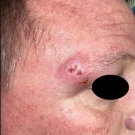
A Pregnant Woman Presents With a Red Nodule on Her Finger
History
A 28-year-old Caucasian woman, who at 28 weeks gestation, presented with a red nodule on the left index finger. The lesion was asymptomatic and was first noted 6 weeks ago. The mass was rapidly increasing in size and bled on 1 occasion. Her maternal health was unremarkable. There was no history of trauma and she was not on any medication. This was her second pregnancy and no similar lesion occurred with her first pregnancy.

Physical Examination
Physical examination revealed a soft, reddish, dome-shaped nodule with a smooth surface on the left index finger. Examination of the oral cavity, nostrils, and ears was unremarkable.
What’s Your Diagnosis?
A. Bacillary angiomatosis
B. Granuloma gravidarum
C. Verruga peruana
D. Cherry angioma
(Answer and discussion on next page)
Answer: Granuloma gravidarum
Based on the history and physical examination, a diagnosis of granuloma gravidarum was made. Granuloma gravidarum, granuloma of pregnancy, epulis gravidarum, and pregnancy tumor are terms used to describe pyogenic granuloma that occur during pregnancy.1
Epidemiology
Granuloma gravidarum especially on the gingiva, occurs in approximately 2% to 5% of pregnancies, usually in the second or third trimester.2 In this setting, it is often referred to as epulis gravidarum. Granuloma gravidarum occurs exclusively in pregnant females.
Etiopathogenesis
During pregnancy, levels of estrogens and progesterone are markedly elevated. It is believed that these hormones enhance expression of angiogenic factors—such as basic fibroblast growth factor and vascular endothelial growth factor—which will lead to evolution of the pyogenic granuloma.3 A hormone-related exaggerated response to trauma, local irritation, and poor oral hygiene may also play a role.
Histopathology
Histologically, the lesion has a characteristic lobular proliferation of capillaries within a network of fibrovascular tissue at the base, typically accompanied by a mixture of infiltrated inflammatory cells.2,4 In those lesions that are undergoing regression, there may be extensive fibrosis.
Clinical Manifestations
Granuloma gravidarum affects mainly the gingival mucosa, followed by the lips, tongue, and buccal mucosa.5,6 Lesions are slightly more common on the maxillary gingiva than the mandibular gingiva, anterior areas than posterior areas, and facial aspect of the gingiva than the lingual or palatal aspect.2,6 Cutaneous lesions may also occur, as is illustrated in the present case.7 Nasal lesions are rare and generally arise from the nasal septum and/or from turbinates on the roof of the nasal cavity, or in the maxillary sinus.8
Clinically, granuloma gravidarum presents as a painless, soft, dome-shaped papule/nodule or a sessile or pedunculated polypoid growth with a smooth, glistening, erosive, or friable surface.1,9 The color varies from bright red, dusky red, to pink, depending on the vascularity of the growth. The lesion grows rapidly and bleeds easily. Patients often cover the lesions with a bandage to prevent rubbing or trauma, and thus bleeding—often termed the “band-aid” sign.
Diagnosis
The diagnosis is mainly clinical and should be considered if any fleshy mass is found in the oral cavity, nasal cavity, ear, or on the skin of a gravid woman, particularly if it has bled and is growing quickly. Dermoscopy of the lesion reveals red homogenous areas (proliferating vessels) and a white scaly collarette (hyperplastic epithelium).10
Dermoscopy, typically performed by dermatologists, increases the diagnostic accuracy and has been shown to be a very useful tool to evaluate granuloma gravidarum.10 However, dermoscopy is not a substitute for histology, a biopsy is warranted if the diagnosis is in doubt (eg, to rule out amelanotic melanoma).
Differential Diagnosis
Granuloma gravidarum should be differentiated from bacillary angiomatosis (disseminated vascular lesions in immunocompromised individuals) and verruga peruana (crops of vascular nodules in immunocompetent individuals) caused by infection with Bartonella species, though rare in North America.11
Other more common differential diagnoses include pedunculated cherry angioma, granulation tissue, infantile hemangioma, venous lake, glomus tumor, acquired digital fibrokeratoma, amelanotic melanoma, hyperplastic gingival inflammation, peripheral giant cell granuloma, peripheral ossifying fibroma, Spitz nevus, proliferating pilomatricoma, Kaposi’s sarcoma, and angiosarcoma.1
Complications
Granuloma gravidarum tends to bleed and ulcerate.7 An ulcerated lesion is prone to infection especially in the oral cavity.8 The lesion can be unsightly and cosmetically disfiguring, especially if it occurs on the face.
Prognosis
The prognosis is good; many cases resolve spontaneously after childbirth.
Management
If the lesion is small and asymptomatic, a watchful observation is reasonable. Indications for active intervention include severe or recurrent hemorrhage unresponsive to treatment, threatening ulceration in areas where serious complications might ensue, interference with vital structures, life- or function-threatening complications, and significant disfigurement.5 Surgical excision with linear closure allows histologic examination of the tissue.9 Complete surgical excision also has the lowest rate of recurrence and is therefore the treatment of choice.4
Other treatment modalities include laser surgery, electrodessication, curettage, liquid nitrogen cryotherapy, sclerotherapy, topical silver nitrate, and topical imiquimod.4,12 Most commonly, patients are referred to a dermatologist for diagnostic confirmation and/or treatment. While watchful waiting is often advised and treatment performed after the childbirth, some patients prefer to have the lesion removed promptly so as not to interfere with their lives.
Outcome of the Case
This patient was reassured of the benign nature of the condition and that the lesion would regress after the baby was born. She delivered a baby at 38 weeks gestation via Cesarean section for fetal distress. After delivery, there was a steady reduction in the size of the lesion. At 6 months follow-up, the lesion had completely resolved.
Alexander K.C. Leung, MD, is a clinical professor of pediatrics at the University of Calgary and pediatric consultant at the Alberta Children’s Hospital in Calgary, Alberta, Canada.
Benjamin Barankin, MD, is the medical director and founder of the Toronto Dermatology Centre in Toronto, Ontario, Canada.
References:
1. Leung AK, Barankin B, Hon KL. Pyogenic granuloma. Clin Mother Clid Health. [in press].
2. Silva-Sousa YT, Coelho CM, Brentegani LG, et al. Clinical and histological evaluation of granuloma gravidarum: case report. Braz Dent J. 2000;11:135-139.
3. Andrikopoulou M, Chatzistamou I, Gkilas H, et al. Assessment of angiogenic markers and female sex hormone receptors in pregnancy tumor of the gingiva. J Oral Maxillofac Surg. 2013;71:1376-1381.
4. Ting PT, Barankin B. Pyogenic granuloma. Can Fam Physician. 2006;52:35-36.
5. Cardoso JA, Spanemberg JC, Cherubin K, et al. Oral granuloma gravidarum: a retrospective study of 41 cases in Southern Brazil. J Appl Oral Sci. 2013;
21:215-218.
6. Cruz LE, Martos J. Granuloma gravidarum (pyogenic granuloma ) treated with periodontal plastic surgery. Int J Gynaecol Obstret. 2010;109:73-74.
7. Rader C, Piorkowski J, Bass DM, et al. Epulis gravidarum manum: pyogenic granuloma of the hand occurring in pregnant women. J Hand Surg. 2008;
33A:263-265.
8. Patil P, Singla S, Mane R, et al. Nasal lobular capillary hemangioma. J Clin Imaging Sci. 2013;3:40.
9. Leung AK. Pyogenic granuloma. In: Leung AK, ed. Common Problems in Ambulatory Pediatrics: Specific Clinical Problems. Vol 2. New York: Nova Science Publishers, Inc.; 2011;143-147.
10. Zaballoos P, Carulla M, Ozdemir F, et al. Dermoscopy of pyogenic granuloma: a morphology study. Br J Dermatol. 2010;
163:1229-1237.
11. Al-Thunayan A, Al-Rehaili M, Al-Meshai O, et al. Bacillary angiomatosis presenting as a pyogenic granuloma of the hand in an otherwise apparently healthy patient. Ann Plast Surg. 2013;70:652-653.
12. Musumeci ML, Lacarrubba F, Anfuso R, et al. Two pediatric cases of pyogenic granuloma with imiquimod 5% cream: combined clinical and dermatoscopic evaluation and review of the literature. G Ital Dermatol Venereol. 2013;148:147-152.