Obesity in Children and Adolescents: Identifying Eating Disorders
ABSTRACT: The hallmarks of an eating disorder are disturbed eating behaviors (eg, binge eating, compulsive eating, and purging), dissatisfaction with body image, and medical or psychiatric comorbidities. Certain factors such as dieting, parental weight-related teasing, and family meal frequency influence the emergence of disordered eating. Depressive and anxious symptoms also contribute to eating disorder pathology. Nutrition and medical evaluation is of equal importance to psychological assessment. Routine screening of children and teens of varying sizes will increase recognition of eating disorders and improve clinical skills and confidence. Collaboration with additional providers early on is essential for effective treatment of obese children.
Addressing the obesity epidemic in America is a complex undertaking. To simplify it by saying that it is just an intake of too many calories ignores the impact of the food industry, neighborhood developers, and a convenience-driven society. All of these issues probably contribute to the problem, but it is also essential to consider a disordered relationship with food as one of the underlying causes of overweight and obesity.
Primary care clinicians are responsible for the screening and treatment of eating disorders and obesity. Eating disorders are psychological conditions with physical manifestations.1,2 Anorexia nervosa (AN) and bulimia nervosa (BN) are the most recognizable eating disorders. Increasingly, investigators are looking at the disordered eating habits of overweight and obese children and considering whether overweight and obesity are physical manifestations of binge eating disorder (BED).3 Many of these children have the same disturbed eating behaviors, dissatisfaction with body image, and medical or psychiatric comorbidities commonly found in patients with AN or BN.4-8
A lack of understanding of the varying manifestations and possible comorbidities of eating disorders and obesity may lead to a disproportionate focus on the balance between calories in and calories out. What follows is a brief review of the complexity of problems that may coexist with overweight and obesity in both children and teens. It focuses on 2 studies that address the prevalence of eating disorder symptoms and other psychopathology in this age group. These studies, along with other valuable studies on obesity, support the concern that problems contributing to obesity are not being addressed and children are not receiving adequate diagnosis and care.9-12
DIAGNOSTIC CRITERIA
FOR EATING DISORDERS
The current Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition, Text Revision (DSM-IV-TR) includes diagnostic criteria for AN, BN, and eating disorder not otherwise specified (EDNOS).1,2 The Eating Disorders Workgroup for the fifth edition of the DSM is considering classifying BED as a free-standing eating disorder.3 Table 1 includes the diagnostic criteria for eating disorders associated with overweight and obesity.
Patients with AN weigh less than 85% of their expected weight and have a distorted body image, an intense fear of gaining weight or becoming fat, and amenorrhea. In contrast, patients with BN are of normal weight or may be overweight. Patients with BN, like those with EDNOS, engage in inappropriate compensatory behaviors (self-induced vomiting, misuse of laxatives, diuretics, enemas, fasting, excessive exercising). EDNOS describes a disorder of eating that does not meet the criteria for either AN or BN and consists of a subset of disorders that includes BED and night eating syndrome. Much like BN, patients with BED engage in uncontrolled binge eating; however, they do not vomit, purge, or abuse laxatives. Patients with BED are often overweight or obese. Diagnostic criteria for eating disorders are not mutually exclusive. At diagnosis, most patients have characteristics of more than one eating disorder.
FACTORS THAT INFLUENCE DISORDERED EATING
Haines and coworkers7 conducted a prospective cohort study to identify shared risk and protective factors for purging, binge eating, and overweight. The authors used questionnaires of US children and adolescents aged 11 to 17 years enrolled in the Growing Up Today Study (the offspring of participants in the second Nurses’ Health Study). Over 3 years, more than 10,000 boys and girls answered questions about purging behaviors, binge eating, and weight. Other behaviors assessed during that time include weight concerns, dieting, fast-food intake, breakfast frequency, physical activity, and television viewing. The average age of the cohort was about 14 years; participants were predominantly white (93%) and female (57%). Researchers also inquired about socioenvironmental factors, such as maternal dieting, parental weight-related teasing, peer concern with thinness, desire to look like same-sex media figure, and family meal frequency. Table 2 shows the outcomes related to weight and disordered eating and selected predictors.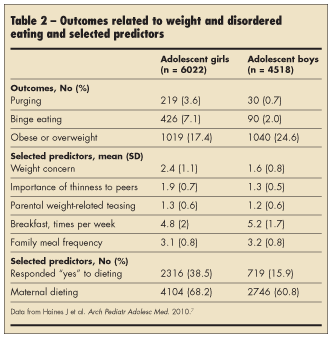
At the end of the study, 331 girls (7.8%) began purging; 503 girls (11.8%) and 132 boys (4.5%) started binge eating. Also of note, 424 girls (10%) and 382 boys (13.6%) became overweight. The results of the study suggested that concern for weight had a direct relationship to binge eating, purging, and becoming overweight. In girls, factors such as dieting, parental weight-related teasing, and family meal frequency influenced the emergence of overweight and disordered eating.
EATING DISORDERS AND DEPRESSION AND ANXIETY
In a smaller study, Eddy and colleagues6 investigated disordered eating and mental illness in children and adolescents seeking treatment in the Optimal Weight for Life pediatric weight management program at Children’s Hospital Boston. Exclusion criteria were psychotic disorders, developmental disorders with cognitive impairment, and obesity-related disorders associated with mental retardation. After 18 months of recruiting, 122 participants met the inclusion criteria. Participants and their parents received compensation for their time and participation.
Researchers used multiple interviews, inventories, scales, and questionnaires to evaluate patients for eating disorders, mood and anxiety disorders, psychopathology, and other risk factors. The results of the questionnaires and statistical analysis revealed a positive association between eating disorder pathology and depressive and anxious symptoms (ie, depression, generalized anxiety, and separation anxiety). A teasing experience, thin-ideal internalization, and decreased perfectionism all increased the possibility of an eating disorder, having an elevated negative affect. Of special note, 10 patients (8.2%) met the criteria for an eating disorder while at least one-third disclosed recent binge eating. Researchers also suggested that overweight patients with disordered eating or binge eating have a poorer prognosis for treatment.
ASSESSMENTS FOR OVERWEIGHT AND OBESITY
Both of the studies described above highlight the importance of performing psychological assessments in overweight and obese children and adolescents.13 Of equal importance are the nutritional and medical assessments that help to identify causes and consequences of being overweight.
 Nutritional and medical evaluation. Table 3 includes key components of the history, physical examination, and laboratory evaluations. A complete blood cell count and metabolic panel can help determine nutritional status. Measurement of the glycosylated hemoglobin level and a lipid panel helps screen for complications of overweight and obesity.14 In the presence of obesity and arrested linear growth, checking thyroid function may be helpful. A 12-lead ECG, which is simple and inexpensive, can provide a great deal of information in the case of obesity (eg, identify ventricular hypertrophy as a result of hypertension). An ECG can also help identify arrhythmias and ventricular or atrial hypertrophies that are possible adverse effects of laxatives, diuretics, or appetite suppressants.
Nutritional and medical evaluation. Table 3 includes key components of the history, physical examination, and laboratory evaluations. A complete blood cell count and metabolic panel can help determine nutritional status. Measurement of the glycosylated hemoglobin level and a lipid panel helps screen for complications of overweight and obesity.14 In the presence of obesity and arrested linear growth, checking thyroid function may be helpful. A 12-lead ECG, which is simple and inexpensive, can provide a great deal of information in the case of obesity (eg, identify ventricular hypertrophy as a result of hypertension). An ECG can also help identify arrhythmias and ventricular or atrial hypertrophies that are possible adverse effects of laxatives, diuretics, or appetite suppressants.
Psychological screening. There are 2 main obstacles that can make it difficult to screen for obesity or disordered eating. First, use of questionnaires to determine the presence of disordered eating behavior and mood disorders may not be conducive to the time constraints of a busy physician in private practice. However, dietitians, psychologists, or other clinical providers may have more expertise and time to administer these tools after the physician performs the initial screen. In some communities, onsite dietitions and psychologists can expedite this assessment and transfer of information.
Often patients present for issues unrelated to disordered eating, mood disorders, or obesity. As such, the appointment schedule may not allow time to screen or inquire about binge eating. After children complete the primary series of vaccines and the frequency of well child assessments decreases, there are fewer opportunities to assess growth and thus fewer plots on the growth curve to assess linear, weight, and body mass index velocity. Even when a clinician identifies an eating disorder, there is no guarantee the family will return for follow-up, especially because an eating disorder is usually not on the list of family concerns. Second, how to code a follow-up appointment and the risk of not being reimbursed for time spent is always a concern.
In addition to the issues of time and reimbursement are the challenges of patient nondisclosure and parental influence. The Haines7 and Eddy6 studies highlight that at least 1 of 4 overweight or obese patients has either binge eating behaviors or symptoms of a mood disorder.6,7 Patients tend to withhold information or downplay the severity of their disordered behaviors. Clinicians should consider interviewing patients, especially adolescents, without their parents in the room.
Some parents struggle with their own subclinical (or overt) eating disorders. Other parents are not aware of the signs of an eating or mood disorder. Sadly, some parents chide and lecture the child about making better food choices, and overlook the tearfulness, withdrawal, and signs of depression. The child sneaks food not because of hunger but because of feelings of sadness or anxiety. Parents may not mention that they recently separated or divorced. Military families may not realize that every time a parent is deployed, the child withdraws, changes eating habits, and gains weight.
During the psychological assessment, it is important to also consider whether being corpulent is a sign of wealth or health in various cultures.5 Neither clinicians nor parents may view consumption of food during celebrations, bereavement, or days of worship as binging. In some cultures, friends and family go out to dinner after church or Sunday worship. In the midst of all of the fellowship, is someone binge eating? In other cultures, using food to mute feelings of pain, depression, or low self-esteem is more acceptable than talking about the feelings. Many families do not like to discuss feelings or uncomfortable events. As long as everyone remains “quiet” either by not speaking or keeping their mouth full, then everything is okay.
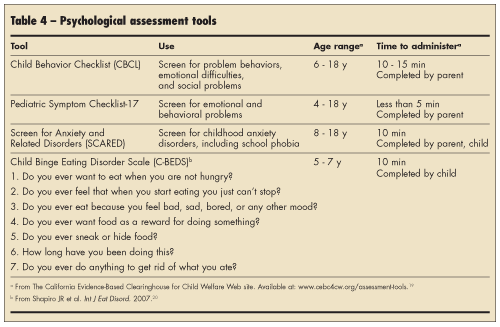
Tools of assessment. Interviews, inventories, scales, and questionnaires used to evaluate patients for eating disorders, mood and anxiety disorders, psychopathology, and other risk factors are listed in Table 4. Routine psychological screening of children of varying sizes for eating disorders will increase recognition of eating disorders and improve clinical skills and confidence. Along with screening questions typical for overweight and obesity, ask about skipping meals and sneaking or stealing food. Patients may disclose that they often feel as though they cannot stop eating or that their eating is out of control; parents may describe a child who likes to eat so much that it is hard to stop the child from overeating.15
Ask parents about the frequency of family meals and how often they find hidden spoiled food and food wrappers. In addition to obtaining a family history for weight-related chronic diseases, inquire about a family history of substance abuse, mood disorders, and eating disorders or obesity. A personal history of mental illness; sexual, physical, or verbal abuse; or parental weight-related teasing should prompt further questions about binge eating. Many of these are risk factors for both obesity and eating disorders.16
TREATMENT AND REFERRAL
Obese patients with known or suspected binge eating and those with a possible mood disorder should be further evaluated by a mental health professional. The American Academy of Pediatrics’ recommended approach to obesity treatment follows 4 stages. Stage 1 (Prevention Plus) and Stage 2 (Structured Weight Management) can be completed in a primary care setting, often with the support of a dietitian, counselor or other mental health professional. Recent evidence suggests that obesity management in primary care settings can work when physicians collaborate with other health professionals.17 Stage 3 (Comprehensive Multidisciplinary Intervention) and Stage 4 (Tertiary Care Intervention) are characterized by multidisciplinary teams specializing in treatment of obese children and adolescents. Many of these teams include clinical social workers and psychologists familiar with disordered eating in obese patients. These providers play an important role in assessing readiness for change and in identifying specific family needs. Treatment plans may include behavioral weight management, mental health or developmental consult, family therapy, or a combination of these options to increase the likelihood of success.18
Evaluation and treatment of childhood obesity is difficult enough without adding eating disorders to the equation. Traditionally, treatment of obesity focuses on energy balance. However, focusing on calories and weight loss without resolving the underlying body image or psychiatric problems represents partial treatment and is likely to lead to relapse. If the fifth edition of the
1. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, 4th Edition, Text Revision. Washington DC: American Psychiatric Association; 2000.
2. Franco KN. Eating Disorders. Cleveland Clinic Center for Continuing Education. Available at: http://www.clevelandclinicmeded.com/medicalpubs/diseasemanagement/psychiatry-psychology/eating-disorders/. Accessed November 13, 2011.
3. American Psychiatric Association DSM-5 Development. Proposed Draft Revisions to DSM Disorders and Criteria. Available at: http://www.dsm5.org/ProposedRevisions/Pages/Default.aspx. Accessed November 13, 2011.
4. Decaluwé V, Braet C. Assessment of eating disorder psychopathology in obese children and adolescents: interview versus self-report questionnaire. Behav Res Ther.2004;42:799-811.
5. Desocio JE, O’toole JK, Nemirow SJ, et al. Screening for childhood eating disorders in primary care. Prim Care Companion J Clin Psychiatry. 2007;9:16-20.
6. Eddy KT, Tanofsky-Kraff M, Thompson-Brenner H, et al. Eating disorder pathology among overweight treatment-seeking youth: clinical correlates and cross-sectional risk modeling. Behav Res Ther. 2007;45:2360-2371.
7. Haines J, Kleinman KP, Rifas-Shiman SL, et al. Examination of shared risk and protective factors for overweight and disordered eating among adolescents. Arch Pediatr Adolesc Med. 2010;164:336-343.
8. Hamilton JD. Eating disorders in preadolescent children. Nurse Pract. 2007;32:44-48.
9. Bean MK, Stewart K, Olbrisch ME. Obesity in America: implications for clinical and health psychologists. J Clin Psychol Med Settings. 2008;15:214-224.
10. Haines J, Neumark-Sztainer D. Prevention of obesity and eating disorders: a consideration of shared risk factors. Health Educ Res. 2006;21:770-782.
11. Tanofsky-Kraff M, Yanovski SZ. Eating disorder or disordered eating? Non-normative eating patterns in obese individuals. Obes Res. 2004;12:1361-1366.
12. Zametkin AJ, Zoon CK, Klein HW, Munson S. Psychiatric aspects of child and adolescent obesity: a review of the past 10 years. J Am Acad Child
Adolesc Psychiatry. 2004;43:134-150.
13. American Academy of Pediatrics. Policy Statement: identifying and treating eating disorders.
Pediatrics. 2003;111:204-214.
14. Ozier AD, Henry BW; American Dietetic Association. Position of the American Dietetic Association: nutrition intervention in the treatment of eating disorders. J Am Diet Assoc. 2011;111:1236-1241.
15. Marcus MD, Kalarchian MA. Binge eating in children and adolescents. Int J Eat Disord. 2003;34:S47-S57.
16. Rome ES, Ammerman S, Rosen DS, et al. Children and adolescents with eating disorders: the state of the art. Pediatrics. 2003;111:e98-e108.
17. Wadden TA, Volger S, Sarwer DB, et al. A two-year randomized trial of obesity treatment in primary care practice [published online ahead of print November 14, 2011]. N Engl J Med.
18. Spear BA, Barlow SE, Ervin C, et al. Recommendations for treatment of child and adolescent overweight and obesity. Pediatrics. 2007;120:S254-S288.
19. The California Evidence-Based Clearinghouse for Child Welfare Web site. Screening and Assesment Tools for Child Welfare. Available at: www.cebc4cw.org/assessment-tools. Accessed November 18, 2011.
20. Shapiro JR, Woolson SL, Hamer RM, et al. Evaluating binge eating disorder in children: development of the children’s binge eating disorder scale (C-BEDS). Int J Eat Disord. 2007;40:82-89.


