Neonatal Asymmetric Crying Facies
A 2-week-old infant presented with asymmetry of the left side of his face that occurred every time he cried and that had been present since birth (A). The parents had noted that the right side of the lower lip droops while the left side stays higher.

The child had been born via vaginal delivery after an uneventful full-term pregnancy. His Apgar scores were 9 and 10 at 1 and 5 minutes, respectively. No forceps, vacuums, or other instruments were used to facilitate delivery. The parents denied any trauma to the infant’s face or head. There was no family history of similar asymmetry of the face.
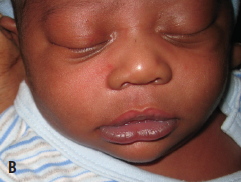 The infant had no asymmetry of the face when he was asleep or quiet (B). The asymmetry during crying was limited to the lower face, with no lagophthalmos or asymmetry of the upper face. The results of the physical examination were completely normal, other than this feature. The nasolabial folds were intact and symmetric when he was quiet. Sucking was normal, and there was no drooling during feeding. There were no neurologic deficits; the infant moved all extremities normally, and no cranial nerve deficits were detected. Results of a cardiac examination also were normal, with no murmurs heard and normal femoral pulses.
The infant had no asymmetry of the face when he was asleep or quiet (B). The asymmetry during crying was limited to the lower face, with no lagophthalmos or asymmetry of the upper face. The results of the physical examination were completely normal, other than this feature. The nasolabial folds were intact and symmetric when he was quiet. Sucking was normal, and there was no drooling during feeding. There were no neurologic deficits; the infant moved all extremities normally, and no cranial nerve deficits were detected. Results of a cardiac examination also were normal, with no murmurs heard and normal femoral pulses.
Among the possible etiologies we considered were birth trauma, congenital facial nerve (cranial nerve VII) palsy, congenital absence of the facial nerve, and hemiatrophy of the face. However, the lack of history of trauma, no involvement of the upper face, and no asymmetry at rest made these diagnoses unlikely and are pathognomonic for neonatal asymmetric crying facies (NACF).
After careful evaluation, our patient was found not to have any cardiac or other systemic abnormalities. The condition was explained to the parents, including that the infant’s left side was the abnormal side, despite the abnormal appearance of the right side. They were asked to return in a month for reevaluation. At that time, the asymmetry had improved somewhat, and the parents were reassured that there was a good chance the condition would resolve spontaneously.
Discussion
NACF is a relatively common condition with an annual incidence of approximately 0.4% to 0.6%.1 It is thought to result from weakness of the depressor muscles of the mouth.2,3 It is typically a self-limited condition that resolves or becomes less obvious over time, although significant genetic systemic abnormalities are associated in a small number of cases.1,2,4
The depressors of the angle of the mouth are the depressor anguli oris muscle (DAOM) and the depressor labii inferioris muscle (DLIM). The DAOM inserts into the corner of the mouth and allows mouth eversion and the ability to pull it downward and slightly laterally. The DLIM is located slightly anterior to the DAOM, inserting into the lower lip with the primary action of depressing it. In addition, the mentalis muscle extends from the lower lip to the chin and raises and protrudes the lower lip. All of these muscles are enervated by the marginal mandibular branch of the facial nerve. In neonates, unlike in adults, this branch lies very close to the edge of the mandible and is therefore susceptible to trauma. Trauma can result from forceps injury during birth, but it also can occur in utero as a result of fetal positioning or during vaginal delivery as a result of compression by the birth canal.
Approximately 20% of NACF cases are caused by partial facial nerve palsy as a result of trauma.1 Most cases involve the left side. Nearly 90% of traumatic palsies resolve spontaneously by 1 year of age and do not have associated systemic abnormalities.1
A far more common cause (80%) of NACF is congenital hypoplasia of the DAOM, less commonly the DLIM, and rarely the mentalis muscle.3 Congenital hypoplasia can result in a clinical picture that is indistinguishable from that of traumatic palsy of the marginal mandibular branch of the facial nerve. However, this condition is more likely to be right-sided. Hypoplasia of the DAOM is inherited in an autosomal dominant fashion in a number of cases. Family members might demonstrate only slightly irregular lower lips on grimacing. Unlike traumatic palsy, hypoplasia of the muscles does not resolve and might require surgical management for cosmetic reasons.
Approximately 10% of congenital hypoplasia cases have associated systemic abnormalities, primarily cardiac anomalies (craniofacial syndrome), although defects in nearly all systems have been described. Associated cardiac defects include ventricular and atrial septal defects and tetralogy of Fallot. Other defects described have included neuroblastoma, mediastinal teratoma, trisomy 18, collodion skin disease, and neurofibromatosis type 1.
In the small percentage of patients with facial asymmetry and cardiac anomalies or with familial NACF, genetic testing reveals microdeletions from 22q11.2, a very common chromosomal defect that occurs in approximately 1 in 4,000 births.2 This defect commonly is associated with cardiac (75%) and neurologic (80%) abnormalities, as well as NACF (50%).2
In children with NACF, a careful history should be obtained regarding any birth trauma or perinatal factors associated with facial nerve compression, such as primiparity, uterine tumors, a large baby, multiple births, or a difficult labor or delivery. If evidence suggests trauma, no further workup is needed. In other cases, or in patients with a positive family history, a careful examination should be done to rule out cardiac or neurologic abnormalities. Genetic testing also may be indicated in these cases.
Children with NACF can be observed for spontaneous resolution, which occurs in most traumatic cases within 1 to 2 years. Even in cases that do not resolve, conservative management is a valid option, since the asymmetry typically becomes less obvious as a child gets older, only manifests during crying, and does not affect other facial expressions.
In children with more severe facial asymmetry, surgical management may be indicated.5 This traditionally involves myectomy or selective neurectomy of the marginal mandibular branch of the facial nerve on the unaffected side to make the lip symmetric. However, these procedures can lead to lack of emotive movement and unintentional biting of the lip and cheek.
More aggressive surgical techniques such as neurovascular transposition and autologous fascia lata grafts result in better cosmesis but have higher rates of complications. Because these surgeries usually are done after 2 years of age to allow for spontaneous resolution, temporary symmetry may be achieved by injecting botulinum toxin into the normal depressors.6
References:
1.
Sapin SO, Miller AA, Bass HN. Neonatal asymmetric crying facies: a new look at an old problem. Clin Pediatr (Phila). 2005;44(2):109-119.
2.
Lahat E, Heyman E, Barkay A, Goldberg M. Asymmetric crying facies and associated congenital anomalies: prospective study and review of the literature. J Child Neurol. 2000;15(12):808-810.
3.
Miller M, Hall JG. Familial asymmetric crying facies: its occurrence secondary to hypoplasia of the anguli oris depressor muscles. Am J Dis Child. 1979;133(7):743-746.
4.
Stewart HS, Clayton-Smith J. 22q11 deletion: a cause of asymmetric crying facies [letter]. Arch Dis Child. 1996;75(1):89.
5.
Udagawa A, Arikawa K, Shimizu S, et al. A simple reconstruction for congenital unilateral lower lip palsy. Plast Reconstr Surg. 2007;120(1):238-244.
6.
Isken T, Gunlemez A, Kara B, Izmirli H, Gercek H. Botulinum toxin for the correction of asymmetric crying facies. Aesthet Surg J. 2009;29(6):524-527.
SANJEEV Y. TULI, MD; MARIA N. KELLY, MD; DONALD J. FILLIPPS, MD; and SONAL S. TULI, MD
University of Florida College of
Medicine, Gainesville


