parents that reinforcement must be delivered more frequently than with older children. Reinforcement options may need to be altered more often in order to maintain the novelty of the system. Although preschoolers do not have homework, parents can establish a “curriculum of the home” through consistently communicating the value of education and creating a home environment that supports learning (ie, by limiting TV and video game time and providing educational games and materials).30,31
Working with adolescents. Disruptive behavior problems often persist or emerge in the adolescent years. In adolescence, externalizing problems are often associated with more serious impairments. Perhaps the most important adaptation when working with adolescents with disruptive behavior disorders is the need for greater inclusion of the adolescent in many aspects of treatment. Given adolescents’ desire for greater autonomy from parents, traditional parent-mediated interventions are likely to generate significant conflict without sufficient engagement from the adolescent. Adherence and outcomes are likely to be optimal when an adolescent acknowledges a concern and is a willing participant in therapy. Teens may be increasingly involved in the development of token economies or the implementation of homework strategies.32 Individual therapy to address comorbid internalizing problems, additional school supports, and the involvement of peers when establishing antecedent strategies of a contingency management system may also be needed.
Working with underserved populations. Families in inner-city urban or isolated rural environments may encounter more difficulties in obtaining care than other families. Inner-city urban families face economic hardships, high levels of family unemployment, single-parent homes, and community violence at a higher rate than other families.33 All of these factors may have an impact on help-seeking behavior. Because of issues related to mistrust of the health care system,34 these families may be hesitant to seek help when a problem exists. By definition, isolated rural families must travel long distances to visit health care providers and may be uninsured or live below the poverty line.35,36 A recent study found that only 36% of rural children with an identifiable mental health disorder had received care in the preceding months.37
Eiraldi and colleagues38 proposed a model of help-seeking behavior that is specifically designed for underserved children with disruptive behavior disorders. The model highlights challenges and proposed solutions to promote help-seeking in each of 4 stages: problem recognition, decision to seek help, service selection, and use of service. One strategy to improve access is to offer mental health services in more trusted medical homes (ie, pediatric primary care center) or alongside health care providers or social workers who have an established relationship with the family. Regularly screening for behavior problems, educating parents and caregivers about the nature and treatment of behavioral health problems, and discussing parents’ expectations of and attitudes about treatment can also address certain barriers to care. it may be helpful for primary care practices to designate a staff member to serve as a behavioral health liaison and consult with families who screen positive for behavior problems.
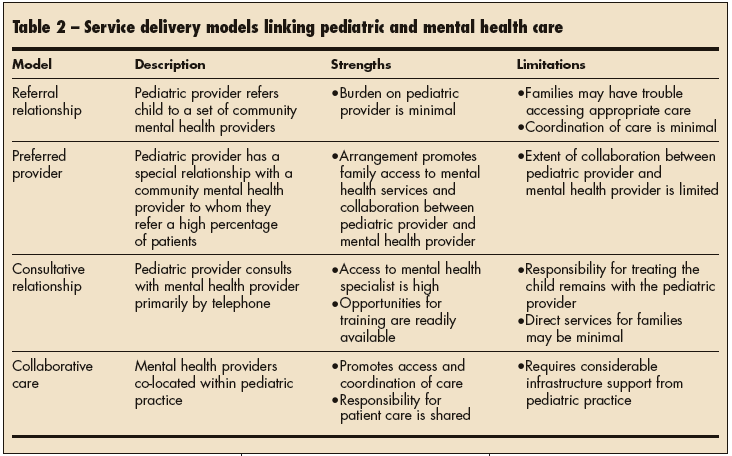
MODELS OF SERVICE DELIVERY
Table 2 lists 4 service delivery options that promote collaboration between pediatric providers and mental health professionals to address the behavioral health needs of children identified in pediatric practice.38-40 Strengths and limitations of each model are described. The approach that is best suited to a particular practice depends on the goals and preferences of pediatric providers, feasibility issues (space in the practice setting and administrative support for mental health services), and mental health resources in the community.■


