Primary Epiploic Appendagitis
For the past 24 hours, a 15-year-old girl had localized abdominal pain (10 on a scale of 10) that was sharp and nonradiating. Her bowel movements had been normal. She was afebrile on presentation to the emergency department. She denied vomiting or diarrhea.
On examination, she had borderline tachycardia (heart rate, 95 beats per minute). Other vital signs were normal. She had tenderness and rebound of the right lower quadrant, with no rigidity or organomegaly, and normal bowel sounds.
Results of a urine pregnancy test were negative. A complete blood count showed leukocytosis (17,100 white blood cells/µL, with 78% neutrophils). A chemistry profile and urinalysis yielded normal results.
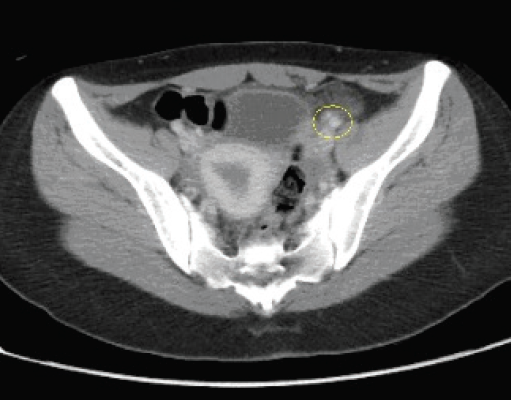
An abdominal computed tomography (CT) scan with oral and intravenous contrast showed a normal appendix, with stranding of retroperitoneal fat adjacent to the sigmoid colon and the proximal ileum representing epiploic appendagitis (Figure). The patient was admitted for conservative management with analgesics; within 2 days, her pain had resolved and she was discharged.
Primary epiploic appendagitis (PEA) is a rare disease characterized by inflammation of the epiploic appendages caused by spontaneous torsion or venous thrombosis of an appendage.1-4 In contrast, secondary epiploic appendagitis is caused by inflammatory or infectious processes in adjacent areas.
The incidence of PEA is low, especially in the pediatric population.5 Physical examination findings are nonspecific. The most common finding is localized tenderness in the right or left lower quadrant, with occasional rebound tenderness but no rigidity.3,5-7 Other associated symptoms include nausea, vomiting, high fever (temperature above 39°C [102.2°F]), and anorexia.5 Leukocytosis is another reported finding in PEA.5
The differential diagnosis of acute abdominal pain is vast and includes appendicitis, diverticulitis, cholecystitis, ovarian torsion, ectopic pregnancy, and mesenteric lymphadenitis. The radiologic differential diagnosis includes acute abdomen.8
Diagnosis most commonly is with ultrasonography or CT, with the latter being the preferred modality.9 In normal conditions, epiploic appendages are not visible on a CT scan. The characteristic CT finding is a small adipose mass (usually less than 5 cm) surrounded by a hyperdense rim adjacent to the colon.5
Almost all cases of PEA are putatively diagnosed as appendicitis or diverticulitis.5 In the past, the condition often had been misdiagnosed as acute abdomen, occasionally resulting in unnecessary surgery.6,7,10,11 With advances in radiology and established radiologic findings, PEA now is diagnosed more frequently.
Overall awareness of the entity still is low among surgeons.5 PEA is a self-limited disease that generally resolves spontaneously.12 Most patients recover with conservative management.6,9,12,13
REFERENCES:
1. Carmichael DH, Organ CH Jr. Epiploic disorders: conditions of the epiploic appendages. Arch Surg. 1985;120(10):1167-1172.
2. Dockerty MB, Lynn TE, Waugh JM. A clinicopathologic study of the epiploic appendages. Surg Gynecol Obstet. 1956;103(4):423-433.
3. Thomas JH, Rosato FE, Patterson LT. Epiploic appendagitis. Surg Gynecol Obstet. 1974;138(1):23-25.
4. Fieber SS, Forman J. Appendices epiploicae: clinical and pathological considerations; report of three cases and statistical analysis on one hundred five cases. AMA Arch Surg. 1953;66(3):329-338.
5. Choi YU, Choi PW, Park YH, et al. Clinical characteristics of primary epiploic appendagitis. J Korean Soc Coloproctol. 2011;27(3):114-121.
6. Legome EL, Belton AL, Murray RE, Rao PM, Novelline RA. Epiploic appendagitis: the emergency department presentation. J Emerg Med. 2002;22(1):9-13.
7. Rioux M, Langis P. Primary epiploic appendagitis: clinical, US, and CT findings in 14 cases. Radiology. 1994;191(2):523-526.
8. Danielson K, Chernin MM, Amberg JR, Goff S, Durham JR. Epiploic appendicitis: CT characteristics. J Comput Assist Tomogr. 1986;10(1):142-143.
9. Hiller N, Berelowitz D, Hadas-Halpern I. Primary epiploic appendagitis: clinical and radiological manifestations. Isr Med Assoc J. 2000;2(12):896-898.
10.Desai HP, Tripodi J, Gold BM, Burakoff R. Infarction of an epiploic appendage: review of the literature. J Clin Gastroenterol. 1993;16(4):323-325.
11. Shehan JJ, Organ C, Sullivan JF. Infarction of the appendices epiploicae. Am J Gastroenterol. 1966;46(6):469-476.
12. Epstein LI, Lempke RE. Primary idiopathic segmental infarction of the greater omentum: case report and collective review of the literature. Ann Surg. 1968;167(3):437-443.
13. Son HJ, Lee SJ, Lee JH, et al. Clinical diagnosis of primary epiploic appendagitis: differentiation from acute diverticulitis. J Clin Gastroenterol. 2002;34(4):435-438.


