A Teenaged Girl With an Itchy, Papulonodular Eruption on the Feet
A 15-year-old girl presented with an intensely pruritic, papulonodular eruption on the dorsa of the feet of 2 months’ duration. Seven months earlier, she had been diagnosed with scabies affecting the feet and legs, for which she was treated with 5% permethrin cream. The patient had atopic dermatitis and allergic rhinitis. She had no history of psychiatric conditions. There was no family history of similar skin lesions.
Physical examination revealed numerous symmetrically distributed papulonodules on the dorsal aspect of both feet. The papulonodules measured 3 mm to 8 mm. Some of the lesions were excoriated and lichenified. The rest of the physical examination findings were normal.

What’s your diagnosis?
(Answer and discussion on next page)
Answer: Prurigo nodularis
Prurigo (derived from the Latin word prurire, “to itch”) nodularis, also known as prurigo nodularis of Hyde or nodular prurigo, is characterized by intensely pruritic, lichenified or excoriated papulonodules that occur chiefly on the anterior surfaces of the lower extremities. Hardaway first described the condition in 1880.1 The term prurigo nodularis was coined by Hyde in 1909.2
EPIDEMIOLOGY
The prevalence of prurigo nodularis is not known. The condition occurs at all ages, although most patients are between 20 and 60 years of age.3,4 Patients with an atopic diathesis have a significantly much earlier age of onset.3-5 The sex incidence is approximately equal.4-6 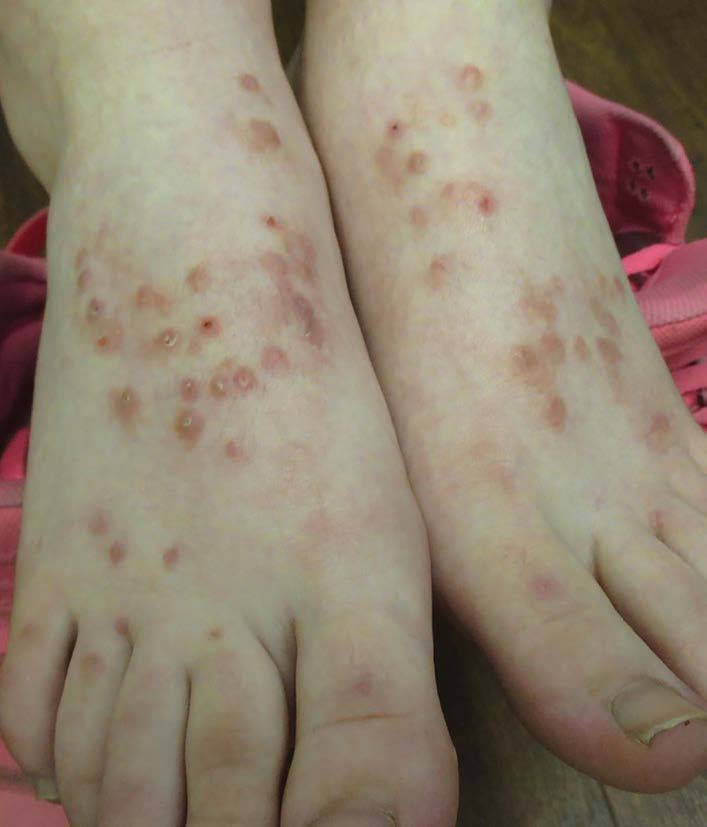
ETIOLOGY AND PATHOGENESIS
Recent evidence suggests that prurigo nodularis is a secondary complication of chronic pruritus, which may be the result of numerous dermatologic or systemic diseases. Dermatologic diseases include atopic dermatitis, contact dermatitis, nummular eczema, scabies, lichen planus, psoriasis, xerosis, and bullous pemphigoid.7 Atopic predisposition is a major factor in approximately 50% of patients with prurigo nodularis.7 Systemic diseases associated with prurigo nodularis include hepatic dysfunction, thyroid dysfunction, chronic renal failure, polycythemia rubra vera, diabetes mellitus, gluten enteropathy, malignancy (eg, lymphoma, leukemia, gastrointestinal carcinomas), infections (eg, HIV, mycobacteria, hepatitis B virus, hepatitis C virus), parasitic infestation, and psychosocial disorders (eg, emotional stress, depression, anxiety).7-9
It is generally believed that chronic mechanical scratching and/or rubbing as a result of pruritus leads to the development of papulonodular or plaque-like lesions that may become excoriated, crusted, and lichenified.3 Nerve growth factor, substance P, calcitonin gene-related peptide, mast cells, and type 2 helper T cell cytokines play an important in the cutaneous neurogenic inflammation and pruritic response of the skin in prurigo nodularis.4,6
HISTOPATHOLOGY
Histologic features include thick, compact orthohyperkeratosis, folliculosebaceous units in nonvolar skin in conjunction with a thick and compact cornified layer like that of volar skin (hairy palm sign); irregular epidermal hyperplasia or pseudoepitheliomatous hyperplasia; focal parakeratosis with irregular acanthosis; hypergranulosis; fibrosis of the papillary dermis with vertically arranged collagen fibers; and a superficial perivascular and/or interstitial inflammatory infiltrate of lymphocytes, macrophages, eosinophils, and neutrophils.6,10
CLINICAL MANIFESTATIONS
Patients with prurigo nodularis often present with a long-standing history of severe, unremitting pruritus in the affected area, followed by the appearance of pruritic papulonodules.3 Clinically, prurigo nodularis presents with multiple, intensely pruritic, firm, hyperkeratotic, dome-shaped papules and/or nodules that are found mostly on the extensor surfaces of the extremities. The lesions can be flesh-colored, erythematous, or brown-violaceous.
There is a tendency for symmetric distribution. A linear arrangement of lesions is common. The individual lesions usually are 0.2 to 2 cm in diameter.4,10 Some of the lesions may be excoriated, crusted, or lichenified. Lichenoid plaques are also a frequent finding. The face, palms, and soles are rarely affected.4 The mid-back often is spared because it is difficult to reach, a pattern known as the “butterfly sign.”4,7
Pruritus usually is severe and confined to the lesions themselves. It can be paroxysmal or continuous and is worsened by heat or sweating.6 The number of lesions may vary from a few to hundreds.6 New lesions may develop from time to time, while some existing lesions occasionally may regress spontaneously. The skin between the lesions usually is normal but can be xerotic or lichenified.
DIAGNOSIS
The diagnosis is mainly clinical, based on a history of chronic pruritus and the physical finding of the characteristic excoriated, symmetrically distributed, papulonodular lesions. A skin biopsy should be performed if the diagnosis is in doubt.
Laboratory investigations should be directed by the history and physical examination findings to rule out underlying associations. Laboratory tests to be considered whenever appropriate include complete blood cell count, total serum IgE level, liver function tests, renal function tests, thyroid function tests, hepatitis serology, HIV serology, and chest radiography, among others. Testing a scraping for scabies should be considered if the history is relevant.
DIFFERENTIAL DIAGNOSIS
Differential diagnosis includes pemphigus nodularis, hypertrophic lichen planus, lichen simplex chronicus, nodular scabies, mastocytosis, keratoacanthomas, dermatofibromas, cutaneous T-cell lymphoma, and epidermolysis bullosa pruriginosa.4,6
COMPLICATIONS
Prurigo nodularis is a distressing condition that has a significant negative impact on the quality of life due to the severe pruritus and chronic, persistent, visible skin lesions.7 Intensive pruritus may cause insomnia and difficulty concentrating. Skin excoriation may lead to secondary infection. Postinflammatory hypopigmentation or hyperpigmentation may result.4
PROGNOSIS
Although the disease is benign, it tends to run a protracted course with exacerbations and remissions.
MANAGEMENT
The sensation of itch often is relieved by scratching. However, the first scratch initiates the second itch, and this may become a vicious cycle. As such, it is important to break the itch-scratch-itch cycle. Any underlying cause of pruritus should be treated if possible. Oral antihistamines can provide symptomatic relief because of their sedative properties and may be effective for the pruritus. Of the H1 antihistamines, hydroxyzine is more effective than diphenhydramine and cyproheptadine.
To avoid injury to the skin from scratching, fingernails should be kept short, smooth, and clean. Gloves occasionally are necessary to control scratching while sleeping.
Prurigo nodularis is notoriously difficult to treat. Referral to a dermatologist always should be a consideration. Treatment options include topical ultrapotent corticosteroids, topical immunomodulators (ie, tacrolimus and pimecrolimus), topical capsaicin, liquid nitrogen cryotherapy, intralesional corticosteroids, oral pregabalin, oral gabapentin, oral naltrexone, oral thalidomide, oral cyclosporine, oral methotrexate, narrow-band ultraviolet B (NB-UVB) therapy, and phototherapy with psoralen plus ultraviolet A (PUVA).9,11 Unfortunately, evidence about their efficacy from randomized controlled trials is limited.
The present consensus is that topical ultrapotent corticosteroids are the mainstay of therapy for those with a limited number of small papulonodular lesions.6 These can be used in conjunction with an occlusive dressing to enhance penetration and to protect against scratching.4 Tacrolimus and pimecrolimus are not as fast or effective as topical ultrapotent corticosteroids in the treatment of this skin condition, although they can be considered in the maintenance phase of treatment.
For patients with a limited number of large nodular lesions, intralesional corticosteroids may be considered.6 NB-UVB therapy and PUVA may be considered for patients with widespread disease or patients who do not respond to topical or intralesional corticosteroids.6
For recalcitrant and severe cases unresponsive to these measures, immunosuppressants such as cyclosporine and methotrexate have occasionally been used, with variable success. These immunosuppressants have potential adverse effects, requiring therapy to be carefully monitored and thus restricting their clinical usefulness.
Alexander K. C. Leung, MD, is a clinical professor of pediatrics at the University of Calgary and a pediatric consultant at the Alberta Children’s Hospital in Calgary.
Benjamin Barankin, MD, is medical director and founder of the Toronto Dermatology Centre.
REFERENCES
1. Hardaway WA. Case of multiple tumor of the skin accompanied by intense pruritus. Arch Dermatol. January 1880;6:129-132.
2. Hyde JN. Prurigo nodularis. In: Hyde JN, ed. A Practical Treatise on Diseases of the Skin for the Use of Students and Practitioners. 8th ed. Philadelphia, PA: Lea and Febiger; 1909:174-175.
3. Amer A, Fischer H. Prurigo nodularis in a 9-year-old girl. Clin Pediatr (Phila). 2009;48(1):93-95.
4. Vaidya DC, Schwartz RA. Prurigo nodularis: a benign dermatosis derived from a persistent pruritus. Acta Dermatovenerol Croat. 2008;16(1):38-44.
5. Tan WS, Tey HL. Extensive prurigo nodularis: characterization and etiology. Dermatology. 2014;228(3):276-280.
6. Watsky K. Prurigo nodularis. UpToDate. http://www.uptodate.com/contents/prurigo-nodularis. Updated July 17, 2014. Accessed September 24, 2014.
7. Iking A, Grundmann S, Chatzigeorgakidis E, Phan NQ, Klein D, Ständer S. Prurigo as a symptom of atopic and non-atopic diseases: aetiological survey in a consecutive cohort of 108 patients. J Eur Acad Dermatol Venereol. 2013;27(5):550-557.
8. Dazzi C, Erma D, Piccinno R, Veraldi S, Caccialanza M. Psychological factors involved in prurigo nodularis: a pilot study. J Dermatolog Treat. 2011;22(4):211-214.
9. Fostini AC, Girolomoni G, Tessari G. Prurigo nodularis: an update on etiopathogenesis and therapy. J Dermatolog Treat. 2013;24(6):458-462.
10. Weigelt N, Metze D, Ständer S. Prurigo nodularis: systematic analysis of 58 histological criteria in 136 patients. J Cutan Pathol. 2010:37(5):578-586.
11. Gencoglan G, Inanir I, Gunduz K. Therapeutic hotline: treatment of prurigo nodularis and lichen simplex chronicus with gabapentin. Dermatol Ther. 2010;23(2):194-198.


