Topical Calcineurin Inhibitors for Vitiligo: Treatment Options
Consultations & Comments
Reader Reaction and Timely Answers From Experts
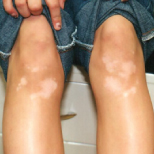 I read with interest Dr Alexander K. C. Leung and Mr Andrew S. Wong’s What’s Your Diagnosis? quiz featuring a 16-year-old boy with progressive hypopigmented lesions (CONSULTANT FOR PEDIATRICIANS, December 2010, page 433). I am curious to know how Dr Leung treats vitiligo with pimecrolimus——twice daily, for how long? Does he have Medicaid cover the cost?
I read with interest Dr Alexander K. C. Leung and Mr Andrew S. Wong’s What’s Your Diagnosis? quiz featuring a 16-year-old boy with progressive hypopigmented lesions (CONSULTANT FOR PEDIATRICIANS, December 2010, page 433). I am curious to know how Dr Leung treats vitiligo with pimecrolimus——twice daily, for how long? Does he have Medicaid cover the cost?
Dmitri De La Cruz, MD
Fresno, Calif
Topical calcineurin inhibitors, such as tacrolimus and pimecrolimus, are effective in the repigmentation of vitiligo.1,2 They can be applied to the lesion twice a day. I continue treatment until repigmentation is complete or until the lesion shows no further improvement after continuous application of the medication.
Compared with topical corticosteroids, topical calcineurin inhibitors are a lot more costly. However, they have a better safety profile than corticosteroids and are generally preferred for lesions on the face, neck, genitalia, and intertriginous areas.3,4 In Canada, topical calcineurin inhibitors are covered by the majority of insurance plans. Perhaps a US physician could respond to the question regarding Medicaid?
Alexander K. C. Leung, MD
Clinical Professor of Pediatrics
University of Calgary
Pediatric Consultant
Alberta Children’s Hospital
REFERENCES:
1. Isenstein AL, Morrell DS, Burkhart CN. Vitiligo: treatment approach in children. Pediatr Ann. 2009;38:339-344.
2. Lo YH, Cheng GS, Huang CC, et al. Efficacy and safety of topical tacrolimus for the treatment of face and neck vitiligo. J Dermatol. 2010;37:125-129.
3. Taïeb A, Picardo M. Clinical practice. Vitiligo. N Engl J Med. 2009;360:160-169.|
4. Leung AK. Vitiligo. In: Leung AK, ed. Common Problems in Ambulatory Pediatrics. New York: Nova Science Publishers, Inc; 2011:1249-1254.
I am happy to offer my opinion on the use of topical calcineurin inhibitors for vitiligo in the United States. I do not believe there is any standard protocol for the use of pimecrolimus in the treatment of vitiligo. Unfortunately, we typically are unable to obtain Medicaid coverage for this treatment. I usually start with a mid-potency topical corticosteroid,
such as mometasone, once a day. If the response is unsatisfactory after 3 months, I like to add topical pimecrolimus once a day. For facial vitiligo, I try to decrease the corticosteroid to 2 to 3 times a week and watch closely for the unwanted adverse effect of steroid atrophy. If I see no response after 6 to 9 months, I usually discontinue treatment.
Barbara B. Wilson, MD
Associate Professor of Dermatology
Associate Director, Residency Program
Department of Dermatology
University of Virginia School of Medicine
Charlottesville


