Rectoperineal Fistula With Imperforate Anus
A 1-month-old boy presented with a 1-day history of fussiness, decreased feeding, and fever. He had been delivered at full term and was healthy, aside from 1 week of observation in a neonatal intensive care (NICU) for difficulty breathing and hyperbilirubinemia, the latter of which had required phototherapy.
After discharge from the NICU at 2 weeks of age, he had developed a fever related to urinary tract infection (UTI) with Enterococcus faecalis and had been treated with 10 days of intravenous ampicillin at a different facility. Seven days after that hospitalization, he presented to our emergency department with new-onset fever. He had no vomiting, lethargy, or upper respiratory symptoms. A history revealed chronic constipation that his parents described as straining with stools.
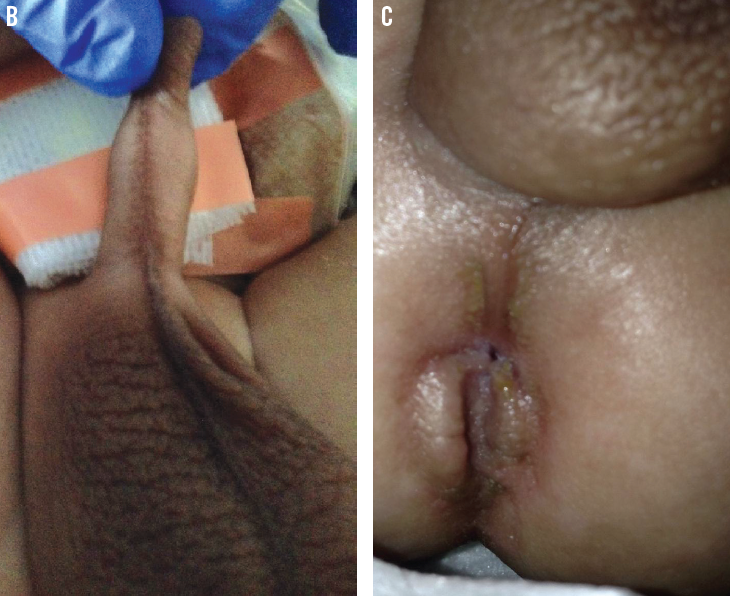
On physical examination, the patient had a temperature of 38.2°C, heart rate of 140 beats/min, respiratory rate of 35 breaths/min, and blood pressure of 87/47 mm Hg. Bilateral polythelia on the midclavicular line, abdominal distension (A), a hyperpigmented perineal raphe (B), and an abnormal opening anterior to imperforate anal sphincter musculature (C) were noted.
Results of urine microscopy from in-and-out catheterization showed pyuria (20-50 white blood cells per high-power field), and urinalysis was significant for occult blood, protein, large leukocyte esterase, and no nitrites. He was admitted and placed on intravenous broad-spectrum antibiotics for his second UTI and out of concern for sepsis.

Blood and cerebrospinal fluid culture results were negative; however, his urine again grew ampicillin-susceptible E faecalis. Specialists in urology, pediatric surgery, and genetics were consulted due to the abnormalities noted on physical examination and the recurrent UTI. A renal ultrasonogram showed moderate bilateral pyelectasis, an enlarged right kidney and ureter, and a dilated bladder. A voiding cystourethrogram showed grade 5 vesicoureteral reflux.
The boy received a diagnosis of anorectal malformation (ARM), specifically rectoperineal fistula with imperforate anus, and he underwent diverting colostomy. To screen for defects and genetic syndromes associated with ARM, further evaluations (echocardiography, repeat hearing screen, ophthalmology consult, spinal ultrasonography, skeletal radiography, magnetic resonance imaging of the brain, upper gastrointestinal radiography with barium swallow, chromosomal breakage analysis, DNA microarray analysis) were performed, and all results were normal.
ARM represents a spectrum of anomalies that involve the distal anus, the rectum, and the genitourinary tract. ARM occurs in approximately 1 in 5,000 live births.1 The diagnosis of ARM often is missed prenatally because fluid is resorbed in intestinal loops, leaving no obvious distension on fetal ultrasonography despite distal obstruction. As with this patient’s case, a perineal fistula may be mistaken for a normal anus on physical examination after birth.1
Rectoperineal fistulas involve the rectum opening into a small orifice, typically located anterior to the anal sphincter. Patients with such fistulas usually have preserved sphincter mechanisms and a normal sacrum. Fistulas also can form between the rectal and urinary anatomy, leading to recurrent UTIs. The presence or absence of fistulas, the severity of obstruction, and the number of organ systems involved help determine whether surgeons choose to directly repair the defects in infancy or perform diverting colostomy with later correction.
ARM can be an isolated finding but is associated with genitourinary defects, which occur in approximately 50% of all patients with anorectal malformations,2 and sacral and spinal cord anomalies, including tethered cord.3 ARM also can be seen with trisomy 21, VACTERL association (vertebral defects, anal atresia, cardiac defects, tracheoesophageal fistula, renal anomalies, and limb abnormalities), and numerous other genetic disorders. Screening for associated defects and syndromes after the diagnosis of ARM is recommended.3
Some reports have linked the presence of extra nipples with urogenital anomalies. However, patients with polythelia who are otherwise healthy do not need routine urologic imaging.2
References
1. Kim HLN, Gow KW, Penner JG, Blair GK, Murphy JJ, Webber EM. Presentation of low anorectal malformations beyond the neonatal period. Pediatrics. 2000;105(5):e68.
2. Brown J, Schwartz RA. Supernumerary nipples: an overview. Cutis. 2003; 71(5):344-346.
3. Levitt MA, Peña A. Anorectal malformations. Orphanet J Rare Dis. 2007;2:33.


