Osteochondritis Dissecans of the Knee: Differential Diagnosis, Approaches to Treatment
A 14-year-old girl presented with gradual onset of activity-related left anterior knee pain of 1 year’s duration that had been worsening over the past 3 months. She is a multisport athlete, with cross-country running being her favorite and most symptom-provoking activity. She has no history of acute injury, and she reported no episodes of instability, giving-way, or locking of the knee.
Physical examination revealed a subtle limp but no tenderness to palpation about the left knee. A small joint effusion without warmth was present. Range of motion was normal and without pain in the hip and knee. The left patella tracked normally without crepitus, McMurray test was negative for meniscal injury, and the collateral and cruciate ligaments were stable during stress testing.
Anteroposterior tunnel view (Figure 1A) and lateral view (Figure 1B) radiographs of the left knee were ordered. The films showed a well-demarcated, crescent-shaped lytic lesion of the lateral area of the medial femoral condyle with a sclerotic base.

Figures 1A and 1B – Tunnel view radiograph and lateral radiograph of the left knee showing a crescent-shaped lytic lesion of the lateral area of the medial femoral condyle, the hallmark of osteochondritis dissecans.
DIFFERENTIAL DIAGNOSIS
The appearance and location of this lesion are the classic signs of osteochondritis dissecans (in this case, of the medial femoral condyle) and distinguish it from other conditions of the knee. For example, a distal femoral stress fracture may appear normal on radiographs early, or a subtle radiolucent line near the cortex with periosteal reaction (thickening) may be visible after a few weeks.
In tibial tuberosity osteochondritis (Osgood-Schlatter disease), patients will have swelling, thickening, and tenderness of the tibial tubercle on physical examination. The radiographs usually reveal enlargement and/or fragmentation of the tibial tubercle, which is best seen on lateral radiographic images.
Chronic osteomyelitis can have a variety of radiographic appearances, but our patient’s history was not consistent with this diagnosis.
If an intra-articular loose body is present in the knee and becomes calcified, it can be seen as a radiodense object within the intracapsular joint space and may change location over time on serial radiographs.
PATHOPHYSIOLOGY
Osteochondritis dissecans is a localized condition of the joint, most often occurring before skeletal maturity. The process involves both subchondral bone and articular cartilage. Osteochondritis dissecans lesions most often occur in the knees and are most common among active children between 10 and 15 years of age.1-3
The exact etiology of osteochondritis dissecans remains speculative, but repetitive microtrauma and ischemia are thought to be important contributing factors in most cases.4,5 Repetitive stresses can lead to vascular compromise of a subchondral bone segment; this compromise can result in loss of support of the overlying articular cartilage, leading to softening and subsequent fragmentation of the cartilage.5 If left untreated, these osteochondral lesions can become completely detached (unstable), resulting in a loose body within the joint.
Repetitive microtrauma between the medial femoral condyle and the tibial spine might explain the classic crescent-shaped osteochondritis dissecans lesion seen on the lateral aspect of the medial femoral condyle, which accounts for 70% to 80% of all knee lesions.2,4,5 Bilateral lesions are seen in approximately 20% of cases, suggesting the possibility of a genetic predisposition to osteochondritis dissecans.3
PRESENTATION
The clinical presentation of osteochondritis dissecans is variable and depends on the size, the location, and the stability of the lesion.6 Early in its course, osteochondritis dissecans is an easily missed diagnosis because of the mild, vague presenting symptoms and the often unremarkable physical examination, both of which are scenarios that are similar to other causes of anterior knee pain. Patients with stable lesions often complain of dull, aching anterior knee pain related to physical activity. The insidious onset of pain typically is unrelated to acute trauma and occurs over a period of weeks or months. Mild joint effusion on physical examination occurs in less than 20% of patients.7 Mechanical symptoms of catching, locking, and restricted range of motion usually occur in the more advanced stages as the lesion becomes unstable.1,2,6 The patient may display an antalgic gait and crepitus on knee range of motion.4
IMAGING AND GRADING
The diagnosis of osteochondritis dissecans can be confirmed on plain radiographs.2 A complete knee series, including anteroposterior, lateral, Merchant, and tunnel views, is important. The tunnel or notch view is used to identify posterior femoral condylar lesions, while the Merchant view can identify rare patellar lesions.1,2 Radiographic imaging of the contralateral knee also should be considered because of the possibility of bilateral lesions.1
Once osteochondritis dissecans has been diagnosed using plain radiographs, magnetic resonance imaging is used to define the stability of the lesion and to develop a subsequent treatment plan.1,2,6 Using these imaging studies, osteochondritis dissecans lesions then are graded generally as stable (grades I and II) or unstable (grades III and IV) according to the degree of fragmentation and detachment.6,8
• Grade I lesions show compression injury but no visible fragmentation.
• Grade II lesions have a definable fragment but no detachment of the articular cartilage (Figures 2A and 2B).
• Grade III lesions show complete detachment of the articular cartilage but without displacement.
• Grade IV lesions have complete detachment and displacement, resulting in an intra-articular loose body.

Figures 2A and 2B – Coronal plane and sagittal plane T2-weighted magnetic resonance images showing a grade II medial femoral condyle osteochondritis dissecans lesion, with intact articular cartilage.
MANAGEMENT
Nonoperative management of stable osteochondritis dissecans lesions in skeletally immature patients (ie, open distal femoral physis visible on radiographs) has a high potential for healing. Conservative treatment involves activity modification, bracing, protected weight-bearing, and stopping any activities that reproduce symptoms. A gradual return to full activity is permitted when both the patient is symptom-free and follow-up imaging shows signs of proper healing.6
Conversely, unstable lesions do not heal well with a conservative treatment approach and typically require surgery. Other surgical candidates are patients with stable lesions who have failed
6 months of conservative treatment, and adolescents who have minimal growth remaining.2,4 Surgical goals include enhancing the blood supply to the subchondral bone, stabilizing osteochondral fragments, and restoring normal articular congruency.6
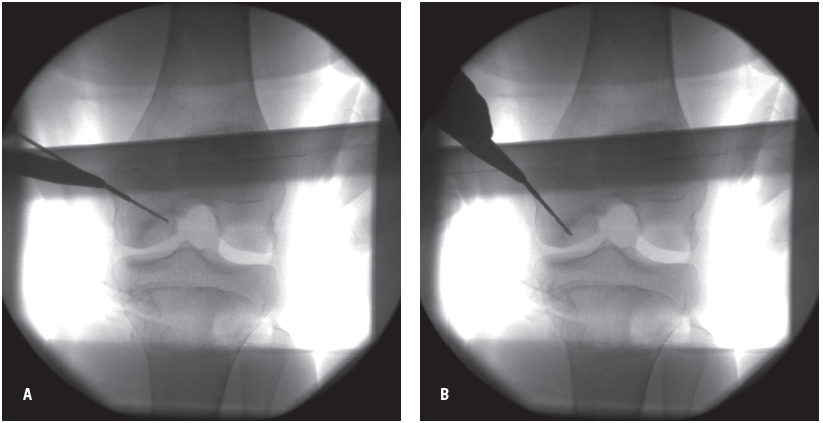
Figures 3A and 3B – Intraoperative fluoroscopic images of antegrade drilling with multiple holes into the osteochondritis dissecans lesion. Care is taken to avoid penetration of the intact articular cartilage and the open growth plate.

Figure 4 – Intraoperative photograph of the right knee showing a hinged grade III osteochondritis dissecans lesion.

Figure 5 – Intraoperative photograph of the right knee during headless subchondral compression screw fixation of osteochondritis dissecans.
For stable lesions requiring surgical intervention, drilling of the osteochondritis dissecans lesion is effective at promoting an intrinsic healing response (Figures 3A and 3B). Using this technique, small channels are drilled into the subchondral bone near the site of the lesion, allowing for the influx of healing elements such as mesenchymal stem cells and growth factors.6,9 Unstable, nondisplaced osteochondral fragments (grade III lesions) often can be stabilized with screw fixation (Figures 4, 5, and 6). Unstable, displaced osteochondral fragments (grade IV lesions) that are not salvageable often require surgical techniques involving osteochondral tissue (autograft or allograft) or autologous chondrocyte implantation.2

Figure 6 – Immediate postoperative anteroposterior radiograph of the right knee following internal screw fixation of osteochondritis dissecans.
REFERENCES:
1. Kodali P, Islam A, Andrish J. Anterior knee pain in the young athlete: diagnosis and treatment. Sports Med Arthrosc. 2011;19(1):27-33.
2. Polousky JD. Juvenile osteochondritis dissecans. Sports Med Arthrosc. 2011;19(1):56-63.
3. Mercier LR. Osteochondritis dissecans. In: Ferri FF, ed. Ferri’s Clinical Advisor 2013. Philadelphia, PA: Elsevier Mosby; 2012:722.
4. Flynn JM, Kocher MS, Ganley TJ. Osteochondritis dissecans of the knee. J Pediatr Orthop. 2004;
24(4):434-443.
5. Lim HC, Bae JH. Meniscoplasty for stable osteochondritis dissecans of the lateral femoral
condyle combined with a discoid lateral meniscus: a case report. J Med Case Reports. 2011;5(1):
434.
6. Detterline AJ, Goldstein JL, Rue JP, Bach BR Jr. Evaluation and treatment of osteochondritis
dissecans lesions of the knee. J Knee Surg. 2008;21(2):106-115.
7. Hefti F, Beguiristain J, Krauspe R, et al. Osteochondritis dissecans: a multicenter study of the European Pediatric Orthopedic Society. J Pediatr Orthop B. 1999;8(4):231-245.
8. Dipaola JD, Nelson DW, Colville MR. Characterizing osteochondral lesions by magnetic resonance imaging. Arthroscopy. 1991;7(1):101-104.
9. Lewis PB, McCarty LP III, Kang RW, Cole BJ. Basic science and treatment options for articular cartilage injuries. J Orthop Sports Phys Ther. 2006;36(10):717-727.


