Testicular Microlithiasis
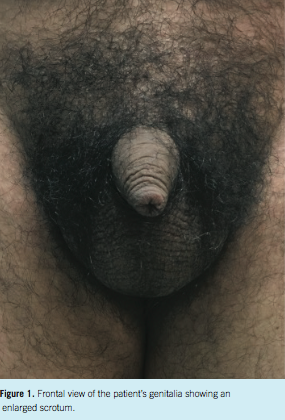
A 17-year-old boy presented for a well-adolescent visit and had no complaints. However, his physical examination was remarkable for a body mass index of 33 kg/m2 (98th percentile) and a scrotum that appeared enlarged (Figure 1). Palpation of the testes was difficult, but there were no signs of hernia or torsion. The rest of the physical examination was unremarkable, and his past medical and family histories were noncontributory. Scrotal ultrasonography with color and spectral Doppler imaging was performed, and the results showed bilateral testicular microlithiases and bilateral epididymal cysts (Figures 2-7). Furthermore, the scrotal ultrasonography showed normal testicular size without the presence of a hydrocele or a spermatocele.



DISCUSSION
Testicular microlithiasis. Testicular microlithiasis is an uncommon incidental finding identified during sonographic examination for evaluation of scrotal abnormalities.1 It can be found in pediatric patients of all ages, but it is rare in patients under 2 years of age.2 These densities are thought to originate from the degeneration of epithelial cells in the seminiferous tubules or from Sertoli cell dysfunction due to abnormal gonadal development.3,4
Our patient had classic microlithiasis, which is defined as > 5 microprecipitates measuring 1 to 3 mm in diameter in at least one sonographic plane of a testicle.5 Fewer than 5 microliths on a single image is considered limited testicular microlithiasis.6 The prevalence of testicular microlithiasis ranges between 0.6% and 9% in patients referred for scrotal ultrasonography.7,8
Testicular microlithiasis is more common in patients with other testicular pathologies, including cryptorchidism, varicocele, pseudohermaphroditism, germ cell tumors, and infertility. The condition is also more common in patients with Down or Klinefelter syndromes.1,9-12 Testicular microlithiases occur in up to 50% of patients with cryptorchidism and up to 40% in patients with germ cell tumors.13 They have also been associated with similar calcifications in other anatomic locations, including the lungs and the central nervous system.14
Testicular microlithiasis may also be linked to an increased risk of testicular malignancy as well as an increased frequency of infertility.15-17 Microliths are more common in testes with cancer than in those without malignant pathology, and, although it is debatable if testicular microlithiasis is an independent risk factor for testicular cancer, it is generally accepted that there is an increased risk of testicular cancer in patients with proven testicular microlithiasis.7,17-19 The most commonly reported testicular cancer subtypes reported in patients with confirmed testicular microlithiasis include seminomas, teratomas, and mixed germ cell tumors.20 Although the exact incidence of testicular malignancies seen in patients with testicular microlithiasis is unknown, one literature review and meta-analysis showed there was a significantly increased risk of testicular germ cell tumors or germ cell neoplasia in situ in men with proven testicular microlithiasis compared with those in whom testicular microlithiasis was not found.21
Epididymal cysts. Epididymal cysts are benign, painless cysts of the epididymal head and, similarly to testicular microlithiasis, are usually diagnosed during sonographic evaluation for other testicular pathologies.22 Epididymal cysts occur in 5% to 20% in the pediatric population.23-25 Although the etiology of these cysts is unknown, they may result from congenital anomalies related to hormonal dysfunction during embryogenesis or from epididymal duct obstruction.25-29 On examination, epididymal cysts can be solitary or multiple and present as fluctuant, firm testicular swellings that are easily distinguishable from the testicle.24 Conservative treatment with clinical and ultrasonography monitoring is recommended for asymptomatic patients. Surgical treatment is reserved for patients with large or symptomatic epididymal cysts.25,28-30
CONCLUSION
A genitourinary examination should be part of every well child or adolescent visit, even in patients without complaints. The etiology of our patient’s enlarged scrotum was unclear but was unlikely related to the epididymal cysts or testicular microlithiasis. It is also unclear whether serial physical examinations and ultrasonography are beneficial.31 In the case of microliths, follow-up recommendations can be based on past medical history if the patient has a high risk for testicular cancer due to other factors, such as undescended tests, infertility, testicular atrophy, and contralateral testicular cancer. In addition, regular testicular self-examination is recommended for all patients diagnosed with testicular microlithiasis or epididymal cysts.n
Hunter Nolen, BS; Vikas Gupta, BS; and Micah Gibson, BS, are from the John P. and Kathrine G. McGovern Medical School at University of Texas Health Science Center in Houston.
Lynnette Mazur, MD, MPH, is a Professor of Pediatrics at the John P. and Kathrine G. McGovern Medical School at University of Texas Health Science Center in Houston.
REFERENCES
1. Furness PD III, Husmann DA, Brock JW III, et al. Multi-institutional study of testicular microlithiasis in childhood: a benign or premalignant condition? J Urol. 1998;160(3 Pt 2):1151-1154.
2. Cooper ML, Kaefer M, Fan R, Rink RC, Jennings SG, Karmazyn B. Testicular microlithiasis in children and associated testicular cancer. Radiology. 2014;270(3):857-863.
3. Vegni-Talluri M, Bigliardi E, Vanni MG, Tota G. Testicular microliths: their origin and structure. J Urol. 1980;124(1):105-107.
4. Drut R, Drut RM. Testicular microlithiasis: histologic and immunohistochemical findings in 11 pediatric cases. Pediatr Dev Pathol. 2002;5(6):544-550.
5. Bennett HF, Middleton WD, Bullock AD, Teefey SA. Testicular microlithiasis: US follow-up. Radiology. 2001;218(2):359-363.
6. Bullock AD, Bennett HF, Middleton WD, Teefey JA, Basler JW. Sonographic follow-up of patients with testicular microlithiasis. J Urol. 1998;159 (Suppl):316.
7. Bach AM, Hann LE, Shi WT, et al. Testicular microlithiasis: what is its association with testicular cancer? Radiology. 2001;220(1):70-75.
8. Höbarth K, Susani M, Szabo N, Kratzik C. Incidence of testicular microlithiasis. Urology. 1992;40(5):464-467.
9. Guzmán Martínez-Valls PL, Hita Villaplana G, Fernández Aparicio T, Miñana López B, Martínez Díaz F, Sánchez Gascon F. Significance and management of testicular microlithiasis. Archivos Espanoles de Urologia. 2003;56(5):472–477.
10. Thomas K, Wood SJ, Thompson AJ, Pilling D, Lewis-Jone DI. The incidence and significance of testicular microlithiasis in a subfertile population. Br J Radiol. 2000;73(869):494-497.
11. Ganem JP, Workman KR, Shaban SF. Testicular microlithiasis is associated with testicular pathology. Urology. 1999; 53(1): 209-213.
12. Rashid HH, Cos LR, Weinberg E, Messing EM. Testicular microlithiasis: a review and its association with testicular cancer. Urol Oncol. 2004;22(4):285-289.
13. Renshaw A. Testicular calcifications: incidence, histology and proposed pathological criteria for testicular microlithiasis. J Urol. 1998;160(5):1625-1628.
14. Coetzee T. Pulmonary alveolar microlithiasis with involvement of the sympathetic nervous system and gonads. Thorax. 1970;25(5):637-642.
15 Peterson AC, Bauman JM, Light DE, McMann LP, Costabile RA. The prevalence of testicular microlithiasis in an asymptomatic population of men 18 to 35 years old. J Urol. 2001;166(6):2061-2064.
16. Aizenstein R, DiDomenico D, Wilbur A, O’Neil H. Testicular microlithiasis: association with male infertility. J Clin Ultrasound. 1998;26(4):195-198.
17. Ringdahl E, Claybrook K, Teague L, Northrup M. Testicular microlithiasis and its relation to testicular cancer on ultrasound findings of symptomatic men. J Urol. 2004;172(5):1904-1906.
18. Schjerling L, Kvist E, Rasmussen SG, Wåhlin AB. Testicular microlithiasis: are biopsy and follow-up necessary? Ugeskrift for Laeger. 2002;164 (15):2041-2045.
19. Lam DL, Gerscovich EO, Kuo MC, McGahan JP. Testicular microlithiasis: our experience of 10 years. J Ultrasound Med. 2007;26(7):867-873.
20. Yee WS, Kim YS, Kim SJ, Choi JB, Kim SI, Ahn HS. Testicular microlithiasis: prevalence and clinical significance in a population referred for scrotal ultrasonography. Korean Urol. 2011;52(3):172-177.
21.Tan IB, Ang KK, Ching BC, et al. Testicular microlithiasis predicts concurrent testicular germ cell tumors and intratubular germ cell neoplasia of unclassified type in adults: a meta-analysis and systematic review. Cancer. 2010;116(9):4520-4532.
22. Posey ZQ, Ahn HJ, Junewick J, Chen JJ, Steinhardt GF. Rate and associations of epididymal cysts on pediatric scrotal ultrasound. J Urol. 2010;184(4 suppl):1739-1742.
23. Finkelstein MS, Rosenberg HK, Snyder HM 3rd, et al. Ultrasound evaluation of scrotum in pediatrics. Urology. 1986;27(1):1-9.
24. Rifkin MD, Kurt AB, Goldberg BB. Epididymis examined by ultrasound. Correlation with pathology. Radiology. 1984;151(1):187-190.
25. Niedzielski J, Miodek M, Krakós M. Epididymal cysts in childhood - conservative or surgical approach? Pol Przegl Chir. 2012;84(8):406-410.
26. Atanassova N, McKinnell C, Turner KJ, et al. Comparative effects of neonatal exposure of male rats to potent and weak (environmental) estrogens on spermatogenesis at puberty and the relationship to adult testis size and fertility: evidence for stimulatory effects of low estrogen levels. Endocrinology. 2000;141(10):3898-3907.
27. Bibbo M, Al-Naqeeb M, Baccerini I, et al. Follow-up study of male and female offspring of DES-related mothers: a preliminary report. J Reprod Med. 1975;15(1):29-32.
28. Homayoon K, Suhre CD, Steinhardt GF. Epididymal cysts in children: natural history. J Urol. 2004;171(3):1274-1276.
29. Chillon SF, Dominguez HC, Serrano DA, et al. Epididymal cysts in childhood. Arch Esp Urol. 2005;58(4):325-328.
30. Tanski S, Garfunkel LC, Duncan PM, Weitzman M, eds. Performing Preventive Services: A Bright Futures Handbook. 1st ed. Elk Grove Village, IL: American Academy of Pediatrics; 2010.
31. Jaganathan K, Ahmed S, Henderson A, Rane A. Current management strategies for testicular microlithiasis. Nat Clin Pract Urol. 2007;4(9):492-497.


