Peer Reviewed
Pachyonychia Congenita
AUTHORS:
LaDonna J. Johnson, MD; Hansa Wongprasert, MD; and Mary Mullins
Children’s Hospital of Michigan, Detroit
CITATION:
Johnson LJ, Wongprasert H, Mullins M. Pachyonychia congenita. Consultant for Pediatricians. 2012;12(10):476-477.
An 8-month-old African American girl was brought to the hospital with a 3-day history of a barking cough with associated respiratory distress, rhinorrhea, and decreased oral intake. Her past medical history was significant only for being born via cesarean section at 31 weeks of gestation because of fetal heart deceleration. She has no history of chronic skin infection or rash. Her vaccinations are up to date, and she has reached all developmental milestones normally.
Physical examination findings included mild tachypnea with a respiratory rate of 60 breaths per minute, minimal clear nasal discharge, and inspiratory stridor. Her oxygen saturation was 99% to 100% on room air. An incidental finding was the presence of very thick, dystrophic, yellow to brown fingernails and toenails, without clubbing or cyanosis (A and B). Examination findings were otherwise unremarkable, with no mucosal or skin lesions.


After receiving a diagnosis of viral croup, she was admitted to the hospital for treatment. Her respiratory symptoms improved significantly with treatment, and she was discharged home the next day. At the time of her discharge, we met with the child’s father, who had not been present at the time of admission. Interestingly, the patient’s father has the same characteristic hypertrophic dystrophy of the fingernails and toenails (C), as well as multiple nodular skin lesions along his face and neck. The child’s mother has normal nail and skin texture.
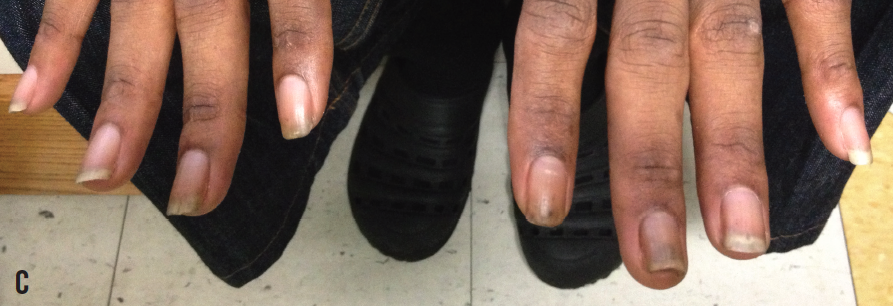
Based on the physical appearance of the child’s fingernails and toenails, and those of her father, the most likely diagnosis for this patient’s condition is pachyonychia congenita, a rare, autosomal dominant disorder caused by mutations of 1 of 4 keratin genes (KRT6A, KRT6B, KRT16, and KRT17).1 A mutation of any of the keratin genes changes the structure of the keratin protein, preventing strong keratin networks from forming within cells. Skin becomes fragile and susceptible to trauma from even mild friction—skin can blister or callus simply as a result of walking. The growth and function of cells in hair follicles and nails also are disrupted by the defective keratin.
Pachyonychia congenita usually becomes apparent in the first few months of life, with hypertrophic nail dystrophy as the primary presenting symptom. Many affected children also develop painful blisters or calluses on the palms and soles, which can lead to delayed walking. Additional features include oral leukoplakia, follicular keratosis, cutaneous cysts, coarse or twisted hair, early primary tooth loss, and the presence of natal or prenatal teeth.2
In this patient, hypertrophic nail dystrophy was the only one of these distinctive features present. Further assessment and follow-up by a dermatologist is important, because this patient may develop other clinical features as she ages. Molecular DNA analysis may be performed to obtain a definitive diagnosis of this patient’s condition.
REFERENCES:
- Smith FJD, Hansen CD, Hull PR, et al. Pachyonychia congenita. In: Pagon RA, Adam MP, Bird TD, et al, eds. GeneReviews. Seattle: University of Washington. http://www.ncbi.nlm.nih.gov/books/NBK1280/. Published January 27, 2006. Updated December 1, 2011. Accessed August 15, 2013.
- Leachman SA, Kaspar RL, Fleckman P, et al. Clinical and pathological features of pachyonychia congenita. J Investig Dermatol Symp Proc. 2005;10(1):3-17.


